
Introduction
Diet and nutrition account for approximately 5.1% of cancer deaths in the USA — yet most patients never receive a single dietary recommendation alongside their treatment. That gap persists despite growing evidence that what you eat directly influences cancer cell behavior, tumor growth conditions, and treatment outcomes.
This guide covers the science behind food and cancer biology, evidence-backed foods to prioritize, micronutrients with health-supporting properties, dietary patterns that fuel cancer growth, and practical steps for translating research into daily habits.
TLDR
- Cruciferous vegetables, berries, allium vegetables, flaxseed, and legumes deliver phytochemicals that strengthen cancer defenses
- Refined sugar, processed meats, alcohol, and ultra-processed foods drive inflammation and feed cancer cell growth
- Selenium, vitamin D, folate, and omega-3s are being researched for their roles in DNA stability, immune function, and cellular metabolic health
- Consistent, science-guided dietary choices can measurably reduce risk and support the body through treatment — no single food does it alone
Why What You Eat Can Influence Cancer Cell Behavior
Cancer cells exhibit distinct metabolic vulnerabilities that dietary choices can directly influence.
Cancer's Unique Energy Demands
Cancer cells rely disproportionately on glucose for energy, a phenomenon called the Warburg Effect. Unlike normal cells, they consume glucose through aerobic glycolysis and produce lactate even when oxygen is available. Diets that lower circulating glucose and insulin can restrict the fuel source cancer cells depend on most.
Many tumor cells also require dietary methionine to proliferate and cannot substitute other amino acids the way normal cells can (the Hoffman Effect). Restricting methionine disrupts the cellular machinery cancer cells need to divide, triggering cell cycle arrest in cancer models.
Inflammation Creates Tumor-Friendly Conditions
Chronic inflammation acts as fertilizer for cancer development. Diets high in processed foods, refined sugars, and certain fats promote systemic inflammation, tracked through the Dietary Inflammatory Index (DII). Higher DII scores associate with a 25% increase in overall cancer incidence and a 67% increase in cancer mortality.
Anti-inflammatory foods counteract this by reducing inflammatory cytokines and oxidative stress, creating a less hospitable environment for tumor development.
Hormonal Pathways Drive Cancer Growth
Excess calories and certain food compounds dysregulate insulin, IGF-1, and estrogen signaling. High-glycemic diets trigger elevated insulin levels, which amplify the activity of Insulin-like Growth Factor-1 (IGF-1). IGF-1 then activates growth-signaling pathways (PI3K/AKT/mTOR) that stimulate cell proliferation and sex-steroid synthesis — key drivers of breast and prostate cancer.
In plain terms: spiking blood sugar repeatedly signals your body to grow cells faster, including cancer cells. Red meat and alcohol compound this by elevating circulating estrogens and impairing folate metabolism.
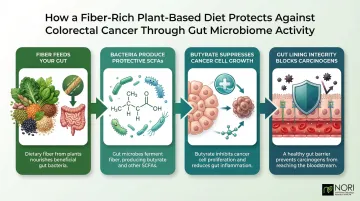
Your Gut Microbiome Shapes Cancer Risk
A plant-rich, fiber-heavy diet cultivates beneficial gut bacteria that produce short-chain fatty acids (SCFAs), particularly butyrate. Butyrate functions as a natural brake on cancer cell growth in the colon — it suppresses inflammatory signals and slows proliferation of colonocytes. Beyond butyrate, these bacteria also:
- Lower colon pH, making the environment less hospitable to cancer
- Reduce the activity of procarcinogenic enzymes
- Support the gut lining that prevents harmful compounds from entering circulation
Together, these effects make fiber intake one of the most consistently supported dietary factors in colorectal cancer prevention.
NORI's targeted approach: NORI's nutritional protocol applies cycled methionine restriction to exploit cancer cells' dependency on dietary methionine, combined with proprietary nutraceuticals developed in-house. Where general dietary guidelines address broad risk reduction, NORI's protocol targets the specific metabolic and epigenetic vulnerabilities outlined above — a focus shaped by over 20 years of translational research by founder Mark Simon and scientific advisor Dr. Robert Hoffman.
