
Introduction
The pancreas plays two distinct roles in your body: its exocrine function produces enzymes that break down fats, proteins, and carbohydrates, while its endocrine function releases insulin to control blood glucose. Pancreatic cancer can disrupt both — and that dual failure is what makes nutritional management so challenging.
That organ dysfunction isn't the only threat to your nutritional status. Even patients eating normally can lose muscle and fat — because cancer-released compounds called cytokines trigger muscle wasting independent of food intake.
Up to 87% of pancreatic cancer patients experience cachexia—a severe wasting syndrome associated with shorter survival and reduced treatment tolerance.
Nutrition during treatment directly influences your ability to tolerate chemotherapy, fight infection, and preserve quality of life. This article provides 12 practical, research-backed diet tips to help patients and caregivers make smarter food choices at every stage of treatment.
Why Pancreatic Cancer Makes Nutrition So Challenging
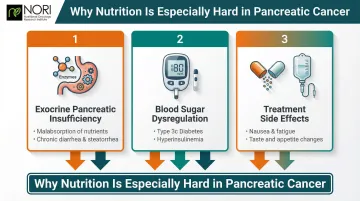
The pancreas produces digestive enzymes that break down fats, proteins, and carbohydrates. Tumor growth or surgical removal of pancreatic tissue often leads to Exocrine Pancreatic Insufficiency (EPI), which affects 50–100% of patients with unresectable pancreatic cancer and over 75% post-resection. EPI causes malabsorption, diarrhea, bloating, and weight loss because food passes through undigested.
Pancreatic cancer is also strongly associated with blood sugar dysregulation. Approximately 80% of patients have abnormal glucose levels, and nearly two-thirds develop diabetes—most within 24–36 months before diagnosis. This is Type 3c (pancreatogenic) diabetes, caused when cancer damages insulin-producing beta cells.
Chronically high insulin levels (hyperinsulinemia) can drive tumor progression by activating insulin receptors in pancreatic tissue and promoting inflammation—making blood sugar management a metabolic priority, not just a side concern.
Treatment side effects—nausea, vomiting, taste changes, fatigue—compound the challenge of eating adequately. These three forces together (EPI, blood sugar dysregulation, and treatment burden) make nutrition far harder to manage in pancreatic cancer than in most other diagnoses. The 12 tips below address each of these layers directly.
TLDR: 12 Diet Tips at a Glance
- Eat small, frequent meals (5–6 per day) to reduce nausea and digestive strain
- Drink 64+ ounces of water daily; skip caffeine and alcohol
- Weigh yourself weekly and alert your care team if you lose more than 1–2 pounds per week
- Prioritize protein at every meal; use liquid supplements when solid food is difficult
- Focus on colorful vegetables, omega-3 fish, healthy fats, and whole grains at every meal
- Cut back on sugar, processed foods, and fried foods that strain digestion
Tips 1–4: Managing How You Eat — Portions, Hydration, Weight, and Supplements
Tip 1: Eat Small, Frequent Meals
Five to six small meals spaced every 3–4 hours are easier for a compromised pancreas to process than two to three large meals. This reduces bloating, nausea, and early satiety. Smaller portions also help manage blood sugar spikes—critical since a high proportion of pancreatic cancer patients develop glucose intolerance.
Set a reminder or alarm to eat on schedule. When appetite is poor, structure beats waiting until you feel hungry.
Tip 2: Stay Hydrated
Aim for approximately 64 ounces (eight glasses) of fluid daily. Drink fluids one hour before or after meals rather than during to avoid filling up and reducing food intake.
Best hydrating options:
- Water
- Herbal teas
- Bone broth
- Diluted fruit juices
Avoid:
- Caffeinated beverages
- Alcohol
- Sugar-sweetened drinks
Tip 3: Monitor and Protect Your Weight
Some weight loss is expected after diagnosis and during treatment. Rapid or unintended weight loss weakens immunity, reduces treatment tolerance, and accelerates muscle wasting. Cachexia affects 45% of advanced pancreatic cancer patients and is associated with significantly earlier treatment failure and lower survival.
Weigh yourself weekly. Alert your care team if you're losing more than 1–2 pounds per week.
Tip 4: Use Liquid Supplements When Food Is Hard to Tolerate
When food becomes difficult to tolerate, liquid nutrition is one of the most effective ways to maintain caloric intake and protect weight. It's especially useful during chemotherapy, post-surgery recovery, or periods of severe appetite loss.
