This growing interest isn't unfounded. Conventional cervical cancer treatments carry serious side effects: radical hysterectomy brings risks of urologic complications and nerve damage, pelvic radiation can cause premature ovarian failure and chronic gastrointestinal issues, and cisplatin chemotherapy causes nephrotoxicity and ototoxicity—in one study, 100% of patients showed significant hearing damage by six months. These toxicities, combined with the reality of treatment resistance, drive patients to seek gentler, less toxic approaches.
This article examines the scientific evidence behind natural treatment approaches for cervical cancer—from dietary patterns to specific plant compounds and nutrients. We'll explain honestly what the research supports and what it doesn't, helping you make informed decisions about complementary nutritional strategies.
TLDR
- HPV infection drives cervical cancer, but diet and nutrition measurably influence both HPV clearance and cancer progression risk
- 60+ plant-derived compounds show health-supporting activity in lab studies — curcumin, EGCG, thymoquinone, and resveratrol are among the most researched
- Up to 67% of women with cervical dysplasia show deficiencies in folate, vitamins C and D, beta-carotene, or selenium
- Natural approaches work best as complementary strategies supporting immune function and may enhance conventional treatment outcomes — not replace them
Why Patients Are Seeking Natural Cervical Cancer Treatments
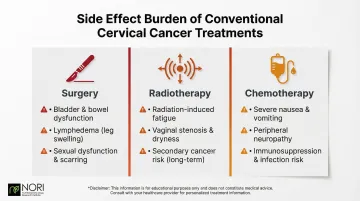
The side-effect burden of conventional cervical cancer treatment is substantial and well-documented. Each primary treatment modality carries its own documented harms:
- Surgery can cause intraoperative urologic complications, including bladder and ureteral injuries, plus postoperative genitourinary fistulas
- Radiotherapy triggers acute and late gastrointestinal toxicity, with vaginal stenosis occurring in over 60% of patients and premature ovarian insufficiency in premenopausal women
- Chemotherapy carries significant toxicity — cisplatin causes nephrotoxicity, neurotoxicity, and severe ototoxicity, while adding 5-fluorouracil increases grade 4 hematologic toxicities
Beyond toxicity, drug resistance creates a separate documented clinical gap. Cervical tumors frequently develop cisplatin resistance through upregulation of DNA repair mechanisms and altered copper transporters that reduce intracellular platinum accumulation. When cancer cells hijack normal repair pathways to survive chemotherapy-induced DNA damage, treatment fails and patients face likely relapse. Together, these two factors — toxicity and resistance — drive growing research into natural sensitizing agents that might restore chemotherapy effectiveness.
In this context, "natural treatment" means dietary patterns, whole-food nutrients, and specific phytochemical compounds — not unvalidated home remedies. The research base remains largely preclinical, but it's expanding with increasing scientific rigor.
How Diet Shapes Cervical Cancer Risk and Progression
The Inflammation-HPV-Cancer Connection
Diets high in added sugars, processed meats, and refined carbohydrates create chronic low-grade inflammation that impairs immune function. Women with the highest Dietary Inflammatory Index scores face triple the risk of developing high-grade cervical intraepithelial neoplasia (CIN2/3) compared to those eating anti-inflammatory diets. High glycemic loads specifically increase CIN1 risk nearly three-fold.
Inflammatory diets weaken the immune system's ability to clear HPV infections, allowing persistent infection to progress toward cancer.
By contrast, Mediterranean dietary patterns—high in colorful fruits and vegetables, legumes, healthy fats, and whole grains—show protective effects. Research in approximately 300,000 women found that a 100g daily increase in fruit intake reduces invasive squamous cervical cancer risk by 17%. Medium adherence to a Mediterranean diet is associated with a 60% reduction in high-risk HPV infection rates.
Antioxidant-Rich Diets, HPV Clearance, and Cancer Prevention
Antioxidants—including carotenoids (lutein, zeaxanthin, beta-carotene), vitamins C, E, and A, and lycopene—neutralize oxidative stress, support immune surveillance, and may suppress HPV-driven cellular changes. These nutrients work synergistically, not in isolation.
