
Introduction
Neuroendocrine cancer (NET) disrupts one of the most fundamental parts of daily life: eating. Unlike most cancers where dietary advice follows predictable patterns, NETs produce hormones that directly interfere with digestion, nutrient absorption, and how the body processes food.
Tumors secreting serotonin, gastrin, insulin, or other hormones create symptoms that make nutrition both critically important and genuinely complex to manage.
According to the first global NET patient survey, 58% of NET patients report having to make dietary changes as a result of their disease. This guide covers what to eat, what to avoid, symptom-specific strategies, and when to seek specialized nutritional support to help you navigate this challenging landscape.
TLDR:
- NET nutrition must be individualized based on tumor location and hormone profile
- High-amine foods (aged cheese, alcohol, fermented items) trigger flushing and diarrhea in many patients
- Small, frequent meals reduce symptom burden better than three large meals
- Niacin deficiency affects 28% of carcinoid syndrome patients due to serotonin production
- Food-symptom diaries help identify personal triggers and avoid unnecessary restrictions
Why Diet Is Especially Complicated with Neuroendocrine Cancer
NETs Are Not One Disease
NETs can arise in the GI tract, pancreas, lungs, and elsewhere. Each location determines which symptoms affect eating. A midgut NET producing serotonin creates vastly different dietary challenges than a pancreatic NET secreting insulin. The 2025 ENETS consensus explicitly rejects universal dietary protocols, stating that "dietary advice must be tailored to disease type, stage, and treatment."
Hormones Create Unique Nutritional Challenges
Hormone-secreting NETs disrupt digestion in ways most other cancers don't:
- Serotonin overproduction increases intestinal movement, reducing water and electrolyte absorption and causing chronic diarrhea
- Gastrin excess triggers severe acid reflux and watery or oily stools
- Insulin hypersecretion causes recurrent low blood sugar requiring frequent carbohydrate intake
- VIP (vasoactive intestinal peptide) causes persistent watery diarrhea with severe electrolyte depletion
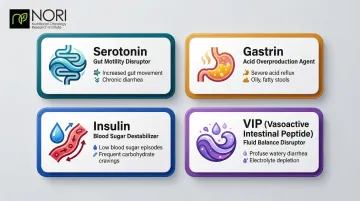
Understanding which hormones are overactive is the starting point for any meaningful dietary plan — because what helps one NET patient can worsen symptoms in another.
No "NET Diet" Cures Disease
There is no single NET diet proven to cure or control the disease. What the evidence does support is that targeted dietary adjustments can reduce symptom severity, protect nutritional status, and support immune function during treatment.
A retrospective review of 69 NET patients with diarrhea found that 80% experienced symptom improvement with dietary modification. A further 51% reported more than 50% reduction in diarrhea frequency.
Managing Common Symptoms Through Food
Diarrhea: The Most Damaging NET Symptom
Chronic diarrhea causes rapid loss of fluid, electrolytes, and protein. Clinical guidance supports:
- Eat small, frequent meals at room temperature rather than large portions
- Limit fiber to 18-24g daily during active diarrhea flares
- Follow a low-amine, low-fat approach to reduce bowel frequency
- Choose dry foods (crackers, toast, plain rice) that don't stimulate intestinal movement
Weight Loss Despite Adequate Intake
NETs can cause weight loss even when calories seem sufficient due to malabsorption. Strategies include:
- Switch to lactose-free dairy products to avoid additional GI distress
- Soft-cooked proteins — poached chicken, scrambled eggs, steamed fish — are easier to digest than grilled or fried options
- Add healthy fats in small amounts: olive oil drizzled on cooked vegetables or a few tablespoons of mashed avocado
- Prioritizing calorie-dense but easily digestible options
Fat Malabsorption (Steatorrhea)
Steatorrhea — pale, floating, foul-smelling stools — results from pancreatic enzyme insufficiency caused by surgery or tumor effects. SSA (somatostatin analog) treatment causes steatorrhea in 26-65% of lanreotide users and 36-61% of octreotide users.
Management:
- Pancreatic enzyme replacement therapy (PERT) may be prescribed—start at 44,000-50,000 units of lipase with meals and 22,000-25,000 units with snacks
- Until enzyme therapy is optimized, favor easily digestible unsaturated fats (olive oil, small amounts of avocado) over saturated and fried fats
Nausea Control
Dietary adjustments that reduce nausea:
- Eating small, bland meals throughout the day
- Avoiding greasy, fatty, or heavily seasoned foods
- Prioritizing easily tolerated options: plain toast, white rice, scrambled eggs, applesauce, bananas
Keep a Food-Symptom Diary
NET symptoms can mimic each other — diarrhea, bloating, and nausea often share triggers. Before cutting out entire food groups, track what you eat, portion sizes, and any symptoms within 2-4 hours. Patterns you spot may point to specific culprits, helping you manage symptoms without creating avoidable nutritional gaps.
