Introduction
The days after an endometrial cancer diagnosis bring a flood of medical decisions—treatment options, surgery schedules, oncology appointments. But there's another question that surfaces quietly in the middle of everyday moments: What should I actually eat now?
For endometrial cancer, that question carries real weight. Roughly 80% of cases are classified as Type 1 — closely linked to estrogen dominance and metabolic factors that nutrition directly influences.
Your daily food choices can meaningfully affect circulating estrogen levels, insulin response, and inflammation — all of which play a role in cancer progression and recurrence risk.
This article provides evidence-based guidance on the foods that support recovery, the ones worth limiting, and how dietary strategy evolves from active treatment through long-term survivorship.
TL;DR
- Type 1 endometrial cancer is hormone-driven — diet that lowers excess estrogen and reduces inflammation directly supports recovery
- Prioritize colorful fruits and vegetables, legumes, whole grains, and healthy fats like olive oil and nuts
- Limit red and processed meats, full-fat dairy, sugary beverages, refined carbohydrates, and excess alcohol
- Coffee and green tea are linked to lower endometrial cancer risk across several prospective studies
- The Mediterranean diet matches the evidence closely and provides a practical, sustainable eating framework
Why Diet Matters: The Estrogen-Nutrition Connection
Type 1 endometrial cancer is driven by prolonged exposure to unopposed estrogen. Excess body fat is a major source of circulating estrogen because adipose tissue contains aromatase enzymes that convert androgens into estrogen. Research shows the risk of endometrial cancer increases by approximately 50% for every 5 kg/m² increase in body mass index, making dietary choices that support a healthy weight directly relevant to hormonal balance.
A Western-style diet high in animal fat, refined carbohydrates, and processed foods elevates insulin and promotes chronic low-grade inflammation. Both accelerate tumor-promoting signaling pathways in the endometrium, creating a metabolic environment that favors cancer growth. What you eat can shift that environment — and the mechanisms are well-documented.
The Fiber-Estrogen Link
Dietary fiber from whole plant foods directly lowers circulating estrogen levels. Fiber binds excess estrogen in the gut and promotes its excretion, preventing reabsorption into the bloodstream. This mechanism is a key reason why plant-rich diets are consistently associated with lower endometrial cancer risk.
Phytochemicals and Hormonal Modulation
Plant-based compounds offer additional hormonal benefits beyond weight management:
- Lignans in flaxseed and sesame inhibit aromatase activity, reducing estrogen-driven cell proliferation
- Isoflavones in soy interact with estrogen receptors to moderate hormonal signaling
- Indole-3-carbinol in cruciferous vegetables (broccoli, Brussels sprouts, kale) shifts estrogen metabolism toward less active pathways — a Phase I trial found a 400 mg daily dose increased the urinary 2-hydroxyestrone to 16alpha-hydroxyestrone ratio by 66%
- Carotenoids in orange and red vegetables provide antioxidant protection against DNA damage

These mechanisms extend beyond prevention. During and after treatment, an anti-inflammatory diet supports immune function, reduces side effect burden, aids tissue repair, and helps prevent the insulin resistance and weight gain that independently worsen endometrial cancer outcomes.
Foods to Eat for Endometrial Cancer
Fruits, Vegetables, and Legumes
Antioxidant-rich, colorful plant foods protect against DNA damage caused by free radicals. A meta-analysis of 10 case-control studies found the highest category of total vegetable intake was associated with a 29% reduced risk of endometrial cancer (RR = 0.71; 95% CI: 0.55-0.91). The protective effect was particularly strong among women who had never used hormone replacement therapy.
Key plant compounds to emphasize:
- Cruciferous vegetables (broccoli, Brussels sprouts, kale, cauliflower) contain indole-3-carbinol, which shifts estrogen metabolism toward less active pathways
- Legumes (lentils, chickpeas, beans) are rich in fiber and plant protein with a low glycemic impact, helping stabilize blood sugar and insulin levels
- Soy foods (tofu, edamame, tempeh) have been studied as natural aromatase inhibitors—a meta-analysis of 13 epidemiologic studies showed higher dietary isoflavone levels from soy and legumes were associated with a 19% reduced endometrial cancer risk (OR = 0.81; 95% CI: 0.74-0.89)
Whole Grains
Replacing refined carbohydrates with whole grains lowers glycemic load, improves insulin sensitivity, and provides insoluble fiber that supports gut health. The World Cancer Research Fund meta-analysis found a statistically significant 15% increased risk of endometrial cancer per 50 units per day of dietary glycemic load (RR = 1.15; 95% CI: 1.06-1.25).
