
Introduction
Conventional cancer treatments — surgery, chemotherapy, radiation — can carry side effects severe enough to reshape daily life. That's why so many patients look beyond standard care, searching for approaches that help manage symptoms, support recovery, and restore a sense of control. The challenge: the information landscape is full of contradictions, mixing legitimate evidence-based options with outright fraudulent "cure" claims.
This guide covers the most studied holistic and natural medicine approaches — mind-body therapies, nutritional oncology, plant-derived nutraceuticals, and movement-based practices — so you can make informed decisions alongside your care team, not instead of it.
TLDR
- Integrative oncology pairs evidence-based complementary therapies with conventional treatment for better outcomes
- Skipping conventional treatment entirely increases mortality risk up to 5.68-fold — complementary approaches work best alongside standard care
- Mind-body interventions like MBSR reduce anxiety by 51% and depression by 73% in cancer patients
- Nutritional oncology targets cancer cell metabolism through dietary strategies like methionine restriction
- Acupuncture effectively reduces chemotherapy-induced nausea, pain, and hot flashes per NCCN guidelines
- Always disclose all complementary approaches to your oncology team to prevent dangerous herb-drug interactions
What Does "Holistic Cancer Care" Actually Mean?
Understanding the Key Terms
Cancer patients encounter confusing terminology when exploring holistic options. Complementary medicine refers to non-mainstream approaches used alongside conventional treatment, while alternative medicine means using therapies instead of standard medical care. Integrative oncology represents the gold standard: evidence-based complementary approaches coordinated with your oncology team.
The term "holistic" means treating the whole person — physical, mental, emotional, and spiritual — not just the disease itself.
The Critical Distinction: Complementary vs. Alternative
Holistic cancer care does not mean abandoning conventional medicine. Patients who choose alternative therapies over conventional cancer care face a 2.50-fold increased risk of death overall. For breast cancer specifically, using alternative medicine instead of conventional cancer care results in a 5.68-fold increased risk of death.
The integrative approach expands your treatment options — adding evidence-based nutritional, mind-body, and supportive therapies on top of, not in place of, proven medical care. That distinction is precisely why major cancer centers have built formal integrative medicine programs.
Growing Mainstream Acceptance
Major cancer centers now recognize the value of evidence-based complementary care:
- Memorial Sloan Kettering established its Integrative Medicine Service in 1999
- MD Anderson Cancer Center founded its Integrative Medicine Program in 1998
- SIO and ASCO publish joint clinical practice guidelines recommending specific complementary therapies
- NCCN Adult Cancer Pain guidelines reference acupuncture, massage, and cognitive behavioral therapy as supportive options
When these institutions dedicate entire departments to integrative care, it reflects genuine clinical evidence — not trend-chasing. The sections ahead break down which specific therapies have earned that institutional endorsement and why.

Evidence-Based Mind-Body Therapies for Cancer Patients
Meditation and Mindfulness-Based Stress Reduction (MBSR)
MBSR is an 8-week structured program combining mindfulness meditation, body awareness, and gentle movement. It's one of the most researched mind-body interventions in oncology.
A 2020 meta-analysis in JAMA Network Open analyzing 28 randomized controlled trials with 3,053 cancer patients found that MBSR significantly reduced:
- Short-term anxiety by 51% (Standardized Mean Difference -0.51)
- Short-term depression by 73% (SMD -0.73)
How to access mindfulness practice:
- Hospital-based programs at major cancer centers
- UMass Memorial Health online MBSR programs
- MSK's Integrative Medicine at Home guided meditations
- Smartphone apps like Calm, Headspace, and Insight Timer
Many cancer centers now offer MBSR during active treatment, making it one of the few mind-body practices patients can begin at diagnosis rather than waiting until after treatment ends.
