
Introduction
A blood cancer diagnosis raises immediate, practical questions — one of the most urgent being: "What should I eat?" Blood cancers like leukemia, lymphoma, and myeloma compromise your body's defenses at a cellular level, making nutrition both more challenging and more critical than ever.
Treatments like chemotherapy, targeted therapy, and steroids add another layer of difficulty. They can deplete key nutrients, disrupt digestion, and stress the body's ability to absorb what it needs.
While no food can cure blood cancer, the right nutritional choices can directly support immune function, help manage side effects like nausea and fatigue, maintain strength, and improve quality of life. This guide covers what to eat, what to avoid, and how to adapt your diet when eating becomes difficult — with practical, evidence-based strategies at every stage of treatment.
TLDR
- Protein intake of at least 1.0–1.5 g/kg/day supports immune function, muscle maintenance, and blood cell production during blood cancer treatment
- Prioritize thoroughly cooked lean proteins, washed produce, whole grains, and healthy fats while avoiding raw foods, unpasteurized dairy, and alcohol
- Food safety is critical — chemotherapy-induced neutropenia makes foodborne infections potentially life-threatening
- Small frequent meals, soft textures, and cold foods help manage common side effects like nausea, appetite loss, and taste changes
- Your cancer type, treatment protocol, and disease stage all shape which dietary strategies will work best — personalized nutrition guidance accounts for these differences
Why Nutrition Matters During Blood Cancer Treatment
Blood cancer treatments directly alter metabolism, appetite, and nutrient absorption. Chemotherapy regimens like R-CHOP and HyperCVAD frequently cause treatment-related complications that directly affect your ability to eat and absorb nutrients, including:
- Grade 3-4 oral mucositis and mouth sores
- Severe diarrhea and gastrointestinal toxicity
- Profound neutropenia (dangerously low white blood cell counts)
- Steroid-driven muscle wasting and blood sugar spikes (from dexamethasone, prednisone)
- Bone density loss through accelerated protein catabolism
Each of these creates a different nutritional challenge — and often several occur at once.
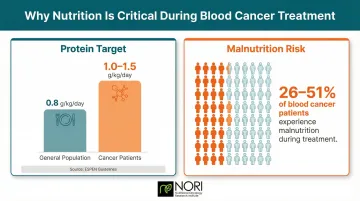
Protein is the most critical macronutrient for blood cancer patients. The European Society for Clinical Nutrition and Metabolism (ESPEN) recommends protein intake of 1.0-1.5 g/kg/day for cancer patients, roughly double the general population guideline of ~0.8 g/kg/day. This elevated protein need exists because your body constantly repairs tissue, produces new blood cells, and maintains immune defenses — all of which are disrupted by blood cancers and their treatments. Research shows that optimizing nitrogen balance with higher protein provision is associated with lower mortality and better functional outcomes in critically ill patients, including those with hematologic malignancies.
Protein needs don't exist in isolation. A body undergoing chemotherapy burns more calories at rest than normal, making overall caloric intake equally important to prevent muscle wasting and dangerous weight loss. Between 25.8% and 50.74% of patients with hematologic malignancies experience malnutrition during treatment — meaning roughly half of blood cancer patients are already nutritionally compromised when they need their bodies most.
Beyond managing treatment side effects, certain dietary strategies may target specific vulnerabilities in cancer cell biology. Methionine restriction is one research-backed approach: by reducing methionine-rich foods, patients may limit a nutrient cancer cells preferentially use to grow, while healthy cells adapt more readily. Preclinical studies in leukemia show that methionine restriction reduced plasma methionine by 59% and slowed leukemic growth by 35% in murine models.
NORI's protocol applies this targeted approach, pairing methionine-restricted plant-based diets with specific nutraceuticals. The goal is to exploit cancer cell vulnerabilities while preserving normal cell function.
Individual needs vary considerably based on blood cancer type, treatment phase (active treatment vs. remission vs. watch-and-wait), and personal health factors. The sections below break down what to eat — and what to avoid — at each stage.
Best Foods to Eat When You Have Blood Cancer
Prioritize nutrient-dense, easy-to-digest, food-safe options across all meals. The goal is combining immune support, adequate protein, steady energy, and micronutrient coverage in every meal and snack.
High-Protein Foods
Protein is the most critical macronutrient because your body constantly needs to repair tissue, produce new blood cells, and maintain immune defenses during treatment.
