
The truth is simpler: nutrition is one of the most powerful tools a breast cancer patient can control. This guide cuts through the noise with research-backed information on what to eat, what to avoid, how to manage eating during treatment, and how diet supports long-term outcomes.
While no single "breast cancer diet" can cure or prevent the disease, mounting evidence shows that food choices meaningfully influence risk, treatment response, and survival. The choices you make today can support your body's ability to fight cancer and improve your quality of life.
TLDR
- Mediterranean-style eating—vegetables, whole grains, legumes, and healthy fats—is linked to improved breast cancer outcomes
- Avoid alcohol, processed meats, saturated fats, added sugars, and fruit juices—all tied to worse outcomes
- Chemotherapy patients benefit from hydration, small frequent meals, and symptom-specific food choices
- Weight management is critical, particularly for postmenopausal women
- The NORI Protocol's methionine restriction targets cancer cell vulnerabilities that standard dietary guidelines don't address
How Diet Influences Breast Cancer Risk and Outcomes
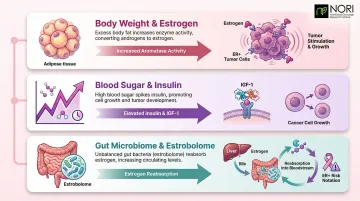
Diet affects breast cancer through three main pathways: body weight regulation, blood sugar control, and gut microbiome health.
- Body weight and estrogen: Excess fat tissue converts androgens to estrogens through a process called aromatization. This continuously stimulates hormone receptor-positive (HR+) tumors—especially in postmenopausal women—while also driving chronic inflammation that accelerates tumor progression.
- Blood sugar and insulin: Diets high in refined carbohydrates raise insulin and insulin-like growth factor 1 (IGF-1), both of which act as growth signals for cancer cells. This hormonal environment supports tumor proliferation across multiple breast cancer subtypes.
- Gut microbiome and estrogen recycling: Certain gut bacteria (collectively called the estrobolome) produce enzymes that reactivate estrogens the body has already processed for elimination. When reabsorbed, these estrogens raise circulating levels and may promote ER+ breast cancer development.
These mechanisms help explain why diet shows up consistently in survival data. A 2022 meta-analysis of 27,346 breast cancer survivors found that those eating high-quality diets had 21% lower all-cause mortality (HR = 0.79) than those with poor-quality diets. Survivors following patterns high in fruits, vegetables, and whole grains—and low in processed meats and saturated fats—showed consistently reduced death risk.
The research is still evolving, and no single food prevents or cures breast cancer. Consistent dietary patterns—not individual "superfoods"—are what move the needle on long-term outcomes.
Best Foods for Breast Cancer Patients
Vegetables and Fruits
Cruciferous vegetables and dark leafy greens offer the strongest evidence for reducing breast cancer mortality.
Broccoli, cauliflower, cabbage, and Brussels sprouts contain compounds that support detoxification pathways. Spinach, kale, and other dark greens provide folate, fiber, and antioxidants that protect cellular DNA.
Women eating the highest amounts of vegetables had 16% lower all-cause mortality (HR = 0.84) in the Nurses' Health Studies involving 8,927 breast cancer survivors.
The fruit juice problem: While whole fruits benefit breast cancer survivors through fiber and antioxidant content, fruit juices may be harmful. The same NHS analysis found that high post-diagnostic fruit juice consumption increased breast cancer-specific mortality by 33% (HR = 1.33) and all-cause mortality by 19%. Apple juice largely drove these risks, while orange juice showed no association.
Whole fruit is the better choice: its fiber slows sugar absorption and supports gut health, two benefits that disappear when fruit is juiced.
Fiber and Whole Grains
Dietary fiber protects against breast cancer through multiple mechanisms:
- Binds to estrogen in the gut, promoting excretion rather than reabsorption
- Regulates blood sugar, preventing insulin spikes that can fuel cancer growth
- Feeds beneficial gut bacteria that support immune function and reduce inflammation
For every 10 grams of daily fiber, breast cancer risk decreases by 4.7% (RR = 0.95), according to a 2022 meta-analysis.
The American Cancer Society and American Institute for Cancer Research recommend 25-35 grams of fiber daily for cancer prevention and survivorship.
Best fiber sources:
- Legumes: lentils, black beans, chickpeas, split peas
- Whole grains: quinoa, barley, oats, brown rice, farro
- Vegetables: artichokes, Brussels sprouts, broccoli
- Fruits: raspberries, pears, apples (with skin)
Healthy Fats and Anti-Inflammatory Foods
Not all fats are equal. Omega-3 fatty acids reduce systemic inflammation — a key driver of tumor progression — while saturated and trans fats promote it.