Top Cancer-Fighting Foods to Add to Your Plate
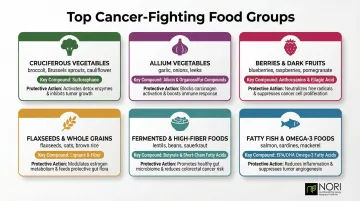
Six food groups stand out in the nutritional oncology research for their consistent, evidence-backed associations with reduced cancer risk:
- Cruciferous vegetables (broccoli, kale, Brussels sprouts)
- Allium vegetables (garlic, onions, leeks)
- Berries and colorful fruits (blueberries, tomatoes, cherries)
- Flaxseed (ground, not oil)
- Legumes and beans (black beans, lentils, chickpeas)
- Fatty fish and omega-3 sources
Cruciferous Vegetables
Broccoli, cauliflower, Brussels sprouts, cabbage, and kale contain glucosinolates that break down into sulforaphane and isothiocyanates when chopped or chewed. These compounds activate the body's detoxification defenses, block enzymes that allow cancer cells to grow, and affect cellular stress pathways being investigated in nutritional oncology research.
Epidemiological meta-analyses link cruciferous vegetable intake to reduced risks of lung, bladder, and prostate cancers. Notably, 3-day-old broccoli sprouts contain 10 to 100 times higher levels of glucoraphanin (sulforaphane's precursor) than mature broccoli plants, making them a highly concentrated source.
Preparation tip: Lightly steam or eat raw to preserve glucosinolates—excessive heat deactivates the enzymes needed to form sulforaphane.
Allium Vegetables
Garlic, onions, leeks, and scallions contain allicin and organosulfur compounds formed when these vegetables are crushed or chopped. High consumption is associated with reduced risk of gastric cancer (OR: 0.71) and colorectal cancer (RR: 0.80) across multiple meta-analyses.
Best preparation: Raw or lightly cooked garlic retains the most active compounds. Human pharmacokinetic studies show that key protective metabolites are 2 to 4 times lower in roasted or cooked garlic compared to raw.
Berries and Colorful Fruits
Blueberries, blackberries, raspberries, and cherries provide anthocyanins and ellagitannins — polyphenols that slow cancer cell growth and spread by interfering with multiple signaling pathways (including NF-κB and PI3K/Akt) that tumors rely on to survive.
Lycopene in cooked tomatoes has been specifically linked to reduced prostate cancer risk. In the Health Professionals Follow-Up Study, higher intake of tomato products and lycopene associated with lower prostate cancer risk in prospective cohort analysis.
Why cooked matters: Cooking tomatoes increases lycopene bioavailability by breaking down cell walls.
Flaxseed
Ground flaxseed is the richest dietary source of lignans — plant compounds metabolized into phytoestrogens that help regulate estrogen activity in the body. This matters for hormone-sensitive cancers in particular.
In a randomized trial of postmenopausal women with newly diagnosed breast cancer, 25g/day of dietary flaxseed reduced the Ki-67 tumor cell proliferation index by 34.2% and increased cellular stress pathway activity (30.7%) in ways being investigated in nutritional oncology research.
Key difference: Flaxseed oil lacks lignans and does not provide the same protective benefits — only ground flaxseed does.
Legumes and Beans
Black beans, chickpeas, and lentils provide fiber, folate, and resistant starch that support gut microbiome health. Research across multiple cohort studies indicates higher legume consumption is associated with decreased colorectal cancer risk (RR: 0.91). Gut bacteria ferment these foods to produce short-chain fatty acids like butyrate, which help protect the colon lining.
