
Introduction
Ovarian cancer remains one of the most challenging gynecologic malignancies, with approximately 20,890 new cases and 12,730 deaths estimated in the United States in 2025. Most diagnoses occur at advanced stages, when symptoms finally become noticeable — contributing to a five-year survival rate of roughly 50% across all stages. By contrast, patients diagnosed at localized stages have a 91.7% five-year survival rate, which speaks to how much early detection and comprehensive care matter.
Nutrition has become a growing focus in oncology — and for good reason. Dietary choices don't replace medical treatment, but evidence shows they can meaningfully support immune function, help maintain a healthy weight, reduce treatment side effects, and potentially influence long-term survival. Research from the Ovarian Cancer Association Consortium found that adherence to high-quality diets reduces mortality risk by up to 34% in early-stage patients.
This guide covers the best foods to eat during treatment, what to limit, strategies for managing common side effects through diet, and emerging nutritional approaches that may support recovery and long-term health.
TLDR
- Plant-forward diets—vegetables, fruits, whole grains, legumes, lean protein—are best supported by research for ovarian cancer patients
- Processed meats, high saturated fat foods, added sugars, and excess alcohol have been linked to poorer outcomes and should be minimized
- Nutrition needs differ dramatically based on treatment phase—active chemotherapy requires different strategies than post-surgery recovery or survivorship
- Specific dietary adjustments—addressing nausea, appetite loss, and constipation—help patients stay on treatment schedules
- Methionine restriction targets a known vulnerability in cancer cells and is one of the most researched dietary adjuncts available to ovarian cancer patients
Best Foods to Eat During Ovarian Cancer Treatment
Rather than searching for a single "superfood," research consistently points to overall dietary patterns—particularly plant-forward eating—as most beneficial for ovarian cancer patients. The focus should be on building meals around nutrient-dense whole foods rather than relying on any one magical ingredient.
Vegetables and Fruits
Cruciferous vegetables deserve special attention. Research has found that higher intake of cruciferous vegetables is inversely related to ovarian cancer incidence, with case-control studies showing a 16% risk reduction. Fill at least half your plate with colorful vegetables at every meal, emphasizing:
- Broccoli, cauliflower, Brussels sprouts, and kale
- Dark leafy greens like spinach and Swiss chard
- Bell peppers, tomatoes, and carrots
- Berries, citrus fruits, and other colorful produce
These plant foods deliver antioxidants, vitamin C, and phytonutrients that support immune function during treatment. Preclinical research also shows that sulforaphane—a compound concentrated in broccoli and Brussels sprouts—can inhibit ovarian cancer cell growth and work alongside chemotherapy agents. Organic produce isn't required. Variety matters more than sourcing.

Protein and Whole Grains
Adequate protein is essential during treatment to prevent muscle wasting, support tissue repair after surgery, and maintain immune cell production. Prioritize lean, plant-based, or low-saturated-fat sources:
- Legumes, beans, lentils, and chickpeas
- Fish (especially fatty fish like salmon)
- Tofu, tempeh, and edamame
- Eggs in moderation
- Small amounts of poultry
Research also supports inclusion of soy products. High soy intake is linked to reduced ovarian cancer risk, particularly in Asian populations (RR 0.29), and authoritative sources confirm whole soy foods don't increase risk for hormone-sensitive cancers.
Whole grains are worth prioritizing for more than energy alone. Higher fiber intake and lower glycemic index diets are linked to better post-diagnosis survival, with the highest quartile of pre-diagnosis fiber intake associated with a 31% mortality reduction (HR 0.69). Choose:
- Quinoa, oats, brown rice, and farro
- Whole wheat bread and pasta
- Barley and bulgur
Beyond blood sugar stability and digestive support, this fiber intake may be one of the most impactful dietary choices a patient makes—which connects directly to why staying hydrated matters just as much.
Hydration
Hydration becomes especially critical during treatment. Adequate fluid intake reduces constipation risk, aids kidney function during chemotherapy (helping flush toxins), and may ease fatigue. Aim for at least 6–8 cups of fluid daily, including:
- Plain water
- Herbal teas (ginger tea can help with nausea)
- Broths and soups
- High-water-content foods like cucumber, watermelon, and celery
Don't wait until you feel thirsty—treatment can dull thirst signals while increasing fluid needs.
Foods and Habits to Avoid with Ovarian Cancer
Avoidance doesn't mean strict restriction. Overly restrictive diets during treatment can cause dangerous calorie and nutrient deficits. However, certain foods have a strong enough evidence to guide your choices.
Red and Processed Meats
Animal fat and processed meats influence estrogen activity and elevate insulin-like growth factor-1 (IGF-1), a compound linked to cancer progression. The NIH-AARP Diet and Health Study found that women in the highest quintile of animal fat intake had a 30% greater risk of ovarian cancer (RR 1.30). Processed meats also introduce N-nitroso compounds and heterocyclic amines — potential carcinogens formed during preservation and high-heat cooking.
