
Introduction
Cancer-related fatigue (CRF) stands as one of the most debilitating and underaddressed side effects of cancer and its treatment. Affecting not just physical energy but mental clarity, emotional well-being, and quality of life, CRF touches up to 80% of patients during chemotherapy and radiotherapy. Yet despite its overwhelming prevalence, there's a sharp disconnect: self-reported severe fatigue is documented 20 times more often by patients than by physicians (23.6% vs. 1.6%), leaving many suffering in silence.
Unlike ordinary tiredness that resolves with a good night's sleep, CRF is persistent, disproportionate to activity levels, and deeply resistant to rest alone. The heaviness in your limbs, the brain fog, the emotional exhaustion that makes a single day feel insurmountable: these are signals of biological disruption at the cellular level.
This guide offers a different path forward. A multi-domain holistic approach can meaningfully reduce fatigue and restore energy where pharmaceuticals alone fall short.
We'll cover evidence-based strategies across nutrition, gentle movement, sleep optimization, mind-body practices, and targeted natural supplements. You'll also find practical frameworks like the 5 P's of energy management, along with how structured nutritional support—including NORI's research-based protocol combining cycled methionine restriction with proprietary nutraceuticals—can address the metabolic vulnerabilities that drive depletion.
TLDR:
- Cancer-related fatigue affects 80% of patients and persists for months to years post-treatment
- Protein intake below 1.0 g/kg/day doubles fatigue risk during chemotherapy
- Exercise reduces fatigue moderately (SMD -0.5); mindfulness-based stress reduction carries a Category 1 recommendation
- American ginseng (2,000 mg/day) shows significant CRF improvement in clinical trials
- The 5 P's (Pacing, Planning, Prioritizing, Positioning, Problem-Solving) help conserve and strategically deploy energy
What Is Cancer-Related Fatigue and Why Does It Happen?
Defining CRF: More Than Just Tiredness
Cancer-related fatigue is a distressing, persistent sense of physical, emotional, and cognitive tiredness related to cancer or its treatment that is not proportional to recent activity and interferes with usual functioning. It can strike before diagnosis, intensify during treatment, and linger for months or years after treatment ends.
What CRF feels like from the patient's perspective:
- Physical heaviness making simple tasks feel impossible
- Mental fog and difficulty concentrating
- Emotional exhaustion and feeling depleted even after eight hours of sleep
- Complete lack of energy despite minimal exertion
According to an NCCN clinical practice guideline analysis of 1,569 patients, 80% of cancer patients experience fatigue during chemotherapy and/or radiotherapy. Chemotherapy induces approximately 1.5 times higher prevalence of severe CRF (33.1%) than radiotherapy (24.2%) or surgery (22.0%).
The Long-Term Burden
CRF frequently persists long after the final treatment. Approximately 30% of patients report persistent fatigue one year post-treatment, per a 2022 review in European Journal of Cancer, while 34% of breast cancer survivors report significant fatigue 5–10 years post-diagnosis, according to a 2025 study in British Journal of Cancer.
Biological Mechanisms Behind CRF
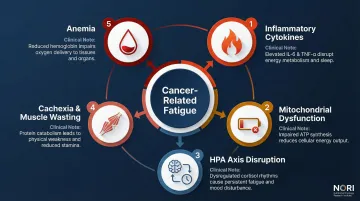
| Mechanism | Clinical Impact |
|---|---|
| Inflammatory Cytokines | Elevated IL-6, TNF-alpha, and CRP create systemic inflammation that drives exhaustion before, during, and after treatment |
| Mitochondrial Dysfunction | Impaired ATP generation at the cellular level reduces energy production |
| HPA Axis Disruption | Hypothalamic-pituitary-adrenal axis dysregulation creates neuroendocrine imbalances |
| Cachexia & Muscle Wasting | Breakdown of muscle mass decreases functional capacity and cannot be reversed by conventional nutrition alone |
| Anemia | Reduced oxygen transport from treatment-induced blood cell depletion exacerbates exhaustion |
Each of these mechanisms is measurable — not subjective. The link between severe fatigue and mitochondrial respiratory dysfunction confirms that what patients describe as bone-deep exhaustion has a cellular basis, which also explains why rest alone rarely resolves it.