High-protein options easier to consume:
- Protein drinks
- Greek yogurt smoothies
- Pureed soups
- Bone broth-enriched shakes
- High-protein milks
Look for options with at least 200–300 calories per serving and under 10g of added sugar.
Tips 5–7: What to Eat — Protein, Healthy Fats, and Easy-to-Digest Foods
Tip 5: Include High-Quality Protein at Every Meal
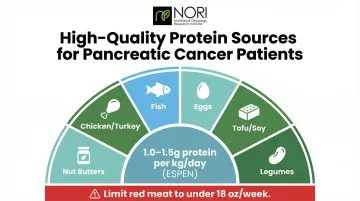
Protein requirements increase during cancer care. Your body uses protein to repair damaged cells, support immune function, and counteract muscle breakdown caused by cytokines and cachexia. ESPEN guidelines recommend 1.0–1.5 g/kg/day of protein during active cancer care, significantly higher than the 0.8 g/kg/day RDA for healthy adults.
Best protein sources for pancreatic cancer patients:
- Baked or grilled chicken, turkey, and fish
- Eggs
- Legumes (beans, lentils)
- Tofu and other soy products
- Nut butters
- Low-fat dairy
Limit red meat to under 18 ounces per week and avoid charred or heavily processed meats. Since protein alone rarely provides enough calories during treatment, healthy fats fill the gap efficiently.
Tip 6: Embrace Healthy Fats
Healthy fats are calorie-dense, allowing you to increase energy intake without requiring large food volumes—critical when appetite is suppressed.
Omega-3 fatty acids from fatty fish (salmon, mackerel, sardines), flaxseeds, and walnuts stand out for their direct impact on cancer care outcomes. Clinical studies show omega-3s help preserve muscle mass in cachexia, reduce chemotherapy-induced inflammation, and may enhance gemcitabine effectiveness in pancreatic cancer care.
Additional healthy fats to build into daily meals:
- Olive oil
- Avocado
- Nuts
- Seeds (flaxseeds, chia seeds)
Tip 7: Choose Easy-to-Digest Foods
Treatment side effects and reduced enzyme production can make digestion difficult. Soft, cooked, or well-chopped foods place less strain on the digestive system than raw or fibrous alternatives.
Easy-to-digest, nutrient-dense foods:
- Oatmeal
- Cooked vegetables (carrots, zucchini, sweet potatoes)
- Sourdough bread
- Scrambled eggs
- Pureed soups
- Soft fruits (bananas, avocados)
Avoid raw vegetables, high-fiber legumes, and fatty or fried foods during periods of digestive distress.
Tips 8–10: Supercharging Your Diet with Plant Power
Tips 8–10: Plant-Based Strategies to Support Pancreatic Cancer Nutrition
Tip 8: Eat Colorful Fruits and Vegetables for Antioxidants
Colorful produce is rich in vitamins (C, A, E), minerals, and antioxidants that help neutralize free radicals—unstable molecules that accelerate cellular damage and tumor progression. Aim for at least five servings of fruits and vegetables per day.
Antioxidant-rich choices:
- Berries
- Leafy greens
- Cruciferous vegetables (broccoli, cauliflower)
- Citrus fruits (high in Vitamin C)
- Orange/yellow produce (beta-carotene)
Research shows Vitamin C can synergize with gemcitabine in pancreatic cancer care. A randomized trial found that adding intravenous pharmacological ascorbate to gemcitabine and nab-paclitaxel doubled median overall survival to 16 months compared to 8.3 months for chemotherapy alone.
Tip 9: Choose Whole Grains Over Refined Carbohydrates
Whole grains—oatmeal, quinoa, brown rice, farro, bulgur, whole grain bread—provide complex carbohydrates and fiber that digest slowly, avoiding rapid blood sugar spikes. This is critical given pancreatic cancer's link to insulin dysregulation.
Hyperglycemia feeds tumor growth. Frequent consumption of high-glycemic load foods may increase pancreatic cancer risk by inducing insulin resistance. A low-glycemic dietary pattern may help reduce cancer cell proliferation by keeping insulin and IGF-1 levels lower — unlike refined carbohydrates such as white bread, pasta, and sugary cereals, which spike blood sugar rapidly.
Tip 10: Add Cancer-Fighting Plant Compounds to Your Meals
Three evidence-supported plant compounds show promise in pancreatic cancer research:
Curcumin (turmeric): Clinical trials show curcumin reduces NF-κB activation and improves gemcitabine tolerance. Turmeric integrates easily into soups, stir-fries, and rice dishes.
Sulforaphane (broccoli, Brussels sprouts): Sulforaphane targets pancreatic cancer stem cells and potentiates chemotherapy effects — making regular cruciferous vegetable intake one of the more actionable dietary shifts patients can make.
