Most cervical cancers stem from persistent HPV infection, and emerging research shows diet plays a surprising role in how your immune system handles that infection. Certain foods can strengthen your body's ability to clear HPV and support recovery, while others create the inflammatory environment where cancer cells thrive.
This guide breaks down the science behind nutrition and cervical cancer, identifies specific foods that support your immune defenses against HPV, highlights what to avoid, and offers practical tips for eating well during treatment.
TLDR:
- Fruits, vegetables, and folate-rich foods strengthen immune defenses against HPV and reduce cancer risk
- Processed meats, refined sugars, alcohol, and fried foods fuel inflammation and should be minimized
- Vitamins A, C, E, and carotenoids show documented protective benefits in research
- Diet supports but never replaces medical treatment—it meaningfully improves recovery and quality of life
- Personalized nutritional guidance during active treatment delivers the best outcomes
Why Nutrition Matters for Cervical Cancer Patients
HPV causes almost all cervical cancers—but initial infection isn't the real problem. Persistent HPV infection is what drives cervical cancer progression. A well-nourished immune system is your first line of defense, and dietary deficiencies directly weaken that defense by increasing DNA damage and reducing immune cell function.
Oxidative stress—the same cellular damage that ages your cells—can activate transcription factors like AP-1 that promote HPV oncogene expression. These viral proteins (E6 and E7) are what transform normal cervical cells into cancerous ones.
Antioxidant-rich foods counteract this process directly, making diet an active part of cancer management—not just general wellness.
The population data is striking. A 2022 study of 558 women found that low intake of vegetables, fruits, and dairy was significantly associated with elevated cervical cancer risk—even after adjusting for age, BMI, family history, and HPV-related factors. Women consuming fewer than four servings of vegetables daily had a nearly 10-fold increased risk.

What nutrition can and cannot do:
Dietary changes won't cure cancer on their own. They're powerful adjuncts to medical treatment, not replacements. Good nutrition supports:
- Energy levels and treatment tolerance
- Immune function and tissue repair
- Reduced inflammation and oxidative stress
- Better management of treatment side effects
These benefits are why integrative oncology programs—including NORI's home-based nutritional support protocols—focus on diet as a targeted, research-backed component of cancer care, not simply a lifestyle recommendation.
Foods to Eat to Support Cervical Cancer Recovery
Fruits and vegetables are the cornerstone of any cancer-supportive diet. They supply antioxidants (vitamins C and E), carotenoids (beta-carotene, lycopene, lutein), and flavonoids that reduce viral load, suppress HPV-driven cellular changes, and reduce inflammation.
That protective effect shows up in the data: fruit intake alone was associated with meaningfully lower risk of invasive squamous cervical cancer in large prospective studies, with every 100-gram daily increase reducing risk by 17%.
Cruciferous and Dark Leafy Vegetables
Cruciferous vegetables deserve special attention:
- Broccoli, kale, cabbage, Brussels sprouts contain indole-3-carbinol (I3C) and sulforaphane
- I3C has documented wellness-supporting effects: A placebo-controlled trial found complete regression of cervical intraepithelial neoplasia (CIN II-III) in 50% of women taking I3C for 12 weeks, compared to zero in the placebo group
- Sulforaphane reverses tumor suppressor gene silencing by reducing DNA methyltransferase activity in cervical cancer cells
Dark leafy greens—spinach, romaine, kale—are rich in folate, which is critical for DNA repair and reducing HPV-associated cancer risk. Spinach delivers 193 mcg of folate per 100 grams, while kale provides 62 mcg.
Folate-Rich Foods
Folate's role in cervical cancer prevention is one of the most well-researched nutrition-cancer connections. Women with higher plasma folate levels (≥14.29 ng/mL) were 75% less likely to be diagnosed with CIN 2+ when they also had sufficient vitamin B12.
Folate supports DNA methylation and repair pathways that limit HPV's ability to alter cervical cell DNA. When folate is deficient, DNA damage accumulates—creating the conditions for cancer progression.
Top folate-rich foods:
- Lentils (358 mcg per cooked cup)
- Chickpeas and beans
- Avocados (205 mcg per cup, pureed)
- Orange juice (202 mcg per cup, frozen concentrate)
- Strawberries
- Dark leafy greens
Legumes, Whole Grains, and Fiber
Legumes—beans, lentils, chickpeas—and whole grains deliver:
- Fiber that supports a healthy gut microbiome and reduces systemic inflammation
- Folate for DNA repair
- Complex carbohydrates for steady energy (important during treatment-related fatigue)
A healthy gut microbiome supports immune function, regulates inflammation, and helps your body process nutrients efficiently—all of which matter during active cancer treatment.
Healthy Fats and Probiotic Foods
Adequate fat intake ties directly into the vitamins discussed above. Vitamins A, D, E, and K are fat-soluble, meaning your body needs dietary fat to absorb them—and all four play direct roles in immune surveillance and cervical cell health.
