
Introduction
Unintentional weight loss ranks among the most physically damaging challenges cancer patients face during treatment. Up to 33% of cancer patients overall meet cachexia criteria, with that figure climbing to 61%–87% in lung, pancreatic, and gastric cancers. This isn't about appearance—maintaining or regaining weight directly impacts treatment tolerance, immune function, and recovery outcomes. Without adequate nutrition, the body struggles on multiple fronts: chemotherapy side effects intensify, surgical wounds heal more slowly, and the immune system becomes less equipped to fight infection.
This guide provides practical, evidence-based strategies for gaining weight safely during cancer treatment. It covers what to eat, how to structure meals around treatment schedules, which factors make weight gain harder than expected, and the common mistakes that quietly set patients back.
TLDR
- Cancer-driven weight loss stems from reduced appetite, treatment side effects, and metabolic changes, not from eating too little
- High-calorie, high-protein foods form the foundation: healthy fats, full-fat dairy, nut butters, eggs, and legumes
- Eating 5–6 small scheduled meals works better than waiting for hunger signals that treatment has suppressed
- Drinking calories through smoothies and nutritional supplements helps when solid food feels impossible
- NORI's home-based program pairs patients with oncology nutrition specialists who customize dietary protocols for their specific cancer type and treatment plan
Why Do Cancer Patients Lose Weight?
Cancer-related weight loss has two primary drivers. First, treatment side effects—nausea, mouth sores, taste changes, fatigue—make eating difficult or unpleasant. Second, cancer itself triggers metabolic changes that increase caloric expenditure even at rest. Research shows approximately 50% of newly diagnosed cancer patients who are losing weight are hypermetabolic00079-0/fulltext), meaning their bodies burn more calories than expected based on activity level.
Understanding Cachexia
Cachexia represents a complex metabolic syndrome distinct from simple starvation. The 2011 international consensus defines cachexia as "ongoing loss of skeletal muscle mass that cannot be fully reversed by conventional nutritional support." Your body breaks down muscle and fat even when caloric intake seems adequate. Tumor-derived compounds trigger inflammatory cascades that accelerate protein breakdown and fat wasting. Unlike starvation—where the body preserves protein and burns fat—cachexia actively destroys lean muscle tissue.
Why This Distinction Matters
Understanding the metabolic nature of cancer-related weight loss sets realistic expectations. If you're experiencing cachexia, simply "eating more" won't fully reverse muscle loss. Strategic nutritional interventions make the difference:
- Prioritize protein to preserve lean muscle mass
- Maximize caloric density to overcome poor appetite
- Eat on schedule rather than waiting for hunger signals your treatment has suppressed
Working with an oncology-focused nutrition program helps align your plan with your specific cancer type and treatment regimen. NORI's personalized home-based support is designed exactly for this — giving patients practical, research-backed guidance without requiring clinic visits.
The Best Foods for Cancer Patients to Gain Weight
Focus on caloric density: maximum nutrition and calories in small volumes. Large portions often fail when treatment causes early fullness or low appetite. The four categories below — protein, fats, carbohydrates, and calorie boosters — each play a specific role in rebuilding weight without overwhelming a reduced appetite.
High-Protein Foods
Protein preserves lean muscle mass, which treatment puts at risk. ESPEN guidelines recommend protein intake above 1.0 up to 1.5 g/kg/day for cancer patients, with higher intakes supporting muscle maintenance during therapy.
Top protein sources:
- Eggs (whole eggs provide 6g protein plus healthy fats)
- Full-fat Greek yogurt (15-20g protein per cup)
- Cottage cheese (14g protein per half cup)
- Poultry and fish (25-30g protein per 4 oz)
- Legumes (beans, lentils: 15g protein per cup)
- Nut butters (7-8g protein per 2 tablespoons)

Note: NORI's specialized protocol uses a very low protein intake (under 0.3 g/kg/day), emphasizing plant-based sources to restrict methionine and cysteine — amino acids cancer cells require. Reducing protein intake in this way, without causing malnutrition, can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. If you're working with NORI, your customized plan will include cycled protein restriction that maintains weight while targeting cancer cells. Call 800-634-3804 for personalized guidance.
Healthy High-Calorie Fats
Fats deliver 9 calories per gram—more than double protein or carbohydrates. At that caloric density, fats become one of the most efficient tools for weight gain when appetite is limited.
