
This article addresses that gap directly. We'll cover what research actually shows about plant-based diets and cancer outcomes, the biological mechanisms involved, how to apply these principles during and after treatment, which nutritional gaps to watch, and how targeted protocols extend these foundations further.
One important note: nutritional oncology is still evolving. However, a growing body of research—including meta-analyses from major institutions—gives patients and clinicians meaningful, actionable guidance today.
TLDR: Key Takeaways
- Plant-predominant diets are recommended by major cancer organizations and linked to reduced cancer mortality
- Four mechanisms drive the benefit: lower inflammation, reduced IGF-1, protective fiber and antioxidants, and a healthier gut microbiome
- Post-diagnosis diet quality matters—what you eat after diagnosis influences survival, not just pre-diagnosis risk
- Nutritional gaps (B12, omega-3s, iron) require monitoring when following plant-based eating
- Advanced protocols like methionine restriction extend plant-based eating by targeting metabolic vulnerabilities in cancer cells
What Does "Plant-Based" Mean for Cancer Patients?
"Plant-based" isn't a single diet—it's a spectrum. The term encompasses vegetarian, vegan, Mediterranean, and whole-food plant-based (WFPB) patterns. The American Cancer Society encourages this framing, as does the World Cancer Research Fund/American Institute for Cancer Research (WCRF/AICR), because rigid labels create unnecessary barriers for patients already navigating a difficult journey.
That said, the label matters less than what ends up on the plate. Ultra-processed plant products don't carry the same protective benefits as whole, minimally processed foods. Chips, refined grain snacks, and plant-based fast food fall outside what the research actually supports—the evidence is built on whole foods.
All beneficial plant-based patterns for cancer patients share core features:
- Abundant fiber from whole grains, legumes, vegetables, and fruits—plus nuts and seeds for healthy fats
- Rich in phytochemicals and antioxidants from minimally processed plant foods
- Reduced or eliminated processed meat and red meat
- Limited saturated fat
What the Research Shows: Plant-Based Diets and Cancer Outcomes
Vegetarian and Vegan Diets
Large vegetarian cohort studies have produced nuanced findings. When pooled across studies covering over 139,000 participants, vegetarian versus non-vegetarian diets did not show a statistically significant reduction in overall cancer mortality (pooled HR approximately 0.97). Trends consistently favored vegetarians, though limitations in study size and dietary misclassification affected results.
Stronger signals emerged for specific cancers:
- Pancreatic cancer: Vegetarians and vegans had 52% lower mortality risk (HR 0.48; 95% CI: 0.28-0.82) compared to regular meat-eaters
- Lymphatic/hematopoietic cancers: 50% lower mortality risk (HR 0.50; 95% CI: 0.32-0.79) for vegetarians and vegans
A 2024 UK Biobank study of 472,377 participants found vegetarians had 14% lower risk of all cancers (HR 0.86; 95% CI: 0.80-0.93) compared to regular meat-eaters.
Mediterranean Diet Pattern
The Mediterranean diet produces the most consistent findings. A meta-analysis of studies covering nearly 2 million individuals found high versus low adherence to the Mediterranean diet was associated with 16% reduction in overall cancer mortality (HR 0.84; 95% CI: 0.79-0.89).
Important caveat: Most of these studies were conducted in general populations prior to diagnosis and did not control for cancer care regimens. The true independent dietary effect on cancer mortality is still being refined.
Post-Diagnosis Evidence
Those population-level findings are encouraging, but cancer patients need to know what the evidence shows after diagnosis. That data is more limited — yet consistently promising:
- Colorectal cancer: The German PopGen Biobank Study showed highest adherence to a modified Mediterranean diet post-diagnosis reduced all-cause mortality by 52% (HR 0.48; 95% CI: 0.32-0.74)
- Prostate cancer: The Health Professionals Follow-up Study found Mediterranean diet adherence reduced all-cause mortality by 22% (HR 0.78; 95% CI: 0.67-0.90), though prostate cancer-specific mortality did not reach significance
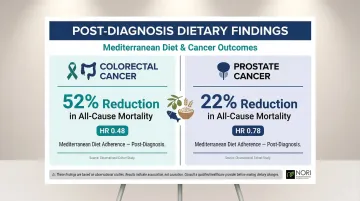
Only six post-diagnosis dietary pattern studies were identified in the most comprehensive rapid review to date — a striking evidence gap. What exists points in the right direction; what's missing is the large-scale, long-term intervention data that would let clinicians make firm recommendations.
The Biological Mechanisms: Why Plant-Based Eating May Fight Cancer
Inflammation and Immune Surveillance
Chronic low-grade inflammation drives cancer initiation, progression, and recurrence. Plant bioactives—including flavonoids, isoflavones, polyphenols, and omega-3 fatty acids from walnuts and flaxseed—suppress pro-inflammatory pathways including NF-κB activation.
