
Conventional oncology has historically centered on surgery, chemotherapy, and radiation—treating the tumor while often neglecting the metabolic and nutritional environment that influences cancer progression. Research increasingly reveals that what patients eat, which natural compounds they use, and how they manage lifestyle factors can meaningfully affect treatment tolerance, tumor behavior, and long-term outcomes. Yet the gap between this evidence and clinical practice remains wide.
This article explores the clinical evidence behind integrative nutrition for cancer, key dietary strategies grounded in research, the role of evidence-based nutraceuticals, and how patients can build a science-backed nutrition plan that complements or, in select cases, serves as a primary intervention.
TLDR:
- Malnutrition affects 30-80% of cancer patients, yet access to oncology dietitians is severely limited
- High-quality post-diagnosis diets reduce breast cancer mortality by up to 42% and prostate cancer mortality by 2.5 times
- Plant-rich, methionine-restricted diets exploit cancer cells' unique metabolic vulnerabilities
- Pro-oxidant nutraceuticals are being investigated for their interaction with cellular stress conditions associated with elevated ROS levels in cancer cells
- Early nutritional intervention improves treatment tolerance and reduces therapy toxicity
What Is Integrative Nutrition for Cancer?
Integrative nutrition for cancer is the evidence-informed use of diet, therapeutic foods, nutraceuticals, and lifestyle practices — whether alongside conventional oncology treatments or as a stand-alone approach. It's grounded in published research, clinical outcomes, and mechanistic understanding of how nutrition affects cancer biology.
How It Differs from General Healthy Eating
General wellness nutrition focuses on nutrient sufficiency, disease prevention, and overall health optimization. Integrative nutrition for cancer is fundamentally different—it uses food and compounds strategically to target cancer cell biology. Specific goals include:
- Disrupting metabolic pathways cancer cells depend on
- Reducing treatment toxicity and side effects
- Supporting immune surveillance and tumor clearance
- Preventing malnutrition and muscle wasting
- Lowering recurrence risk through metabolic reprogramming
The American Institute for Cancer Research (AICR) and World Cancer Research Fund (WCRF) framework emphasizes plant-rich, whole-food dietary patterns linked to improved survival and reduced cancer progression. The goal is selecting specific foods that modulate inflammation, insulin signaling, and oxidative stress in ways that directly affect tumor behavior — not generic healthy eating.
The Unmet Need: Malnutrition and Access Gaps
Research shows that malnutrition affects 30-80% of cancer patients, with the highest rates in pancreatic (80-85%), stomach (65-85%), and head/neck cancers (65-75%). Malnutrition drives worse treatment outcomes, higher toxicity, and increased mortality.
Yet access to specialized nutritional care remains critically limited — the US outpatient oncology dietitian-to-patient ratio is 1:2,308, against a desirable ratio of 1:120. That gap is precisely why proactive, patient-driven nutritional intervention matters — and why organizations like NORI exist to fill it with accessible, home-based support.
The Evidence: How Diet and Nutrition Impact Cancer Outcomes
What Major Organizations Say
The American Cancer Society, AICR/WCRF, and the Society for Integrative Oncology (SIO) all recommend plant-rich, whole-food dietary patterns for cancer patients. These recommendations are grounded in evidence linking high-quality diets to:
- Improved treatment response
- Reduced tumor growth signals
- Better survival across multiple cancer types
Nutrition is a modifiable factor with direct biological impact on cancer outcomes.
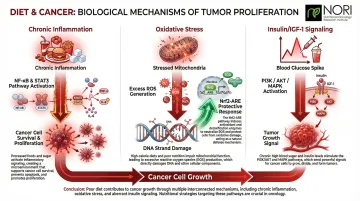
Biological Mechanisms: How Diet Affects Cancer
Poor diet quality creates a biological environment that promotes cancer cell growth. Key mechanisms include:
- Chronic inflammation: Processed foods, red meat, and refined sugar drive systemic inflammation through NF-κB and STAT3 pathways, promoting cancer cell survival and proliferation.
- Oxidative stress: Mitochondrial overload generates reactive oxygen species (ROS), causing DNA damage. Antioxidant-rich plant foods protect normal cells by activating the Nrf2-ARE pathway, while pro-oxidant strategies are being investigated in nutritional oncology research for how they may interact with the elevated oxidative conditions characteristic of cancer cells.