Resveratrol (red grapes, berries): Resveratrol inhibits pancreatic cancer cell proliferation and enhances gemcitabine sensitivity. Berries and small amounts of dark grapes are practical ways to incorporate it into your daily meals.

Tips 11–12: What to Limit and What to Watch For
Tip 11: Limit Sugar, Processed Foods, Alcohol, and High-Fat Junk Foods
High glucose levels activate EGFR signaling pathways that drive tumor proliferation. A high glycemic load diet is associated with elevated pancreatic cancer risk, particularly in patients with insulin resistance37962-1/fulltext).
Foods and beverages to limit or eliminate:
- Sugary drinks, cakes, candy, refined pastries
- Processed/deli meats (WHO Group 1 carcinogen)
- Alcohol (a known carcinogen contributing to dehydration)
- Fried/high saturated-fat foods that worsen digestive symptoms
Tip 12: Watch for Digestive Changes and Consider Enzyme Support
Changes in bowel habits — diarrhea, constipation, greasy stools (steatorrhea), bloating, or gas — are common indicators of EPI and poor nutrient absorption. Report these to your care team promptly.
Pancreatic enzyme replacement therapy (PERT) may be prescribed to help absorb nutrients from food. Ask your care team to monitor these nutrients through regular bloodwork — deficiencies are common and often go undetected:
- Vitamins A, D, E, K (fat-soluble; poorly absorbed with EPI)
- Vitamin B12 (frequently depleted in pancreatic cancer patients)
A Holistic Nutritional Approach for Pancreatic Cancer Patients
While the 12 tips above form a strong foundation, nutritional oncology goes deeper. The specific composition of your diet—including protein sources, amino acid profiles, and targeted nutraceuticals—can be tailored to exploit vulnerabilities in cancer cell metabolism rather than simply managing side effects.
One emerging approach is methionine restriction: cancer cells are typically methionine-dependent, meaning restricting dietary methionine (found most abundantly in red meat and eggs) through a largely plant-based, fruit-forward diet may help selectively inhibit cancer cell growth while normal cells adapt. Reducing protein intake — especially animal protein — without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research.
NORI (Nutritional Oncology Research Institute) offers a home-based nutritional support program built around methionine-restricted dietary protocols combined with proprietary nutraceuticals, designed to complement conventional treatment. The program requires no clinic visits and serves patients worldwide.
NORI offers a free initial consultation for patients exploring integrative nutritional support. Reach them at 800-634-3804 or info@nutritionaloncology.net.
Whether you pursue an integrative program or not, working with a registered oncology dietitian remains essential. Personalized nutrition planning based on bloodwork, treatment phase, and individual tolerance produces far more reliable results than a one-size-fits-all approach.
Frequently Asked Questions
What is the best diet for pancreatic cancer patients?
Evidence supports small, frequent protein-rich meals, healthy fats (especially omega-3s), antioxidant-rich vegetables and fruits, whole grains, and reduced sugar and processed foods. An oncology dietitian can tailor this pattern to your specific treatment stage and symptoms.
What foods should be avoided with pancreatic cancer?
Limit added sugars and sweetened beverages, alcohol, fried and high-fat processed foods, processed/cured meats, refined carbohydrates, and excess red meat. These worsen inflammation, blood sugar regulation, and digestive symptoms.
What foods are good for fighting pancreatic cancer?
Fatty fish rich in omega-3s, cruciferous vegetables like broccoli and Brussels sprouts, turmeric, berries, citrus, and legumes are strong choices. Combining these within a low-glycemic eating pattern strengthens their overall effect.
What is a good meal for someone with pancreatic cancer?
Baked salmon with steamed sweet potatoes and cooked broccoli is a solid option. On days when solid food is hard to tolerate, a smoothie with spinach, berries, almond milk, and plant-based protein powder works well. Aim for meals that are soft, protein-rich, and low in added sugar.
What is a holistic diet for pancreatic cancer patients?
A holistic diet combines plant-forward, low-glycemic, anti-inflammatory, and omega-3-rich eating with targeted nutraceuticals. Some protocols, including NORI's, also incorporate methionine restriction to support the body's broader response to cancer alongside symptom management.
What is a superfood for the pancreas?
Broccoli (sulforaphane), turmeric (curcumin), and fatty fish like salmon (omega-3 EPA/DHA) are among the most studied foods for pancreatic health. All three have documented evidence of inhibiting pancreatic cancer cell growth and supporting immune response.