Research shows plant-predominant diets are associated with significantly lower inflammatory biomarkers (CRP, fibrinogen) compared to Western dietary patterns. A meta-analysis found vegan diets reduced C-reactive protein levels by 0.54 mg/L on average.
Fiber, Gut Microbiome, and Short-Chain Fatty Acids
Fiber—present only in plant foods—feeds beneficial gut bacteria that produce short-chain fatty acids (SCFAs) such as butyrate. These have well-documented wellness-supporting effects:
- Support intestinal barrier integrity
- Regulate immune homeostasis
- Inhibit cancer cell proliferation through histone deacetylase (HDAC) inhibition
Due to the Warburg effect, cancerous colonocytes rely on glucose, allowing butyrate to accumulate in the nucleus where it functions as an HDAC inhibitor, has been investigated for its effects on cellular stress pathways in nutritional oncology research. This mechanism is particularly relevant for colorectal cancer but also influences systemic immune surveillance.
IGF-1 and Hormonal Pathways
Elevated insulin-like growth factor 1 (IGF-1) stimulates cell proliferation and is associated with increased risk of breast, prostate, and endometrial cancers.
Research shows vegan men have 9% lower serum IGF-1 concentrations than meat-eaters, and vegan women have 13% lower levels—likely driven by lower overall animal protein intake.
Antioxidants and Cancer Cell Oxidative Stress
Cancer cells generate elevated reactive oxygen species (ROS) that promote tumor development and metastasis. Plant-sourced antioxidants—carotenoids, vitamin C, vitamin E, phenolic acids—neutralize these free radicals and protect healthy cells.
During chemotherapy, these drugs themselves generate additional ROS. Antioxidant support from whole foods can help manage that oxidative burden without the risks associated with high-dose supplementation.
Important caution: The SWOG S0221 trial found breast cancer patients taking high-dose antioxidant supplements during chemotherapy were 41% more likely to have recurrence and 40% more likely to die. Get antioxidants from whole foods, not high-dose supplements during treatment.
Weight, Adiposity, and Hormonal Balance
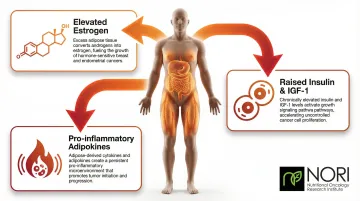
Excess adipose tissue produces estrogen (linked to breast, endometrial, and ovarian cancers), elevates insulin and IGF-1, and generates pro-inflammatory adipokines. Each of these effects independently promotes tumor growth. Plant-based diets consistently track with lower BMI and adiposity markers across study populations.
The connection matters clinically. The WCRF/AICR identifies overweight and obesity as a convincing cause of 12 cancers—making weight management one of the most evidence-backed modifiable risk factors in oncology.
Key mechanisms by which excess adiposity fuels cancer:
- Elevates circulating estrogen, driving hormone-sensitive cancers
- Raises insulin and IGF-1, stimulating cell proliferation
- Increases pro-inflammatory adipokines, sustaining chronic inflammation
Plant-Based Nutrition During and After Cancer Care
Eating Plant-Based During Active Treatment
Plant-based eating can complement active treatment. Anti-inflammatory phytochemicals may help manage treatment side effects, and fiber supports gut health disrupted by chemotherapy.
Practical adjustments are often needed:
- High-fiber foods may worsen diarrhea during certain treatments
- Citrus and acidic foods can irritate mouth sores
- Nausea may require flexible food choices
A plant-based approach during treatment should always be coordinated with your oncology care team. That coordination matters especially for protein, since cancer patients often have higher requirements than healthy adults. Legumes, soy products, whole grains, nuts, seeds, and nut butters can meet these needs on a plant-based plan.
Soy is worth highlighting specifically: multiple cohort studies link soy consumption to reduced breast cancer recurrence and improved survival, with breast cancer patients consuming ≥10 mg isoflavones daily showing 25% lower recurrence risk.
After Treatment: Recovery and Long-Term Prevention
Post-treatment nutrition can directly affect long-term survival outcomes. The American Institute for Cancer Research found that every 10-gram increase in daily fiber intake is associated with 16% reduced total mortality in colorectal cancer survivors.
WCRF/AICR post-diagnosis recommendations mirror their prevention guidelines:
- Emphasize whole grains, vegetables, fruits, and legumes
- Limit processed meats and red meat
- Minimize added sugar and alcohol
- Maintain a healthy weight with physical activity
Gut microbiome disruption from chemotherapy and antibiotics can persist well beyond active treatment. A fiber-rich plant-based diet is one of the most practical tools for supporting microbiome recovery during this period.