Recommended protein sources:
- Lean poultry (chicken, turkey — thoroughly cooked)
- Fish (cooked to safe temperatures)
- Eggs (fully cooked, not runny)
- Low-fat dairy (pasteurized only)
- Beans and lentils (well-cooked)
- Tofu and tempeh
Aim for a serving of protein at every meal and snack to meet the 1.0-1.5 g/kg/day target recommended by ESPEN.
Colorful Fruits and Vegetables
Phytochemicals — naturally occurring compounds in colorful plant foods — support immune function, reduce inflammation, and may slow abnormal cell growth.
Prioritize diverse options:
- Dark leafy greens (spinach, kale, Swiss chard)
- Cruciferous vegetables (broccoli, cauliflower, Brussels sprouts)
- Orange and red produce (carrots, bell peppers, berries)
During neutropenia or active treatment, all produce must be thoroughly washed. Cooking vegetables reduces infection risk while maintaining most nutrient value.
Whole Grains
Whole grains (oats, brown rice, quinoa, whole wheat) are preferable to refined carbohydrates. They provide fiber for gut health, release energy more slowly to stabilize blood sugar, and contain more vitamins and phytochemicals per serving than processed alternatives — making them especially important for patients on steroids.
A systematic review of 80 randomized trials found that whole grain intake significantly reduces postprandial glycemia and insulinemia compared to refined grains, which directly supports managing steroid-induced blood sugar spikes.
Healthy Fats
Unsaturated fats provide caloric density and anti-inflammatory properties — especially useful for patients experiencing unintended weight loss during treatment.
Good sources include:
- Avocado
- Olive oil
- Nuts and seeds
- Oily fish (salmon, mackerel, sardines)
Healthy fats are the most calorie-efficient way to boost intake when appetite is low, delivering 9 calories per gram compared to 4 from protein or carbohydrates.

Staying Hydrated
Adequate hydration supports kidney function, aids digestion, reduces fatigue, and helps flush treatment-related toxins. Aim for 6-8 cups of fluid daily through water, herbal teas, broths, and high-moisture foods. Limit caffeine and alcohol. If diarrhea or vomiting is present, sports drinks or electrolyte solutions may be needed to replace lost minerals.
Foods to Avoid During Blood Cancer Treatment
Avoiding certain foods reduces infection risk, manages side effects, and supports treatment effectiveness. Blood cancer patients are often immunosuppressed, which shifts the risk calculus of everyday food choices.
Raw and Undercooked Foods
Raw or rare meat, raw fish (sushi), undercooked eggs, and raw sprouts carry heightened infection risk for patients with low white blood cell counts (neutropenia). A 2026 Phase III trial in hematopoietic stem-cell transplantation and acute leukemia patients found that a liberalized diet resulted in a significantly higher major infection rate (31.4%) compared to a strict neutropenic diet (20.2%), demonstrating that fresh raw produce poses genuine danger during profound immunosuppression.
Practical guidance:
- Cook meats to safe internal temperatures (165°F for poultry)
- Avoid salad bars and buffets
- Skip sushi, ceviche, and raw oysters
- Cook eggs until yolks are firm
Unpasteurized Products and High-Risk Dairy
Avoid unpasteurized juices, raw milk, and soft cheeses made from unpasteurized milk (brie, camembert, feta, queso fresco). For healthy individuals, the bacteria risk from these foods is manageable — but it can become life-threatening when immunity is compromised. Immunocompromised patients are up to 50 times more likely to contract a Listeria infection than healthy adults.
Ultra-Processed Foods, Excessive Sugar, and Alcohol
The common misconception that "sugar feeds cancer" is overly simplistic: all cells, including healthy cells, use glucose for energy, and eliminating sugar does not "starve" cancer. However, diets heavy in added sugar, processed snacks, and refined carbohydrates displace the nutrient-dense foods your body needs during treatment and contribute to blood sugar instability, especially problematic for steroid users.
Practical guidance:
- Replace sugary snacks with whole-food options like fruit, nuts, or legumes
- Avoid ultra-processed packaged foods (chips, cookies, fast food) that crowd out nutrients
- Limit or eliminate alcohol — the FDA warns that methotrexate can cause severe hepatotoxicity, with risk significantly increased by alcohol use
- Note that alcohol also interacts with other cancer drugs and accelerates dehydration
Food Safety: Protecting Yourself with a Weakened Immune System
Chemotherapy and other blood cancer treatments can cause neutropenia — a dangerous drop in neutrophil counts that leaves you vulnerable to foodborne infections a healthy immune system would normally clear without issue. In diffuse large B-cell lymphoma patients treated with R-CHOP, 60.2% experienced at least one episode of grade 4 neutropenia, and 42.2% of those episodes progressed to febrile neutropenia.
