
Understanding the Challenge
Cancer patients face a difficult reality during treatment: solid food often becomes painful or impossible to consume. Treatment side effects create real barriers to eating:
- Nausea and vomiting that make meals unbearable
- Mouth sores (mucositis) that make chewing and swallowing painful
- Taste changes that make familiar foods unpalatable
- Severe fatigue that eliminates the energy needed to prepare or eat meals
These barriers lead to unintended weight loss and nutritional deficiencies—problems that directly worsen treatment outcomes and recovery prospects.
Liquid supplements offer a practical bridge between what patients can physically tolerate and what their bodies urgently need. They're clinical tools designed to deliver concentrated nutrition when solid meals aren't an option. But not all liquid supplements are created equal—and choosing the right formulation can make a measurable difference in a patient's strength, weight stability, and ability to continue treatment.
TLDR: Key Takeaways
- Cancer treatment causes appetite loss, nausea, and swallowing difficulties in most patients, making liquid nutrition essential
- Liquid options include commercial high-calorie shakes, homemade smoothies, and specialized medical formulas
- Prioritize calorie density (300–500+ calories per serving) and high-quality protein (15–25g per serving)
- Skip products labeled "diet" or "low-fat," and watch for high added sugar content
- Consult your oncology team before starting any supplement, as certain nutrients can interfere with active treatment
Why Cancer Patients Struggle to Eat—and Why Liquid Supplements Help
Cancer increases the body's metabolic demands while simultaneously triggering symptoms that make eating difficult or nearly impossible. Malnutrition affects 30% to 85% of cancer patients, with cachexia—a severe wasting syndrome—affecting approximately 33% of patients.
Cancer cachexia differs fundamentally from ordinary weight loss. This condition involves progressive muscle wasting driven by systemic inflammation and metabolic disruption specific to cancer biology. Unlike simple caloric restriction, cachexia cannot be fully reversed through conventional nutritional support alone. It carries serious consequences: lower survival rates, decreased performance status, and reduced ability to tolerate treatment.
Treatment toxicities compound these challenges. Radiotherapy to the head, neck, or esophagus causes mucositis and significant weight loss in up to 80% of patients. Chemotherapy frequently triggers severe nausea, vomiting, and taste alterations that make the thought of food unbearable.
Why liquid formats work better:
- Less aromatic, reducing nausea triggers
- Gentler on damaged GI tract tissue
- Easier to swallow with mucositis or surgical restrictions
- Require minimal physical effort to consume
- Can be sipped slowly throughout the day

Liquid supplements are not intended to replace whole foods when eating is possible—they're targeted interventions for patients who cannot meet nutritional needs through solid food alone. During active treatment, the primary goals are weight maintenance and preservation of lean muscle mass, and liquid formats make hitting those targets feasible even on the worst treatment days.
Types of Liquid Supplements for Cancer Patients
Commercial Meal-Replacement and Nutritional Shakes
Commercial ready-to-drink formulas offer unmatched convenience: no preparation required, portable packaging, and shelf-stable storage. These products typically deliver 350–600 calories per serving, making them practical for maintaining calorie intake and preventing dangerous weight loss.
However, quality varies widely across brands. Higher-quality oncology formulas derive nutrients from whole-food sources—pea protein, MCT oil from coconut, and real fruit extracts—rather than synthetic fillers and artificial ingredients. ESPEN guidelines recommend protein intake of 1.0–1.5 g/kg body weight daily00079-0/fulltext) during active cancer care, so checking the protein content per serving is essential.
Standard nutritional shakes work for general malnutrition, but specialized oncology formulas address specific cancer-related needs. Some are enriched with EPA omega-3 fatty acids to combat inflammation and cachexia. Others use semi-elemental proteins (already broken down into peptides) for patients with compromised digestion or malabsorption.
For patients with dairy sensitivities or lactose intolerance, plant-based protein options offer comparable amino acid profiles. Pea protein provides highly digestible, hypoallergenic nutrition that supports muscle synthesis comparably to whey when adequately dosed.
Critical warning: Avoid "diet," "low-fat," or "low-sugar" versions of commercial shakes. These products are counterproductive for cancer patients who need caloric density to prevent dangerous weight loss.
Homemade Smoothies and Blended Drinks
Homemade smoothies allow complete customization of ingredients, calorie density, and flavor profiles. You can incorporate anti-inflammatory whole foods while avoiding artificial additives and excessive sugars common in commercial products.
High-calorie, nutrient-dense add-ins:
- Avocado (240 calories, healthy fats)
- Nut butters (190–200 calories per 2 tablespoons)
- Full-fat coconut milk (445 calories per cup)
- MCT oil (115 calories per tablespoon)
- Hemp hearts (170 calories per 3 tablespoons)
- Ground flaxseed (37 calories per tablespoon, omega-3s)
- Chia seeds (138 calories per ounce)
Practical blending tips:
- Add liquids before solids to prevent blender jamming
- Blend in small batches for smoother consistency
- Store leftovers in the refrigerator up to 24 hours maximum
- Adjust texture (thinner or thicker) based on swallowing comfort
Smoothies accommodate mouth sores, swallowing issues, and digestive sensitivities better than most commercial products because you control every ingredient.