Why CRF Remains Undertreated
Many clinicians and patients accept fatigue as an inevitable side effect rather than a treatable condition. Pharmaceutical approaches — psychostimulants and antidepressants — have shown limited effectiveness in clinical trials. That leaves most patients without a meaningful management plan, which is precisely where nutrition-based and integrative strategies have begun to show measurable results.
Nutritional Strategies to Combat Cancer Fatigue
The Foundational Connection Between Nutrition and Energy
At the cellular level, cancer and its treatment deplete critical micronutrients, disrupt metabolism, and increase oxidative stress—all worsening fatigue. Malnutrition affects 30% to 87% of cancer patients, with the highest prevalence in upper gastrointestinal (28.1%) and lower gastrointestinal cancers (20.3%).
Most critically, low protein intake (<1 g/kg body weight) is associated with more than a twofold higher risk of cancer-related fatigue and increased six-month mortality in patients undergoing chemotherapy. This finding emerged as the strongest predictor of CRF—even more than nausea, insomnia, or age.
Eating Patterns and Macronutrients
Practical strategies to sustain energy:
- Small, frequent protein-rich meals (aim for 1.0-1.2 g/kg body weight daily minimum)
- Anti-inflammatory foods: leafy greens, berries, omega-3-rich fish, healthy fats
- Whole grains for steady glucose release
- Adequate hydration throughout the day
- Calorie-dense additions when appetite is poor: nut butters, avocado, olive oil
Addressing treatment barriers:
- Nausea and taste changes: Try cold or room-temperature foods, bland options as needed
- Mouth sores: Soft, smooth textures; avoid acidic or spicy foods
- Low appetite: Focus on nutrient density rather than volume
Anti-inflammatory dietary interventions:
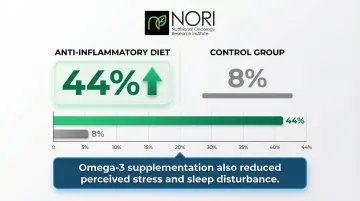
A pilot RCT in breast cancer survivors following a "Fatigue Reduction Diet" showed fatigue improved by 44% compared to just 8% in the control group. Similarly, omega-3 supplementation (2,040 mg/week) significantly decreased fatigue, perceived stress, and sleep disturbance in breast cancer survivors.
The Role of Targeted Nutritional Support
Beyond general dietary advice, a structured nutritional approach that addresses the specific metabolic vulnerabilities of cancer cells can support both energy levels and recovery. NORI's nutritional support program takes this further, combining cycled methionine restriction with proprietary nutraceuticals designed to address the metabolic factors that drive cancer-related energy loss.
The protocol is fully home-based, with personalized nutrition plans and ongoing support through phone and Zoom consultations — accessible to patients worldwide. NORI formulates and manufactures all nutraceuticals at its own facility, which allows direct control over potency and purity standards.
The program integrates diet, nutraceuticals, stress reduction, and anti-inflammatory strategies into a single coordinated plan — one designed to preserve energy while targeting the metabolic conditions that cancer cells depend on.
Movement, Sleep, and Daily Rhythm
The Exercise Paradox
Though counterintuitive when exhausted, gentle, consistent physical activity is one of the best-evidenced strategies for reducing CRF. Meta-analyses report exercise provides a moderate reduction in fatigue with a standardized mean difference of -0.52, and ASCO-SIO guidelines strongly recommend aerobic, resistance, or combined exercise to reduce fatigue severity.
Recommended modalities:
- Walking (even 10-15 minutes daily)
- Restorative yoga
- Tai chi
- Light stretching
Critical caveat: Exercise must be tailored to your baseline fitness, current treatment, and safety considerations (bone metastases, thrombocytopenia, anemia, fall risk). Always consult your care team before starting.
Sleep Quality Over Quantity
A meta-analysis of 160 studies (46,279 patients) found 60.7% of cancer patients experience sleep disturbance, linked to decreased cognitive functioning, poor healing, and reduced quality of life.