High serum levels of lutein, zeaxanthin, and lycopene significantly decrease clearance time of incident oncogenic HPV, particularly in the first 120 days of infection. Faster viral clearance prevents integration into host DNA—the critical step in carcinogenesis (cancer development).
Best dietary sources for cervical cancer prevention:
- Carotenoids: carrots, sweet potatoes, and squash
- Vitamin C: citrus fruits and peppers
- Folate: leafy greens, lentils, and avocados
- Indole compounds: broccoli, Brussels sprouts, and cabbage
- Organosulfur compounds: garlic and onions
What to limit:
- Added sugars (linked to increased risk across multiple cancer types)
- Red and processed meats (associated with elevated cervical cancer risk)
- Trans fats and excess saturated fats (promote tumor growth and disrupt the gut microbiome)

Plant-Derived Compounds with the Strongest Research Evidence
Polyphenols: Curcumin, EGCG, and Resveratrol
Curcumin (from turmeric) demonstrates powerful effects in laboratory models. Studies show it is being studied for its effects on cellular health in nutritional oncology research, stops cell cycle progression, and is being researched for its role in metabolic health and cellular function in cervical cancer cell lines and animal models. Key molecular targets include:
- Upregulating p53 (a tumor suppressor protein)
- Downregulating Bcl-2 (an anti-apoptotic protein)
- Inhibiting NF-κB (a pro-inflammatory signaling pathway)
The challenge? Curcumin's bioavailability is severely limited in standard supplemental form. Advanced delivery systems using nanoparticles and liposomal formulations show promise in preclinical studies by enhancing cellular uptake.
EGCG from green tea inhibits cervical cancer cell metastasis and proliferation by reducing MMP-2, MMP-9, and VEGF expression—proteins that drive tumor spread and blood vessel formation feeding tumor growth. EGCG represents one of the few natural compounds with both anti-metastatic and pro-apoptotic activity.
Where EGCG targets metastatic pathways broadly, resveratrol (found in grapes and berries) and its cousin pterostilbene work more specifically against HPV-positive cervical cancer. They inhibit the viral oncogene E6 and reduce tumor growth through cell cycle arrest—directly targeting the viral proteins that drive malignant transformation.
Thymoquinone, Indole-3-Carbinol, and Other Notable Compounds
Thymoquinone (from black seed/Nigella sativa) acts through multiple mechanisms: it has been investigated for its effects on cellular stress pathways in nutritional oncology research, inhibits cell migration and invasion, and suppresses epithelial-to-mesenchymal transition—a key step in metastasis.
It's also one of the few natural agents studied for effects on multi-drug resistance in cervical cancer cells, making it particularly relevant for patients who've encountered treatment resistance.
Indole-3-carbinol (I3C) and its metabolite diindolylmethane (DIM), both derived from cruciferous vegetables, are the most studied natural compounds in controlled human trials for cervical dysplasia. A small double-blind placebo-controlled trial found I3C (200-400mg daily) achieved complete regression in 50% of patients with CIN II-III, compared to 0% in the placebo group.
A subsequent trial of oral DIM (150mg daily) failed to show efficacy for low-grade lesions, attributed to poor oral bioavailability. Newer research using intravaginal DIM suppositories shows higher regression rates, suggesting delivery method matters significantly.
Key Nutrients and Supplements Linked to Cervical Cancer
Research consistently shows that nutritional status influences both HPV infection outcomes and cervical dysplasia risk. The evidence is strongest for a handful of specific micronutrients — though an important distinction runs through all of it: deficiency associates with higher risk, but supplementation has not been shown to reverse established disease.