Practical whole grain swaps include:
- Oats or quinoa in place of white-flour cereals
- Brown rice instead of white rice
- Whole wheat bread and pasta over refined versions
- Barley and farro as base grains for salads and soups
Healthy Fats and Lean Proteins
Not all fats are equal. Monounsaturated fats in olive oil and omega-3 fatty acids in walnuts, flaxseeds, and fatty fish like salmon are anti-inflammatory and support cell membrane integrity. A high ratio of monounsaturated to saturated fats is a defining feature of the Mediterranean diet, which has been linked to a 57% lower risk of endometrial cancer (OR = 0.43; 95% CI: 0.34-0.56).

In contrast, saturated fats found in red meat and full-fat dairy have been associated with elevated endometrial cancer risk.
Choose:
- Extra virgin olive oil for cooking and dressings
- Walnuts, almonds, and flaxseeds
- Fatty fish (salmon, mackerel, sardines) twice weekly
- Avocados
Protective Beverages
Coffee reduces endometrial cancer risk through two key mechanisms: it increases sex hormone-binding globulin (SHBG), lowering circulating free estrogen, and it improves insulin sensitivity. A pooled analysis of 19 epidemiologic studies found coffee drinkers had a 13% lower overall risk, with caffeinated coffee showing a 39% reduction compared to 27% for decaffeinated (OR = 0.87; 95% CI: 0.79-0.95). One to two cups daily is a practical, well-supported amount.
Green Tea: A systematic review and meta-analysis indicated that green tea consumption may be related to a reduction in endometrial cancer risk. The active compound EGCG (epigallocatechin-3-gallate) has demonstrated anti-estrogen and apoptosis-promoting effects in laboratory studies.
Foods to Limit or Avoid with Endometrial Cancer
Red and Processed Meats
Red and processed meats are high in saturated fat and heme iron, both associated with elevated endometrial cancer risk. A meta-analysis found a 51% increase in endometrial cancer risk per 100 g/day of red meat consumption (pooled OR = 1.51; 95% CI: 1.19-1.93).
Research from the Swedish Mammography Cohort showed that higher intakes of heme iron were associated with a 24% higher risk of endometrial cancer (RR = 1.24; 95% CI: 1.01-1.53) when comparing the highest with the lowest quartile.
These risks extend beyond fat and iron. Rapidly dividing cancer cells depend heavily on the amino acid methionine, and red meat and processed animal products are among its densest dietary sources — making methionine restriction a scientifically grounded strategy in nutritional oncology research. Reducing protein intake, especially animal protein, without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research.
Practical reductions to consider:
- Replace red meat with legumes, tofu, or fish at least 3–4 days per week
- Avoid processed meats (bacon, sausage, deli cuts) entirely during active treatment
- Choose plant-based protein sources when meeting methionine-restriction goals
Sugary Foods, Refined Carbohydrates, and Sweetened Beverages
Data from the Iowa Women's Health Study showed that women consuming the most sugar-sweetened beverages had a 78% higher risk of Type I endometrial cancer (95% CI: 1.32-2.40) compared to the lowest consumers, even after adjusting for BMI.
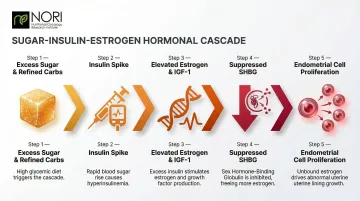
Excess sugar spikes insulin, which elevates estrogen and promotes cell proliferation in the endometrium. High insulin levels also increase bioavailable insulin-like growth factor-1 (IGF-1) and suppress sex hormone-binding globulin (SHBG) — both changes that amplify estrogen exposure.
Limit or avoid:
- Soda and fruit juice
- Candy, cookies, pastries
- White bread, white rice, and refined pasta
- Sweetened cereals and snack bars
High-Fat and Full-Fat Dairy Products
Full-fat dairy contributes to higher saturated fat intake and may independently raise endometrial cancer risk. The Nurses' Health Study found that postmenopausal women consuming three or more servings of total dairy per day had a 58% elevated risk (RR = 1.58; 95% CI: 1.05-2.36) compared to low consumers, particularly among those not using hormone therapy.