Specialized Nutraceutical Formulas
Unlike calorie-focused shakes, specialized nutraceutical formulas target the biochemistry of cancer itself. These liquids are built around specific bioactive compounds, including:
- Curcumin (anti-inflammatory, pro-apoptotic activity)
- Omega-3 fatty acids (combat cachexia and systemic inflammation)
- Selenium (antioxidant support, immune function)
- Medicinal mushroom extracts (immune modulation)
Research on omega-3 supplementation shows significant improvements in body weight and quality of life for patients with cancer cachexia, particularly in advanced non-small cell lung cancer. Because dosing and timing affect outcomes meaningfully in this category, medical supervision is essential before starting any nutraceutical protocol.
Key Nutrients to Prioritize in Liquid Supplements
Protein
Protein is non-negotiable for cancer patients. It repairs tissue damage from treatment, supports immune function, and prevents muscle wasting. Cancer patients have higher protein requirements than the general population—ESPEN clinical guidelines strongly recommend 1.0-1.5 g/kg body weight daily during active treatment.
For a 70 kg (154 lb) patient, this translates to 70-105 grams of protein daily—substantially higher than the standard recommendation for healthy adults.
Protein quality matters:
- Whey protein isolate: complete amino acid profile with 8.8% leucine content, fast-absorbing
- Pea protein: hypoallergenic and lactose-free, with comparable amino acid content to whey
Clinical trials show pea protein fortified with leucine stimulates muscle protein synthesis similarly to whey in aging populations, making it an excellent alternative for patients with dairy sensitivities.
One caveat: caloric needs must be met first. Without enough calories, the body burns protein for energy rather than using it for tissue repair—which makes calorie density the next priority.
Calories and Healthy Fats
When appetite is severely limited during active treatment, every sip must count. High-calorie, low-volume ingredients let patients meet energy needs without forcing large portions.
Healthy fat sources efficiently boost calorie content without increasing volume:
- MCT oil: 115 calories per tablespoon
- Avocado: 240 calories per fruit
- Full-fat coconut milk: 445 calories per cup
- Nut butters: 190-200 calories per 2 tablespoons
Beyond calorie density, omega-3 fatty acids deserve special attention. A 2024 dose-response meta-analysis found omega-3 supplementation significantly increases body weight in cancer cachexia patients, with particularly strong effects in older patients and those with lower baseline weight.
ESPEN guidelines suggest long-chain omega-3 fatty acids to stabilize or improve appetite, food intake, and body weight in advanced cancer patients undergoing chemotherapy.
Anti-Inflammatory and Functional Nutrients
Certain micronutrients and phytonutrients show particular promise in oncology nutrition:
- Vitamin D: Lower serum vitamin D levels correlate with higher cancer mortality; supplementation may reduce cancer mortality by 13% over 3-10 years of follow-up
- Selenium: Supports key antioxidant enzymes that protect cells from oxidative stress during treatment
- Curcumin: At 3g daily in prostate cancer patients receiving radiation, curcumin produced lower PSA levels and fewer side effects—though poor bioavailability requires advanced delivery forms
A note on antioxidant supplements during treatment:
The NCI and ASCO strongly caution against high-dose antioxidants (vitamins C and E) during chemotherapy and radiation. These supplements may shield cancer cells from the oxidative damage that treatment is designed to cause, potentially reducing efficacy.
Clinical studies link antioxidant supplement use during treatment to increased mortality risk and worsened recurrence-free survival. Always confirm antioxidant use with your oncologist before starting active treatment.
What to Check on the Label Before Buying
Beyond vitamins and minerals, all other ingredients should be recognizable whole-food sources. Unfamiliar synthetic additives, artificial flavors, and excessive preservatives are worth avoiding — especially for patients with compromised digestion.
Once you've confirmed the ingredient list looks clean, the next step is checking the numbers.
