
This article reviews the most evidence-backed natural treatment options for bone cancer, clarifies what the research actually shows, and helps patients ask better questions of their care team. We'll examine plant-derived compounds with bone-specific mechanisms, nutritional strategies that target cancer cell vulnerabilities, and supportive therapies for pain and quality of life—all grounded in published research rather than speculation.
TLDR: Key Takeaways
- Plant compounds like curcumin, resveratrol, and plumbagin show health-supporting effects and bone-protective properties in preclinical studies
- Nutritional approaches targeting cancer metabolism—including methionine restriction—can exploit vulnerabilities in rapidly dividing cancer cells
- Omega-3 fatty acids, acupuncture, and mind-body practices are clinically supported for reducing bone cancer pain and easing treatment side effects
- Natural treatments work best alongside conventional care—always inform your oncologist before adding supplements
- NORI's nutritional oncology protocol combines dietary intervention with targeted nutraceuticals in a home-based program
Understanding Bone Cancer: Primary Tumors vs. Bone Metastases
The term "bone cancer" actually encompasses two distinct clinical scenarios. Primary bone cancers—including osteosarcoma, chondrosarcoma, and Ewing's sarcoma—originate in bone tissue itself and account for less than 1% of all cancers. In contrast, bone metastases occur when cancer cells from breast, prostate, lung, or other primary sites spread to bone.
Bone metastases are far more common than primary bone tumors, affecting:
- 88.74% of patients with metastatic prostate cancer
- 53.71% of patients with metastatic breast cancer
- 20–23% of patients with metastatic lung cancer
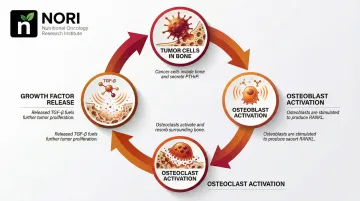
The Vicious Cycle of Bone Destruction
Bone metastasis creates what researchers call a "vicious cycle." Tumor cells in bone secrete parathyroid hormone-related protein (PTHrP), which stimulates bone cells to produce RANKL. RANKL activates osteoclasts—the cells that break down bone—releasing growth factors like TGF-β that fuel further tumor growth. This feedforward loop explains why bone metastases cause severe pain, fractures, and spinal complications.
Current treatments like bisphosphonates and denosumab can delay skeletal complications. In clinical trials, denosumab delayed the time to first skeletal-related event by 16–18% compared to zoledronic acid.
Yet despite that benefit, these agents don't consistently improve overall survival, and 45% of patients still experience fractures, spinal compression, or need for bone surgery. That persistent burden is why researchers are investigating complementary approaches — ones targeting the tumor microenvironment, osteoclast signaling, and inflammatory pathways through nutritional and natural agents.
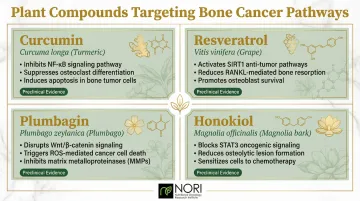
Plant-Derived Compounds: The Most Researched Natural Agents for Bone Cancer
Between 1940 and 2014, 49% of approved anticancer drugs were either unaltered natural products or natural product derivatives. Researchers have identified several plant compounds with specific mechanisms relevant to bone cancer and bone metastasis. The following compounds have the most substantial preclinical support.
Curcumin (from Turmeric)
Curcumin attacks bone cancer through multiple pathways:
- Blocks PTHrP secretion—a key driver of the bone destruction cycle
- Inhibits NF-κB activation, suppressing osteoclast formation
- Reduces TGF-β signaling in breast cancer cells
In mouse models of breast cancer bone metastasis, curcuminoids reduced osteolytic bone lesion area by up to 51% and decreased osteoclast numbers at the bone-tumor interface by 53%.
The bioavailability challenge: Oral curcumin is rapidly metabolized and eliminated. Free curcumin is rarely detected in plasma even at 10-12g doses. Clinical trials have tested 0.5g to 8g daily, finding good tolerability with mild side effects. Combining curcumin with 20mg piperine increases bioavailability by 2000%, while newer liposomal and micellar formulations are under investigation.
Evidence gap: No clinical trials have yet tested curcumin specifically for bone metastases in humans.
Resveratrol
This grape-derived compound offers bone-specific benefits:
- Inhibits RANKL-induced osteoclast differentiation
- Promotes osteoblast maturation, supporting bone formation
- Reduces RANK expression in monocytes and inhibits myeloma cell growth
Animal studies show dietary grape polyphenols inhibited spontaneous metastasis to bone in breast cancer models. A Phase I trial in colorectal cancer patients confirmed that micronized resveratrol at 5.0g daily for 14 days was well-tolerated, though recommended doses for ongoing use are 0.5-1.0g daily.
Clinical status: Resveratrol has not yet been tested in clinical trials targeting bone metastases directly.