High-calorie fat sources:
- Avocado (240 calories per whole avocado)
- Olive oil (120 calories per tablespoon)
- Nuts and seeds (160-200 calories per ¼ cup)
- Nut butters (190 calories per 2 tablespoons)
- Full-fat dairy products (whole milk, cheese, yogurt)
How to add fats without larger portions:
- Drizzle olive oil on cooked vegetables or pasta
- Add half an avocado to smoothies (adds creaminess plus 120 calories)
- Stir a tablespoon of almond butter into oatmeal
- Top soups with a dollop of full-fat sour cream
Smart Calorie-Dense Carbohydrates
Carbohydrates provide sustained energy and are easier to digest than high-protein foods when nausea strikes.
Best options:
- Oats (150 calories per ½ cup dry)
- Sweet potatoes (180 calories per medium potato)
- Rice (200 calories per cooked cup)
- Pasta (200 calories per cooked cup)
- Whole grain bread (80-100 calories per slice)
- Granola (300+ calories per half cup)
- Dried fruit (120 calories per ¼ cup)
A note on raw salads: Low-calorie, high-fiber vegetables fill you up quickly without contributing significant calories. Save them for when appetite improves and calorie-dense foods are already covered.
Calorie Boosters to Add to Any Meal
These "add-on" ingredients increase calories without requiring larger portions—especially useful on low-appetite days.
Practical boosters:
- Full-fat cream in coffee or soup (50 calories per tablespoon)
- Butter on vegetables or toast (100 calories per tablespoon)
- Grated cheese on eggs, pasta, or casseroles (110 calories per ounce)
- Honey drizzled on yogurt or oatmeal (60 calories per tablespoon)
- Powdered milk stirred into smoothies or mashed potatoes (25 calories per tablespoon)
- Protein powder in shakes or pancake batter (80-120 calories per scoop)
How to Structure Your Eating Day for Weight Gain
Meal structure matters as much as food choices when chemotherapy suppresses appetite. Treatment can eliminate hunger cues entirely, so waiting for them means missing critical calories.
Step 1: Shift to 5–6 Small Meals Per Day
Replace 3 large meals with 5–6 small, calorie-dense meals spaced 2–3 hours apart. The National Cancer Institute specifically recommends eating five or six small meals throughout the day rather than three large ones. Set phone reminders if needed. This reduces early fullness and ensures continuous caloric supply.
Sample daily schedule:
- 8:00 AM – Breakfast
- 10:30 AM – Mid-morning snack
- 1:00 PM – Lunch
- 3:30 PM – Afternoon snack
- 6:00 PM – Dinner
- 8:30 PM – Evening snack

Step 2: Front-Load Calories When Appetite Is Strongest
Many cancer patients have their best appetite in the morning or before afternoon fatigue sets in. Plan your most calorie-dense meal during this window. If mornings work best, make breakfast your largest meal—full-fat yogurt with granola and nuts, eggs with cheese and avocado toast, or a high-calorie smoothie.
Step 3: Drink Calories Between—Not During—Meals
Sip only small amounts of liquid during meals, then drink high-calorie beverages between meals. Fluids consumed with food cause early fullness, displacing solid calories.
High-calorie drink formula:
- 2 tablespoons nut butter (190 calories)
- 1 cup full-fat yogurt (150 calories)
- 1 banana (105 calories)
- 1 cup whole milk (150 calories)
- Total: ~600 calories in one smoothie
Step 4: Keep High-Calorie Snacks Accessible
Stock easy, no-prep options at home — low-energy treatment days make cooking unrealistic.
Essential snack stash:
- Trail mix with nuts and dried fruit
- Peanut butter and crackers
- Cheese sticks or cubes
- Protein bars (200+ calories)
- Full-fat yogurt cups
- Individual hummus packs with pita chips
Step 5: Build a Plan Around Your Specific Treatment
These steps form a solid foundation, but chemotherapy, radiation, and cancer type each create distinct nutritional needs that generic plans can't fully address. Personalized guidance helps align calorie and nutrient targets with what your body can actually tolerate during treatment.
NORI's home-based nutritional support program offers individualized weight-gain protocols developed through over 20 years of research in nutritional oncology. The program includes unlimited phone and Zoom support and nutraceuticals formulated and manufactured in-house. For a free initial consultation, contact NORI at 800-634-3804 or info@nutritionaloncology.net.
Key Factors That Affect Weight Gain During Cancer Treatment
Weight gain results vary significantly based on treatment type, cancer stage, and individual side effects.
Treatment Side Effects Require Specific Adjustments
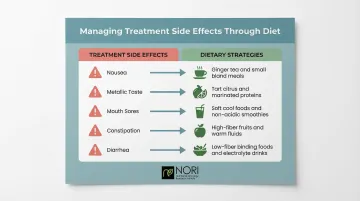
Each side effect demands a different dietary approach:
- Nausea: Cold or room-temperature foods tolerate better than hot meals — try smoothies, yogurt, cheese, or sandwiches.