Include these in your daily meals:
- Walnuts and flaxseeds (omega-3 fatty acids)
- Olive oil
- Salmon and fatty fish
Probiotic-rich foods like Greek yogurt and fermented vegetables can support gut health during treatment, particularly when digestive disruption affects nutrient absorption.
Key Nutrients That Help the Body Fight HPV and Cervical Cancer
Four micronutrients show the strongest evidence for protective roles against HPV and cervical cancer progression.
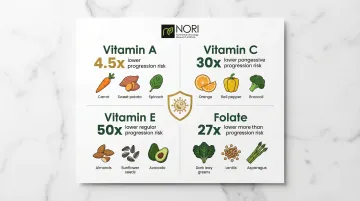
Vitamin A / Retinoids
Retinoids regulate cell growth and differentiation through retinoic acid receptors. They have been investigated for their effects on cellular stress pathways in cellular health research. Women with lower serum retinol are 4.5 times more likely to progress to carcinoma in situ or cervical cancer.
Food sources: Sweet potatoes, carrots, spinach, kale, cantaloupe, red peppers
Vitamin C
Ascorbate is a potent antioxidant that prevents malignant cell transformation, reduces chromosomal damage, and supports immune cell function. Higher intake (>224 mg/day) reduces cervical cancer risk by 47% (OR = 0.53).
Food sources: Citrus fruits, strawberries, bell peppers, broccoli, Brussels sprouts, tomatoes
Vitamin E (Alpha- and Gamma-Tocopherol)
Research shows increasing serum vitamin E concentrations are associated with significantly reduced CIN3 risk—74% lower for alpha-tocopherol and 54% lower for gamma-tocopherol. Vitamin E may counteract HPV's carcinogenic effects directly.
Food sources: Sunflower seeds, almonds, hazelnuts, spinach, avocados
Folate
Folate deficiency combined with high HPV DNA methylation increases the risk of severe cervical lesions (CIN3+) by 8.9-fold. Folate is essential for S-adenosylmethionine (SAM) synthesis, the primary methyl donor for DNA methylation.
Food sources: Dark leafy greens, lentils, black beans, asparagus, fortified grains
Carotenoids and Lycopene
Carotenoids—alpha-carotene, beta-carotene, lutein, zeaxanthin—and lycopene are powerful antioxidants that protect against DNA damage.
The protective effect is substantial across multiple measures:
- Increasing serum lycopene levels reduce CIN3 risk by 57% and invasive cancer risk by 83%
- High total carotenoid concentrations lower CIN3 risk by 61% and invasive cancer risk by 81%
Food sources:
- Lycopene: Tomatoes (especially cooked), papaya, red peppers, watermelon
- Beta-carotene: Carrots, sweet potatoes, butternut squash
- Lutein/zeaxanthin: Kale, spinach, corn, egg yolks
Food-First Approach vs. Supplements
These nutrient findings come from dietary studies, not supplement trials—and that distinction matters. Research on isolated antioxidant supplements for cancer is mixed; supplementing with individual vitamins hasn't consistently delivered the same protective effects seen in whole-food diets. The American Cancer Society recommends meeting nutritional needs through a balanced diet rather than supplements.
The whole-food matrix matters: fiber, phytochemicals, and synergistic nutrients work together in ways isolated supplements can't replicate.
Foods to Avoid with Cervical Cancer
Just as certain foods support recovery, others undermine it by promoting inflammation and weakening immune function. The categories below are the most significant offenders:
Processed and Red Meats
Processed meats—bacon, deli meats, sausages—and regularly consumed red meat create an inflammatory environment that works against treatment. They contain nitrates and other compounds that may promote cell damage.
Inflammation diverts immune resources and interferes with the body's ability to clear HPV. A Western diet high in red and processed meats is associated with higher HPV infection risk overall.
Sugary Foods and Refined Carbohydrates
Refined carbs and added sugars cause blood glucose spikes, triggering insulin release and creating metabolic conditions that support cancer cell survival.
Research shows dietary carbohydrates influence cancer cell survival through gene expression pathways. Cancer cells depend on glycolysis (a sugar-burning process) for growth. High-carb diets suppress AMPK—a cellular energy regulator that normally inhibits tumor growth—allowing cancer cell proliferation to accelerate.
They also displace the nutrient-dense foods your body needs for repair.
Alcohol and Processed Packaged Foods
Alcohol is particularly problematic for HPV-positive women. A study of 9,230 Korean women found drinkers with high HPV viral load had:
- 4.14 times higher risk of 1-year HPV persistence
- 6.61 times higher risk of 2-year HPV persistence
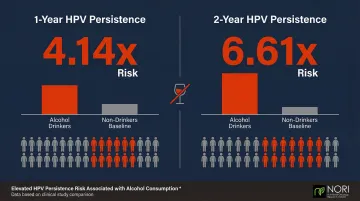
Alcohol impairs immune function and stresses the liver, which is already under pressure during treatment. It also depletes folate and triggers the production of reactive oxygen species—unstable molecules that damage cells and DNA.