- Insulin and IGF-1 signaling: High-sugar diets and obesity trigger hyperinsulinemia, activating PI3K/AKT and MAPK pathways — delivering a direct growth signal to tumor cells.
Clinical Evidence: Diet Quality and Survival
Breast Cancer: A Women's Health Initiative study of 2,295 postmenopausal breast cancer survivors found that women whose diet quality decreased post-diagnosis had a 66% higher risk of breast cancer-specific death. Conversely, maintaining a high-quality diet was associated with 26% lower all-cause mortality and 42% lower non-breast cancer mortality.
Prostate Cancer: The Physicians' Health Study found that men with prostate cancer who followed a Western dietary pattern (high in processed meats, high-fat dairy, refined grains) had 2.53 times higher prostate cancer-specific mortality compared to those with healthier patterns.
Across cancer types, the gap between high- and low-quality diets translates directly into survival outcomes.

Cancer Cells' Metabolic Vulnerabilities
Cancer cells have abnormal metabolic needs visible on PET scans, which use radioactive glucose (FDG) to detect tumors. Because cancer cells consume glucose at far higher rates than normal cells, they light up on imaging — a phenomenon called the Warburg effect. This glucose dependency is a targetable vulnerability.
Beyond glucose, cancer cells depend heavily on specific amino acids like methionine. Restricting methionine through diet selectively stresses tumor metabolism while leaving normal cells largely unharmed — called the Hoffman effect. These two vulnerabilities form the biological basis of NORI's methionine-restriction protocol.
Early Intervention Improves Treatment Tolerance
A meta-analysis published in Annals of Oncology found that early dietary counseling with nutritional supplements reduced grade 3-4 infections from 10% to 4% compared to routine care. Early nutritional support also significantly reduced mortality in hospitalized cancer patients.
Starting nutritional support at diagnosis — rather than after treatment complications emerge — produces measurably better outcomes across infection rates, treatment tolerance, and survival.
Evidence-Based Dietary Strategies for Cancer Patients
Core Dietary Framework: Plant-Based, Whole-Food, Anti-Inflammatory
An evidence-based health-supporting diet emphasizes:
High intake of:
- Cruciferous vegetables (broccoli, kale, Brussels sprouts)
- Deeply pigmented berries (blueberries, blackberries)
- Orange and yellow vegetables (carrots, sweet potatoes)
- Anti-inflammatory spices (turmeric, ginger, garlic)
- Omega-3-rich cold-water fish (salmon, sardines, mackerel)
Minimal or eliminated:
- Processed meats (classified by WHO as Group 1 carcinogens)
- Red meat (Group 2A probable carcinogen)
- Refined sugar and simple carbohydrates
- Alcohol
- Highly processed foods
The risk data is concrete: each 50-gram portion of processed meat eaten daily increases colorectal cancer risk by 18%. These foods carry documented mechanisms that actively promote cancer progression.
The Case Against Refined Sugar
Sugar—especially refined, added sugar—elevates insulin and IGF-1, both of which promote inflammation and provide growth signals to cancer cells. The distinction matters: whole fruit with fiber behaves differently than extracted fruit juice or added sugar, which is stripped of fiber and spikes blood glucose just like other sugary drinks.
Limiting sugar isn't about eliminating fruit—it's about avoiding concentrated, fiber-free sources that fuel tumor growth.
Anti-Inflammatory Foods and Their Mechanisms
Specific foods contain bioactive compounds that modulate cancer-relevant pathways:
- Cruciferous vegetables contain glucosinolates and sulforaphane, which activate the Nrf2-ARE antioxidant pathway and suppress NF-κB, STAT3, PI3K/AKT, and MAPK signaling
- Omega-3 fatty acids from fish reduce pro-inflammatory cytokines (TNF-α, IL-6) and support immune function
- Polyphenols from berries and green tea exert antioxidant and immunomodulatory effects by targeting NF-κB

Each of these compounds has documented molecular mechanisms, making the dietary guidance specific rather than general.
Methionine Restriction: A Targeted Strategy
Cancer cells have a heightened dependency on methionine, a sulfur-containing amino acid, compared to normal cells. This metabolic quirk, called the Hoffman effect, means cancer cells cannot proliferate when methionine is replaced with its precursor, homocysteine, while normal cells remain unaffected.