That level of immune suppression means food handling practices carry real clinical stakes — not just general wellness advice.
Key food safety practices:
- Wash hands and surfaces thoroughly and often
- Use separate cutting boards for raw proteins and produce
- Cook all meat to safe internal temperatures using a food thermometer
- Refrigerate perishables promptly (within 2 hours)
- Check expiration dates on all packaged foods
- Thaw frozen items in the refrigerator or microwave, not on the counter

These practices apply broadly, but stem cell transplant patients typically face tighter restrictions. CDC guidelines recommend a low microbial diet for 3 months post-autologous transplant, and for allogeneic recipients until all immunosuppressive drugs are discontinued.
Before your next treatment cycle, ask your oncology team specifically which foods to avoid and whether a low microbial diet applies to your protocol — the answer varies more than most patients expect.
Managing Common Eating Challenges During Treatment
Even patients who understand good nutrition often struggle to eat well during treatment due to side effects. Nausea, mouth sores, taste changes, swallowing difficulties, fatigue, and appetite loss are all common. These challenges are temporary and manageable with the right strategies.
Practical strategies by side effect:
For nausea:
- Eat small frequent meals every 2-3 hours
- Drink ginger tea
- Avoid strong smells
- Eat cool or room-temperature foods
For appetite loss:
- Keep calorie-dense snacks visible and accessible
- Use healthy fats (nut butters, avocado, olive oil) to boost calories without volume
- Try high-protein oral nutrition supplements (Ensure, Boost) when solid food is difficult
For taste changes:
- Experiment with herbs and seasonings
- Use plastic utensils if metal tastes metallic
- Try cold foods, which have milder odors
- Add tart flavors (citrus) if mouth sores are absent
- Marinate proteins before cooking to improve palatability
For mouth sores:
- Choose soft, moist foods (yogurt, smoothies, mashed foods)
- Avoid acidic or spicy items
- Use a straw for liquids
- Rinse mouth frequently with salt water
When Eating Challenges Require Extra Support
A 2025 systematic review found that high-protein oral nutritional supplements significantly reduced complications and decreased hospital stay length in cancer patients — making professional nutritional guidance especially valuable when side effects limit intake.
For patients who need ongoing support, NORI offers a home-based nutritional support program with individualized dietary guidance built around their research-based protocol, available worldwide without requiring clinic visits.
Frequently Asked Questions
What is the best diet for blood cancer patients?
A balanced, high-protein, plant-rich diet is the evidence-based foundation: lean proteins, colorful produce, whole grains, and healthy fats. ESPEN recommends 1.0–1.5 g/kg/day protein and 25–30 kcal/kg/day energy. Individual needs vary by treatment type, so work with an oncology dietitian familiar with your specific cancer and protocol.
What foods should blood cancer patients avoid?
Avoid raw or undercooked meat/fish/eggs, unpasteurized dairy, unwashed produce, alcohol, and ultra-processed foods. Recent evidence shows that fresh raw produce significantly increases major infection rates in immunosuppressed patients. Avoidance is primarily about managing infection risk and supporting treatment.
What foods should leukemia patients eat?
Leukemia treatments often involve chemotherapy and steroids that affect appetite and blood sugar. Prioritize whole grains for blood sugar stability, protein at every meal to support white blood cell recovery, and thoroughly cooked produce to minimize infection risk during neutropenic periods. Aim for the 1.0-1.5 g/kg/day protein target recommended by ESPEN.
Does sugar feed blood cancer?
No. All cells use glucose for energy, so eliminating sugar does not "starve" cancer — the body will produce glucose from other sources if carbohydrates are restricted. That said, excessive added sugar contributes to weight gain and blood sugar instability, so whole-food carbohydrates are the better choice.
Is it safe to take supplements during blood cancer treatment?
Many supplements interfere with blood cancer drugs — St. John's Wort reduces imatinib levels by 30% and ibrutinib by over 90%, and antioxidant supplements during chemotherapy are linked to a 41% higher recurrence risk. No supplement should be started without consulting your oncologist and pharmacist first. Professional guidance ensures any supplement use supports rather than undermines your treatment.
How can I eat well when treatment kills my appetite?
Eat small, frequent meals every 2-3 hours rather than three large meals. Keep calorie-dense snacks visible and accessible. Use healthy fats and protein powders or oral nutrition supplements (Ensure, Boost) when solid food is difficult. Report persistent appetite loss to your care team, as medical interventions may be available to stimulate appetite.


