
Introduction
Most people understand that diet affects cancer risk, but few grasp what the science actually demonstrates—or why specific plant compounds interact with cancer biology at the cellular level. The relationship goes far deeper than eating more vegetables or avoiding red meat. It involves precise biochemical mechanisms that either enable or restrict cancer cells' ability to survive and proliferate.
Those mechanisms have real consequences at scale. Cancer claimed 9.7 million lives globally in 2022 alone, making it one of the leading causes of death worldwide. Yet 37.8% of all cancer cases are attributable to modifiable risk factors, including diet, physical inactivity, and obesity. The World Cancer Research Fund (WCRF) and American Institute for Cancer Research (AICR) estimate that between 30–50% of all cancers are preventable through lifestyle changes, with diet playing a central role.
This article examines what research actually shows about plant-based diets and cancer incidence, the biological mechanisms driving those protective effects, and which foods carry the strongest evidence. One key finding runs through all of it: diet quality, not dietary labels, determines outcomes.
TLDR: Key Takeaways
- Plant-based dietary patterns, especially the Mediterranean diet, show measurable reductions in cancer risk across large population studies
- Key protective mechanisms include anti-inflammatory phytochemicals, gut-supporting fiber, pro-oxidant nutraceuticals being investigated for their interaction with cellular stress conditions, and lower IGF-1 from reduced animal protein intake
- Whole foods drive the benefit—refined grains and processed vegan products don't offer the same cancer-protective effects
- Research shows stronger evidence for reducing cancer incidence than for reducing cancer mortality
- No single food or diet pattern eliminates cancer risk—consistent dietary patterns over time matter most
What the Research Actually Shows: Plant-Based Diets and Cancer Risk
When evaluating dietary studies, it helps to distinguish between cancer incidence (new diagnoses) and cancer mortality (deaths). Plant-based diets reduce incidence more reliably than mortality — treatment type, cancer stage at diagnosis, and access to care all introduce noise into mortality outcomes.
Vegetarian and Vegan Diets
Large cohort studies provide the foundation for understanding how vegetarian and vegan diets affect cancer risk. A rapid review and meta-analysis found that vegetarian diets showed no statistically significant reduction in overall cancer mortality compared to non-vegetarian diets, with a pooled hazard ratio of 0.97 (95% CI: 0.88–1.06).
However, specific cancer types show stronger protective signals:
Cancer-specific findings from major cohorts:
- Lymphatic/hematopoietic cancers: Vegetarian diets associated with 36% risk reduction (HR 0.64, 95% CI 0.49–0.84) in EPIC-Oxford data
- Pancreatic cancer: 21% risk reduction (HR 0.79, 95% CI 0.65–0.97) among vegetarians
- Colorectal cancer: Pesco-vegetarians showed 43% risk reduction (HR 0.57, 95% CI 0.40–0.82) in the Adventist Health Study-2, while vegans showed a non-significant 16% reduction
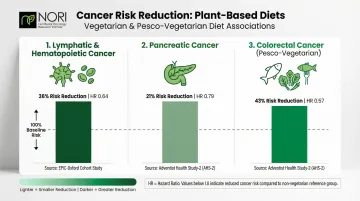
Strict veganism doesn't necessarily offer greater protection than semi-vegetarian or pesco-vegetarian patterns. What you eat within a plant-based diet matters more than whether you eliminate every animal product.
The Mediterranean Diet: The Strongest Plant-Based Evidence
The Mediterranean dietary pattern — abundant plant foods, olive oil, fish, moderate dairy, limited red meat — provides the most consistent evidence for cancer prevention. Unlike strict vegetarian diets, it covers potential nutritional gaps like omega-3 fatty acids and vitamin B12 while keeping plant foods at the center.
High adherence to the Mediterranean diet is associated with a 13% reduction in overall cancer mortality (pooled HR 0.87, 95% CI: 0.81–0.93). This finding holds across multiple scoring systems — the Mediterranean Diet Score, Alternate Mediterranean Diet, and revised Mediterranean Diet — and across diverse populations in Europe, the US, and Asia. Few dietary patterns have been validated this broadly.
