Yet most patients receive little specific dietary guidance alongside their treatment plan. You're told what drugs you'll take and when your appointments are, but rarely does anyone sit down and explain what to put on your plate. Nutrition is one of the few areas where patients have real agency — and it matters more than most people realize.
TLDR
- Build meals around plant proteins, healthy fats, colorful vegetables, and whole grains to maintain strength and reduce inflammation
- Avoid processed meats, alcohol, sugar-sweetened beverages, and ultra-processed foods that fuel inflammation and tumor growth
- Stay consistently hydrated — it supports toxin elimination and counters dehydration from treatment side effects
- Methionine restriction is an advanced dietary strategy that starves cancer cells of an amino acid they depend on but cannot synthesize
- Integrating these dietary principles alongside professional guidance gives your body its best nutritional foundation during treatment
How Cancer Treatment Affects Your Nutritional Needs
Chemotherapy, radiation, and immunotherapy don't distinguish between cancer cells and healthy, fast-dividing cells in your digestive tract, mouth, and gut lining. This non-specific targeting leads to wide-ranging side effects that directly disrupt eating.
The most common treatment-related eating challenges include:
- Nausea and vomiting
- Complete loss of appetite
- Taste and smell changes (metallic taste, food aversion)
- Painful mouth sores and throat irritation
- Constipation or severe diarrhea
- Crushing fatigue that makes meal preparation impossible
Each of these can reduce your ability to maintain adequate nutrition precisely when your body needs it most.
Cancer Patients Need More, Not Less
Cancer patients' dietary needs differ fundamentally from the general population. You often require more protein and calories, not fewer, to preserve muscle mass, support immune function, and sustain energy through treatment. European guidelines recommend 1.0–1.5 g/kg/day for protein and 25–30 kcal/kg/day for energy — well above general adult guidelines.
Different treatment types cause different weight outcomes. Steroid-based regimens for breast and blood cancers often cause weight gain and blood sugar swings. Pancreatic cancer commonly leads to malabsorption and weight loss, with up to 85% of patients experiencing significant weight loss at diagnosis — which is why nutritional guidance must be tailored to your specific treatment and cancer type.
The Food Safety Factor
The same treatments that strain your nutrition also suppress your immune system. In high-dose chemotherapy, 60%–100% of patients experience gastrointestinal side effects that compromise the intestinal barrier — making you far more vulnerable to foodborne illness than a healthy person. What you eat matters, but so does how safely it's prepared.
Top Foods to Add to Your Cancer Diet During Treatment
Plant-Based Proteins
Beans, lentils, chickpeas, tofu, edamame, nuts, and seeds deliver protein without the inflammatory compounds associated with animal proteins. Protein is essential for preserving lean muscle mass during treatment — but the source matters.
Plant proteins are naturally lower in methionine, an amino acid that cancer cells disproportionately rely on for growth. This metabolic vulnerability, known as the "Hoffman effect," sets plant-based protein apart from animal sources in a therapeutic context. Both supply amino acids, but plant proteins give cancer cells less of the fuel they rely on to replicate.
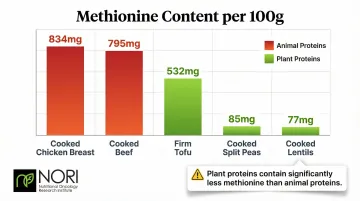
Consider these methionine differences per 100g:
- Cooked chicken breast: 834 mg
- Cooked beef: 795 mg
- Firm tofu: 532 mg
- Cooked lentils: 77 mg
- Cooked split peas: 85 mg
Colorful Fruits and Vegetables
Deeply colored produce — blueberries, red grapes, dark leafy greens, cruciferous vegetables (broccoli, cauliflower, Brussels sprouts), and orange-pigmented foods — are rich in phytonutrients and antioxidants that may reduce inflammation and support immune function. Cruciferous vegetables contain bioactive compounds that upregulate p53 tumor-suppressor genes and have been investigated for their effects on cellular stress pathways in certain cancer cells.
Aim for a variety of colors at each meal. Lightly cooked or steamed vegetables are often better tolerated than raw during treatment, especially if you're experiencing mouth sores or digestive sensitivity.
Healthy Fats
Avocado, olive oil, walnuts, flaxseed, and fatty fish (when tolerated) provide omega-3 and monounsaturated fats that combat inflammation and support cardiovascular health during treatment.
