
Introduction
From the moment of diagnosis, cancer patients face a cascade of treatment decisions: surgery, chemotherapy, radiation, immunotherapy. Yet one of the most modifiable factors influencing outcomes rarely gets dedicated attention in a standard oncology appointment — nutrition.
Research shows that 59.1% of cancer patients are already at risk of malnutrition or overtly malnourished at diagnosis. That figure matters because malnutrition directly worsens treatment tolerance, increases complication rates, and reduces survival.
Most patients are told to "eat well" — but for someone with cancer, that advice is far too thin. Cancer fundamentally alters cellular biology, creating hypermetabolic states in roughly 50% of weight-losing patients and creating metabolic vulnerabilities that standard dietary guidance simply cannot address.
Treatment side effects compound the problem further, impairing absorption and appetite at the very moment the body needs the most support.
What follows breaks down the concrete, outcome-driven case for nutrition consultations in cancer care — and what's at stake when that care is missing.
TL;DR
- Nutrition consultations deliver personalized dietary strategies based on individual metabolic needs, treatment phase, and cancer-specific vulnerabilities—not generic guidelines
- Combined nutritional counseling and supplementation cut severe chemotherapy toxicity by 30.4% in malnourished advanced cancer patients
- Skipping nutrition consultation risks malnutrition—which nearly doubles mortality (HR 1.92) and drives 10–20% of all cancer deaths
- Consultations work best when ongoing and integrated into broader care—not treated as a one-time event
- NORI provides free initial consultations with unlimited ongoing support, making specialized nutritional oncology programs accessible worldwide
What Is a Nutrition Consultation?
A nutrition consultation is a structured, one-on-one session with a qualified nutrition professional who assesses an individual's current dietary intake, health status, and specific medical conditions to develop a personalized nutrition plan. This differs from generic dietary advice found online or in patient education pamphlets—it involves comprehensive clinical assessment using validated tools.
In oncology settings, nutrition consultations serve a specific clinical purpose: identifying malnutrition risk, optimizing nutrient intake around treatment phases, managing side effects like nausea and taste changes, and supporting the body's resilience during and after cancer care.
According to guidelines from ESPEN and ASCO, a comprehensive assessment must evaluate:
- Nutritional intake and recent weight change
- Body mass index and muscle mass
- Nutrition impact symptoms
- Physical performance
- Systemic inflammation markers
A nutrition consultation translates nutritional science into actionable, individualized steps that support and strengthen a patient's existing care plan. For cancer patients, that precision matters: the metabolic demands, treatment toxicities, and nutritional vulnerabilities they face differ substantially from those of healthy adults.
Key Advantages of Nutrition Consultations for Cancer Patients
The advantages below focus on measurable outcomes that matter to cancer patients and their care teams: nutritional status, treatment tolerance, clinical outcomes, and sustained quality of life. Each advantage is tied to outcomes supported by clinical evidence.
Personalized Assessment That Addresses the Patient, Not the Diagnosis
A nutrition consultation begins with a comprehensive assessment—including dietary habits, body composition, metabolic needs, treatment history, food preferences, and any restrictions—creating a patient-specific picture that generic dietary guidelines cannot replicate.
This individualized approach allows the nutrition professional to identify deficiencies or imbalances that may otherwise go unrecognized, and to prescribe specific dietary modifications matched to the patient's current condition and treatment phase. These modifications include:
- Protein and energy intake targets based on actual metabolic needs
- Food timing strategies around treatment schedules
- Supplement use recommendations for specific deficiencies
- Dietary adjustments for treatment-related side effects
For cancer-focused programs like NORI, this process begins with a free initial consultation designed to evaluate the patient's full picture before any protocol is recommended, ensuring that nutritional interventions address individual vulnerabilities rather than applying one-size-fits-all approaches.
Cancer profoundly alters metabolism in ways that make individualized plans clinically necessary, not optional. Approximately 50% of cancer patients losing weight are hypermetabolic, with resting energy expenditure exceeding 110% of predicted values due to systemic inflammation.
Impaired absorption compounds this further. Pancreatic exocrine insufficiency affects 90–100% of patients with locally advanced or metastatic pancreatic cancer, requiring enzyme replacement therapy to restore basic nutrient uptake.
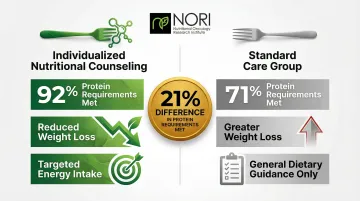
Research in cancer patients undergoing treatment has shown that individualized nutritional counseling significantly reduced weight loss and improved fulfillment of energy and protein requirements compared to standard care—with 92% versus 71% of protein requirements met in the counseled group.