Plumbagin and Honokiol: Emerging Evidence
Plumbagin (from Plumbago plants) works through mechanisms that parallel the curcumin pathway:
- Suppresses RANKL-induced NF-κB activation
- Inhibits osteoclastogenesis at the bone-tumor interface
In mice with breast cancer bone metastasis, plumbagin at 2mg/kg significantly decreased osteolytic lesions and preserved trabecular bone volume. Toxicity is dose-dependent — high doses cause liver and gastrointestinal damage. No human trials have been conducted.
Honokiol (from Magnolia bark) targets bone cancer through a different mechanism:
- Has been investigated for its effects on cellular stress pathways in prostate cancer cells and bone marrow cells
- Demonstrated synergy with low-dose chemotherapy in animal models
In mice with skeletal prostate cancer, honokiol (100mg/kg/day) combined with low-dose docetaxel inhibited tumor growth while preserving bone structure, suggesting potential as an adjuvant therapy. No clinical trials have been conducted for either compound.
Soy Isoflavones
Research from Wayne State University used 3D-printed bone scaffolds releasing soy isoflavones. Genistein caused a 90% reduction in osteosarcoma cell viability after 11 days while improving healthy bone cell growth. Separately, a meta-analysis found soy isoflavone intake >90mg/day for 6 months increased spine bone mineral density by 28.5mg/cm² in menopausal women.
Where research stands: The genistein findings are promising, but human trials targeting bone cancer have not yet been conducted.
Nutritional Strategies That Target Cancer Biology
Cancer cells have distinct metabolic dependencies—they overuse certain amino acids and nutrients to sustain rapid division. Nutritional strategies that target these dependencies aim to disrupt cancer metabolism while sparing healthy cells.
Exploiting Serine Dependency in Osteosarcoma
Research from Washington University showed that osteosarcoma cells exhibit high expression of PHGDH, the rate-limiting enzyme in serine biosynthesis. When researchers blocked this pathway, osteosarcoma cells stopped dividing. Combining PHGDH inhibition with an mTORC1 inhibitor created synergistic cell death, suggesting that disrupting cancer's energy production pathways can be amplified by blocking survival signals.
Methionine Restriction: Targeting a Cancer-Specific Vulnerability
Cancer cells are highly dependent on methionine, an essential amino acid, due to their elevated metabolic activity and abnormal epigenetics. Normal cells can survive on restricted methionine levels, but cancer cells cannot. This vulnerability is known as the "Hoffman effect."
A low-methionine diet in humans achieved a 60% reduction in serum methionine within 3 weeks, demonstrating the practical feasibility of this approach.
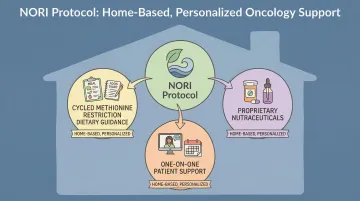
NORI's approach: The NORI Protocol implements cycled methionine restriction—alternating periods of restriction with regular eating. This is combined with targeted nutraceuticals designed to work synergistically with the dietary restriction. The protocol focuses on a plant-based diet naturally low in methionine, limiting protein to less than 0.3g per kilogram of body weight daily.
Anti-Inflammatory Diet Framework
Chronic inflammation drives both cancer progression and bone destruction. The key principles:
- Colorful whole plant foods rich in antioxidants and phytonutrients
- Omega-3-rich foods: fatty fish, walnuts, flaxseed
- Cruciferous vegetables: broccoli, cauliflower, Brussels sprouts
- Eliminate processed foods, refined sugars, and pro-inflammatory oils
Mediterranean dietary patterns significantly reduce inflammatory biomarkers, including IL-6 and IL-1β — both cytokines implicated in bone destruction in metastatic disease.
Foods to Avoid for Bone Cancer Patients
- Processed meats and high-fat animal proteins — high in methionine and pro-inflammatory compounds
- Refined sugars and high-glycemic foods — cancer cells preferentially consume glucose through glycolytic metabolism
- Alcohol — impairs both bone health and immune function
Patients on certain chemotherapy drugs should also avoid grapefruit and supplements that affect drug metabolism—always check with your oncologist.
The Malnutrition Challenge
Dietary restriction only works if patients maintain enough calories and nutritional quality to sustain treatment. That balance is harder to strike than it sounds: malnutrition and cachexia affect 30% to 85% of cancer patients, with rates highest in advanced solid tumors. Practical steps to manage this risk include:
- Tracking total caloric intake alongside protein restriction targets — reducing animal protein without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research
- Prioritizing protein quality (not just quantity) to preserve lean mass
- Working with a nutritionist experienced in oncology to adjust the protocol as needs change
Supportive Natural Therapies for Pain Relief and Quality of Life
Omega-3 Fatty Acids
EPA and DHA reduce pro-inflammatory prostaglandins and cytokines—major drivers of bone cancer pain. These omega-3s alter membrane composition and generate pro-resolution mediators that actively halt inflammation.