For cancer survivors, the evidence extends beyond general health: post-diagnosis Mediterranean diet adherence has been associated with supportive wellness outcomes in observational research by 17% (HR 0.83, 95% CI: 0.70–0.99), with particularly strong evidence in colorectal and prostate cancer cohorts.
How Plant-Based Foods Protect Against Cancer: The Key Mechanisms
Population studies establish association, but understanding biological mechanisms explains why certain dietary patterns work and which foods deliver the strongest effects.
Phytochemicals and Antioxidants
Phytochemicals are bioactive compounds found exclusively in plant foods, offering two primary cancer-protective mechanisms:
Antioxidants neutralize free radicals that damage DNA and initiate cancer-promoting mutations. Unlike cancer cells, normal cells maintain balanced antioxidant systems that prevent excessive oxidative damage without supporting malignant growth.
Specific health-supporting compounds include:
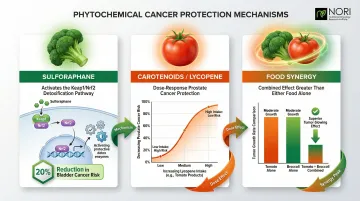
- Sulforaphane (cruciferous vegetables): Activates phase II detoxification enzymes via the Keap1/Nrf2 pathway, preventing DNA damage. Cruciferous vegetable consumption reduces bladder cancer risk by 20% (RR 0.80, 95% CI 0.69–0.92)
- Carotenoids (colorful produce): Lycopene from tomatoes shows dose-response protection against prostate cancer, with each 5mg daily increment reducing risk
- Food synergy: Combining tomato and broccoli proved more effective at slowing prostate tumor growth than either food alone, demonstrating that whole dietary patterns outperform single-nutrient approaches
Fiber, Gut Microbiome, and Immune Function
Dietary fiber operates through a two-tier protective mechanism. First, each 10g daily increment of fiber reduces colorectal cancer risk by 10% (RR 0.90, 95% CI 0.86–0.94) by physically accelerating waste transit through the colon, limiting carcinogen exposure to intestinal cells.
Second, fiber feeds beneficial gut bacteria that produce short-chain fatty acids (SCFAs), particularly butyrate. Butyrate has been investigated for its role in cellular health and reduces inflammation by blocking enzymes that allow cancer cells to multiply.
A fiber-rich plant-based diet increases microbiome diversity and SCFA-producing bacteria populations. Comparative studies between European children and rural African children on traditional high-fiber diets show the rural diet enriches Bacteroidetes species and substantially increases SCFA production — protecting against colonic inflammation, a primary driver of cancer development.
Inflammation, Hormones, and IGF-1
Obesity-driven chronic inflammation links diet to cancer through multiple pathways. Excess adipose tissue elevates circulating estrogen (driving breast and endometrial cancers) and increases insulin and insulin-like growth factor 1 (IGF-1), which promotes cell proliferation.
Elevated IGF-1 increases cancer risk across multiple cancer types:
- Breast cancer: 24% increased risk (HR 1.24, 95% CI 1.12–1.36)
- Prostate cancer: 20% increased risk (HR 1.20, 95% CI 1.10–1.30)
- Colorectal cancer: 21% increased risk (HR 1.21, 95% CI 1.08–1.36)
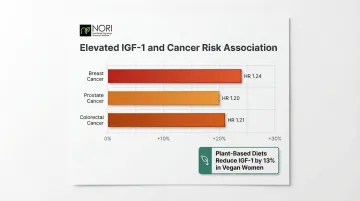
Plant-based diets reduce IGF-1 levels substantially. Vegan women show 13% lower serum IGF-1 compared to meat-eaters and vegetarians (P = 0.0006), with 20-40% higher levels of IGF-binding proteins that reduce IGF-1 bioavailability.
Plant foods rich in omega-3 fatty acids (walnuts, flaxseed), flavonoids, and polyphenols directly suppress inflammatory pathways, including the NF-κB transcription factor pathway that promotes cancer initiation and progression.