Research shows omega-3 supplementation in breast cancer survivors reduced fatigue and prevented increases in C-reactive protein (CRP), a key inflammation marker. Good sources include fatty fish (salmon, sardines, mackerel), walnuts, flaxseeds, and extra-virgin olive oil.
Mediterranean diet protection: Postmenopausal women closely following a Mediterranean diet showed 40% lower risk (HR = 0.60) of developing ER-negative breast cancer in the Netherlands Cohort Study. This protection is particularly important because ER-negative breast cancers historically have poorer prognoses.
The Mediterranean pattern emphasizes:
- Extra-virgin olive oil as primary fat
- Fatty fish 2-3 times weekly
- Abundant vegetables and fruits
- Whole grains and legumes
- Minimal red meat and processed foods

Soy and Phytoestrogens
Many breast cancer patients avoid soy, fearing its phytoestrogen content will fuel hormone-sensitive cancers. The research tells a different story.
Whole soy foods consumed in moderate amounts are associated with 26% reduced recurrence risk (HR = 0.74), particularly among postmenopausal and ER-positive survivors.
Important distinctions:
- Safe: Whole soy foods like tofu, edamame, tempeh, miso (1-2 servings daily)
- Avoid: High-dose soy supplements and isolated isoflavone extracts
The American Cancer Society and American Institute for Cancer Research confirm that moderate whole soy food consumption is safe for breast cancer survivors. The phytoestrogens in whole soy foods are much weaker than human estrogen and may actually block stronger estrogens from binding to receptors.
Key Nutrients: Calcium and Vitamin D
Beyond food choices, treatment itself can affect nutritional needs. Aromatase inhibitors and chemotherapy reduce bone mineral density, increasing fracture risk — making adequate calcium and vitamin D essential protective measures.
Chemotherapy-induced ovarian failure causes rapid bone loss — median decreases of 4.0% in the first six months and 3.7% from six to twelve months. Aromatase inhibitors cause additional annual bone loss of 1-2% at the hip and spine.
ASCO guidelines recommend 1,000-1,200 mg daily calcium and 800-1,000 IU daily vitamin D for cancer survivors at risk of bone loss.
Calcium sources:
- Low-fat dairy: yogurt, milk, cottage cheese
- Fortified plant milks: almond, soy, oat
- Sardines with bones
- Dark leafy greens: collards, kale, bok choy
- Calcium-set tofu and tempeh
Vitamin D sources:
- Fatty fish: salmon, mackerel, sardines
- Fortified foods: milk, plant milks, cereals
- Sunlight exposure (10-30 minutes several times weekly)
- Supplements (if levels are low)
Foods Breast Cancer Patients Should Avoid
Certain foods and beverages consistently show up in research as harmful for breast cancer patients — raising recurrence risk, driving inflammation, or disrupting hormonal balance. Here's what the evidence says to avoid.
Alcohol
The evidence is unambiguous: any level of alcohol consumption increases breast cancer risk and worsens outcomes.
The World Cancer Research Fund states there is no safe level of drinking for breast cancer prevention. In survivors, the news gets worse.
Drinking 3-4 alcoholic drinks per week increases recurrence risk by 35% (HR = 1.35) and breast cancer-specific death by 51% (HR = 1.51) in the Life After Cancer Epidemiology (LACE) study. The increased recurrence risk was even greater among postmenopausal women (HR = 1.51).
Recommendation: Avoid alcohol completely — no amount has been proven safe for breast cancer patients.
Saturated and Trans Fats
High-fat dairy products, red meat, processed meats, and fried foods contain saturated and trans fats linked to increased breast cancer mortality.
Women in the group with the highest trans fat intake faced 78% increased all-cause mortality risk (HR = 1.78) in the Collaborative Women's Longevity Study of 4,441 breast cancer survivors.
Foods to limit or avoid:
- Butter, full-fat cheese, whole milk
- Red meat (beef, pork, lamb)
- Processed meats (bacon, hot dogs, deli meats, sausages)
- Fried foods and fast food
- Packaged snacks with partially hydrogenated oils

Choose lean proteins (poultry, fish, legumes), low-fat or non-fat dairy, and healthy fats from plants and fish instead.