- Metallic taste: Switch to plastic utensils and add strong flavors like lemon, pickles, or marinades. Cold foods typically taste more neutral.
- Mouth sores: Choose soft, bland options — mashed potatoes, scrambled eggs, oatmeal, or pudding. Avoid acidic, spicy, or crunchy foods.
- Constipation: Gradually increase fiber through oats, beans, and cooked vegetables.
- Diarrhea: Stick to bland, low-fiber foods like white rice, bananas, and toast until symptoms resolve.
Hydration Balance
NICE guidelines recommend 25–30 ml/kg/day of fluids for maintenance, with lower volumes (20–25 ml/kg/day) for older adults and those with heart or kidney issues. A 150-pound (68 kg) patient needs approximately 1,700–2,000 ml (7–8 cups) daily.
Timing and beverage choice both matter:
- Drink most fluids between meals, not during, to avoid displacing caloric intake
- Choose calorie-containing beverages — whole milk, 100% juice, or nutritional supplements — when drinking is easier than eating
Emotional and Psychological Factors
Research shows 33% of cancer patients experience depression and 31% experience anxiety, with malnutrition increasing depression risk more than threefold. These psychological factors — combined with treatment-associated food aversions — can significantly suppress intake on top of physical symptoms.
Caregivers directly shape the eating environment during this period. Don't force food, but do offer small portions frequently. Celebrate small victories — finishing half a smoothie is genuine progress.
Common Mistakes That Prevent Cancer Patients From Gaining Weight
Relying on "Healthy but Low-Calorie" Foods
Well-meaning patients fill plates with raw vegetables, light soups, and fruit because they're "healthy." During active treatment, caloric density must take priority. Large volumes of low-calorie food cause fullness without meeting caloric needs. A massive salad might contain 100 calories; a small serving of pasta with olive oil and cheese delivers 400+ calories in the same stomach space.
Waiting for Hunger Before Eating
Treatment commonly suppresses hunger signals entirely. A patient who eats only when hungry may go 12+ hours without nutrition. Scheduled eating is essential—your body needs fuel even when hunger signals fail. Set reminders and eat by the clock, not by appetite.
Using Hydration as a Substitute for Calories
Drinking large amounts of water, herbal tea, or broth during meals displaces caloric intake. Hydration still matters, but what you drink makes a significant difference. When drinking feels easier than eating, choose beverages that deliver calories alongside fluids:
- Smoothies made with full-fat dairy or nut butters
- Whole milk or fortified plant-based alternatives
- 100% fruit juice (no added water or sweeteners)
- Oral nutritional supplements such as Ensure or Boost

Frequently Asked Questions
What should cancer patients eat to gain weight?
Focus on high-calorie, high-protein foods: nut butters, full-fat dairy, eggs, avocado, olive oil, and calorie-dense carbohydrates like oats and sweet potatoes. Eat 5–6 small scheduled meals daily rather than waiting for hunger, and add calorie boosters like butter, cheese, or honey to increase intake without larger portions.
How does cancer cause weight loss?
Cancer-related weight loss stems from both reduced food intake (nausea, taste changes, fatigue) and direct metabolic effects. The cancer itself increases calorie expenditure and triggers inflammatory processes that break down muscle and fat—in advanced cases, this escalates into cachexia, a complex metabolic syndrome causing muscle wasting even with adequate caloric intake.
How do you gain weight during chemo?
Eat 5–6 small scheduled meals daily, prioritize calorie-dense foods, drink high-calorie smoothies between meals, and manage nausea with cold or bland foods. Consult an oncology dietitian or specialized nutritional support program like NORI's home-based service for guidance tailored to your specific treatment and side effects.
What can cancer patients eat to maintain weight?
Maintaining weight follows the same principles as gaining: calorie-dense foods, frequent meals, and enough protein. Eat on schedule even without hunger—focus on foods you tolerate well and add nutritional drinks when solid food feels challenging.
How many calories per day does a cancer patient need to gain weight?
ESPEN recommends total energy expenditure similar to healthy adults at 25–30 kcal/kg/day, with ASPEN recommending at least 30 kcal/kg/day for head and neck cancer patients. A 150-pound (68 kg) patient needs approximately 1,700–2,000 calories daily for maintenance, more for weight gain. Individual needs vary by cancer type and treatment intensity—consult a registered dietitian for personalized assessment.
Are nutritional supplements safe to use during cancer treatment?
Oral nutritional supplements are generally safe and often recommended when patients cannot meet caloric needs through food alone. However, antioxidant supplements during chemotherapy or radiation may reduce treatment effectiveness—always consult your oncologist before starting any supplement.


