
This guide covers the key pillars of integrative cancer care, the science behind them, and practical tools patients can use—including those available from home.
TLDR:
- Integrative medicine combines conventional treatment with evidence-based complementary approaches like nutrition, mind-body practices, and nutraceuticals
- Anti-inflammatory diets (Mediterranean, plant-based) reduce cancer recurrence risk by 17% for colorectal cancer
- Exercise reduces breast cancer mortality by 31% through wellness-supporting "myokines"
- Sleep disturbance affects 60% of cancer patients and accelerates tumor growth
- Social isolation increases breast cancer mortality risk by 64%
What Is Integrative Medicine for Cancer Patients?
Integrative medicine in oncology combines evidence-based conventional treatment—surgery, chemotherapy, radiation—with complementary approaches such as nutrition, mind-body practices, acupuncture, and nutraceuticals. It treats the whole person, not just the disease.
Integrative vs. Alternative Medicine: A Critical Distinction
The distinction between integrative and alternative medicine is life-or-death important. Integrative therapies are used alongside standard care to improve quality of life and outcomes. Alternative medicine replaces standard care—and research shows this approach increases mortality risk 2-fold for curable cancers.
A landmark 2018 study analyzing 1.9 million cancer patients found that those who chose alternative medicine over conventional treatment were significantly more likely to die.
The Society for Integrative Oncology (SIO) and ASCO have since issued joint guidelines supporting complementary approaches when used alongside — not instead of — standard care.
Growing Acceptance and Patient Demand
Studies estimate 31-54% of cancer patients in Asia currently use complementary approaches, with comparable rates reported worldwide. The pattern points to real gaps that standard treatment alone often leaves unaddressed:
- Persistent pain during and after treatment
- Fatigue that doesn't respond to rest
- Anxiety, depression, and emotional distress
- Declining quality of life between treatment cycles
Institutional medicine has taken notice. Major cancer centers including Memorial Sloan Kettering and MD Anderson now offer dedicated integrative oncology programs — a signal that patient demand has reached a scale too large to ignore.
Nutrition as a Foundation of Integrative Cancer Care
Nutrition is central to integrative oncology. Chronic inflammation driven by poor diet enables cancer progression, while whole-food, plant-rich, anti-inflammatory dietary patterns reduce cancer incidence and improve survival.
Living with overweight or obesity increases the risk of at least 13 cancer types—including bowel, breast, and pancreatic—through insulin resistance, elevated IGF-1, and altered adipokine signaling that creates a tumor-promoting environment.
Dietary Patterns That Reduce Cancer Recurrence
The evidence for post-diagnosis dietary intervention is substantial:
| Diet Pattern | Cancer Type | Key Findings |
|---|---|---|
| Mediterranean Diet | Colorectal | 17% lower recurrence risk (HR=0.83) |
| Plant-Based Diet | Prostate | 47% lower progression risk (HR=0.53) |
| Low-Fat Dietary Pattern | Breast | 22% better 10-year survival (HR=0.78) |
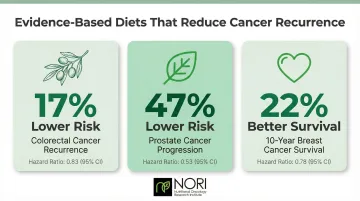
These plant-forward diets reduce inflammatory markers, improve omega-6 to omega-3 ratios, and provide antioxidants and phytochemicals that inhibit cancer-related biological pathways including cell proliferation and angiogenesis.
The Gut Microbiome and Cancer Progression
Diet shapes the microbiome, which regulates immune function and influences cancer progression. Patients responding to anti-PD-1 immunotherapy have significantly higher diversity of beneficial gut bacteria like Akkermansia muciniphila.
Antibiotic exposure within 30 days before checkpoint inhibitors significantly reduces overall survival and progression-free survival by disrupting the microbiome. A 2023 study found any antibiotic use within one year before immunotherapy worsened survival outcomes. Protecting microbiome diversity — through fiber-rich foods, fermented foods, and judicious antibiotic use — should be an active part of nutritional planning during immunotherapy.
Protective Foods and Foods to Limit
Foods shown to be protective:
- Cruciferous vegetables (broccoli, cauliflower, kale) — associated with 23% lower cancer risk
- Berries rich in antioxidants
- Legumes (beans, lentils)
- Olive oil
- Green tea
Foods to limit or avoid:
- Processed meats
- Refined sugars
- Ultra-processed foods
- Excessive alcohol
Nutritional needs may change across treatment phases. Work with a qualified practitioner to personalize your approach.
Methionine Restriction and Targeted Nutritional Strategies
Beyond general dietary patterns, some targeted nutritional strategies exploit specific metabolic vulnerabilities within cancer cells. One of the most researched is methionine restriction.