Methionine and Cancer Cell Vulnerability
Cancer cells exhibit abnormally high dependency on the amino acid methionine for survival and replication — a vulnerability normal cells don't share. Research suggests cancer cells may have distinct methionine dependencies, an area of ongoing nutritional oncology investigation.
Plant-based diets are naturally low in methionine, which concentrates in animal proteins:
- Beef (cooked): 905mg per 100g
- Pork chops: 850mg per 100g
- Tofu: 211mg per 100g
- Lentils: 146mg per 100g
Reducing protein intake — especially animal protein — without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. This three-part effect operates through two linked pathways: lower animal protein intake directly limits the methionine supply that tumor cells depend on for replication, and it also suppresses the IGF-1 signaling axis that drives cell proliferation across multiple cancer types. By restricting methionine and lowering IGF-1 simultaneously, a protein-modulated plant-based diet addresses cancer cell metabolism while preserving normal cell function. NORI (Nutritional Oncology Research Institute) has focused on methionine restriction for over 20 years, applying it as a core component of comprehensive nutritional protocols across various cancer types and stages. Preclinical models are investigating how methionine restriction interacts with cancer cell metabolism — an area that continues to attract growing interest in nutritional oncology research.
Which Plant Foods Offer the Strongest Cancer Protection?
Decades of epidemiological and laboratory research point to several food groups with the strongest, most consistent cancer-protective evidence:
Cruciferous vegetables (broccoli, Brussels sprouts, cauliflower, kale)
- Rich in sulforaphane and indole-3-carbinol
- Activate detoxification enzymes
- Show particular protection against bladder, prostate, and lung cancers
Allium vegetables (garlic, onions, leeks)
- High consumption reduces gastric cancer risk by 46% (OR 0.54, 95% CI 0.43–0.65)
- Contain sulfur compounds with anti-carcinogenic properties
Legumes and whole grains
- Provide fiber, resistant starch, and phytate
- Drive short-chain fatty acid (SCFA) production in the gut
- Lower colorectal cancer risk through multiple pathways
Colorful fruits and vegetables
- Carotenoids, flavonoids, and vitamin C
- Tomatoes (lycopene) particularly protective for prostate cancer
- Berries rich in polyphenols that inhibit NF-κB (a protein complex that drives inflammation)
Polyphenol-rich foods
- Green tea, olive oil, berries
- Anti-inflammatory and antioxidant properties
- Support immune surveillance against abnormal cells
No single food drives cancer protection on its own — the benefit comes from combining these groups consistently across meals. The WCRF/AICR recommends at least 400g (five portions) of non-starchy vegetables and fruits daily, plus at least 30g of fiber from whole food sources.
Why Diet Quality Matters More Than the Label
"Plant-based" doesn't automatically mean "cancer-protective." Refined grains, sugar-sweetened beverages, fruit juices, and highly processed vegan products are technically plant-derived but associate with worse health outcomes.
Research using plant-based diet quality indices shows that a 10-point increase in unhealthful plant-based diet score raises cardiovascular mortality risk by 8% (95% CI 2–14%), while healthful plant-based indices lower risk.
The standard pro-vegetarian score (simply measuring proportion of plant vs. animal foods) showed weaker cancer mortality associations than quality-adjusted scores. The shift away from animal foods matters less than the shift toward high-quality whole plant foods.
Western dietary patterns (high red/processed meat, saturated fat from dairy, refined foods) consistently correlate with elevated cancer risk:
- Breast cancer: 14% increased risk (RR 1.14, 95% CI 1.02–1.28)
- Prostate cancer: 34% increased risk (OR 1.34, 95% CI 1.08–1.65)
- Ultra-processed foods: a 10% increase in consumption raises overall cancer risk by more than 10%
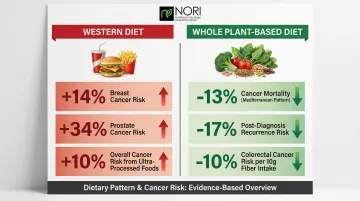
Populations consuming traditionally whole plant-based diets (rural China, traditional Asian populations) show substantially lower rates of breast and prostate cancers compared to Westernized populations.
