
Research demonstrates that brain tumors and their treatments—surgery, chemotherapy, and radiation—place extraordinary metabolic demands on the body. Targeted nutrition helps maintain muscle mass, support healing, and reduce inflammation. Emerging science reveals that brain cancer cells metabolize nutrients differently than healthy brain cells, particularly glucose and certain amino acids. This metabolic vulnerability creates an opportunity to use diet as a therapeutic tool alongside standard medical care.
TLDR
- Anti-inflammatory whole foods, lean proteins, healthy fats, and antioxidant-rich vegetables support immune function and treatment tolerance
- Ketogenic, anti-inflammatory, and methionine-restricted dietary approaches disrupt tumor metabolism by exploiting cancer cells' dependence on glucose and specific amino acids
- Refined sugars, processed foods, and high-sodium items promote inflammation and elevate blood glucose levels that cancer cells preferentially consume — cut them first
- Nutritional needs shift throughout treatment phases—adjusting intake at each stage reduces side effects and maintains strength
- Working with a nutritional oncology specialist helps tailor dietary protocols — such as cycled methionine restriction — to your specific cancer type and treatment stage
Why Nutrition Matters for Brain Cancer Patients
Brain tumors and their treatments create significant metabolic demands that increase the need for strategic nutrition. Malnutrition affects 17.6% of brain tumor patients and is associated with increased postoperative complications, infections, delayed wound healing, and reduced overall survival. Despite brain cancer patients showing lower malnutrition rates than other cancer types, the impact on outcomes is profound—making proactive nutritional planning essential from diagnosis onward.
Tumor Metabolism Creates Therapeutic Opportunities
Brain cancer cells undergo metabolic reprogramming that differs dramatically from healthy brain tissue. Glioblastoma cells rely heavily on aerobic glycolysis (the Warburg effect), consuming glucose at accelerated rates even when oxygen is present. This metabolic shift generates rapid energy for tumor cells while supplying precursors that promote invasiveness and therapy resistance.
That glucose dependency is just one exploitable weakness. Glioblastoma also shows the highest expression of cysteine and methionine pathway genes among 32 human cancers — meaning tumor cells scavenge these sulfur-containing amino acids from the bloodstream rather than producing them internally.
Two key metabolic vulnerabilities emerge from this research:
- Glucose dependence: Tumor cells prioritize aerobic glycolysis, making carbohydrate intake a lever worth managing
- Amino acid scavenging: Glioblastoma's reliance on dietary cysteine and methionine creates a targeted restriction opportunity
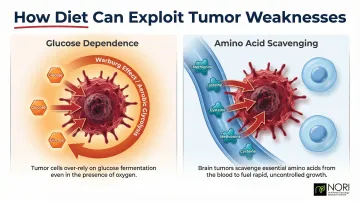
These vulnerabilities give nutrition a functional role in cancer care — one that works alongside medical treatment to reduce the resources available to tumor cells.
The Best Foods to Eat for Brain Cancer Patients
Prioritize whole, nutrient-dense foods that reduce inflammation, support cellular repair, and provide steady energy without feeding tumor growth. This foundational principle guides every dietary choice throughout your treatment journey.
Lean Proteins for Tissue Repair and Immune Support
Adequate protein is essential during brain cancer treatment to preserve muscle mass, support immune cell production, and aid tissue recovery. Cancer patients should consume 1.0 to 1.5 grams of protein per kilogram of body weight daily to maintain strength during treatment.
Best protein sources include:
- Wild-caught fish (salmon, mackerel, sardines)
- Pasture-raised eggs
- Legumes (lentils, chickpeas, black beans)
- Organic poultry
- Tofu and tempeh
Plant-based proteins offer an additional advantage: Plant-based proteins carry a notable advantage — they naturally contain lower levels of methionine, an amino acid that brain tumor cells depend on for growth. Pairing plant proteins with moderate animal protein meets your daily needs while limiting the nutrients that may support tumor metabolism.
Healthy Fats for Brain Health and Anti-Inflammation
Omega-3 fatty acids reduce neuroinflammation and support brain cell integrity — important for brain cancer patients. Research demonstrates that EPA and DHA can enhance the efficacy of temozolomide chemotherapy by increasing reactive oxygen species formation and apoptosis in glioblastoma cells.