Omega-3 supplementation helps preserve lean body mass in cachectic patients and significantly reduces the incidence of severe chemotherapy-induced oral mucositis. At roughly 9 calories per gram, these fats help maintain body weight on days when eating feels difficult — a tablespoon of olive oil or a quarter of an avocado adds meaningful calories without requiring large portions.
Whole Grains
Minimally processed whole grains like oats, brown rice, quinoa, and whole wheat provide soluble fiber, B vitamins, and support for beneficial gut bacteria.
Soluble fiber promotes short-chain fatty acid production, particularly butyrate. Preclinical research shows that butyrate enhances intestinal barrier function and mitigates chemotherapy-induced gastrointestinal toxicity by maintaining epithelial integrity — potentially preventing severe diarrhea and weight loss.
Hydrating Foods and Fluids
Chemotherapy and radiation both stress the body's ability to stay hydrated — through nausea, vomiting, diarrhea, and reduced appetite. Replacing those fluids consistently is one of the most practical things you can do to reduce fatigue and support treatment tolerance.
Practical options to meet your daily 8–12 cup target:
- Water remains the best baseline — sip consistently rather than drinking large amounts at once
- Coconut water replaces electrolytes naturally after vomiting or heavy sweating
- Watermelon and grapes add fluid when solid food feels unappealing
- Drink between meals rather than with them to avoid feeling full before finishing eating
Foods to Avoid During Cancer Treatment
Processed and Red Meats
Processed meats are classified as Group 1 carcinogens by the International Agency for Research on Cancer, meaning there is sufficient evidence they cause cancer in humans. This category includes bacon, sausage, deli meats, and hot dogs.
Red meat is classified as probably carcinogenic (Group 2A). Both are linked to colorectal cancer risk and contribute to systemic inflammation. Each 50g daily portion of processed meat is associated with an 18% increase in colorectal cancer risk.
Both are also high in methionine and saturated fat. Elevated methionine availability is particularly relevant during treatment, as cancer cells rely heavily on methionine for growth — making dietary methionine restriction a meaningful therapeutic consideration.
Added Sugars and Ultra-Processed Foods
Sugar-sweetened beverages, packaged snacks, refined grain products, fast food, and commercially processed ready-to-eat meals are high in added sugars, refined carbohydrates, and unhealthy fats that drive inflammation.
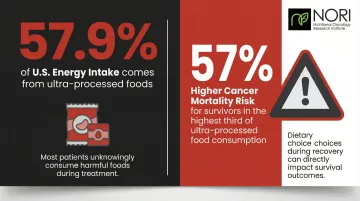
Ultra-processed foods comprise 57.9% of U.S. energy intake and contribute nearly 90% of added sugars consumed. A prospective study found that long-term cancer survivors in the highest third of ultra-processed food consumption faced a 57% higher risk of cancer mortality.
During treatment, the body has a heightened need for micronutrients and anti-inflammatory compounds. Calories from ultra-processed foods displace those sources while actively worsening the inflammatory environment treatment is trying to address.
Alcohol
Alcohol is classified as a Group 1 carcinogen, causally linked to at least eight types of cancer including oral cavity, pharynx, larynx, esophagus, liver, colorectum, and female breast. Ethanol metabolizes into acetaldehyde, which mediates genotoxic effects and DNA damage.
No safe intake level has been established for cancer patients. Avoid alcohol entirely during treatment.
Foods That Pose Food Safety Risks
Certain foods carry heightened contamination risk for immunocompromised patients:
- Raw or undercooked fish and shellfish (sushi, ceviche)
- Soft-cooked or raw eggs
- Unpasteurized dairy products
- Raw sprouts (alfalfa, clover, mung bean)
- Unwashed produce
Restrictive "neutropenic diets" that ban all raw fruits and vegetables are no longer recommended — they don't reduce infection rates but do worsen malnutrition. Proper washing and food handling guidelines are sufficient for most patients.