Yoga and Tai Chi
A 2024 meta-analysis in Medicine (18 studies) demonstrated that yoga reduces cancer-related fatigue in breast cancer patients (SMD -0.51) while improving:
- Sleep quality (Mean Difference -3.86)
- Overall quality of life (MD -11.20)
These are statistically significant findings across small-to-moderate effect sizes, consistent with what integrative oncology researchers classify as clinically relevant improvements in patient-reported outcomes.
**Tai chi and qigong** offer lower-impact alternatives for patients with physical limitations. A 2020 meta-analysis of 9 RCTs found tai chi significantly alleviated:
- Cancer-related fatigue (SMD -1.29)
- Sleep quality (SMD -0.45)

Hypnosis and Guided Imagery
Clinical hypnosis provides targeted symptom relief when administered by trained, licensed providers.
Research supports its use across several common treatment-related symptoms:
- Procedural anxiety and pain: A 2006 RCT in Pain showed hypnosis significantly decreased patient anxiety during large core breast biopsies
- Hot flashes: A 2008 RCT in Journal of Clinical Oncology found hypnosis reduced hot flash scores by 68% in breast cancer survivors
- Treatment-related nausea: Hypnosis reduces both anticipatory and chemotherapy-induced nausea
- Clinical recognition: The SIO-ASCO 2022 Pain Management guideline recommends hypnosis for procedural pain based on intermediate-quality evidence
Nutritional Oncology: How Diet Can Target Cancer at the Cellular Level
Beyond General Healthy Eating
Nutritional oncology goes far beyond eating more vegetables. Certain cancer cells have distinct metabolic vulnerabilities that may be targeted through specific dietary strategies—making diet an active component of cancer care, not just supportive.
Cancer Cell Metabolism and Nutrient Dependence
Some cancer cells are disproportionately dependent on specific amino acids compared to normal cells. This metabolic difference creates a potential therapeutic window.
Methionine restriction targets this vulnerability. Research demonstrates that cancer cells depend heavily on methionine—a sulfur-containing amino acid—for growth and survival. Depriving cancer cells of methionine through dietary restriction can slow cancer cell proliferation through several mechanisms:
- Glutathione depletion (cancer cells' primary antioxidant defense)
- Cell cycle arrest (halting division in the cell replication cycle)
- Increased oxidative stress selectively affecting malignant cells
Phase I/II clinical trials have shown that methionine depletion safely reduces serum methionine in metastatic cancer patients without significant side effects.
Broader Evidence for Anti-Inflammatory Dietary Patterns
What the research shows:
| Dietary Factor | Cancer Type | Finding | Source |
|---|---|---|---|
| Dietary fiber | Colorectal cancer | 16% decreased mortality risk per 10g/day fiber increase | Cancers 2022 |
| Pro-inflammatory diet | Stage III colon cancer | 87% higher risk of death compared to anti-inflammatory diets | ASCO 2025 |
| Plant-based diet | Breast cancer | No significant reduction in recurrence or mortality | WHEL Trial |
While anti-inflammatory and high-fiber diets significantly improve overall survival, large trials show plant-based diets alone do not support cancer wellness recurrence—underscoring the need for more targeted strategies.

Methionine Restriction as a Studied Dietary Strategy
Methionine restriction involves limiting sulfur-containing amino acids—methionine and cysteine—to approximately 10 mg/kg body weight per day. In practice, this means a predominantly plant-based diet emphasizing fruits and vegetables, while minimizing animal proteins, nuts, seeds, and grains.
This is the dietary foundation of NORI's home-based support program, which pairs cycled methionine restriction with nutraceutical combinations being studied for their role in oxidative stress pathways and cellular health, developed through over 20 years of focused research. Reducing protein intake — especially animal protein — without causing malnutrition is being explored in nutritional oncology research for its role in metabolic wellness and its relationship to IGF-1 levels. Cancer cells are known to have elevated ROS levels; these pro-oxidant agents are being investigated for how they may interact with these cellular conditions, with ongoing research into their selective effects. Natural pro-oxidant agents used in this approach include high-dose Vitamin C, piperlongumine, menadione, and certain carotenoids, which are also being explored alongside conventional care approaches in ongoing nutritional oncology research. Because the approach addresses metabolic patterns being researched in cancer cells, it has been applied to a broad range of diagnoses and stages — without requiring clinic visits. Free initial consultations are available at 800-634-3804 or info@nutritionaloncology.net.