Added Sugars and High-Glycemic Foods
Cancer cells consume glucose preferentially — and high-glycemic diets exploit this by raising insulin levels and creating hormonal conditions that support tumor growth.
Higher post-diagnostic dietary glycemic load increased breast cancer-specific mortality by 33% (HR = 1.33) and all-cause mortality by 26% (HR = 1.26) in the Nurses' Health Studies analysis.
High-glycemic foods to minimize:
- White bread, white rice, refined cereals
- Pastries, cookies, cakes, candy
- Sugary drinks (sodas, sweetened teas, energy drinks)
- Processed snacks and packaged desserts
Replace these with whole grains, legumes, and whole fruits that release glucose slowly and don't spike insulin.
Processed and Ultra-Processed Foods
The Western diet pattern — refined grains, processed snacks, packaged foods high in additives — drives inflammation and weight gain, both key risk factors for recurrence.
Ultra-processed foods typically contain:
- Multiple ingredients not used in home cooking
- Added sugars, unhealthy fats, and sodium
- Artificial colors, flavors, and preservatives
- Minimal fiber, vitamins, or beneficial compounds
Better alternatives include fresh produce, whole grains, legumes, nuts, seeds, and lean proteins prepared at home — minimally processed and nutrient-dense.
Fruit Juices and Sweetened Beverages
Fruit juices lack fiber and spike blood sugar rapidly — survivor studies link them to higher mortality despite their "healthy" reputation.
Better choices:
- Water (plain or infused with lemon, cucumber, mint)
- Herbal teas (unsweetened)
- Sparkling water with fresh fruit slices
- Whole fruits eaten with meals or as snacks
Eating Well During Chemotherapy
Chemotherapy commonly disrupts normal eating through nausea, taste changes, mouth sores, fatigue, constipation, and diarrhea. The following symptom-specific strategies make treatment more tolerable.
Managing Nausea
Strategies that help:
- Eat small, frequent meals (5-6 times daily rather than 3 large meals)
- Choose cold or room-temperature foods, which have less odor
- Opt for bland, easy-to-digest options: plain crackers, toast, broth, bananas, plain rice
- Sip ginger tea or water between meals (not during meals)
- Avoid strong-smelling, greasy, or heavily spiced foods
Cold foods are better tolerated because heat releases volatile aromatic compounds that can trigger nausea. A cold sandwich generates less odor than a hot meal.
Managing Fatigue and Appetite Loss
Sustaining energy requires adequate protein at each meal, even when appetite is poor.
Practical approaches:
- Include protein at every meal: eggs, Greek yogurt, legumes, nuts, lean poultry
- Make nutrient-dense smoothies with fruits, vegetables, nut butter, and protein powder when appetite is low
- Avoid relying on high-sugar foods for quick energy—they cause blood sugar crashes
- Keep easy, protein-rich snacks accessible: nuts, cheese, hummus with vegetables

Staying Hydrated
Adequate hydration protects kidneys and bladder from chemotherapy drugs, reduces constipation, and manages fatigue.
Daily hydration targets:
- Aim for at least 8 cups of water daily, more on treatment days
- Add lemon, cucumber, or ginger if plain water is unappealing
- Sip consistently throughout the day rather than drinking large amounts at once
Supplements During Chemotherapy
High-dose antioxidant supplements can interfere with how chemotherapy works — an important consideration for anyone taking vitamins during active treatment.
Many anticancer agents work by generating reactive oxygen species that damage cancer cell DNA. High-dose antioxidant supplements (vitamins C, E, beta-carotene) can shield tumor cells from this oxidative stress, potentially reducing chemotherapy efficacy.
This concern is backed by patient data. The LACE (Life After Cancer Epidemiology) cohort study found that frequent use of combination carotenoids during chemotherapy increased breast cancer death risk (HR = 2.07) — a finding that underscores the need for caution.
Guidance: Consult your oncologist before taking any supplements during active treatment. Vitamin D supplementation may be an exception—discuss testing and appropriate dosing with your care team.
Food Safety During Treatment
Beyond what you take in supplement form, how you handle and prepare food also matters. Chemotherapy suppresses immune function, so food safety practices become essential during this period.
Safety practices:
- Avoid raw or undercooked meats and eggs
- Avoid unpasteurized dairy and raw sprouts
- Wash all produce thoroughly under running water
- Follow safe food storage practices (refrigerate promptly, check expiration dates)
- Avoid deli counters and buffets where food sits at room temperature
Managing Weight and Bone Health During Treatment
Weight gain is common during chemotherapy — steroids, reduced activity, and emotional eating all contribute. Unintended weight loss happens too, particularly with nausea or appetite changes. Both affect how well your body tolerates treatment and can influence long-term recovery.