Practical application: A plant-centered diet is naturally lower in methionine than animal-based diets. Cycled methionine restriction—alternating periods of strict limitation with normal eating—can selectively stress tumor metabolism.
This strategy forms a core element of evidence-based protocols like the NORI Protocol, which combines a methionine-restricted plant-based diet with targeted nutraceuticals to exploit cancer cells' metabolic vulnerabilities.
Common Dietary Questions
Soy: Large studies confirm that whole-food soy consumption is safe and beneficial for breast cancer survivors, including those with ER+ disease and tamoxifen users. The Shanghai Breast Cancer Survival Study found that highest soy protein intake was associated with 33% lower mortality and 34% lower recurrence. This applies to whole soy foods, not concentrated isoflavone supplements.
Dairy: Worth limiting due to associations with hormone-driven cancers and IGF-1 elevation.
Ketogenic Diet: Systematic reviews conclude there is inadequate and inconclusive evidence to support ketogenic diets for wellness-supporting effects or improved survival. While the diet may improve metabolic markers like fasting glucose and insulin, it restricts cancer-protective plant foods and shows low patient adherence.
Organic Foods: Preferable to reduce pesticide and chemical exposure, supporting a comprehensive integrative strategy.
Nutraceuticals and Targeted Supplements in Cancer Care
Not All Supplements Are Equal
Some nutraceuticals have strong mechanistic and clinical data supporting oncology use. Others lack evidence or may interfere with treatment. The distinction is critical.
Evidence-based examples:
- Omega-3 fatty acids: Safe and beneficial for nutritional status in pancreatic cancer patients; reduce pro-inflammatory cytokines and complications in GI cancers
- Modified citrus pectin (MCP): A phase II trial in biochemically relapsed prostate cancer showed 85% of patients had durable long-term response after 18 months, with 62% showing decreased/stable PSA
- Vitamin D: Supplementation significantly reduced total cancer mortality in randomized trials, though it did not reduce cancer incidence
Bioactive Plant Compounds and Mechanisms
Nutraceutical-grade compounds work at a molecular level:
- Glucosinolates/Sulforaphane activate antioxidant defenses and suppress pro-survival signaling
- Polyphenols target inflammatory pathways (NF-κB) that drive tumor progression
- Medicinal mushroom extracts (e.g., lentinan) activate immune cells—T cells, NK cells, macrophages—through pattern recognition receptors
These aren't general wellness boosters—they modulate specific cancer-relevant pathways.
Quality, Formulation, and Safety
Supplement safety and efficacy depend heavily on purity, dosage, and formulation. Some supplements interfere with chemotherapy—for example, St. John's Wort significantly decreases the efficacy of docetaxel and ixabepilone by inducing metabolic enzymes that clear these drugs faster.
Critical guidelines:
- Disclose all supplements to your oncology team
- Work with a practitioner experienced in oncology nutrition
- Choose pharmaceutical-grade products with third-party testing
NORI's Approach to Nutraceutical Development
Those manufacturing standards matter in practice. The Nutritional Oncology Research Institute (NORI) develops and produces its own nutraceuticals in-house, selecting compounds based on cancer-specific mechanisms rather than general wellness applications.
The NORI Protocol, built on over 20 years of research, centers on cycled methionine restriction paired with nutraceutical combinations that support metabolic wellness. Documented case reports across breast, prostate, and thyroid cancers have shown client-reported wellness improvements in patients on the protocol.

Beyond Diet: Lifestyle Factors That Strengthen Nutritional Therapy
Physical Activity as a Co-Intervention
Regular exercise complements nutritional therapy by:
- Reducing systemic inflammation
- Improving insulin sensitivity
- Counteracting cancer-related fatigue
- Supporting healthy body composition
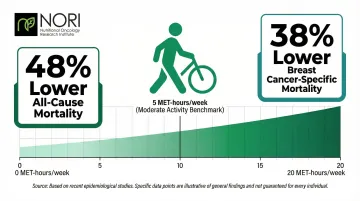
A 2023 meta-analysis found that post-diagnosis physical activity up to 20 MET-hours/week was associated with 48% lower all-cause mortality and 38% lower breast cancer-specific mortality. That translates to roughly five hours of moderate activity per week cutting breast cancer death risk by more than one-third.