Incorporate these healthy fat sources:
- Fatty fish (salmon, mackerel, herring) 2-3 times weekly
- Flaxseeds and chia seeds
- Walnuts
- Algae-based omega-3 supplements
- Extra virgin olive oil
- Avocados
Oleocanthal and related compounds in extra virgin olive oil significantly inhibit inflammatory pathways that drive glioblastoma progression — use it as your default cooking oil and for salad dressings.
Antioxidant-Rich Vegetables and Fruits
Dark, colorful vegetables and fruits combat oxidative stress while supporting immune function. Cruciferous vegetables contain sulforaphane, which rapidly crosses the blood-brain barrier and suppresses glioblastoma cell growth by inducing cell cycle arrest and apoptosis.
Prioritize these antioxidant powerhouses:
- Cruciferous vegetables: broccoli, cauliflower, Brussels sprouts, kale
- Dark leafy greens: spinach, Swiss chard, collard greens
- Deeply colored berries: blueberries, blackberries, strawberries
- Orange vegetables: sweet potatoes, carrots, butternut squash

Light steaming rather than boiling preserves the sulforaphane content in cruciferous vegetables — a simple prep habit that protects the compounds you're eating for.
Vitamins and Minerals That Support Recovery
Whole foods lay the foundation, but specific micronutrients are harder to obtain in therapeutic amounts from diet alone. These nutrients play direct roles in immune regulation, oxidative defense, and neurological function during treatment.
Key micronutrients:
- Vitamin D: Supports immune function; found in fatty fish, fortified foods, and sunlight exposure
- Selenium: Essential for antioxidant defense; sources include Brazil nuts (1-2 daily), seafood, and whole grains
- Zinc: Critical for immune cell production; found in pumpkin seeds, chickpeas, and oysters
- Magnesium: Supports neurological function; abundant in dark leafy greens, nuts, and whole grains
Many brain cancer patients develop deficiencies during treatment. Consider working with your healthcare team to monitor levels and supplement appropriately.
Hydration and Whole Grains
Adequate hydration supports every bodily function, from nutrient transport to toxin elimination. Aim for at least eight 8-ounce glasses of water daily, adjusting for treatment side effects and activity level.
Alongside hydration, complex carbohydrates provide sustained energy without the blood sugar spikes that may fuel tumor cell metabolism. Reach for:
- Steel-cut oats
- Quinoa
- Brown rice
- Sweet potatoes
- Barley
These whole grains digest slowly, providing steady glucose release rather than the rapid spikes associated with refined carbohydrates.
Dietary Strategies That May Help Slow Tumor Growth
Beyond general healthy eating, specific dietary approaches target the metabolic pathways brain tumors depend upon. This represents an evolving but promising area of nutritional oncology.
The Ketogenic Diet
The high-fat, very low-carbohydrate ketogenic diet deprives cancer cells of their primary fuel source (glucose) while providing ketone bodies as alternative energy that healthy brain cells use more efficiently than tumor cells.
A 2025 phase 1 trial demonstrated that glioblastoma patients maintained nutritional ketosis while on standard treatment, with a median overall survival of 29.4 months—notably higher than historical averages. However, earlier studies like the ERGO trial showed the diet was safe but demonstrated no significant clinical activity as a single agent.
Important considerations:
- Requires medical supervision and registered dietitian support
- May cause insufficient energy intake and weight loss if not properly managed
- Not suitable for all patients
- Should never replace standard medical treatment
The ketogenic diet remains investigational for brain cancer. If you're considering this approach, discuss it thoroughly with your oncology team before making changes.
Anti-Inflammatory Diet
Chronic inflammation drives tumor progression and worsens treatment side effects. Tumor-associated macrophages release pro-inflammatory cytokines like IL-6 that promote glioblastoma growth, invasion, and immunosuppression.
An anti-inflammatory dietary approach emphasizes protective foods while cutting the ones that feed inflammation:
- Include: omega-3-rich fish, flaxseeds, walnuts, turmeric, ginger, berries, dark leafy greens, extra virgin olive oil, and green tea
- Limit or avoid: processed foods, refined sugars, trans fats, and excessive omega-6 oils
A matched case-control study found that adhering to the Mediterranean diet—a classic anti-inflammatory pattern—was associated with significantly reduced glioma risk. While this research examined prevention rather than treatment, the same anti-inflammatory principles support patients throughout their cancer journey.