Low-fat dairy or fortified plant-based alternatives — oat, soy, or almond milk — meet calcium and vitamin D needs without the associated risk increase.
Alcohol
Like sugar, alcohol affects endometrial cancer risk partly through its impact on estrogen metabolism. A meta-analysis of seven prospective cohort studies found a J-shaped relationship: women drinking up to 0.5 drinks per day showed a modest 4% lower risk, but risk climbed above two drinks per day — reaching 25% higher risk at more than 2.5 drinks per day.
During active treatment, eliminating alcohol removes one modifiable source of estrogen amplification. For long-term survivors, even modest intake warrants discussion with an oncology-informed clinician.
The Mediterranean Diet as a Practical Framework
Of all dietary frameworks studied in relation to endometrial cancer, the Mediterranean diet has the strongest research backing. This pattern emphasizes:
- High intake of vegetables, fruits, legumes, whole grains, fish, and olive oil
- Moderate wine consumption
- Low intake of red meat and full-fat dairy
That combination carries measurable impact: high adherence to a Mediterranean dietary pattern is associated with a 57% lower risk of endometrial cancer (OR = 0.43; 95% CI: 0.34–0.56) compared to a Western-style diet. For patients managing or working to prevent endometrial cancer, this is one of the most actionable dietary shifts supported by current evidence.
Practical Starting Points
You don't need to overhaul your entire diet overnight. Start with these manageable shifts:
- Swap butter for olive oil in cooking and on bread
- Add a legume-based side dish three nights per week (lentil soup, chickpea salad, black bean tacos)
- Choose fish over red meat twice a week
- Build half your plate with vegetables at each meal — leafy greens, tomatoes, and cruciferous options like broccoli fit naturally into this pattern

Dietary Strategies During Treatment vs. Long-Term Survivorship
Nutritional priorities shift during active treatment. When undergoing chemotherapy, radiation, or surgery, the focus moves away from restriction and toward support:
- Maintaining body weight and caloric intake
- Managing side effects such as nausea, fatigue, and taste changes
- Preserving lean muscle mass through adequate protein
The general anti-inflammatory principles still apply, but deliberate caloric restriction is not appropriate during this phase.
Survivorship nutrition refocuses on long-term recurrence prevention: sustained weight management to minimize estrogen exposure, consistent fiber intake, limiting inflammatory foods, and building lasting dietary habits rather than short-term interventions. Regular physical activity amplifies the benefits of dietary changes by further lowering circulating estrogen levels.
Because every patient's treatment regimen, metabolic profile, and food tolerances differ, individualized guidance matters more than any one-size-fits-all plan. NORI's nutritional oncology support program draws on over 20 years of research into diet, natural agents, and cancer cell vulnerabilities to provide personalized, home-based support for patients at every stage.
Frequently Asked Questions
What is the best diet for uterine cancer patients?
The evidence most consistently supports a predominantly plant-based diet—rich in vegetables, legumes, whole grains, and healthy fats—similar to the Mediterranean diet, while limiting red meat, saturated fat, refined sugars, and alcohol.
Can diet reduce the risk of endometrial cancer recurrence?
Maintaining a healthy weight, reducing estrogen-promoting foods, and eating an anti-inflammatory plant-rich diet are all associated with lower recurrence risk. Diet works best as part of a broader survivorship plan that includes regular physical activity and ongoing medical monitoring.
Is soy safe for endometrial cancer patients?
Moderate consumption of whole soy foods (tofu, edamame, tempeh) appears safe and may even be protective due to soy's ability to act as a natural aromatase inhibitor. Highly concentrated soy supplements carry more risk and should be discussed with a healthcare provider.
Which beverages are recommended or restricted for endometrial cancer patients?
Water should be your primary beverage. Green tea and coffee are supported by research for their potential protective effects. Avoid sugary beverages and limit alcohol, especially during active treatment.
How does weight management connect to diet and endometrial cancer?
Excess body fat contains aromatase enzymes that produce estrogen, so maintaining a healthy weight through diet and exercise is one of the most impactful modifiable factors for both risk and recurrence.
Which nutrients or supplements should endometrial cancer patients consider?
Dietary fiber, omega-3 fatty acids, vitamins C, D, and E, and lignans from flaxseed have supportive evidence from dietary studies. Supplements should only be taken under guidance from a healthcare provider or oncology nutritionist, as some may interfere with treatment.