Introduction
Thyroid cancer patients face a confusing nutritional landscape. Before radioactive iodine treatment, doctors prescribe a low-iodine diet—no salt, dairy, or seafood—but offer little guidance on what to eat afterward. Many patients complete treatment without understanding how diet influences recovery speed, hormone stability, and potentially cancer recurrence.
The stakes are real. While thyroid cancer has a five-year survival rate exceeding 98%, emerging research shows that diet directly shapes treatment effectiveness and long-term outcomes. Obesity increases thyroid cancer risk by 55%, and metabolic dysfunction correlates with larger tumors and more aggressive disease.
This guide covers both phases of thyroid cancer nutrition: the short-term low-iodine protocol required before radioactive iodine therapy, and research-backed long-term strategies that support metabolic health and target cancer cell vulnerabilities.
TLDR
- A low-iodine diet (under 50 mcg/day) is required 1-2 weeks before RAI therapy — avoid iodized salt, dairy, seafood, egg yolks, soy, and processed foods during this window
- Long-term, plant-forward eating with limited red meat reduces thyroid cancer risk and supports recovery
- Methionine restriction shows promise by targeting how cancer cells process protein differently than healthy cells
- Work with your oncologist or a dietitian familiar with integrative oncology before making major dietary changes
The Low-Iodine Diet: What It Is and When to Follow It
The low-iodine diet (LID) is a temporary medical protocol that restricts iodine intake to 50 micrograms per day or less—one-third of the standard 150 mcg daily recommendation for adults. This restriction makes thyroid cells "hungry" for iodine, maximizing their uptake of radioactive iodine-131 during treatment.
Who needs it: Only patients with differentiated thyroid cancers (papillary and follicular) preparing for radioactive iodine therapy or diagnostic whole-body scans. Medullary and anaplastic thyroid cancers don't absorb iodine, making this diet unnecessary for those diagnoses.
Timing matters: most oncologists recommend starting the LID 1-2 weeks before RAI treatment and continuing 1-3 days after. If iodine depletion is insufficient, thyroid tissue may not absorb the radioactive iodine adequately. This can reduce scan accuracy or weaken treatment effectiveness.
Hidden iodine sources patients overlook:
- Vitamins and supplements containing kelp, dulse, or oyster shell-derived calcium
- FD&C Red No. 3 (erythrosine) in food colorings and medications
- Restaurant food prepared with iodized salt
- Iodate dough conditioners in commercial baked goods
- Carrageenan and agar-agar in processed foods
The LID is not a long-term diet. Prolonged iodine restriction can cause nutritional deficiencies and disrupt hormone production — resume normal iodine intake once your medical team approves.
What to Eat and What to Avoid on a Low-Iodine Diet
Because iodized salt and high-iodine ingredients appear in countless packaged foods, home cooking and careful label-reading become essential during the low-iodine diet (LID) period. The lists below break down what's safe and what to cut out.
Foods to Eat (Low-Iodine Safe Foods)
Safe options during the LID include:
- Fresh fruits and vegetables (fresh or frozen without added salt)
- Egg whites only — yolks contain 177 mcg iodine per 100g
- Fresh unseasoned meats like chicken, turkey, beef, or pork (limit to 5–6 oz/day)
- Freshwater fish such as carp, river bass, or lake trout
- Unsalted nuts and nut butters
- Whole grains and pasta without high-iodine ingredients
- Olive oil and vegetable oils
- Non-iodized salt (check labels carefully)
- Coffee and tea (plain, no dairy or soy creamer)
- Natural sweeteners like honey, maple syrup, and jam
Sample LID breakfast: Plain oatmeal topped with fresh berries and maple syrup, scrambled egg whites cooked in olive oil, black coffee. This meal provides approximately 5–10 mcg of iodine — well within the 50 mcg daily limit.