Most cancer cells depend heavily on the amino acid methionine for growth and survival — a phenomenon called the Hoffman effect. Unlike normal cells, which can synthesize methionine through transsulfuration, many tumor cells cannot compensate when dietary methionine is reduced. The approach in practice:
- Follows a plant-based or largely vegan diet low in methionine-rich foods (meat, eggs, dairy)
- Cycles periods of restriction to maintain adherence and metabolic effect
- Often combines dietary restriction with targeted nutraceuticals to amplify impact
This is the foundation of the NORI Protocol, which pairs cycled methionine restriction — reducing animal protein without causing malnutrition is being explored in nutritional oncology research for its role in metabolic wellness and its relationship to IGF-1 levels — with proprietary nutraceutical combinations being studied for their role in oxidative stress pathways and cellular health, drawing on over two decades of focused research in nutritional oncology. Cancer cells are known to have elevated ROS levels; these pro-oxidant agents are being investigated for how they may interact with these cellular conditions, with ongoing research into their selective effects. Natural pro-oxidant agents used in this approach include high-dose Vitamin C, piperlongumine, menadione, and certain carotenoids — compounds also being explored alongside conventional care approaches in ongoing nutritional oncology research.
Early-phase human trials confirm safety, though dietary adherence is difficult and long-term survival data is still emerging. For patients interested in this approach, working with an experienced practitioner is essential.
Mind-Body and Physical Therapies for Cancer Support
Clinical anxiety and depression affect approximately 18-22% of cancer patients. For many, psychological distress isn't just a quality-of-life concern — it has measurable biological consequences.
Chronic stress activates the HPA axis, suppresses immune function, promotes systemic inflammation, and shapes the tumor microenvironment. This is why mind-body interventions are increasingly recognized as essential components of integrative cancer care, not optional add-ons.
Meditation, Yoga, and Relaxation Practices
Meditation and mindfulness reduce anxiety, fatigue, and sleep disturbance. A 2024 meta-analysis found mindfulness interventions produced large reductions in psychological symptoms (Hedges' g = -1.03) in cancer patients.
Yoga, tai chi, and qi gong pair gentle movement with breathwork and mindfulness. Research supports their use for:
- Cancer-specific quality of life
- Fatigue reduction (tai chi reduced fatigue with SMD = -1.29)
- Anxiety and mood
- Sleep quality
- Immune function

These practices are accessible across fitness levels and particularly valuable during and after treatment.
Acupuncture, Massage, and Body-Based Therapies
Body-based therapies extend support beyond what movement alone provides. Acupuncture is among the most studied integrative modalities, with RCT evidence supporting its use for:
- Chemotherapy-induced nausea and vomiting
- Cancer-related fatigue
- Pain management
- Xerostomia (dry mouth) following radiation
Many major cancer centers now include acupuncture within their supportive care services.
Oncology massage has clinical studies showing reductions in anxiety, pain, fatigue, nausea, and depression. Research also documents improvements in immune markers, including lymphocyte counts. Work with a massage therapist trained in oncology protocols to ensure safety.
Exercise as Medicine
Physical activity may be one of the most underutilized tools in cancer support. Large cohort studies show regular post-diagnosis exercise reduces breast cancer mortality by 31% (HR=0.69), with comparable benefits documented for prostate, lung, and colorectal cancers.
Exercise improves:
- All-cause mortality after diagnosis
- Fatigue and mood
- Immune function
- Treatment completion rates
The mechanism: Muscle contraction releases wellness-supporting "myokines" like SPARC. A 2012 study in Gut demonstrated that a single bout of exercise increased SPARC secretion, which inhibited colon tumorigenesis by increasing apoptosis in mice.

Both moderate and vigorous exercise provide benefits. Start where you are and gradually increase intensity with your care team's guidance.
Key Modifiable Lifestyle Factors Affecting Cancer Outcomes
Diet and exercise get most of the attention, but sleep, vitamin D, social connection, and behavioral exposures carry just as much weight in cancer outcomes. The research here is specific — and actionable.
Sleep's Critical Role
60% of cancer patients experience sleep disturbance. Poor sleep dysregulates melatonin, circadian rhythms, and immune surveillance—all of which affect cancer progression.
A meta-analysis found insomnia was associated with modest but meaningful increased cancer risk. Animal models show fragmented sleep accelerates tumor growth through recruitment of tumor-associated macrophages.
Practical steps:
- Maintain consistent sleep/wake times
- Limit screen time before bed
- Create a dark, cool sleep environment
- Address pain and anxiety that disrupt sleep
Vitamin D Deficiency
Lower vitamin D levels are associated with higher cancer-related and all-cause mortality. Vitamin D promotes apoptosis, inhibits angiogenesis, and has anti-proliferative activity.
While a meta-analysis found vitamin D supplementation didn't reduce overall cancer incidence, it was associated with 13% reduced cancer mortality over 3-10 years.
Sunlight exposure is the primary source. Ask your oncology team about testing your levels and whether supplementation makes sense for your situation.
Social Connection and Psychological Wellbeing
This isn't just comfort—it's biology. Social isolation in breast cancer patients increases recurrence risk by 43%, breast cancer mortality by 64%, and total mortality by 69%, even after adjusting for lifestyle and treatment factors.
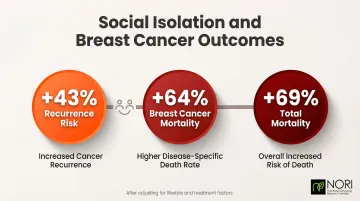
Strong social support meaningfully improves survival. Seek support groups, counseling, and community connections.