The table below summarizes what the evidence currently supports for each key nutrient:
| Nutrient | Key Evidence | Clinical Limitation |
|---|---|---|
| Folate | Low red blood cell folate (≤660 nmol/L) combined with HPV-16 infection increases dysplasia risk fivefold; low dietary intake associates with up to nine-fold higher CIN3+ risk | Supplementation has not been shown to reverse established dysplasia or cancer — role is preventive, not therapeutic |
| Vitamins C, D & Beta-Carotene | One survey found abnormal vitamin levels in 67% of untreated cervical cancer patients, including significantly lowered plasma folate, vitamin A, and vitamin C | Randomized controlled trials have not confirmed supplementation reverses existing disease |
| Selenium | Deficiency associates with cervical dysplasia; observational data show multivitamin use in HPV-positive women correlates with less severe infection and lower progression risk | Evidence is observational only — no controlled trial has established therapeutic benefit |

These nutrients are best obtained through a food-first approach, with supplementation considered as an adjunct under practitioner guidance.
What Natural Approaches Can and Cannot Do: Setting Realistic Expectations
Understanding the Current Evidence Landscape
The large majority of research on plant compounds and cervical cancer consists of in vitro (cell culture) and animal model studies. These are scientifically valuable and informative, but they don't constitute clinical proof of efficacy in humans. A compound showing activity in a HeLa cell line cannot yet be recommended as a treatment, though ongoing research matters.
The translational gap is significant: compounds are rapidly metabolized and cleared from the body before reaching therapeutic concentrations in cervical tissue. Poor bioavailability, rapid metabolism, and lack of large-scale human clinical trials severely limit clinical application of even the most promising phytochemicals (plant-derived compounds).
Most promising research directions:
- Combination approaches (natural agents paired with conventional treatments as sensitizers)
- Anti-angiogenic plant compounds that restrict tumor blood supply
- MicroRNA-regulating compounds offering novel mechanisms
- Advanced delivery systems (nanoparticles, liposomal formulations) improving bioavailability
These represent areas where natural and conventional medicine may genuinely converge in future treatment protocols.
Building a Structured Nutritional Support Strategy
Understanding where the evidence falls short helps clarify what a realistic support strategy looks like. Rather than chasing individual compounds, the most evidence-consistent approach combines an anti-inflammatory dietary pattern, correction of key nutritional deficiencies, and targeted use of well-researched phytochemicals as adjuncts to medical care. A structured program offers more than any single supplement protocol.
For patients seeking this kind of structured nutritional support, the Nutritional Oncology Research Institute (NORI) offers home-based programs built on over 20 years of focused research. Their approach centers on methionine restriction dietary protocols combined with nutraceutical support — designed to work alongside, not replace, conventional care. NORI serves patients worldwide and offers free initial consultations for those exploring their options (800-634-3804 or info@nutritionaloncology.net).
Frequently Asked Questions
What are the early signs of cervical cancer?
Early cervical cancer is often asymptomatic, which is why regular Pap smears and HPV testing are critical. When symptoms occur, they may include abnormal vaginal bleeding (between periods or after intercourse), unusual discharge, or pelvic pain.
Can you live a long life after cervical cancer?
Many cervical cancer patients, particularly those diagnosed at early stages, achieve long-term remission and lead full lives. Five-year survival rates vary by stage: 91.4% for localized disease, 62.3% for regional spread, and 19.5% for distant metastases.
Can natural treatments replace conventional cervical cancer treatment?
Current evidence does not support using natural approaches as a standalone replacement for conventional treatment. They may meaningfully complement medical care by reducing inflammation, supporting immune function, and potentially improving treatment response.
What role does diet play in clearing an HPV infection?
A nutrient-dense, anti-inflammatory diet supports the immune system's ability to suppress and potentially clear HPV. Specific nutrients like folate, carotenoids, and vitamins C and D link to reduced HPV persistence in observational research.
Which plant compounds have the most research support for cervical cancer?
Curcumin, EGCG (from green tea), resveratrol, thymoquinone, and indole-3-carbinol are among the most studied, though most evidence comes from laboratory studies. Clinical trials in humans remain limited.
Is a nutritional protocol safe to use alongside chemotherapy or radiation for cervical cancer?
Some natural compounds have been studied as chemo-sensitizers and radio-sensitizers, suggesting potential synergy. However, any nutritional protocol should be discussed with your treating oncology team to avoid interactions and ensure safety.