Foods to Avoid (High-Iodine Foods)
Eliminate these during the LID period:
- All forms of iodized salt and sea salt (sea salt contains 1.5–4,663 mcg per 100g depending on processing)
- All dairy products including milk, cheese, yogurt, and butter
- Egg yolks
- All seafood and seaweed (nori contains 2,317 mcg per 100g)
- Soy products including soy milk, tofu, and soy sauce
- Processed and packaged foods made with iodized salt
- Commercial bakery products with iodate dough conditioners
- Blackstrap molasses, organ meats, and cured meats
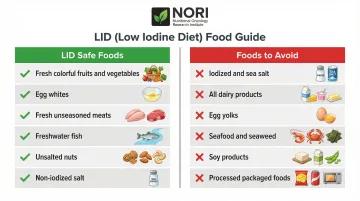
One point worth clarifying: low-iodine is not the same as low-sodium. Non-iodized salt is allowed freely. Sea salt, though it sounds natural, must be avoided — it contains iodine regardless of processing.
Long-Term Nutritional Strategies for Thyroid Cancer Recovery
Once RAI treatment concludes, you shift from temporary iodine restriction to a sustainable, recovery-focused eating pattern. Diet influences thyroid cancer risk and recurrence through insulin resistance, inflammation, and weight management — all areas you can address directly through food choices.
Plant-Forward, Anti-Inflammatory Eating
The EPIC study of over 500,000 participants found that while total fruit and vegetable intake showed no significant association with thyroid cancer risk, red and processed meat consumption correlates with increased cancer risk across multiple types.
Cruciferous vegetables—broccoli, kale, cauliflower—contain bioactive compounds (indoles and thiocyanates) with anti-inflammatory properties. The concern about "goitrogenic" effects is primarily relevant only in iodine-deficient individuals, not post-thyroidectomy patients on adequate levothyroxine replacement. These vegetables are safe to eat, especially when cooked.
Weight and Metabolic Health
Obesity increases thyroid cancer risk by 55% compared to normal-weight individuals. Insulin resistance and metabolic syndrome associate with larger tumor size and extrathyroidal extension, making low-glycemic, whole-food eating directly relevant for long-term recovery.
Key strategies:
- Minimize refined carbohydrates and added sugars
- Pair carbohydrates with protein and healthy fats to stabilize blood sugar
- Focus on whole grains, legumes, and fiber-rich foods
- Maintain healthy body weight through portion control
Methionine Restriction: An Emerging Strategy
Cancer cells exhibit abnormal dependence on the amino acid methionine for growth and replication — a phenomenon called methionine dependence. Restricting dietary methionine by minimizing high-methionine animal proteins can exploit this metabolic vulnerability.
NORI's protocol, developed through over 20 years of focused cancer nutrition research, centers on cycled methionine restriction. This approach has supported thyroid cancer patients in their recovery, including a documented case report of a Stage IV Papillary Thyroid Cancer patient who reported thyroglobulin tumor markers dropping from 13 to nearly undetectable levels within three months.

The core protocol elements include:
- A predominantly plant-based diet limiting protein to under 0.3g per kg body weight daily — reducing animal protein in this way, without causing malnutrition, can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research
- Cycled methionine restriction phases timed to cancer cell vulnerability
- Targeted pro-oxidant nutraceuticals, including sodium selenite, that generate ROS or inhibit glutathione in cancer cells
NORI offers free initial consultations for patients seeking personalized guidance. Contact them at 800-634-3804 or info@nutritionaloncology.net.
Supplements to Discuss With Your Physician
Vitamin D: A 2024 meta-analysis found vitamin D levels 13% lower in thyroid cancer patients than controls, suggesting deficiency as a potential risk factor. Supplementation may support immune function and bone health.
Selenium: Selenium supports thyroid hormone conversion from inactive T4 to active T3, making it especially relevant after thyroidectomy. Most patients supplement with 200 mcg daily for maintenance; therapeutic doses go higher under medical supervision.
Calcium and Vitamin D (Calcitriol): Hypoparathyroidism and resulting hypocalcemia are common post-thyroidectomy complications. Patients with postoperative PTH levels below 15 pg/mL typically require prophylactic oral calcium and active vitamin D supplementation.
Lifestyle Factors That Complement a Thyroid Cancer Diet
Exercise and Cancer Recovery
Exercise is safe and beneficial for cancer survivors, reducing all-cause and cancer-specific mortality. High-intensity interval training (HIIT) and combined aerobic/resistance training improve insulin sensitivity and lower inflammatory markers like C-reactive protein (a key marker of systemic inflammation).