Minimize or eliminate:
- Beef, pork, and lamb
- Cold cuts, sausage, bacon, and hot dogs
- Heavily charred or grilled meats
Plant proteins, fish, and small amounts of poultry are practical substitutes.
Dairy Products
Research on dairy is mixed, but multiple meta-analyses have found associations between high dairy consumption and increased ovarian cancer risk. A pooled analysis of 12 cohorts found that lactose intakes ≥30g/day were associated with 19% higher ovarian cancer risk compared to low intake. This is attributed to lactose metabolism into galactose (which may interfere with ovarian function) and IGF-1 elevation.
Discuss dairy intake with your care team. Common plant-based alternatives include:
- Almond milk or oat milk (for cow's milk)
- Coconut yogurt or soy yogurt
- Cashew-based cheese spreads
Added Sugars and Ultra-Processed Foods
Cutting all sugar is counterproductive — natural sugars in fruit provide essential nutrients. The real concern is added sugars in baked goods, sweetened beverages, and processed snacks, which contribute to obesity (a risk factor for worse outcomes) and displace nutrient-dense foods.
The data on ultra-processed foods is striking: every 10% increase in ultra-processed food consumption is associated with 19% higher ovarian cancer incidence and 30% higher cancer-specific mortality. Reading ingredient labels and reducing packaged snack foods is one of the highest-impact changes you can make.

Alcohol and Food Safety
Comprehensive meta-analyses found no material association between alcohol and epithelial ovarian cancer risk specifically, but high intake is linked to immune suppression and increased risk for other cancers. The World Cancer Research Fund recommends avoiding alcohol for general cancer prevention — a reasonable standard during active treatment.
Food safety is a separate but equally practical concern, particularly during immunosuppressive chemotherapy. When your immune defenses are reduced, certain foods carry real infection risk. Avoid:
- Raw fish (sushi, poke bowls)
- Unpasteurized dairy and soft cheeses
- Undercooked meats and eggs
- Raw sprouts
Standard food safety practices — clean, separate, cook to temperature, chill promptly — protect against foodborne illness and are easy to maintain throughout treatment.
Managing Treatment Side Effects Through Diet
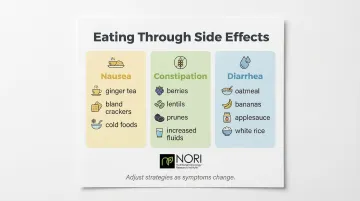
Treatment side effects—nausea, constipation, diarrhea, appetite loss, fatigue, and taste changes—often make eating the biggest challenge for ovarian cancer patients. Targeted dietary adjustments for each symptom can improve tolerance and quality of life.
Nausea and Vomiting
Small, frequent meals work better than three large ones. Your stomach tolerates smaller volumes more easily when nausea strikes.
Try these strategies:
- Cool or room-temperature foods (frozen fruit, cold smoothies) to reduce smell-triggered nausea
- Bland options like saltine crackers, toast, or plain rice for acute episodes
- Ginger-based foods or teas—oral ginger supplementation (0.5g to 1.0g daily) reduces acute chemotherapy-induced vomiting by 42%
- Avoid greasy, fried, or heavily spiced meals during flares
Eat slowly and rest after meals in an upright position.
Constipation and Diarrhea
For constipation: Gradually increase fiber intake with whole grains, berries, avocado, lentils, and broccoli. Pair with increased fluid intake—fiber without adequate water worsens constipation. Prunes and prune juice provide natural sorbitol, which draws water into the intestines. Consider discussing soluble fiber supplements with your clinician.
For diarrhea: Limit raw vegetables, fruit juices, caffeine, and fried foods. Focus on:
- Soluble-fiber foods like oatmeal, bananas, applesauce, and white rice (the BRAT diet foundation)
- Well-cooked vegetables
- Lean proteins
- Plenty of fluids to prevent dehydration
Appetite Loss and Fatigue
When appetite is poor, prioritize calorie- and protein-dense foods in small portions:
- Nut butters on toast or fruit
- Full-fat yogurt or Greek yogurt
- Eggs prepared any way you tolerate
- Avocado added to meals
- Protein smoothies with banana, nut butter, and protein powder
The "food fortification" approach works well here: adding cream, olive oil, butter, or nut butter increases calorie density without increasing volume.
For fatigue-related eating challenges, try these practical habits:
- Keep simple ready-to-eat foods on hand (cheese sticks, hard-boiled eggs, trail mix)
- Limit caffeine to mornings to avoid disrupting sleep
- Don't skip meals even when appetite is low — consistent intake prevents energy crashes
Taste Changes
Metallic taste and flavor changes are common during chemotherapy. Try these adjustments:
- Add acidic flavor enhancers (lemon, lime, vinegar) to counter metallic taste
- Use wooden or plastic utensils instead of metal
- Experiment with cold foods, which may taste better
- Use fresh herbs and mild seasonings to enhance palatability
- Try different protein sources if meat tastes strange
Taste changes typically resolve within weeks of completing a treatment cycle — keeping a short log of what tastes tolerable helps you rebuild a sustainable eating routine faster.