The goal during treatment is to maintain a stable, healthy weight — not to actively diet. Post-treatment is the better window for addressing excess weight through gradual dietary changes, when your body has more capacity to adapt.
Practical weight management tips:
- Fill two-thirds of your plate with plant-based foods (vegetables, fruits, whole grains)
- Track food intake with a simple diary or app to identify patterns
- Eat mindfully without distractions (no television or phone)
- Limit liquid calories from juice and sweetened drinks
Protecting Bone Health
Treatment doesn't only affect weight — it can weaken bones too. Aromatase inhibitors and chemotherapy-induced early menopause both accelerate bone density loss, raising osteoporosis risk well beyond what's typical for your age.
Steps that help protect bone density during treatment:
- Weight-bearing exercise: walking, dancing, light resistance training
- Adequate calcium (1,000–1,200 mg daily) and vitamin D (800–1,000 IU daily)
- Discuss bone density screening with your oncologist to catch changes early
A Targeted Nutritional Approach: The NORI Protocol
Beyond general healthy eating, some nutritional strategies target cancer cell vulnerabilities more specifically. Methionine restriction is one such approach.
Methionine is an essential amino acid that cancer cells depend on disproportionately for growth. The Nutritional Oncology Research Institute (NORI) built its protocol around this vulnerability, with methionine restriction—achieved by limiting animal proteins—as the central dietary strategy, backed by over 20 years of focused research.
Cancer cells cannot adapt to methionine restriction the way healthy cells can. When deprived of methionine, cancer cells experience cell cycle arrest and death, while normal cells synthesize it from homocysteine. This selective vulnerability makes methionine restriction a meaningful therapeutic target in nutritional oncology.
That mechanism is the foundation of NORI's home-based support program, which translates the science into a practical, structured plan. The program includes:
- Cycled methionine restriction to exploit cancer cell vulnerabilities
- Proprietary nutraceutical formulations developed and manufactured in-house
- Personalized guidance tailored to each patient's cancer type and stage
- Unlimited support at one of the lowest costs in integrative cancer care

A 2018 case report documents a Stage IV ER+ breast cancer patient with bone metastases who reported bone pain subsiding within three months on the NORI Protocol, with tumor markers dropping from nearly 1,000 to 250.
NORI presents this approach as complementary to standard care, not a replacement. Patients can schedule a free initial consultation at 800-634-3804 or info@nutritionaloncology.net.
Frequently Asked Questions
What is the best diet for a breast cancer patient?
A predominantly plant-based diet inspired by the Mediterranean pattern offers the best outcomes: rich in vegetables, whole grains, legumes, healthy fats, and lean proteins while low in processed foods, alcohol, and added sugars. Individual needs vary based on cancer type, stage, and treatment.
What foods should breast cancer patients avoid?
Foods consistently linked to inflammation, weight gain, and worse survival outcomes include:
- Alcohol
- Saturated and trans fats (full-fat dairy, red meat, processed meats)
- Highly processed foods and added sugars
- High-glycemic carbohydrates and fruit juices
What should breast cancer patients eat during chemotherapy?
General nutrition strategies during chemotherapy include:
- Small, frequent meals with bland or cold foods to ease nausea
- Protein-rich options at each meal to maintain strength
- Consistent hydration (8+ cups of water daily)
Always consult your oncology team before taking supplements, as high doses can interfere with treatment.
What are the top 5 health-supporting foods?
Cruciferous vegetables (broccoli, Brussels sprouts), dark leafy greens (kale, spinach), fatty fish rich in omega-3s (salmon, sardines), berries and other antioxidant-rich fruits, and legumes (lentils, beans). No single food outperforms a consistently healthy overall dietary pattern.
Is soy safe for breast cancer patients?
Whole soy foods (tofu, edamame, tempeh, miso) consumed in moderate amounts (1-2 servings daily) are considered safe and may reduce recurrence risk by 26% based on current research. Avoid high-dose soy supplements, especially with hormone receptor-positive breast cancer.
Can diet help prevent breast cancer recurrence?
No diet guarantees recurrence prevention, but research shows that eating patterns high in vegetables, fiber, and whole grains — and low in processed foods and alcohol — correlate with a 21% lower mortality risk in breast cancer survivors. Consistent healthy eating improves long-term outcomes even when started after diagnosis.