Foods to Avoid with Neuroendocrine Cancer
Carcinoid Syndrome Trigger Foods
For patients with hormone-secreting NETs, certain foods trigger or worsen flushing and diarrhea by stimulating serotonin or other hormone release. Triggers are highly individual—not everyone reacts to the same foods.
High-Amine Foods: Key Category to Limit
Amines are naturally occurring compounds in foods that can provoke flushing and GI symptoms in NET patients. They trigger vasoactive responses because they are precursors to catecholamines like adrenaline, which can stimulate tumors to secrete hormones.
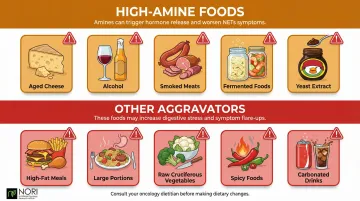
High-Amine Foods to Avoid:
- Aged cheeses (extra sharp cheddar, parmesan, blue cheese)
- Alcohol (all types)
- Smoked, salted, or pickled fish and meats (bacon, salami, smoked salmon)
- Fermented foods (sauerkraut, miso, soy sauce, kimchi, shrimp paste)
- Yeast extracts and nutritional yeast
Moderate-Amine Foods (Limit or Test Individually):
- Caffeine
- Dark chocolate
- Avocado
- Banana
- Raspberries
- Peanuts
- Tempeh
Other Food Characteristics to Minimize
Beyond amines, several other food characteristics commonly aggravate NET symptoms:
- Avoid high-fat meals (especially saturated and fried fats), which slow digestion and worsen malabsorption
- Limit large portions — they can trigger hormonal surges that provoke flushing and pain
- Reduce high-insoluble-fiber foods (wheat bran, raw cruciferous vegetables, dried fruit), which speed GI transit and worsen diarrhea
- Cut very spicy foods, which stimulate gut motility
- Skip carbonated drinks, which cause bloating and gas

Restriction Should Be Targeted, Not Sweeping
These categories flag common problem foods — but that doesn't mean eliminating entire food groups. Blanket restriction risks creating nutritional deficiencies that compound the challenges of treatment. Use a food diary to confirm which specific items are actual triggers for you before cutting them out.
Building a NET-Friendly Plate: What to Eat
Foundation: Lean, Fresh Proteins
Protein is especially important in NET patients with carcinoid syndrome. Serotonin production diverts tryptophan away from niacin synthesis, increasing protein and niacin needs.
Good options include:
- Skinless poultry (chicken breast, turkey)
- Fresh fish (cod, tilapia, halibut)
- Eggs (scrambled, poached, or soft-boiled)
- Low-fat or lactose-free dairy (Greek yogurt, cottage cheese)
- Well-cooked lentils and beans (if tolerated)
Safe Vegetables and Fruits
Cooked or peeled options are better tolerated than raw produce:
- Vegetables: carrots, squash, zucchini, asparagus, green beans, potatoes, sweet potatoes
- Fruits: apple, pear, peach, mango, melon, berries (except raspberries)
Gentle Grains and Starches
White rice, oatmeal, quinoa, and white bread are preferred over high-fiber whole grains during active symptoms. Lower insoluble fiber content reduces GI transit speed and diarrhea burden.
- White rice
- Oatmeal
- Quinoa
- White bread or sourdough
- Plain pasta
Nutritional Oncology as a Complement to Standard Care
Food selection isn't only about managing symptoms — diet can also influence cancer cell metabolism. One emerging area is methionine restriction, which limits high-methionine foods (primarily concentrated in animal proteins) to disrupt the metabolic environment that cancer cells depend on.
NORI's protocol builds on this principle, pairing a plant-based dietary framework with targeted nutraceuticals as part of a personalized integrative support program. For patients interested in exploring this approach alongside their standard care, NORI offers a free initial consultation.
How and When to Eat to Reduce Symptoms
Meal Frequency and Portion Control
Eating 4-6 small meals per day instead of 3 large meals reduces the hormonal burden per meal and lowers the risk of triggering flushing, diarrhea, or pain—large meals are one of the most commonly reported carcinoid syndrome triggers.