KPIs impacted:
- Body weight and lean mass retention
- Daily energy and protein intake adequacy
- Nutritional risk score
- Treatment adherence
When this advantage matters most:
This personalized approach is especially critical for patients undergoing active treatment (chemotherapy, radiation), those with gastrointestinal cancers or head and neck cancers where food intake is directly disrupted, and patients transitioning from hospital to home care. The highest burden of malnutrition at diagnosis is observed in pancreatic (74.2%), esophageal (72.8%), and gastric (65.3%) cancers.
Improved Treatment Tolerance and Clinical Outcomes
Malnutrition in cancer patients is not a side effect to simply accept—it is a modifiable risk factor that directly impairs treatment tolerance, increases complication rates, and reduces overall survival. Nutrition consultation intervenes in this cycle by ensuring the body has the nutritional resources needed to withstand and respond to treatment.
Regular nutrition consultation supports treatment effectiveness through multiple mechanisms:
- Maintaining lean muscle mass reduces fatigue and functional decline
- Adequate protein intake supports immune function and wound healing
- Specific dietary strategies can reduce inflammation and support cellular repair
- Optimized nutritional status allows patients to complete treatment regimens without dose reductions or delays
Severe malnutrition nearly doubles the risk of overall mortality (HR 1.92) and accounts for an estimated 10% to 20% of all cancer-related deaths, independent of the tumor's progression. Malnutrition is also significantly associated with increased risk of postoperative complications (OR 1.90), longer hospital stays, and higher 30-day readmission rates.
The case for intervention is well-documented. Malnourished patients provided with oral nutritional supplements had 38.8% fewer 30-day readmissions, with oncology patients specifically showing a 46.1% reduction31864-1/fulltext). A comprehensive nutrition-focused quality improvement program reduced 30-day readmissions by 27% and shortened length of stay by 25%, resulting in net savings of $3,858 per patient.
An RCT in malnourished advanced cancer patients found that nutritional counseling plus whey protein isolate supplementation (20g/day) reduced the risk of severe (grade ≥3) chemotherapy toxicity by 30.4% while improving phase angle, fat-free mass index, and muscle strength.

KPIs impacted:
- Treatment completion rates
- Hospital readmission rates
- Length of stay
- Complication rates
- Immune function markers
Long-Term Quality of Life and Disease Management
Nutrition consultation's value extends well beyond the active treatment phase. For cancer survivors, the dietary patterns established and maintained post-treatment directly influence recurrence risk, energy levels, immune resilience, and overall quality of life.
Ongoing nutritional guidance helps patients:
- Navigate conflicting dietary information with evidence-based clarity
- Maintain healthy weight and body composition after treatment
- Manage long-term side effects like digestive issues and fatigue
- Build sustainable habits that support long-term disease management
Organizations like NORI offer ongoing, unlimited support as part of their home-based nutritional programs, recognizing that sustained guidance—not a one-time plan—is what drives lasting outcomes. The evidence supports this long-term focus: high adherence to healthy post-treatment dietary patterns reduces overall mortality by 20–22% among cancer survivors. Adherence to the Mediterranean diet is associated with a significant reduction in cancer recurrence (pooled HR 0.83).
An RCT in colorectal cancer patients undergoing radiotherapy demonstrated that early, individualized nutritional counseling improved all quality of life function scores, with this efficacy persisting for 3 months post-intervention. Patients receiving no counseling saw quality of life deteriorate during the same period.
KPIs impacted:
- Quality of life scores
- Body composition maintenance post-treatment
- Dietary adherence rates
- Disease recurrence markers where available
What Happens When Nutrition Is Overlooked in Cancer Care
Nutrition is one of the most frequently undertreated aspects of oncology care. A 2019 national survey revealed that 46.9% of US outpatient cancer centers do not consistently screen for malnutrition, and 76.8% do not bill for nutrition services. The registered dietitian-to-patient ratio stands at a staggering 1:2,308.
Many patients receive no formal nutritional guidance, leaving them to manage dietary decisions amid complex symptoms, treatment side effects, and conflicting information. The clinical consequences are severe:
- Malnutrition accelerates undetected. Without systematic screening, muscle wasting (cachexia) progresses, immune function weakens, and treatment toxicity rises. In one large cohort of malnourished inpatients, only 3.1% received oral nutritional supplements.