Evidence-based sleep hygiene strategies:
- Consistent sleep and wake times (even on weekends)
- Dark, cool bedroom environment
- Limit caffeine after midday
- Reduce screen time 1-2 hours before bed
- Pre-sleep relaxation routines (gentle stretching, reading, meditation)
Energy Pacing: Working With Your Body
Energy pacing means matching your activity load to your actual capacity — not pushing through until you crash. Done consistently, it preserves functional ability without worsening deconditioning.
Core pacing strategies:
- Schedule demanding tasks during your peak energy window (often mid-morning)
- Take short rest breaks before exhaustion sets in, not after
- Alternate physically and mentally demanding tasks throughout the day
Circadian Rhythm Support
Cancer treatment disrupts the body's internal clock. Actigraphy studies show 30% to 95% of advanced cancer patients have disrupted circadian rhythms, with those maintaining better day-night activity patterns experiencing improved quality of life and less fatigue.
Support strategies:
- Gentle morning light exposure (15-30 minutes outside or near a window)
- Consistent meal timing
- Structured daily routines
Mind-Body Practices and Emotional Resilience
The Stress-Fatigue Connection
Chronic psychological stress elevates inflammatory markers (cortisol, cytokines) that worsen CRF. The average correlation of fatigue with depression is 0.56, and with anxiety is 0.46, demonstrating the bidirectional link between emotional and physical exhaustion.
Mindfulness-Based Stress Reduction (MBSR) holds a strong Category 1 recommendation from ASCO-SIO guidelines and is also cited in NCCN guidelines as an evidence-based approach for cancer fatigue.
Daily practice typically includes:
- 5-15 minutes of breath-focused meditation
- Body scan exercises
- Guided imagery
- Simply sitting quietly and observing thoughts without judgment
Additional Mind-Body Modalities
MBSR is a strong starting point, but several complementary practices can further reduce the stress response and ease fatigue:
- Deep breathing exercises (4-7-8 technique, box breathing)
- Progressive muscle relaxation
- Journaling for emotional processing
- Time in nature
- Expressive arts, yoga, and acupuncture (recognized in integrative oncology guidelines)
The Power of Connection
Individual practices address the internal stress response, but the social environment matters just as much. Isolation amplifies fatigue — studies show an inverse relationship between perceived social support and physical fatigue, meaning more connection directly reduces exhaustion.
Ways to connect:
- Cancer support groups (in-person or online)
- Leaning on family and caregivers
- Professional counseling
- NORI offers free weekly Zoom workshops every Saturday and Wednesday for community support and education
Evidence-Based Natural Supplements and Botanicals
American Ginseng: The Gold Standard
American ginseng (Panax quinquefolius) is the most clinically validated natural supplement for CRF. A multisite, double-blind Phase III RCT (N=364) evaluated American ginseng versus placebo for eight weeks in fatigued cancer survivors. At eight weeks, there was statistically significant improvement in fatigue for the ginseng group (change score 20) versus placebo (10.3) (P=.003), with greater benefit in patients actively receiving cancer care.
Evidence-based dosing:
- 2,000 mg/day (1,000 mg twice daily)
- Products must contain at least 3% ginsenosides
- Duration: Eight weeks minimum for full effect
Important safety considerations:
- May antagonize warfarin, lowering INR and increasing bleeding risk—patients on blood thinners must monitor INR closely
- May reduce blood glucose—caution for diabetics
- Species matters: Panax quinquefolius (American) has evidence; Panax ginseng (Asian/Korean) did not show effectiveness in trials

Other Adaptogenic and Anti-Inflammatory Agents
American ginseng has the strongest evidence, but other botanicals show early-stage promise:
- Ashwagandha (Withania somnifera): A small open-label trial suggested potential against CRF, but larger randomized trials are needed
- Rhodiola rosea: Popular for general wellness, but high-quality Phase III oncology RCTs are lacking
- Anti-inflammatory botanicals: Boswellia serrata, ginger extract, and grapeseed extract have mechanisms that may support energy through inflammation reduction
Critical guidance: Always consult your oncology team before adding any supplement due to potential drug-herb interactions.