Plant-Derived Nutraceuticals and Natural Compounds
What Are Nutraceuticals in Oncology?
Nutraceuticals are plant-derived bioactive compounds studied for their potential to inhibit cancer cell growth, reduce inflammation, and support immune function. These differ from general vitamins—quality, formulation, and dosage matter significantly.
Key Compounds with Clinical Research
| Compound | Mechanism | Evidence Status | Limitations |
|---|---|---|---|
| Curcumin (turmeric) | Inhibits NF-κB, PI3K/Akt, MAPK pathways | Phase I/II trials show variable inflammatory marker reduction | Extremely low oral bioavailability; requires nano-formulations |
| Quercetin | Modulates microRNA expression to stimulate tumor suppressor genes | Human efficacy studies remain sparse and inconclusive | Poor systemic bioavailability; rapid biotransformation |
| Resveratrol | Modulates p53, STAT3, NF-κB | Well-tolerated up to 1g/day; reduces inflammatory markers | Rapid metabolism prevents therapeutic plasma concentrations |
| EGCG (green tea) | Inhibits PI3K/Akt, EGFR signaling | Phase II trials show tissue accumulation in bladder cancer | Low oral bioavailability constrains systemic application |
Most evidence remains preclinical or from limited human trials—commercial supplements frequently fail to reach therapeutic concentrations.
That gap between promise and delivery is one concern. A more immediate one is safety.
Critical Safety Point: Herb-Drug Interactions
Some natural compounds actively interfere with cancer care.
St. John's Wort is particularly dangerous: it reduces the active metabolite of irinotecan (SN-38) by 42% and significantly lowers exposure to:
Any nutraceutical used alongside active cancer care should be reviewed for drug-herb interactions by a qualified practitioner before use.
Evaluating Nutraceutical Products
What to look for:
- USP Dietary Supplement Verification or NSF certification confirms the product contains what the label claims
- FDA cGMP compliance: Manufacturers must follow current Good Manufacturing Practices (21 CFR Part 111)
- In-house formulation with documented quality controls — rather than reselling third-party products — offers stronger assurance of potency and purity. NORI formulates and manufactures its own nutraceuticals at its own facility for this reason
Acupuncture, Massage, and Other Body-Based Approaches
Acupuncture for Cancer Symptom Management
Acupuncture is now referenced in NCCN guidelines as a standard supportive approach for specific symptoms.
Evidence from meta-analyses:
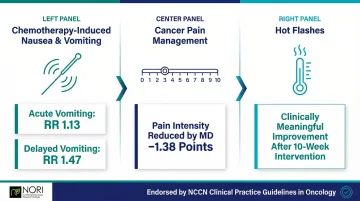
- Chemotherapy-induced nausea: Increases complete control of acute vomiting (RR 1.13) and delayed vomiting (RR 1.47)
- Cancer pain: Significantly reduces pain intensity (Mean Difference -1.38 points)
- Hot flashes: Clinically meaningful improvements after 10-week intervention
Massage Therapy in Cancer Care
Evidence suggests massage provides benefits for anxiety, pain, and general well-being. A meta-analysis in Integrative Cancer Therapies (12 studies) showed massage significantly reduced cancer pain, particularly surgery-related pain.
Important safety consideration: Oncology-trained massage therapists must modify pressure and technique in areas affected by cancer or treatment. They should also avoid lymphedema-risk areas entirely — practitioner specialization is essential, not optional.