Supplements and Advanced Nutritional Strategies for Ovarian Cancer
Most supplement marketing is "more marketing than science"—the priority should always be obtaining nutrients from whole foods. That said, certain supplementation may be appropriate under medical supervision.
Watch for Supplement-Drug Interactions
Certain supplements can interfere with chemotherapy or radiation. St. John's Wort interacts with many chemotherapy agents, and high-dose antioxidants may protect cancer cells during treatment. Always discuss any supplement with your oncology team before starting.
Vitamin D: Get Your Levels Tested
Higher serum 25(OH)D concentrations at diagnosis are associated with longer survival (adjusted HR 0.93 per 10 nmol/L increase). Vitamin D deficiency is common in cancer patients — have your levels tested and supplement appropriately under medical supervision.
Methionine Restriction: A Targeted Metabolic Approach
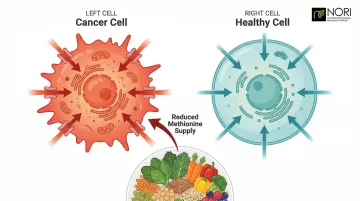
Beyond individual supplements, some nutritional protocols target cancer metabolism directly. Methionine restriction is one such approach — it exploits a documented vulnerability in cancer cells.
Methionine is an amino acid found predominantly in animal proteins. Cancer cells often have an elevated need for it, and depriving them of methionine can arrest their growth. Reducing animal protein intake without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. NORI's protocol uses a low-methionine, plant-based dietary approach combined with proprietary nutraceuticals, built on over 20 years of focused research into this mechanism. Clinical case reports show oral methioninase dosing achieved a 50% reduction in circulating methionine in a high-stage ovarian cancer patient.
Building a Plan Around Your Situation
Nutritional needs shift depending on where you are in treatment — active chemotherapy, post-surgery recovery, and survivorship each call for different priorities. Work with a registered dietitian experienced in oncology alongside any integrative program to build a plan matched to your specific situation.
Conclusion
No single food or diet cures ovarian cancer, but overall dietary choices—prioritizing plants, adequate protein, hydration, and whole foods while minimizing processed foods and animal fats—can meaningfully support treatment outcomes, quality of life, and long-term survival. The Ovarian Cancer Association Consortium found that adherence to healthy eating patterns reduces early-stage mortality by up to 34%.
Working with your care team to implement even a few of these dietary shifts is a practical starting point. For patients looking for structured, science-based nutritional support, NORI (Nutritional Oncology Research Institute) offers a home-based program built on founder Mark Simon's cancer nutrition research dating back to 2004. The program includes personalized guidance, free initial consultations, and is available to patients worldwide. Contact NORI at 800-634-3804 or info@nutritionaloncology.net to learn more.
Frequently Asked Questions
What is the best diet for ovarian cancer patients?
There is no single perfect diet, but research most consistently supports a plant-forward, whole-food dietary pattern rich in vegetables, legumes, whole grains, and lean protein, while minimizing processed meats, added sugars, and excess saturated fat. This eating pattern reduces inflammation, supports immune function, and is associated with better survival outcomes.
What foods should ovarian cancer patients avoid?
Limit processed and red meats (linked to elevated IGF-1 and estrogen activity), high-sugar processed foods, excess dairy, alcohol during treatment, and raw or unpasteurized foods when immunosuppressed. Ultra-processed foods are particularly concerning: each 10% increase in consumption is associated with 30% higher ovarian cancer mortality.
Does ovarian cancer affect your bowels?
Yes, ovarian cancer and its treatments commonly affect bowel function, causing constipation, diarrhea, bloating, or obstruction due to the tumor's proximity to the bowel, ascites (fluid accumulation), and chemotherapy side effects. Dietary adjustments including adequate fiber, hydration, and gentle foods can help manage these symptoms.
Is ovarian cancer aggressive?
Ovarian cancer is frequently diagnosed at advanced stages (III or IV), which is why early nutritional intervention matters. Stage at diagnosis strongly influences outcomes, making diet and lifestyle support a meaningful part of ongoing management at any stage.
When does ovarian cancer come back?
Recurrence most commonly occurs within the first two years after treatment, with roughly 70% of advanced-stage patients experiencing relapse within three years. Maintaining a healthy weight, staying active, and following an anti-inflammatory diet may help reduce that risk.
Can you live a long life after ovarian cancer?
Yes, many people live long, full lives after ovarian cancer, particularly those diagnosed at early stages. Data from the Ovarian Cancer Association Consortium found that high-quality eating patterns post-diagnosis reduce all-cause mortality risk by up to 34% in early-stage patients.