The Quality and Purity Challenge
Because ginseng product quality varies widely across brands, sourcing matters as much as dosage. The FDA regulates dietary supplements as foods, not drugs — manufacturers don't need FDA approval before marketing, which makes third-party verification essential.
Look for products certified by one of these independent testing organizations:
- USP Dietary Supplement Verification — confirms identity, potency, and purity
- NSF International — screens for contaminants and label accuracy
- ConsumerLab — independently tests commercial supplements for quality
NORI formulates and manufactures its own nutraceuticals in-house, which allows direct control over ingredient sourcing, ginsenoside concentration, and batch-level purity — eliminating the guesswork that comes with third-party sourced products.
Managing Energy With the 5 P's Framework
The 5 P's of energy conservation came out of occupational therapy in the 1990s as a practical tool for managing fatigue in chronic illness. Institutions like the NHS and Macmillan Cancer Support have since brought the framework into oncology rehabilitation, where it's now a standard resource for patients navigating treatment-related exhaustion.
The 5 P's Explained
| The "P" | Practical Application |
|---|---|
| Pacing | Break tasks into smaller stages. Take regular breaks and stop to rest before exhaustion hits. Example: Fold laundry in three 10-minute sessions instead of one 30-minute push. |
| Planning | Schedule high-priority tasks during peak energy times. Spread heavy tasks throughout the week. Example: Grocery shopping on Monday, laundry on Wednesday, cooking batch meals on Saturday. |
| Prioritizing | Identify what's essential. Ask: Does this need to be done today? Can someone else do it? Example: Let the bed go unmade on low-energy days; focus on taking medications and eating well. |
| Positioning | Use ergonomic supports to reduce physical effort. Sit instead of standing. Example: Use a shower chair, keep frequently used items at waist height, use a wheeled cart to transport items. |
| Problem-Solving | Give yourself permission to rest and adapt. Review routines when fatigue flares. Example: Pre-cut vegetables when energy is good, use delivery services during treatment weeks, accept help from friends. |
Used consistently, the 5 P's turn energy management into a daily practice rather than a reactive scramble. Patients who build these habits often report retaining more capacity for the activities that support both recovery and quality of life.

Frequently Asked Questions
What is cancer fatigue?
Cancer-related fatigue is a persistent, overwhelming exhaustion caused by cancer itself and its treatments that is not relieved by rest or sleep. Unlike normal tiredness, CRF is disproportionate to activity levels and interferes significantly with daily functioning.
What does cancer fatigue feel like?
Physically, CRF manifests as heaviness and inability to complete basic tasks. Cognitively, it causes difficulty thinking, concentrating, and making decisions (brain fog). Emotionally, it creates a sense of complete depletion even after a full night's sleep.
What can cancer patients do for fatigue?
Key holistic strategies include:
- Optimizing protein intake (>1.0 g/kg/day)
- Engaging in gentle, tailored exercise
- Practicing consistent sleep hygiene
- Managing stress through mindfulness-based approaches
- Considering American ginseng (2,000 mg/day)
- Applying the 5 P's energy pacing framework throughout the day
How to prevent chemo fatigue?
While chemo fatigue can't be fully prevented, starting treatment well-nourished, maintaining low-impact physical activity, managing stress proactively, and working with a nutritional support team can significantly reduce its severity. Structured programs like NORI's protocol offer targeted metabolic support during active treatment.
How long does fatigue last after cancer care?
Post-treatment fatigue duration varies widely. For some, it resolves within weeks; however, research shows approximately 30% of patients experience persistent fatigue one year after treatment, and 34% of breast cancer survivors report significant fatigue 5-10 years post-diagnosis.
What are the 5 P's of fatigue management?
The 5 P's (Pacing, Planning, Prioritizing, Positioning, and Problem-Solving) provide a structured framework to conserve and strategically deploy energy throughout the day. This approach prevents "boom and bust" cycles and preserves capacity for the activities that matter most.
Ready to explore targeted nutritional support for cancer-related fatigue? NORI offers free initial consultations to discuss your specific situation. Contact them at 800-634-3804 or info@nutritionaloncology.net to learn how their home-based nutritional support program, accessible worldwide, might support your energy and recovery journey.