Sample daily eating pattern:
- 7:00 AM: Small breakfast (oatmeal with peeled apple)
- 10:00 AM: Mid-morning snack (lactose-free yogurt)
- 1:00 PM: Small lunch (white rice with steamed chicken and carrots)
- 4:00 PM: Afternoon snack (peeled pear, plain crackers)
- 7:00 PM: Small dinner (baked fish with mashed potato and green beans)
- 9:00 PM (optional): Light snack if needed

Hydration Strategy
NET patients—particularly those managing active diarrhea—need to stay well-hydrated throughout the day.
Recommended approach:
- Sip 6-8 glasses of water or diluted fluids throughout the day
- Don't drink large amounts with meals (this can worsen bloating and diarrhea)
- Limit caffeinated, alcoholic, and high-sugar beverages
- During acute diarrhea, sip small amounts frequently rather than gulping
Beyond what you drink and when, how you handle food itself can significantly affect symptoms.
Food Safety and Storage
Compromised digestion and reduced immune function make NET patients more vulnerable to foodborne illness—so food handling matters more than most people realize.
Key practices:
- Refrigerate leftovers promptly (within 2 hours)
- Avoid aged or fermented foods that spike amine levels
- Discard leftovers after 48 hours
- Wash produce thoroughly before peeling or cooking
Nutritional Gaps to Watch: Niacin, Vitamins, and Minerals
NET-Specific Risk: Niacin Deficiency
When NETs overproduce serotonin, the body diverts tryptophan (an amino acid) to make serotonin instead of niacin (vitamin B3). Biochemical niacin deficiency affects approximately 28% of carcinoid syndrome patients, leading to symptoms including dermatitis, diarrhea, and neurological effects.
Prevention:
- Adequate protein intake from lean sources
- Low-dose niacin supplement (such as niacinamide) may be appropriate—always under medical guidance
- Monitor for symptoms of deficiency
Other Potential Deficiencies
Two common consequences of NETs and their treatments create additional nutritional vulnerabilities:
- Fat malabsorption impairs uptake of fat-soluble vitamins A, D, E, and K. In long-term SSA users, 78% are deficient in one or more vitamins, with vitamin K1 deficiency in 63% and vitamin D deficiency in 28%
- Chronic diarrhea depletes electrolytes—sodium, potassium, and magnesium—and can lead to dehydration and hypoproteinemia
Work with Your Healthcare Team
These deficiencies should be tested and addressed individually with a registered dietitian and oncology team through bloodwork. The 2025 ENETS guidance recommends evaluating and supplementing vitamin B12 and vitamin D at baseline and throughout follow-up visits, with niacin evaluation and supplementation considered in carcinoid syndrome patients.
Do not supplement blindly—nutritional needs change across the disease course.
Frequently Asked Questions
Frequently Asked Questions
What not to eat with neuroendocrine cancer?
Limit or avoid high-amine foods (aged cheeses, alcohol, fermented foods, smoked meats), large fatty meals, raw spicy foods, and high-insoluble-fiber foods. Individual triggers vary significantly, so keep a food diary to identify personal sensitivities rather than restricting broadly.
Do neuroendocrine tumors cause fatigue?
Yes. Fatigue is reported by 36-61% of NET patients and stems from hormonal disruption, poor nutrient absorption, diarrhea-related dehydration, and the metabolic burden of cancer itself. Improving nutrition and hydration can help reduce fatigue.
Can diet help control carcinoid syndrome symptoms?
Dietary changes can noticeably reduce the frequency and severity of carcinoid syndrome symptoms—primarily by avoiding amine-rich trigger foods and eating smaller, more frequent meals rather than large portions.
Do NET patients need vitamin or mineral supplements?
Some NET patients—especially those with fat malabsorption or serotonin-secreting tumors—are at risk for deficiencies in niacin, fat-soluble vitamins, and electrolytes. Supplementation should be guided by blood tests and your healthcare team, not self-prescribed.
Should I follow a low-fiber diet with neuroendocrine cancer?
A low-insoluble-fiber diet is often recommended during active diarrhea or GI symptoms, as high-fiber foods can worsen bowel frequency. However, this is not a permanent requirement for all NET patients—it depends on your individual symptom status.
How do I maintain a healthy weight with neuroendocrine cancer?
Prioritize protein-rich foods and calorie-dense but gentle options (lactose-free dairy, soft-cooked proteins, healthy fats in moderation). Eat small frequent meals and work with a dietitian to monitor nutritional status throughout treatment.