Stress Reduction, Sleep, and Cancer Progression
Chronic stress and poor sleep disrupt cortisol regulation, suppress immune function, and create conditions that drive cancer progression. Stress activates the sympathetic nervous system, releasing catecholamines that stimulate tumor angiogenesis, cell migration, and invasion.
Mind-body interventions — meditation, yoga, tai chi, and guided relaxation — improve patient-reported anxiety, fatigue, sleep quality, and depression. Pilot studies from MD Anderson's Integrative Medicine Center show meaningful reductions in anxiety, fatigue, and depression scores from self-administered practices.
Sleep disturbances suppress NK cell and cytotoxic T-cell activity, facilitating tumor immune evasion. Consistent sleep schedules, limiting screen exposure before bed, and managing nighttime cortisol through stress practices are practical starting points for any integrative care plan.
Environmental Toxin Reduction
Reducing exposure to environmental carcinogens supports comprehensive integrative strategy:
- Choose organic produce when possible
- Limit processed food chemicals and additives
- Reduce alcohol consumption (alcohol is a Group 1 carcinogen)
- Avoid unnecessary pesticide and herbicide exposure
AICR guidelines support each of these steps, and reducing total toxic burden gives nutritional interventions a cleaner biological environment in which to work.
How to Build Your Integrative Nutrition Support Plan
Start Early and Make It Personalized
Research consistently shows nutrition should be integrated from diagnosis, not as an afterthought. Each patient's plan should be individualized based on:
- Cancer type and stage
- Treatment protocol (surgery, chemotherapy, radiation, hormonal therapy)
- Body composition and nutritional status
- Concurrent health conditions
- Personal preferences and cultural food practices
Even a single nutrition consultation has shown statistically significant improvements in self-reported symptoms, but ongoing support produces more meaningful and lasting change.
NORI's Home-Based Program: An Accessible Starting Point
That ongoing support is exactly what NORI's home-based nutritional program is built around. The program includes:
- Free initial consultations to assess individual circumstances
- Customized diet plans and nutraceutical protocols
- Unlimited ongoing support via phone and Zoom
- All nutraceuticals manufactured in-house to guarantee potency and purity
The program serves patients with breast, prostate, thyroid, and advanced cancers — whether they're augmenting standard treatment or have exhausted conventional options. Flat-fee monthly, yearly, and lifetime plans keep costs lower than most integrative cancer support programs.
To learn more or schedule a free consultation, contact NORI at 800-634-3804 or info@nutritionaloncology.net.
Frequently Asked Questions
What is an integrative treatment for cancer?
Integrative cancer care combines conventional oncology (surgery, chemotherapy, radiation) with evidence-based complementary approaches — nutritional therapy, nutraceuticals, exercise, stress reduction, and mind-body practices — to improve treatment outcomes, reduce side effects, and support quality of life throughout the treatment process.
How does diet affect cancer treatment outcomes?
Diet quality impacts tumor growth, treatment response, side effect severity, and survival. High-quality plant-rich diets are linked to reduced cancer mortality, while poor dietary patterns high in sugar and processed foods correlate with worse outcomes across multiple cancer types.
What foods should cancer patients avoid?
Cancer patients should minimize or eliminate refined sugar, processed meats (a WHO Group 1 carcinogen), red meat, alcohol, and highly processed foods. These are consistently linked to increased cancer risk and worse outcomes.
Can nutritional therapy replace conventional cancer treatment?
Many patients use integrative nutrition alongside conventional treatment to enhance outcomes and reduce toxicity. Others — particularly those who have exhausted standard options or are choosing to avoid chemotherapy — pursue nutrition-centered protocols as their primary approach. Either way, the strategy should be individualized based on cancer type, stage, and personal goals.
What is methionine restriction in cancer care?
Methionine is an amino acid that cancer cells depend on more heavily than normal cells. Restricting it through a cycled, low-methionine plant-centered diet can selectively stress tumor metabolism. This approach is central to research-based protocols like the NORI Protocol.
How do I know which supplements are safe during cancer treatment?
Supplement safety in oncology depends on the specific compound, dosage, cancer type, and current treatment. Some — like omega-3s and certain plant compounds — have strong supporting evidence, while others may interfere with chemotherapy. Disclose all supplements to your oncology team and consult a practitioner trained in integrative oncology nutrition before starting any protocol.


