
This article reviews current scientific evidence for natural and nutritional approaches to bone cancer care. We'll clarify what these interventions realistically can and cannot accomplish, examine plant-derived compounds showing measurable health-supporting activity, explore dietary strategies targeting cancer metabolism, and review natural approaches for pain relief. The goal is to help you make informed decisions alongside your medical team—not to replace conventional care, but to understand what complementary options exist.
We'll cover three key areas: plant-derived compounds with documented effects on bone cancer cells and bone-protective mechanisms, dietary strategies that exploit cancer cell vulnerabilities, and evidence-based natural approaches for managing pain and improving quality of life during treatment.
TLDR: Key Takeaways
- Plant compounds like curcumin, resveratrol, and omega-3s show health-supporting and bone-protective effects, with several advancing to clinical trials
- Dietary approaches including methionine restriction and anti-inflammatory eating target cancer cell metabolic weaknesses
- Acupuncture, omega-3 supplementation, and mind-body practices have clinical evidence supporting pain management and quality of life gains
- Natural treatments support—not replace—conventional oncology; always disclose them to your medical team to avoid harmful interactions
- Nutritional oncology programs pair targeted dietary protocols with nutraceuticals to address cancer cell vulnerabilities directly
Why Patients Look Beyond Conventional Treatment for Bone Cancer
Primary bone cancer—including osteosarcoma, chondrosarcoma, and Ewing's sarcoma—represents just 0.2% of all new cancer cases in the U.S., with 3,770 new cases projected for 2025. Far more common is metastatic bone cancer, where 70% of advanced breast and prostate cancer patients and 30–40% of lung cancer patients develop bone metastases.
Understanding the difference matters for treatment goals. Metastatic bone cancer is generally considered incurable with current standard therapies, making supportive and complementary care especially relevant.
The Vicious Cycle of Bone Metastasis
Bone metastasis creates a self-perpetuating problem driven by a three-step cycle:
- Tumor cells secrete factors that trigger osteoblasts to produce RANKL (receptor activator of nuclear factor kappa-B ligand)
- RANKL binds to osteoclast precursors, stimulating bone-destroying osteoclast formation
- That bone destruction releases growth factors that further fuel tumor growth—restarting the cycle
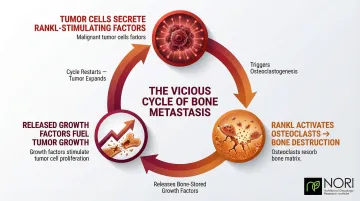
Each step in this process is a potential target for natural compounds.
Gaps in Conventional Treatment
Standard drugs like bisphosphonates (zoledronic acid) and denosumab target parts of this cycle, but their reach is limited. They effectively reduce skeletal-related events such as fractures and spinal cord compression by up to 40%, yet they are primarily palliative and don't consistently produce tumor regression in established bone metastases.
Side effects are common and significant:
- 66.4% of advanced cancer patients experience cancer-related pain
- 49–60% suffer cancer-related fatigue
- Approximately 50% develop chemotherapy-induced peripheral neuropathy
These limitations create genuine medical need for complementary strategies that can interrupt the bone destruction cycle while managing symptoms and supporting quality of life.
Plant-Derived Compounds with Evidence in Bone Cancer Research
Several botanical compounds have demonstrated measurable effects on bone cancer cells and bone-preserving mechanisms in laboratory and clinical studies.
Curcumin (Turmeric)
Curcumin suppresses osteoclast formation by inhibiting NF-κB and RANKL signaling—key pathways in the bone destruction cycle. In a mouse model of breast cancer bone metastasis, curcumin blocked TGF-β-stimulated PTHrP secretion, reducing osteolytic bone lesion area by up to 51%.
A Phase II trial in advanced pancreatic cancer found 8 g/day oral curcumin was well tolerated with no toxicities, though blood levels remained extremely low (22–41 ng/mL)—a direct consequence of poor absorption.
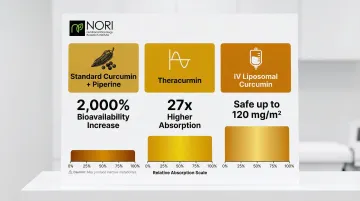
Standard curcumin is poorly absorbed, which limits its clinical usefulness. Advanced delivery methods address this directly:
- Piperine (20 mg, black pepper extract) increased bioavailability by 2,000%, though the resulting metabolites are largely inactive
- Theracurmin achieved 27-fold higher absorption compared to standard curcumin
- Intravenous liposomal curcumin proved safe up to 120 mg/m² in early trials
Resveratrol (Grapes, Berries)
Research published in Calcified Tissue International verified that structurally modified resveratrol analogues showed up to 5,000-fold increased potency to inhibit osteoclast differentiation compared to parent resveratrol.
Resveratrol promotes bone health through dual mechanisms: it blocks RANKL-induced osteoclast formation while promoting osteoblast differentiation and bone-building proteins like osteocalcin. This combination of slowing bone loss and supporting new bone formation is clinically relevant in metastatic disease.