Highly processed packaged foods are high in sodium, preservatives, and artificial additives that burden the liver while delivering few healing nutrients.
Fried and Greasy Foods
Fried foods are difficult to digest and require extra energy to process—a burden when your body is focused on healing. They worsen treatment side effects like nausea, bloating, and fatigue.
The trans fats and oxidized oils in fried foods promote systemic inflammation. Women in the highest quintile of trans fat intake had 73% higher C-reactive protein levels and 17% higher Interleukin-6 levels—both markers of inflammation.
Practical Dietary Tips During Treatment
Chemotherapy and pelvic radiation create unique nutritional challenges: nausea, digestive disruption, appetite changes, and fatigue. Here's how to maintain good nutrition despite these side effects.
Managing common side effects:
- Eat small, frequent meals to manage nausea; ginger tea and bland foods like oatmeal, bananas, and white toast are easier to keep down
- Boost calorie intake when appetite drops with avocados, nut butters, and smoothies blended with Greek yogurt and berries
- Sip liquids slowly and include probiotic foods like plain yogurt to ease digestive disruption; avoid heavy, fatty meals
- Pre-portion nutrient-dense snacks so fatigue doesn't lead to skipped meals
These adjustments help on rough days, but side effects vary widely by treatment type and individual. That's where professional guidance makes a real difference.
Work with a nutritional oncology specialist
General guidelines are a starting point, but personalized dietary plans account for your treatment type, side effect profile, weight status, and individual nutrient deficiencies. A nutritional oncology specialist can tailor recommendations to your specific circumstances.
NORI's home-based nutritional support program connects patients worldwide with personalized nutritional protocols built around their specific treatment plan. Continuous guidance and unlimited support are included, which matters when your needs shift from week to week during treatment.
Simple meal-building framework:
Use this template daily to ensure nutrient density:
- Fill half your plate with colorful vegetables and fruits — variety matters more than perfection
- Dedicate one quarter to whole grains or legumes: quinoa, brown rice, or lentils
- Use the remaining quarter for lean protein; if including animal protein, keep portions small
- Add a healthy fat like a drizzle of olive oil or a few slices of avocado

Example day of eating:
- Breakfast: Oatmeal topped with strawberries, blueberries, and ground flaxseed
- Snack: Carrot sticks with hummus
- Lunch: Lentil soup with spinach and tomatoes, side of whole-grain bread
- Snack: Orange slices and a handful of almonds
- Dinner: Quinoa bowl with roasted broccoli, bell peppers, chickpeas, and tahini dressing
Nutrient density and consistency are the targets. On difficult treatment days, even a small whole-food snack counts — every meal is an opportunity to support your body's recovery.
Frequently Asked Questions
What foods help fight cervical cancer?
Fruits, vegetables (especially cruciferous and dark leafy greens), folate-rich foods like lentils and avocados, and carotenoid-rich foods like tomatoes and sweet potatoes are the most well-evidenced dietary choices. They supply antioxidants and nutrients that support the immune system against HPV and reduce cervical cancer risk.
What foods should be avoided with cervical cancer?
Processed meats, refined sugars, fried foods, alcohol, and highly processed packaged foods undermine immune function and promote inflammation. Processed meats contain nitrates that damage cells; refined sugars support cancer cell metabolism; alcohol significantly increases HPV persistence; fried foods promote systemic inflammation.
What vitamins help fight HPV?
Vitamins A, C, and E, along with folate, have the strongest research support for limiting HPV persistence and slowing progression to cervical intraepithelial neoplasia. Food sources outperform isolated supplements: sweet potatoes and carrots (vitamin A), citrus and bell peppers (vitamin C), nuts and seeds (vitamin E), lentils and leafy greens (folate).
Can diet help clear an HPV infection?
Diet cannot guarantee clearance, but higher intake of antioxidant-rich foods and adequate folate levels are linked to better HPV clearance rates. Carotenoids and vitamins C and E appear to strengthen the immune response needed to resolve infection over time.
Does alcohol increase cervical cancer risk?
Yes. Research links regular alcohol consumption to significantly greater HPV persistence, particularly among women with high viral loads. Drinkers with high HPV levels face more than four times the risk of 1-year persistence and more than six times the risk of 2-year persistence compared to non-drinkers.
Diet won't replace medical treatment, but the research is clear: what you eat directly affects immune function, HPV persistence, and inflammation. Small, consistent changes add up — an extra serving of vegetables, whole grains instead of refined, less alcohol and processed food. Start there and build.
For personalized guidance tailored to your treatment plan and individual needs, contact NORI at 800-634-3804 or info@nutritionaloncology.net for a no-cost consultation.