Methionine Restriction: A Targeted Nutritional Strategy
Unlike the broader approaches above, methionine restriction targets a specific metabolic weakness in tumor cells. Brain tumor cells scavenge the amino acid methionine from the blood rather than synthesizing it internally — a dependency that creates a direct opportunity for dietary intervention.
Research published in Nature Communications demonstrated that dietary cysteine and methionine restriction sensitizes glioma cells to cellular health pathways being investigated in nutritional oncology research (including iron-dependent lipid peroxidation). In mouse models, this dietary approach doubled survival time when combined with targeted therapies.
The science is compelling: PNAS research showed that glioblastoma's unique susceptibility to cysteine creates toxic accumulation of hydrogen peroxide, particularly when glucose is limited. This metabolic weakness exists specifically in tumor cells, with healthy tissue showing far less vulnerability.
NORI's Cycled Methionine Restriction Protocol
The Nutritional Oncology Research Institute (NORI) has applied methionine restriction research in clinical practice for over 20 years. The NORI Protocol uses cycled dietary methionine and cysteine restriction within a predominantly plant-based framework — reducing animal protein without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research — combined with targeted pro-oxidant nutraceutical combinations being studied in nutritional oncology research. Because cancer cells are known to have elevated oxidative stress, these pro-oxidant agents are being investigated for how they may interact with these cellular conditions, affecting cellular health pathways, as investigated in nutritional oncology research, with ongoing research into their selective effects on different cell types. Natural pro-oxidant agents used in this approach include high-dose Vitamin C, piperlongumine, menadione, and certain carotenoids, which are being explored alongside conventional care in ongoing research.
Protocols are individualized and delivered through NORI's home-based program, which includes continuous guidance and support — no clinic visits required.
For detailed information about methionine restriction protocols specific to your situation, contact NORI at 800-634-3804 or info@nutritionaloncology.net for a complimentary consultation.
Foods and Habits to Avoid with Brain Cancer
What you eliminate from your diet matters as much as what you include. Certain foods and habits directly fuel tumor metabolism or impair immune function.
Refined Sugars and High-Glycemic Foods
White bread, sugary drinks, candy, and processed snacks spike blood glucose rapidly, directly fueling the glucose-hungry metabolism of tumor cells. This connects directly to the Warburg effect, where cancer cells rely heavily on glycolysis for energy production.
The problem intensifies for brain cancer patients taking dexamethasone for cerebral edema. This commonly prescribed corticosteroid frequently induces hyperglycemia, which is linked to poorer functional recovery, increased infection rates, and reduced overall survival.
Eliminate or strictly limit:
- Sugary beverages and fruit juices
- White bread, pastries, and refined grains
- Candy and desserts
- Processed breakfast cereals
Processed and Ultra-Processed Foods
Packaged snacks, deli meats, fast food, and convenience meals contain pro-inflammatory additives, trans fats, and chemical preservatives that impair immune function. Large-scale meta-analyses link high consumption of ultra-processed foods to increased cancer risk, though research specific to brain tumors remains limited.
These foods are also calorie-dense but nutrient-poor, crowding out whole foods that provide genuine therapeutic benefit. Common sources to cut:
- Packaged chips, crackers, and snack bars
- Deli meats and processed sausages
- Fast food and frozen convenience meals
- Flavored instant noodles and canned pasta
Excessive Sodium
Canned soups, processed foods, and restaurant meals contain excessive sodium that can increase fluid retention—a specific concern for brain tumor patients managing intracranial pressure. While direct evidence linking dietary sodium to intracranial pressure is limited, keeping sodium moderate supports fluid balance and reduces strain on an already compromised system.
High-sodium sources to reduce:
- Canned soups and broths
- Processed deli meats and cheeses
- Restaurant and takeout meals
- Packaged sauces, seasonings, and condiments
Alcohol
The World Health Organization classifies alcohol as a Group 1 carcinogen, noting there is no safe consumption level for cancer risk. The American Cancer Society recommends avoiding alcohol during cancer treatment, as it can irritate mouth sores, interact with medications, and increase harmful side effects.