Safety data is mixed. A Phase I trial of micronized resveratrol (SRT501) at 5 g/day in colorectal cancer patients with liver metastases showed good tolerance. However, a Phase II trial combining SRT501 with bortezomib in myeloma was halted due to renal failure—medical supervision is required before use.
Omega-3 Fatty Acids (EPA/DHA)
Meta-analyses show omega-3 supplementation significantly reduces inflammatory markers TNF-α and IL-6 in cancer patients. Standard oncology trial doses range from 1–4 g/day of combined EPA/DHA.
Evidence for cancer pain reduction is mixed. One randomized trial in breast cancer patients receiving paclitaxel found 4 g/day omega-3s did not significantly reduce pain compared to placebo.
On bleeding risk, a 2024 meta-analysis of 120,643 patients found omega-3s were not associated with increased overall bleeding risk, though high-dose purified EPA showed a modest 0.6% absolute risk increase. Patients on blood thinners should consult their oncologist before high-dose supplementation.
Plumbagin (Ayurvedic Medicine)
Plumbagin suppresses RANKL-induced NF-κB activation. In mice with breast cancer bone metastasis, plumbagin (2 mg/kg) significantly reduced the number and area of osteolytic bone lesions.
Important caution: Preclinical data shows a narrow therapeutic window with acute LD50 of 9.4 mg/kg in mice. Dose-dependent toxicity concerns require further study before clinical use.
Honokiol (Magnolia Bark)
In a mouse model of prostate cancer bone metastasis, honokiol (100 mg/kg) combined with low-dose docetaxel slowed tumor growth without added toxicity. The combination affected cellular processes being investigated in research while increasing cortical bone.
Honokiol inhibits platelet aggregation and prolongs bleeding time, requiring caution in patients with clotting disorders or those taking anticoagulants.
Dietary Strategies That Target Cancer Cell Vulnerabilities
Comprehensive dietary approaches can selectively stress cancer cells by targeting the metabolic differences that separate them from healthy tissue.
Methionine Restriction: The Scientific Rationale
Cancer cells exhibit "methionine dependence"—they cannot proliferate when methionine is replaced with its precursor, homocysteine, whereas normal cells remain unaffected. Restricting dietary methionine selectively stresses cancer cells.
This principle underlies structured programs like the NORI Protocol, which combines cycled methionine restriction (typically 7 days on, 7 days off) with targeted nutraceuticals. Oral recombinant methioninase converted docetaxel-resistant osteosarcoma to docetaxel-sensitive in patient-derived mouse models, demonstrating clinical potential.
Practical implementation: A plant-based diet high in fruits and vegetables naturally restricts methionine and cysteine (both abundant in animal proteins). Daily protein intake should be limited to less than 0.3 g/kg body weight, with fat restricted to under 10% of calories. Reducing animal protein in this way, without causing malnutrition, can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research.
Anti-Inflammatory Eating Framework
Inflammation promotes both tumor growth and bone resorption. An anti-inflammatory dietary approach emphasizes:
- Colorful vegetables and cruciferous plants (broccoli, kale, Brussels sprouts)
- Berries rich in polyphenols
- Fatty fish (if not restricting methionine)
- Minimizing processed foods, refined sugars, and omega-6 oils
This framework reduces systemic inflammation while providing nutrients that support bone health and immune function.
Soy Isoflavones and Bone Cancer
Research from Washington State University showed soy-derived genistein caused a 90% reduction in osteosarcoma cell viability in lab models while promoting healthy bone cell growth and reducing inflammation. The mechanism involves plant-based estrogens that impede cancer cell signaling without toxicity to normal cells.
Important nuance: While genistein shows promise, mixed soy isoflavones produced mixed results in breast cancer models—some formulations increased metastases. Compound selection matters: not all isoflavone formulations carry the same risk profile, and a clinician familiar with nutritional oncology should guide decisions here.
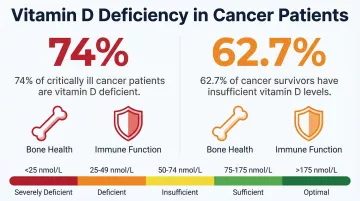
Vitamin D, Calcium, and Bone Support
Bone cancer patients face elevated fracture risk, compounded by widespread vitamin D deficiency. A study of critically ill cancer patients found 74% were vitamin D deficient (<20 ng/mL), with 62.7% deficiency among Korean cancer survivors.
Vitamin D's role extends well past bone mineralization. Vitamin D receptor expression is significantly decreased in bone metastases compared to primary breast tumors — a pattern that points to active health-supporting and immunomodulatory signaling.
ASCO guidelines recommend cancer survivors at osteoporosis risk consume 1,000-1,200 mg/day calcium and 800-1,000 IU/day vitamin D.
Practical Meal Planning
A registered dietitian or nutritional oncology program — such as NORI's home-based support service — can help develop:
- Nutrient-dense meals timed around treatment cycles
- Adequate protein from low-methionine sources when restricting
- Hydration support for kidney function during chemotherapy
- Individualized adjustments based on tolerance and response
Natural Approaches for Pain Relief and Quality of Life
Acupuncture for Cancer Pain
A systematic review in JAMA Oncology found acupuncture combined with analgesic therapy significantly reduced cancer pain intensity and decreased opioid dose by 30 mg morphine equivalent daily dose.