Managing Common Side Effects Through Diet
Nausea and Appetite Loss
When nausea strikes, shift to smaller, more frequent meals:
- Eat every 1–2 hours rather than three large meals
- Choose bland, room-temperature foods: crackers, plain rice, bananas, toast
- Sip ginger tea or try ginger chews
- Drink fluids between meals, not with them, to reduce fullness
- Try high-protein smoothies with Greek yogurt, protein powder, fruit, and vegetables when solid foods aren't tolerable
Taste Changes, Mouth Sores, and Swallowing Difficulty
For metallic or bland taste:
- Use plastic utensils instead of metal
- Marinate proteins in citrus or vinegar-based dressings
- Experiment with different seasonings
For mouth sores and swallowing difficulty, choose soft, cool, mildly flavored foods:
- Yogurt, scrambled eggs, mashed potatoes, smoothies
- Avoid acidic, spicy, crunchy, or very hot foods
- Puree or blend foods if swallowing is painful — soups, soft stews, and protein shakes work well
Constipation and Diarrhea
What you eat matters here — and the strategy shifts depending on the problem.
For constipation:
- Focus on high-fiber foods: whole grains, prunes, beans
- Drink hot beverages
- Ensure adequate hydration
For diarrhea:
- Shift to low-fiber, easy-to-digest options: white rice, baked chicken, bananas, cooked carrots
- Choose electrolyte-rich fluids
- Temporarily avoid raw vegetables, high-fat foods, caffeine, and alcohol
Beyond the Basics: What Nutritional Oncology Adds to the Conversation
Foundational dietary guidance — eat plants, avoid processed food, stay hydrated — provides a solid base. But emerging research in nutritional oncology has identified more targeted dietary strategies that specifically address cancer cell biology rather than just general health.
Methionine Restriction: A Metabolic Vulnerability
Cancer cells have an abnormal dependency on methionine, an essential amino acid found in high concentrations in animal proteins. Normal cells can adapt to low methionine conditions, but cancer cells cannot. Phase I trials show methionine-restricted diets are safe and can sensitize tumors to radiation.
Restricting dietary methionine through a primarily plant-based protocol may create a metabolic disadvantage specifically for cancer cells. Reducing protein intake — especially animal protein — without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. This approach goes beyond general nutrition by exploiting a specific cancer cell weakness.

Structured Support Programs
The Nutritional Oncology Research Institute (NORI) applies this science in a structured, home-based support program built on 20+ years of focused research. Their protocol combines cycled methionine restriction with targeted nutraceutical combinations across multiple cancer types.
The program is designed around practical accessibility:
- Free initial consultations via phone or Zoom
- Worldwide availability — no clinic visits required
- Ongoing support with no session limits
- Lowest-cost option among integrative cancer support programs
To learn more or schedule a consultation, contact NORI at 800-634-3804 or info@nutritionaloncology.net.
Frequently Asked Questions
What is the best diet for cancer patients?
A predominantly plant-based diet rich in vegetables, whole grains, legumes, and healthy fats is broadly recommended. Individual needs vary based on cancer type, treatment regimen, and side effect profile, making personalized guidance from an oncology dietitian important for optimal results.
What are the top health-supporting foods?
Cruciferous vegetables, dark berries, leafy greens, garlic, turmeric, green tea, and omega-3-rich foods are among the most studied for their anti-inflammatory and potentially cancer-supportive properties. Focus on variety and whole food sources rather than isolating single "superfoods."
How can cancer patients naturally boost their immune system?
Key dietary and lifestyle measures with research support include:
- Adequate protein intake to preserve muscle and immune function
- Antioxidant-rich plant foods and probiotic sources (yogurt, kefir)
- Sufficient hydration throughout the day
- Avoiding alcohol and ultra-processed foods
- Consistent sleep to support immune recovery
No single step is sufficient on its own. Staying consistent with the basics produces the most reliable results.
What are the best supplements for cancer patients?
Evidence for most supplements is limited, and some high-dose antioxidant supplements may interfere with treatment. Vitamin D is among the most commonly deficient and recommended. Any supplementation should be discussed with your oncologist before starting to avoid interactions.
Is protein powder safe for cancer patients?
Protein powder can be useful for patients struggling to maintain intake, particularly in smoothies when appetite is low. Animal-based protein powders tend to be high in methionine, which may be a concern depending on your protocol. Plant-based protein options are worth discussing with your care team.
What is the number one food linked to colon cancer?
Processed meat (bacon, hot dogs, deli meats) is the food most consistently linked to colorectal cancer risk through IARC Group 1 classification, followed by red meat. Limiting or eliminating both during and after treatment is recommended.