Smoking, Alcohol, and Environmental Exposures
Both smoking and alcohol drive chronic inflammation and create conditions that support tumor growth — even in patients already undergoing treatment. Reducing or eliminating these exposures can meaningfully support your body's response to therapy.
Steps to take now:
- Talk to your oncology team about cessation support for smoking
- Reduce or eliminate alcohol during active treatment
- Minimize occupational or household chemical exposures where possible
- Review any environmental risk factors with your care team
Nutraceuticals and Herbal Medicine in Integrative Oncology
Not all supplements are created equal — and in oncology, the difference between strategic, evidence-informed nutraceutical use and indiscriminate supplementation can affect both safety and outcomes.
Examples With Scientific Backing
Curcumin shows anti-inflammatory and anti-proliferative properties, modulating multiple cancer pathways. However, clinical translation is limited by poor systemic bioavailability, requiring nanoformulations or adjuvants.
Selenium has antioxidant and anti-angiogenic properties. The SELECT trial, however, was discontinued early due to absence of benefit for prostate cancer prevention and concerns over increased diabetes risk.
Probiotics support gut microbiome and immune regulation. A 2025 meta-analysis showed probiotics reduced chemotherapy-induced diarrhea risk by 49% (RR=0.51) in colorectal cancer patients. They may also prolong survival in patients receiving immunotherapy, particularly mitigating antibiotic damage.
The Antioxidant Controversy
There's a common misconception that antioxidants interfere with chemotherapy. Systematic review evidence shows antioxidant supplementation during chemotherapy does not reduce efficacy and can reduce toxicity and improve outcomes in some contexts.
That said, a prospective study found antioxidant supplement use before and during breast cancer care was associated with increased recurrence risk (HR=1.41). Given this conflicting data, timing, dosage, and supplement type all matter — discuss specifics with your oncology team before starting any antioxidant regimen.
Safety Considerations and Drug-Supplement Interactions
Some herbs and supplements interfere with cancer drugs:
- St. John's Wort reduces irinotecan effectiveness by 42%—concurrent use is contraindicated
- High-dose vitamin C may affect radiation sensitivity in some contexts
Disclose all supplement use to your oncology team. Programs developed under scientific oversight — like those from NORI, which formulates and manufactures all nutraceuticals at its own facility — offer a meaningful alternative to generic off-the-shelf supplements, where sourcing and formulation controls vary widely.
Building an Integrative Cancer Care Plan That Works for You
The Team-Based Approach
Integrative oncology works best when complementary practitioners communicate with your oncology team. Inform your oncologist about all supplements, dietary changes, and therapies, and seek practitioners with oncology-specific training.
Addressing Accessibility
Not all patients have access to clinic-based integrative oncology programs, which can be expensive and geographically limited. Home-based nutritional support programs — such as those offered by NORI (Nutritional Oncology Research Institute) — can fill this gap, providing remote consultations, personalized dietary protocols, and nutraceutical support without requiring clinic visits.
A Practical Starting Framework
Before layering in additional modalities, build your foundation around the most impactful and accessible pillars:
- Anti-inflammatory dietary changes — shift toward Mediterranean or plant-based patterns
- Stress reduction practices — try meditation, yoga, or tai chi
- Adequate sleep and vitamin D — prioritize sleep hygiene and test vitamin D levels
- Regular physical activity — start with moderate exercise and gradually increase
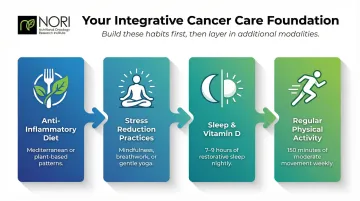
Establish these habits first, then introduce other modalities one at a time. Keep a symptom journal to track what's helping — and what isn't.
Frequently Asked Questions
Is integrative medicine good for cancer patients?
Yes, integrative medicine has substantial evidence for improving quality of life, reducing treatment side effects, and supporting overall outcomes when used alongside standard care. However, it is not a standalone cure and should complement, not replace, conventional treatment.
What is an integrative approach to cancer?
An integrative approach combines conventional cancer care (surgery, chemotherapy, radiation) with evidence-based complementary therapies—nutrition, mind-body practices, exercise, acupuncture, and nutraceuticals. It treats the whole person to improve both outcomes and quality of life.
Is integrative oncology covered by insurance?
Some integrative therapies—acupuncture, chiropractic, massage—are covered by certain insurance plans. Check with your insurer directly, ask your doctor for a referral when possible, and look into HSA/FSA accounts for out-of-pocket costs.
Is there such a thing as a holistic oncologist?
Integrative oncologists are physicians trained in both conventional oncology and evidence-based complementary medicine. They're increasingly available at major cancer centers and can coordinate holistic care alongside standard treatment.
How to stay in remission from cancer?
Sustained remission is supported by ongoing lifestyle vigilance—anti-inflammatory nutrition, regular physical activity, stress management, adequate sleep, and continued monitoring. A structured nutritional oncology program can help patients build and sustain these habits over time.