Fatty Fish and Omega-3 Sources
Marine omega-3 fatty acids (EPA, DHA) suppress pro-inflammatory pathways and may modulate BRCA1/BRCA2 gene expression. A meta-analysis of 21 prospective cohort studies supports a protective role against breast cancer incidence. Aim for 2-3 servings of fatty fish per week — salmon, mackerel, and sardines are among the richest sources.
Plant-based alternatives: Flaxseed and algae-derived DHA supply omega-3s for those avoiding fish. DHA and EPA are originally synthesized by marine microalgae, so algae-based supplements deliver them directly.
Key Anticancer Nutrients and Micronutrients
Selenium
Selenium activates antioxidant enzymes (glutathione peroxidase), supports natural killer cell function, has been investigated for its effects on cellular stress pathways, and is being researched for its role in metabolic health and cellular function. Multiple prospective studies demonstrated significant reductions in prostate, colorectal, and lung cancer incidence with adequate selenium levels.
Best source: Brazil nuts provide 68–91 mcg of selenium per nut—the densest dietary source. However, the SELECT trial found that 200 µg/day of isolated selenium supplements did not prevent prostate cancer in healthy men, a clear signal that whole-food sources outperform isolated high-dose supplements.
Vitamin D
Vitamin D's active form (1,25-OH2D) exerts anti-proliferative, pro-apoptotic, and anti-angiogenic effects on prostate, breast, colon, and pancreatic cells.
Ecological studies document a north-south gradient in cancer mortality tied to sun exposure — populations at higher latitudes show greater cancer mortality, linked directly to reduced endogenous vitamin D synthesis from less UV exposure.
Deficiency prevalence: NHANES data shows darker-skinned populations have significantly higher rates of vitamin D deficiency due to increased skin pigmentation reducing UV-mediated synthesis.
Folate
Folate (abundant in dark leafy greens) is essential for DNA methylation and synthesis. Low folate intake—particularly combined with alcohol consumption—significantly amplifies colorectal and breast cancer risk by increasing DNA strand breakage and genomic instability.
The alcohol interaction: Alcohol acts as a folate antagonist, compounding cancer risk even at moderate intake levels.
Chlorophyll and Carotenoids
Chlorophyllin binds and neutralizes dietary carcinogens. A randomized trial in Qidong, China demonstrated that 100 mg of chlorophyllin taken three times daily reduced urinary aflatoxin-DNA adducts by 55%.
Whole-food carotenoids offer a protective phytonutrient profile, including:
- Alpha-carotene and beta-carotene (orange and yellow vegetables)
- Lycopene (tomatoes, watermelon)
- Lutein and cryptoxanthin (leafy greens, citrus)
The ATBC and CARET trials found that high-dose beta-carotene supplements actually increased lung cancer incidence in smokers — the protective effect belongs to the whole food, not the isolated compound.

Foods and Dietary Patterns That Promote Cancer Growth
Sugar and Refined Carbohydrates
Cancer cells preferentially use glucose for energy (Warburg Effect). High glycemic load diets elevate blood glucose and insulin, creating conditions that support tumor growth. A comprehensive meta-analysis of 39 studies found that high glycemic load diets associate with significantly greater risk of colorectal cancer (RR = 1.26) and endometrial cancer (RR = 1.36).
Limit refined sugar, white bread, white rice, and processed snacks that spike blood glucose.
Red and Processed Meat
In 2015, the IARC classified processed meat as carcinogenic to humans (Group 1) and red meat as probably carcinogenic (Group 2A). Each 50g daily portion of processed meat increases colorectal cancer risk by 18%.
Mechanisms include:
- N-nitroso compounds formed during curing
- Heterocyclic aromatic amines formed during high-temperature cooking
- Heme iron, which catalyzes lipid peroxidation and endogenous nitrosation (internal formation of cancer-linked nitrosamines) in the gut
Practical limit: Minimize or eliminate processed meats (bacon, sausage, deli meats) and limit red meat to occasional small portions.
Alcohol
The IARC and WHO classify alcohol as a Group 1 carcinogen causally linked to at least 7 cancer types: oral cavity, pharynx, larynx, esophagus, liver, colorectum, and female breast.