Benefits for thyroid cancer patients include:
- Managing insulin resistance and metabolic syndrome
- Reducing inflammatory adipose tissue
- Supporting muscle retention during recovery
- Improving energy levels and mood
Begin with moderate activity like walking, then build toward more vigorous exercise as your recovery allows.
Addressing Post-Thyroidectomy Fatigue
After thyroid removal, many patients experience significant fatigue due to disrupted hormone production. This improves as thyroid hormone replacement is optimized, but dietary strategies also help:
- Adequate protein intake supports tissue repair and muscle retention
- Iron-rich foods (spinach, lentils, lean meats) address potential anemia
- Stable blood sugar through regular meals prevents energy crashes
- Timing meals strategically — avoiding calcium-rich foods or coffee within an hour of thyroid medication helps support proper absorption

Expect metabolic stabilization to take several months — dietary consistency during this window makes a real difference.
Sleep, Stress, and Recovery
Chronic stress and poor sleep elevate cortisol and inflammatory markers, undermining dietary benefits. When the body stays locked in a stress response, it suppresses immune function and can drive inflammation that works against recovery efforts.
Integrate these practices:
- Prioritize 7-9 hours of quality sleep nightly
- Practice stress-reduction techniques like meditation or deep breathing
- Maintain social connections and support networks
- Treat diet, sleep, and stress management as a unified recovery strategy — each reinforces the others
Conclusion
Thyroid cancer nutrition involves two distinct phases: a short-term, strictly managed low-iodine diet before radioactive iodine treatment, followed by long-term commitment to anti-inflammatory, whole-food eating that supports metabolic health and reduces recurrence risk.
The temporary LID maximizes treatment effectiveness by depleting iodine stores before RAI. Once that window closes, the focus shifts: a plant-forward diet with controlled protein intake and healthy weight maintenance creates an internal environment less hospitable to cancer cell growth — while supporting your overall health through recovery and beyond.
For personalized nutritional support—especially if you have advanced or recurring thyroid cancer—explore NORI's home-based program. NORI offers free initial consultations and has supported thyroid cancer patients worldwide through its home-based nutritional protocol, which is grounded in over 20 years of focused research. Call 800-634-3804 or visit nutritionaloncology.net to learn more.
Frequently Asked Questions
What foods should I avoid after thyroid cancer?
After active treatment, minimize processed foods, red and cured meats, excessive sugar, and foods promoting insulin resistance. Shift toward a plant-forward, whole-food diet with ample vegetables, fiber, and lean proteins to support long-term metabolic health and reduce recurrence risk.
Should thyroid cancer patients avoid iodine?
Iodine restriction is temporary and specific to the 1-2 week period before RAI treatment (targeting under 50 mcg/day). Long-term, your body needs normal iodine intake for hormone production. Restricting it permanently causes nutritional deficiencies and hormonal disruption.
What can I eat for breakfast on a low iodine diet?
Plain oatmeal with fresh fruit, honey, or maple syrup; egg whites (not yolks) scrambled in vegetable oil; fresh fruit with unsalted nut butter; and black coffee or plain tea—all prepared without iodized salt or dairy products.
Why do I feel so tired after a thyroidectomy?
Fatigue stems from disrupted thyroid hormone production, which regulates metabolism and energy. Hormone replacement medication directly addresses this, while adequate protein, iron-rich foods, and stable blood sugar through regular meals can help manage fatigue levels.
How long does it take to recover from thyroid cancer surgery?
Most patients recover from the surgical procedure itself within 1-2 weeks and can resume light activities. Full hormonal and metabolic stabilization can take several months as thyroid hormone replacement dosing is adjusted.
What should the TSH level be after a total thyroidectomy?
Target TSH levels depend on cancer risk category. High-risk patients may need TSH suppression below 0.1 mU/L, intermediate-risk patients target 0.1-0.5 mU/L, while low-risk patients maintain 0.5-2.0 mU/L. Follow your endocrinologist's guidance and monitor levels regularly for optimal management.