That anti-inflammatory effect translates to clinical use: oncology trials commonly use doses up to 5g/day of combined EPA/DHA. While standard omega-3 supplementation doesn't increase overall bleeding risk, high-dose purified EPA (4g/day) increased serious bleeding events from 2.1% to 2.7% in the REDUCE-IT trial. Patients on anticoagulants should discuss omega-3 dosing with their doctor before starting.
Acupuncture
Systematic reviews confirm acupuncture combined with conventional pain medication significantly improves pain relief in cancer-induced bone pain. It works by stimulating endorphin release and modulating pain processing pathways—making it a strong complement to medication rather than a standalone treatment. Seek licensed practitioners with specific oncology experience for the best outcomes.
Mind-Body Practices
Where acupuncture addresses physical pain pathways, mind-body practices work on the psychological and behavioral dimensions of suffering. Meditation, mindfulness-based stress reduction (MBSR), and gentle yoga provide evidence-supported benefits for:
These approaches require no equipment or clinic visits and can be implemented at home—a practical advantage for bone cancer patients managing pain-related movement limitations.
Integrating Natural Treatments with Conventional Care: Safety and Realistic Expectations
The Complementary Framework
No natural treatment has been proven to cure bone cancer or replace standard-of-care therapies. The strongest evidence positions natural agents as tools that may enhance treatment effectiveness, reduce side effects, protect bone integrity, and improve quality of life when used thoughtfully alongside conventional treatment.
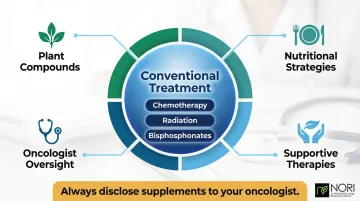
Critical requirement: Patients must explicitly disclose all supplements to their oncologist. Many natural compounds interact with cancer drugs.
Drug Interactions and Safety Flags
| Compound | Key Interactions | Evidence |
|---|---|---|
| Curcumin | Inhibits CYP3A4, CYP2D6, UGTs, P-gp | A Phase I trial combining up to 4g/day curcumin with irinotecan showed no significant alteration in drug levels or toxicity |
| Berberine | Inhibits CYP3A4, CYP2D6, CYP2C9, P-gp | Clinical case reports document significant INR elevation and bleeding risk when combined with warfarin; can potentiate blood sugar lowering |
| High-dose Omega-3 | Platelet aggregation inhibition | May increase bleeding risk, particularly at doses of 4g/day or higher |
| Green Tea Extract | Hepatotoxicity at high doses | EGCG doses ≥800mg/day are associated with liver enzyme elevations |
Understanding these interactions underscores why working within a structured, monitored program matters — not just for safety, but to ensure natural agents are used in ways that genuinely support your treatment goals.
NORI's Integrative Support Model
NORI offers a home-based nutritional support program built on founder Mark Simon's research into nutritional oncology, which began in 2004. The program combines:
- Cycled methionine restriction dietary guidance
- Proprietary nutraceuticals manufactured in-house
- Ongoing one-on-one support via phone and Zoom
- Personalized protocols tailored to individual cancer types
The program is accessible worldwide and requires no clinic visits.
NORI offers a free initial consultation for patients who want to explore how nutritional support can fit alongside their current treatment plan. Contact NORI at 800-634-3804 or info@nutritionaloncology.net to learn more.
Frequently Asked Questions
Is bone cancer treatable?
Primary bone cancer is sometimes curable, particularly early-stage osteosarcoma, which has 5-year survival rates of 60-75% for localized disease. Bone metastases are currently incurable but manageable with both conventional and integrative approaches that can extend survival and improve quality of life.
What are the first signs of metastatic bone cancer?
Persistent deep bone pain (often worse at night), bone fractures from minor injuries, and localized swelling or tenderness are hallmark symptoms. Advanced cases may cause hypercalcemia with fatigue and confusion. These symptoms warrant urgent medical evaluation.
What is the life expectancy of metastatic cancer in the bones?
Life expectancy varies significantly by primary cancer type and treatment response. Median survival after bone metastasis diagnosis is approximately 38 months for breast cancer, 30 months for prostate cancer, and 6-13 months for lung cancer. Ask your oncologist for a prognosis specific to your situation.
What foods should you avoid if you have bone cancer?
Processed meats, refined sugars, high-glycemic foods, excessive alcohol, and trans fats promote inflammation and may fuel cancer cell metabolism. A nutritional oncologist can tailor dietary recommendations to your specific cancer type and treatment stage.
Can natural treatments be used safely alongside chemotherapy?
Many can, but some natural compounds interact with chemotherapy drugs, making disclosure to your oncologist essential before starting any supplement. Curcumin and high-dose omega-3s require particular attention due to their effects on drug metabolism and bleeding risk.
What plant-derived compounds have shown the most promise for bone metastasis?
Curcumin, resveratrol, plumbagin, and honokiol are the most studied plant compounds with bone-specific mechanisms in preclinical research. Most evidence remains at the preclinical stage, with clinical trials still underway — discuss any of these with your care team before starting.