It works by stimulating specific points to trigger endorphin release, modulate pain signal processing in the central nervous system, and improve local blood flow.
Seek a licensed acupuncturist with oncology experience or certification from the Society for Integrative Oncology. Inform your oncologist before starting — especially if you're on blood thinners or have bone fragility from metastases.
Mind-Body Practices
A meta-analysis of 29 studies (3,476 participants) found Mindfulness-Based Stress Reduction (MBSR) significantly lowered anxiety, depression, fatigue, and stress while improving quality of life in cancer patients.
Practical options include:
- MBSR programs (typically 8-week structured courses)
- Daily meditation practice (10-20 minutes)
- Gentle yoga adapted for bone safety
- Deep diaphragmatic breathing (10 minutes, twice daily) — a clinical trial in metastatic gastrointestinal cancer patients showed it significantly reduced both acute and chronic pain scores, and it's especially useful before painful procedures

Heat, Cold, and Massage Therapy
Simple physical comfort measures can make a real difference day-to-day:
- Heat therapy (warm compresses, heating pads) eases muscle tension and chronic bone aching
- Cold therapy (ice packs) reduces acute inflammation and localized pain
- Therapeutic massage by a licensed oncology-trained therapist can lower anxiety and ease soft tissue pain
One consistent caution across all three: avoid applying heat directly over tumor sites, skip massage over known bone metastases or fragile bones, and get medical clearance before starting — particularly near metastatic lesions.
Used thoughtfully, these hands-on approaches complement other pain strategies and support a better overall quality of life throughout treatment.
How to Safely Integrate Natural and Conventional Treatments
Drug Interaction Awareness
Curcumin and several herbal compounds can affect drug metabolism pathways. Curcumin inhibits CYP3A4, CYP2D6, and CYP2C9, and oral curcumin activated CYP3A4 in rats, reducing immunosuppressant bioavailability by over 70%.
Key interactions to discuss with your oncologist:
- Curcumin affecting chemotherapy drug clearance
- Omega-3s at high doses increasing bleeding risk with anticoagulants
- Herbal compounds interfering with immunosuppressants
Never assume natural equals harmless. Disclose all supplements to your medical team.
Supplement Quality and Sourcing
Those safety conversations also depend on knowing what's actually in your supplements. The industry is largely unregulated, so quality varies widely. Look for products with:
- GMP (Good Manufacturing Practice) standards
- Third-party testing (USP, NSF, or similar verification marks)
- Transparent ingredient sourcing
NORI, for example, formulates and manufactures all its nutraceuticals in-house — giving patients direct traceability from ingredients to finished product.
When to Escalate to Your Medical Team
Contact your oncologist immediately if you experience:
- Sudden worsening of bone pain
- New neurological symptoms (numbness, weakness, difficulty walking)
- Signs of fracture (sharp pain, inability to bear weight)
- Unexplained weight loss exceeding 5% body weight
- Fever above 100.4°F (38°C)
Natural treatments do not replace monitoring and emergency medical care.
Frequently Asked Questions
How to get relief from bone cancer?
Relief typically combines conventional pain management (medications, radiation) with complementary approaches such as acupuncture, omega-3 supplementation, and mind-body practices. Working with both an oncologist and a palliative care or integrative medicine specialist gives you the most comprehensive symptom control.
How to strengthen bones with bone cancer?
Prioritize adequate vitamin D (800–1,000 IU/day) and calcium (1,000–1,200 mg/day), and engage in gentle weight-bearing activity as tolerated. Bisphosphonates under medical supervision help preserve bone density, and compounds like resveratrol and curcumin show preliminary evidence for supporting bone cell balance.
Is stage 4 bone cancer curable?
Stage 4 (metastatic) bone cancer is generally not considered curable with current standard therapies, but it can often be managed for extended periods. Outcomes depend on the primary cancer type, location, overall health, and treatment response—some patients achieve long-term stable disease with combined conventional and integrative approaches.
What does bone cancer pain feel like?
Bone cancer pain is often described as a deep, dull ache that may worsen at night or with activity. It can become sharp during weight-bearing and may be accompanied by swelling or tenderness. Pain that is persistent, progressive, or disrupts sleep warrants prompt medical evaluation.
Is bone cancer slow growing?
Growth rate varies significantly by type: chondrosarcoma tends to be slower growing, while osteosarcoma and Ewing's sarcoma are typically aggressive. Metastatic bone cancer's pace depends on the primary cancer's biology, so confirming the specific diagnosis is the first step in any treatment plan.
A note on integration: Natural approaches work best alongside conventional care, not in place of it. Stay transparent with your oncology team about all supplements and dietary changes, and remain alert to symptoms that need immediate medical attention. For patients interested in a structured nutritional oncology program, NORI offers home-based support combining methionine restriction with targeted nutraceuticals — reach them at 800-634-3804 for a free initial consultation.