Reflexology and Energy-Based Therapies
Where massage targets soft tissue directly, therapies like reflexology, Reiki, and therapeutic touch work through different mechanisms — cancer patients typically turn to them for stress relief and general well-being. A 2025 meta-analysis suggests Reiki therapy positively impacts overall quality of life.
The clinical evidence base for these therapies is still developing, but the risk profile is low and the comfort benefits are real for many patients — making them a reasonable complement to more evidence-backed interventions.
Safety Considerations and How to Get Started
Taking a holistic or integrative approach to cancer care requires two things above all: honest communication with your medical team and the ability to tell credible programs from predatory ones. The steps below give you a practical framework for both.
The Non-Negotiable Rule: Disclose Everything
All complementary and natural approaches must be disclosed to your oncology care team. This prevents dangerous interactions and ensures coordinated care.
Questions to ask your oncologist:
- Are there interactions between this approach and my current treatments?
- When should I implement this relative to chemotherapy cycles or radiation schedules?
- Are there specific contraindications based on my cancer type or stage?
Questions to ask complementary practitioners:
- What are your qualifications and experience with cancer patients?
- Are you willing to coordinate with my medical oncology team?
- Do you have liability insurance and professional credentials?
Distinguishing Evidence-Based Care from Fraud
The FDA identifies red flags for fraudulent cancer product claims:
- Promises to "cure" all forms of cancer
- Claims of being "more effective than chemotherapy"
- Pressure to replace conventional treatment
- Testimonials as primary evidence (not clinical trials)
- "Natural" or "alternative" claims without scientific support
The FTC warns that "natural" does not mean safe or effective, and patient testimonials are not substitutes for rigorous research.
Building Your Starting Point
With a clear picture of what to avoid, these practical steps help you move forward with confidence.
Practical steps:
- Discuss integrative options with your oncologist at your next appointment
- Seek programs that offer personalized guidance and continuous professional support — for example, NORI (Nutritional Oncology Research Institute) provides free initial consultations and a home-based nutritional support program accessible to patients worldwide (800-634-3804 or info@nutritionaloncology.net)
- Prioritize approaches backed by peer-reviewed clinical evidence
- Start with low-risk interventions like mindfulness, yoga, or dietary improvements

Frequently Asked Questions
What is the 62-day rule for cancer?
The 62-day rule refers to a benchmark goal in cancer care to initiate treatment within 62 days of a patient's initial cancer-related visit or referral. Research links delays beyond this window to worse survival outcomes—even a 4-week treatment delay increases colorectal cancer mortality by 14%.
Can natural medicine cure cancer on its own?
No natural or complementary approach has been scientifically proven to cure cancer. Using natural medicine as sole treatment in place of conventional care is associated with worse outcomes, including up to a 5.68-fold increased risk of death for breast cancer. However, evidence-based natural approaches can support recovery and quality of life when used alongside standard oncology care.
Is it safe to take herbal supplements during chemotherapy?
Some herbal supplements interfere with chemotherapy effectiveness or increase toxicity. St. John's Wort reduces irinotecan's active metabolite by 42% and lowers imatinib and docetaxel exposure. Review all supplements with your oncology team before use—disclosure is mandatory for safety.
What is the difference between integrative and alternative cancer care?
Integrative oncology uses evidence-based complementary approaches alongside conventional cancer care to manage symptoms and improve quality of life. Alternative medicine refers to using non-conventional approaches instead of standard treatment—a distinction that directly affects survival outcomes.
How does diet affect cancer care outcomes?
Diet shapes immune function, treatment tolerability, and cancer cell behavior. High dietary fiber intake alone reduces colorectal cancer mortality by 16% per 10g/day increase, and approaches like plant-based eating and anti-inflammatory diets are actively being studied for their impact on treatment outcomes.
What should I look for when choosing a holistic cancer care program?
Prioritize programs that are evidence-based, staffed by credentialed professionals, and transparent about coordinating with your oncology team. They should clearly distinguish supportive approaches from unproven cure claims. A free initial consultation lets you assess fit before committing.