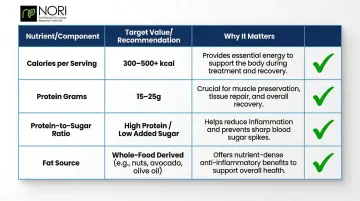
Key numbers to evaluate:
| Label Component | Target for Cancer Patients | Why It Matters |
|---|---|---|
| Calories per serving | 300-500+ | Supports caloric needs to prevent treatment-related weight loss |
| Protein grams | 15-25g | Meets elevated protein needs |
| Protein-to-sugar ratio | High protein, low added sugar | Limit added sugar to 25g daily for women, 36g for men |
| Fat source | Whole-food derived (coconut, MCT oil) | Better absorption, anti-inflammatory |
Additional checks:
- Allergen disclosures (dairy, soy, nuts)
- Third-party testing certification
- Whole-food vs. synthetic nutrient sources
- Expiration dates and storage requirements
Practical Tips for Incorporating Liquid Supplements Into Daily Routine
Small, consistent habits make liquid supplements easier to tolerate and more effective. A few approaches that work well:
- Consume supplements alongside whatever solid food you can manage rather than replacing meals — this maximizes total caloric intake
- Sip throughout the day rather than drinking a full serving at once, which helps prevent nausea or feeling too full to continue
Combat flavor fatigue:
- Rotate between multiple flavors or products weekly
- Serve supplements very cold or over ice (reduces taste intensity)
- Blend commercial shakes into homemade smoothies with cocoa powder, fruit, or nut butter
- Use flavor extracts (vanilla, almond) to change taste profiles
Palatability matters — but so does safety. Cancer treatments weaken the immune system, making food handling practices especially important for patients preparing homemade blends.
Food safety for immunocompromised patients:
- Wash all produce thoroughly under warm running water
- Avoid raw eggs in homemade smoothies
- Use only pasteurized dairy products
- Refrigerate blended drinks within 2 hours (1 hour if temperature exceeds 90°F)
- Consume leftovers within 48 hours maximum
- Use clean blenders and containers for each batch
- Reheat leftovers to 165°F internal temperature

Going Beyond Calories: Targeted Nutritional Support for Cancer Recovery
Mainstream liquid supplement guidance focuses primarily on preventing malnutrition—maintaining weight and muscle mass during treatment. This approach is essential, but integrative oncology research explores how specific nutritional strategies may support the body's ability to manage cancer at a cellular level. Integrative oncology combines conventional treatments with complementary therapies to optimize health, quality of life, and clinical outcomes through evidence-informed, patient-centered care.
One particularly promising area involves targeted dietary interventions that exploit metabolic vulnerabilities specific to cancer cells. Research on methionine restriction demonstrates that limiting this amino acid can reduce S-adenosylmethionine levels and sensitize tumors to chemotherapy in patients with metastatic colorectal cancer.
NORI's Integrative Approach
The Nutritional Oncology Research Institute (NORI) exemplifies this model. Built on over 20 years of focused research, NORI's protocol combines cycled methionine restriction (targeting a known metabolic vulnerability in cancer cells) with proprietary nutraceutical combinations designed to spare healthy tissue.
For patients ready to move beyond standard calorie-replacement supplementation, NORI's program offers:
- Home-based support with no clinic visits required
- Free initial consultations with program specialists
- Remote delivery via phone and Zoom for patients worldwide
- Continuous guidance throughout the program
Patients interested in evidence-based metabolic approaches to cancer management can schedule a free initial consultation to explore whether this level of targeted nutritional support fits their treatment plan.
Frequently Asked Questions
What is the best supplement for cancer patients?
The right supplement depends on cancer type, treatment protocol, and current nutritional status. Calorie-dense, protein-rich liquid supplements are broadly recommended for patients experiencing weight loss. Specialized nutraceuticals should only be introduced under medical guidance.
Are liquid supplements safe to use during chemotherapy or radiation?
Most calorie-focused liquid supplements are generally safe, but high-dose antioxidants and herbal supplements can potentially interfere with treatment efficacy by protecting cancer cells from intended oxidative damage. Always consult your oncologist or registered dietitian before starting any supplement during active treatment.
How many calories should a cancer patient get from liquid supplements per day?
Caloric needs vary by body weight, cancer type, and treatment intensity. A registered dietitian specializing in oncology should determine personalized targets, but liquid supplements contributing 500–1,000 calories daily are common recommendations for patients with significant appetite loss.
What should I look for on a liquid supplement label as a cancer patient?
Key label factors to evaluate:
- Calorie density: 300–500+ calories per serving
- Protein quality: Whole-food derived, 15–25g per serving
- Sugar content: Minimal added sugars
- Additives: Few artificial ingredients
- Testing: Third-party certification for purity and potency
Can I make my own liquid supplements at home?
Yes, homemade smoothies are a valid and customizable alternative to commercial products. Calorie-boosting additions like avocado, nut butters, coconut milk, and plant-based protein powder work well for most patients.
When should a cancer patient use liquid nutrition instead of solid food?
Liquid nutrition is most appropriate when solid food intake is significantly reduced due to nausea, mouth sores, swallowing difficulties, or severe appetite loss. It's best used alongside solid foods when tolerated, not as a permanent replacement unless medically necessary.
Note: This article provides educational information and should not replace personalized medical advice. Always consult your oncology care team before making significant changes to your nutrition plan or starting new supplements during cancer care.