Alcohol also drives systemic inflammation and suppresses immune function at a time when the body needs every resource focused on recovery.
Practical Nutrition Tips: Before, During, and After Treatment
Nutritional needs shift throughout your treatment journey. Adjusting your approach at each phase helps maintain strength and reduce side effects.
Before Treatment
Use the pre-treatment window to build nutritional reserves. Your body will draw on these reserves during the demanding weeks ahead.
Focus on:
- High-protein meals at each eating occasion
- Calorie-dense healthy fats (nuts, avocados, olive oil)
- Maximum vegetable and fruit intake for micronutrient loading
- Gradual implementation of any dietary changes to avoid shock
Enter treatment as nutritionally strong as possible. A strong nutritional foundation directly shapes how well your body handles surgery, radiation, and chemotherapy — affecting everything from immune response to recovery speed.
During Treatment
Treatment side effects—nausea, appetite loss, taste changes, and fatigue—make eating challenging. Adapt your approach rather than forcing large meals.
Practical strategies:
- Eat small frequent meals (5-6 times daily) rather than three large ones
- Choose easy-to-digest options: smoothies, soups, soft proteins, well-cooked vegetables
- Keep bland foods available for nausea days: oatmeal, rice, bananas, applesauce
- Stay hydrated with herbal teas, electrolyte drinks, and water-rich fruits
- Don't force eating when nauseous—wait for windows when appetite improves
Cold foods often work better than hot foods when dealing with nausea or taste changes. Chilled smoothies, room-temperature soups, and cold proteins like hard-boiled eggs tend to be the most tolerated options.

After Treatment and Recovery
Recovery nutrition focuses on rebuilding. Your body needs resources to repair treatment-related damage and restore normal function.
Emphasize:
- High-protein foods for tissue repair (target 1.5–2.0 g per kg of body weight daily)
- Anti-inflammatory foods to reduce post-treatment inflammation
- Gradual reintroduction of full vegetable and whole grain variety as digestive tolerance improves
- Probiotic-rich foods if you experienced digestive disruption
Recovery unfolds over months, not weeks. Consistent daily nutrition — even when appetite is low — gives your body the raw materials it needs to rebuild tissue, restore gut health, and regain strength.
Frequently Asked Questions
What stops a brain tumor from growing?
Controlling brain tumor growth typically requires medical treatments like surgery, radiation, and chemotherapy combined with immune system support. Emerging evidence suggests dietary strategies — particularly glucose restriction and methionine restriction — may also slow progression by targeting metabolic vulnerabilities that cancer cells rely on but healthy cells do not.
What not to eat with a brain tumor?
Avoid refined sugars and high-glycemic foods that spike blood glucose and fuel tumor metabolism. Eliminate trans fats and ultra-processed foods that promote inflammation. Limit excessive sodium, which can worsen fluid retention. Avoid alcohol entirely, as it increases cancer risk and interferes with treatment effectiveness.
Is the ketogenic diet safe for brain cancer patients?
The ketogenic diet shows early promise but must be undertaken with medical supervision. Risks include nutrient deficiencies, inadequate calorie intake, and unintended weight loss — making it unsuitable for all patients. Close monitoring by a registered dietitian is essential.
Can what I eat actually affect brain cancer treatment outcomes?
Emerging research suggests diet can influence treatment outcomes — amino acid restriction has improved treatment responses in preclinical models, and good nutrition supports better treatment tolerance and faster recovery. Diet alone cannot cure brain cancer, but strategic nutrition creates conditions that help medical treatments work more effectively.
What nutrients are most important for brain cancer patients?
Key nutrients include omega-3 fatty acids for brain health and inflammation control, antioxidant vitamins (C, E, D) to reduce oxidative stress, selenium and zinc for immune function, and quality protein to maintain muscle mass during treatment. Prioritizing these supports both treatment tolerance and recovery.
How does methionine restriction work against brain tumors?
Brain tumor cells cannot synthesize methionine internally and must obtain it from the bloodstream. A low-methionine diet starves tumor cells of this essential amino acid, being investigated for its interaction with cellular health pathways. Research shows this approach doubled survival time in mouse models while leaving healthy cells largely unaffected, as normal cells can synthesize methionine when dietary intake is low.