Key Nutritional Considerations for Cancer Patients on a Plant-Based Diet
Certain nutrients require attention and proactive planning:
Vitamin B12: Not naturally available from plant foods—supplementation is essential for all plant-based eaters, particularly important during treatment when red blood cell production and cellular oxygen delivery are critical.
Omega-3 fatty acids EPA and DHA: Both are lower in vegetarians and absent in vegan diets. Algae-based omega-3 supplements offer a direct plant-derived source — and NIH research confirms algal oil delivers DHA at bioavailability equivalent to cooked salmon.
Iron and zinc: Present in legumes, seeds, and whole grains but with lower bioavailability than animal sources (2-10% for non-heme iron vs. 25-30% for heme iron). Vitamin C consumed alongside plant iron sources improves absorption—increasing absorption from 10.4% to 27.4% with 150mg of vitamin C.

Work with a nutritional oncology specialist who can order and interpret relevant lab work (B12 levels, iron studies, omega-3 index, IGF-1, inflammatory markers) and tailor supplementation and dietary strategy to your cancer type, stage, and treatment plan.
That guidance is supported by mainstream oncology nutrition bodies. The American Cancer Society, WCRF/AICR, and Academy of Nutrition and Dietetics all affirm that well-planned plant-based diets are safe and beneficial for cancer patients—and the emphasis on "well-planned" is precisely what makes working with a specialist, not just following general advice, the difference between an optimized protocol and a risky gap.
Beyond the Basics: How Targeted Nutritional Protocols Build on Plant-Based Principles
Cancer cells have an abnormal metabolic dependence on the amino acid methionine. Unlike normal cells, they cannot synthesize it internally and rely entirely on dietary supply—a phenomenon known as methionine dependence (also called the "Hoffman effect"), first described by Dr. Robert M. Hoffman of AntiCancer Inc., who also serves as NORI's Scientific and Medical Advisor.
Plant foods are naturally far lower in methionine than animal proteins—plant-based proteins average 1.0% methionine compared to 2.5% in animal proteins. This is one of the underappreciated reasons plant-based diets may be health-supporting. However, a standard plant-based diet doesn't maximize this mechanism.
Structured nutritional protocols extend this effect by cycling periods of methionine restriction alongside specific nutraceuticals that exploit additional cancer cell vulnerabilities:
- Methionine cycling — timed restriction phases that starve cancer cells of a nutrient they cannot produce internally
- Targeted nutraceuticals — compounds selected to exploit vulnerabilities specific to cancer cell metabolism
- Precision sequencing — combining both approaches to amplify impact across multiple cancer types and stages
This layered strategy is the foundation of the NORI Protocol, developed through more than 20 years of research into nutritional oncology. It takes the principles behind plant-based eating and applies them with clinical precision.
Patients who want to move beyond general dietary guidance can explore personalized nutritional oncology support through NORI. The program is home-based, accessible worldwide, and includes a free initial consultation to assess how targeted nutritional strategies may fit your current treatment plan. Reach NORI at 800-634-3804 or email info@nutritionaloncology.net.
Frequently Asked Questions
Is a plant-based diet best for cancer patients?
No single diet is definitively "best," but plant-predominant, whole-food dietary patterns—especially Mediterranean and WFPB styles—are recommended by major cancer research organizations and associated with reduced cancer mortality in population studies. The key elements are high fiber, abundant phytochemicals, and reduced processed meat and saturated fat.
Do vegans get cancer less than meat eaters?
Large cohort studies show vegetarians and vegans tend to have lower incidence of specific cancers, including pancreatic and lymphatic types. Pooled data on overall cancer mortality has not consistently reached statistical significance, and healthy lifestyle factors common among vegetarians likely contribute to the observed differences.
What is the #1 cancer fighting food?
No single food prevents or treats cancer. Cruciferous vegetables (broccoli, Brussels sprouts, sulforaphane), legumes, berries, and whole grains are among the most consistently studied for cancer-protective properties. Research supports overall dietary patterns, not isolated foods, as the meaningful driver of risk reduction.
How to live longer with stage 4 cancer?
For advanced cancer, combining conventional care with evidence-based nutritional strategies—high plant-food intake, reduced inflammatory foods, adequate protein, and protocols like methionine restriction—may support quality of life and treatment response. A nutritional oncology specialist can help tailor this approach alongside your oncology team.
What happens after chemo ends?
The post-chemotherapy period is critical for rebuilding gut health, reducing inflammation, and lowering recurrence risk. Research shows post-diagnosis dietary quality—particularly fiber intake—is directly associated with improved survival outcomes, making a whole-food plant-based diet a practical priority during recovery.
Can you support cancer wellness twice?
Some patients do overcome multiple cancer diagnoses, with outcomes highly dependent on cancer type, stage, and overall health. Maintaining an anti-inflammatory, plant-predominant diet, healthy weight, and consistent follow-up monitoring are the most evidence-supported steps for reducing recurrence risk.