Even moderate consumption increases breast cancer risk, particularly in women with low folate intake. Alcohol drives risk through several pathways:
- Impairs folate metabolism, reducing the body's ability to repair DNA
- Raises circulating estrogen levels, fueling hormone-sensitive cancers
- Generates acetaldehyde, a toxic metabolite that damages DNA directly
Excess Body Weight and Ultra-Processed Foods
Excess body fat increases risk of at least 13 cancers. In the US, excess body weight accounts for 7.1% to 11.4% of cancers among women and 3.9% to 6.0% among men.
The NutriNet-Santé prospective cohort study found that a 10% increase in ultra-processed food intake associated with a 12% higher risk of overall cancer and an 11% higher risk of breast cancer.
Excess adipose tissue drives these risks by producing pro-inflammatory cytokines, increasing circulating insulin and IGF-1, and elevating estrogens through aromatization in fat tissue.

How to Build a Cancer-Fighting Diet: A Practical Daily Framework
The Two-Thirds Plate Rule
Fill at least two-thirds of every meal with plant foods: vegetables, legumes, whole grains, and fruits. Prioritize variety to maximize phytonutrient diversity.
Practical tips:
- Choose frozen vegetables as a convenient, nutrient-equivalent option
- Select whole grains (brown rice, quinoa, oats) over refined grains
- Include a rainbow of colors daily—each color represents different protective compounds
Cooking and Preparation Habits That Matter
- Lightly steam or eat cruciferous vegetables raw to preserve glucosinolates — prolonged boiling destroys them
- Cook meats at lower temperatures, marinate with herbs, and avoid charring to reduce heterocyclic amine formation
- Choose olive oil or canola oil over saturated fats; minimize processed and packaged foods
- Crush or chop garlic and let it sit 10 minutes before cooking to activate allicin
For Cancer Patients: Beyond General Guidelines
General guidelines are a starting point. For cancer patients, a personalized approach that accounts for cancer type, stage, and treatment status can make a meaningful difference.
NORI's home-based nutritional support program offers individualized guidance using cycled methionine restriction and targeted nutraceuticals, developed through 20 years of focused cancer nutrition research. The program is designed to work alongside standard-of-care treatment, with continuous support included. Contact NORI at 800-634-3804 or info@nutritionaloncology.net for a free initial consultation.
Frequently Asked Questions
How can a health-supporting diet help stop cancer cells from growing?
Dietary strategies like reducing glucose and methionine availability, increasing anti-inflammatory phytochemicals, and supplying nutrients that support apoptosis can alter the metabolic environment in ways that slow or disrupt cancer cell proliferation. Diet should be used as part of a comprehensive approach, not as a standalone cure.
How can a health-supporting diet help you stay in remission from cancer?
A consistently anti-inflammatory, nutrient-dense diet helps regulate hormones, support healthy gut bacteria, and lower recurrence risk. Removing key dietary contributors to cancer recurrence — including sugar, processed meat, and alcohol — reduces the conditions that allow cancer to return.
What foods should you avoid when following a health-supporting diet?
Avoid processed and red meat, alcohol, refined sugar and high-glycemic foods, ultra-processed packaged foods, and refined grains. These promote inflammation, hormonal imbalance, or directly provide metabolic fuel that cancer cells exploit.
Can diet alone support cancer recovery?
No. Diet is a meaningful tool for reducing risk and supporting recovery, but it works best alongside medical treatment. Integrating therapeutic nutrition with clinical care gives patients a more complete approach than either strategy alone.
How does sugar affect cancer cell growth?
Cancer cells consume glucose at much higher rates than healthy cells — a phenomenon known as the Warburg Effect. Diets high in refined sugar and carbohydrates raise insulin and blood glucose levels, creating conditions that may fuel cancer cell proliferation and are linked to higher rates of colorectal, endometrial, and pancreatic cancers.