Practical quality swaps:
- Choose whole grain bread over white bread
- Choose whole fruit over fruit juice
- Choose legumes and vegetables over processed vegan meat alternatives
- Choose water or unsweetened tea over sugar-sweetened beverages
- Choose nuts and seeds over refined seed oils in processed foods
Going Beyond Diet: Nutrition as a Comprehensive Cancer Strategy
While plant-based dietary patterns provide a powerful foundation for cancer prevention, diet alone doesn't fully address cancer cell biology. Structured nutritional protocols that combine dietary modification with targeted natural compounds go further—addressing the metabolic vulnerabilities that standard dietary guidance doesn't reach.
NORI (Nutritional Oncology Research Institute) has conducted over 20 years of research applying methionine restriction and nutraceutical strategies to support patients across various cancer types and stages. Their approach combines plant-based eating principles with targeted pro-oxidant natural compounds designed to support metabolic health in cancer patients by addressing their unique metabolic patterns. Pro-oxidant agents — including high-dose Vitamin C, piperlongumine, menadione, and certain carotenoids — are being investigated for their interaction with oxidative stress pathways and cellular health in nutritional oncology research. Cancer cells are known to have elevated oxidative stress — pro-oxidants are being investigated for how they may interact with these cellular conditions, with ongoing research into their selective effects. These pro-oxidant strategies are also being explored alongside conventional care approaches in ongoing nutritional oncology research.
Published case documentation illustrates the outcomes this approach can produce:
- A Stage IV papillary thyroid cancer patient reported near-undetectable tumor markers within three months using methionine-restricted diet combined with nutraceuticals, with stable markers maintained for over four years
- A Stage IV ER+ breast cancer patient with bone metastasis reported complete bone pain resolution within three months and tumor marker reduction from nearly 1,000 to 250
For individuals already diagnosed or at elevated risk, working with specialists in nutritional oncology ensures the strategy is calibrated to cancer type, stage, and treatment context. NORI offers free initial consultations as an accessible entry point.
That kind of individualized calibration matters especially when diet is combined with broader lifestyle changes. The Ornish Prostate Cancer Lifestyle Trial found that comprehensive intervention—plant-based diet, moderate exercise, stress management, and psychosocial support—produced measurable results in men with low-risk prostate cancer on active surveillance.
The intervention group achieved a mean PSA decrease while controls showed PSA increase. Serum from the intervention group also inhibited prostate cancer cell growth in vitro by 70%, compared to just 9% in controls (p < 0.001).
Frequently Asked Questions
What is 90% of cancer caused by?
Most cancers stem from environmental and lifestyle factors rather than inherited genetics—only 12% of cancers link to inherited gene changes. Modifiable factors include tobacco use, diet and obesity, physical inactivity, alcohol consumption, and carcinogen exposure, meaning a significant proportion of cancers may be supported through behavioral changes.
What stops cancer cells from growing naturally?
The immune system's surveillance function normally identifies and destroys abnormal cells before they develop into tumors. Plant-based diets support this through antioxidants, phytochemicals, and gut microbiome improvements that enhance immune function. They also moderate nutrients like methionine that research suggests cancer cells may rely on more heavily than normal cells.
What diet has the lowest cancer risk?
Dietary patterns built around whole grains, vegetables, fruits, legumes, and limited animal products are most consistently linked to lower cancer risk and mortality. The Mediterranean dietary pattern in particular shows a 13% reduction in cancer mortality across large population studies.
Can a plant-based diet help if you already have cancer?
Post-diagnosis diet quality shows real promise. Mediterranean-style eating has been linked to improved survival outcomes in people with colorectal and prostate cancer. That said, cancer patients should work with a nutritional oncology specialist to ensure any dietary approach fits their specific cancer type, stage, and treatment plan.
Do you have to go fully vegan to reduce cancer risk through diet?
No—research doesn't require strict veganism for cancer prevention benefits. The consistent finding is that greater proportions of whole plant foods and lower intake of red and processed meat correlate with lower cancer risk, making a plant-predominant approach both effective and sustainable.