- Patients make harmful dietary choices. Without personalized guidance, many eliminate entire food groups based on internet advice — cutting essential nutrients precisely when metabolic demand is highest.
- Clinical outcomes decline measurably. Malnourished colorectal cancer patients stay an average of 3.41 days longer in hospital, face higher readmission rates, and are less able to tolerate or complete treatment regimens.

The problem compounds: poor nutrition makes treatment harder to tolerate, which reduces treatment efficacy, which worsens the patient's overall prognosis—a cycle that early nutrition intervention can break before it takes hold.
How to Get the Most Value from Your Nutrition Consultation
Nutrition consultation delivers its greatest impact when treated as an ongoing process rather than a single appointment. Patients who attend multiple sessions, track their dietary intake between visits, and regularly review progress with their nutrition professional see steady improvements in how they feel, eat, and respond to treatment.
Come prepared to maximize each session:
- Bring a record of current medications and supplements
- Gather recent lab work (complete blood count, comprehensive metabolic panel, albumin, prealbumin)
- Keep a rough food diary for 3-5 days before your consultation
- Be transparent about taste changes, appetite loss, or dietary restrictions related to treatment
The more complete the picture, the more targeted the plan. Don't minimize symptoms or challenges—your nutrition professional needs accurate information to create a plan that actually works.
For patients who cannot access in-person consultations due to location, mobility, or cost, home-based programs with continuous remote support can provide equivalent value. What drives results is consistent engagement — not how you show up to a session. NORI offers phone and Zoom consultations worldwide, removing geographic barriers to specialized nutritional care.
Between consultations, track weight, food intake, symptoms, and energy levels. This gives your nutrition professional the real-time feedback needed to refine your plan as you progress.
Conclusion
The value of nutrition consultations for cancer patients is not theoretical—it is measurable in nutritional status, treatment tolerance, clinical outcomes, and quality of life. The evidence shows consistent results across these areas:
- Reduces malnutrition risk during active treatment
- Improves treatment completion rates
- Decreases hospital readmissions
- Supports long-term disease management
This value compounds when nutrition consultation is applied consistently and updated as the patient's condition evolves. Nutrition works best as an active, ongoing component of cancer care — not a reactive measure added late in the process.
Starting qualified, individualized nutritional guidance early in the treatment journey is among the most impactful steps a cancer patient can take for recovery and long-term health.
Organizations like NORI provide specialized nutritional oncology support through home-based programs that include free initial consultations and continuous care, making evidence-based nutritional guidance accessible to cancer patients worldwide. If you're exploring your options, a free initial consultation is a practical first step.
Frequently Asked Questions
What is a dietary consult?
A dietary consult is a structured meeting with a qualified nutrition professional who evaluates a patient's dietary intake, health status, and medical conditions to develop a personalized nutrition plan. Unlike generic nutrition advice, it incorporates clinical assessment and interventions tailored to specific medical needs.
What are the 5 main Dietary Guidelines?
For cancer patients, standard dietary guidelines—emphasizing vegetables, fruits, whole grains, lean proteins, and limited added sugars—are a starting point, not a destination. Cancer patients typically require targeted modifications that account for altered metabolism, treatment side effects, and specific nutritional vulnerabilities that general population guidelines don't address.
How does nutrition affect cancer treatment outcomes?
Adequate nutrition maintains lean mass, supports immune function, and reduces treatment toxicity. Malnourished cancer patients consistently show higher complication rates, longer hospital stays, and lower treatment completion rates compared to those who are nutritionally supported. Research demonstrates that individualized nutritional interventions can reduce severe chemotherapy toxicity by over 30% while improving body composition and functional status.
What happens during a nutrition consultation for cancer patients?
The consultation covers current dietary intake, body composition, treatment history, and side effects — then produces a personalized nutrition plan with specific energy, protein, and supplement targets. Guidance on managing symptoms like nausea, taste changes, and appetite loss through diet is typically included as well.
Can dietary changes alone help support cancer recovery?
Targeted nutritional interventions — such as methionine restriction, which exploits specific cancer cell vulnerabilities — can meaningfully support recovery when applied consistently alongside medical care. Nutritional therapy works best as a complement to your oncology team's treatment plan, not a substitute for it.
How is a cancer-focused nutrition consultation different from general dietary advice?
Cancer-focused consultations go well beyond general dietary advice by addressing metabolic changes, cachexia risk, treatment-induced appetite loss, and nutraceutical strategies that standard nutrition guidance doesn't cover. Assessments use oncology-specific screening tools and build interventions around cancer type, stage, and treatment phase.


