
This guide cuts through the noise by examining what peer-reviewed research actually supports. We'll cover what to eat, what to avoid, how to manage treatment side effects through diet, and how specific nutritional strategies may influence cancer biology itself. While no single food prevents or cures ovarian cancer, emerging evidence shows that dietary patterns—both during and after treatment—are linked to meaningful differences in quality of life, treatment tolerance, and survival outcomes.
TLDR
- Diet directly affects treatment outcomes, immune function, and survival rates in ovarian cancer patients
- Plant-forward eating rich in cruciferous vegetables, legumes, and anti-inflammatory foods is consistently associated with better outcomes
- Reduce animal fat, processed meats, high-dairy intake, added sugars, and alcohol
- Manage side effects like nausea and constipation through targeted dietary choices
- Metabolic strategies — including methionine restriction — can target cancer cell vulnerabilities that conventional treatment does not address
Why Nutrition Matters for Ovarian Cancer
Diet influences multiple biological pathways implicated in ovarian cancer—each capable of shaping tumor behavior and treatment response:
- Estrogen metabolism — affects hormone-driven cancer cell signaling
- IGF-1 production — elevated levels are linked to tumor growth and proliferation
- Systemic inflammation — chronic inflammation creates a permissive environment for cancer progression
- Immune function — nutritional status directly influences the body's ability to recognize and fight cancer cells
A 2014 analysis of the Women's Health Initiative examined 636 ovarian cancer cases and found that women with the highest diet quality scores had a 27% lower risk of all-cause mortality after diagnosis compared to those with the poorest dietary quality. That is a clinically meaningful difference achieved through food choices alone.

Population data reinforces this picture. Japanese research from 1987 found that the age-adjusted ovarian cancer death rate increased 3.6-fold in Japan between 1949 and 1984. The rise tracked directly with westernization of dietary habits: fat intake grew 3.6-fold and dairy consumption increased 30.2-fold over the same period.
Nutrition during treatment serves different purposes than prevention. The priority shifts to maintaining body weight, preserving lean muscle mass, supporting immune resilience, and enabling the body to tolerate chemotherapy or surgery. A 2023 prospective cohort study of 591 invasive epithelial ovarian cancer patients found that higher protein intake (>1.5 vs. ≤1 g/kg body weight) post-treatment was associated with significantly better progression-free survival (HR 0.61).
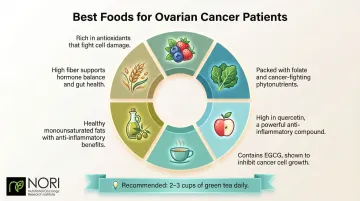
Best Foods to Eat When You Have Ovarian Cancer
Cruciferous and Allium Vegetables
Cruciferous vegetables—broccoli, cauliflower, Brussels sprouts, kale, cabbage—contain compounds called isothiocyanates and glucosinolates with demonstrated anti-inflammatory and potential wellness-supporting activity.
Research supports their protective value:
- A 2015 meta-analysis found 11% reduction in ovarian cancer risk associated with high cruciferous vegetable intake
- Laboratory studies show sulforaphane (from broccoli) affects cellular processes being investigated in research in human ovarian carcinoma cell lines
- Aim for at least 1-2 servings daily when tolerated
Allium vegetables (garlic, onions, leeks) also show protective associations supported by large cohort data. The European EPIC cohort study found a 21% decrease in ovarian cancer risk per 8g/day increment in garlic and onion intake.
Legumes, Soy, and Plant Proteins
Soy products—tofu, tempeh, edamame, soy milk—contain isoflavones, plant compounds structurally similar to estrogen. Despite common fears about hormone-related cancers, a 2009 meta-analysis found the highest soy intake was associated with 48% lower risk of ovarian cancer compared to the lowest intake.
Research consistently indicates soy foods are safe and potentially beneficial for ovarian cancer patients. Isoflavones bind to estrogen receptors and block more potent natural estrogens, which may explain some of the protective effect. Both the American Cancer Society and Memorial Sloan Kettering affirm that dietary soy is safe, though they don't recommend high-dose soy supplements.
Other plant proteins deliver benefits without the saturated fat and IGF-1-elevating effects of animal proteins:
- Lentils
- Black beans, chickpeas, kidney beans
- Quinoa
- Split peas
These provide fiber, folate, and protein while supporting healthy insulin and inflammation levels.
Anti-Inflammatory Foods and Beverages
Alongside vegetables and plant proteins, flavonoid-rich foods round out a dietary pattern with particularly strong protective associations in ovarian cancer research. The Nurses' Health Study found that women in the highest quintile of kaempferol intake (found in broccoli, kale, and tea) had a 40% decrease in epithelial ovarian cancer incidence compared to the lowest quintile.
Green tea stands out in this category. A 2024 pooled analysis of 10 studies found that consuming ≥1 cup/day of green tea before diagnosis was associated with 16% better overall survival and 19% better ovarian cancer-specific survival. Even more compelling, a 2004 study of 254 epithelial ovarian cancer patients in China found that consuming ≥1 cup of green tea daily post-diagnosis enhanced survival significantly (HR 0.43).
Build your diet around:
- Berries (blueberries, strawberries, raspberries)
- Dark leafy greens (spinach, kale, arugula)
- Apples
- Green tea (2-3 cups daily)
- Olive oil as primary fat source
- Whole grains (oats, quinoa, brown rice)
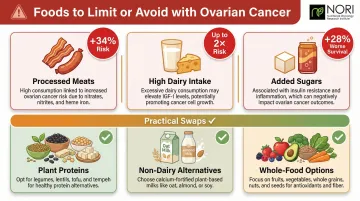
Foods to Limit or Avoid with Ovarian Cancer
Animal Fats and Processed Meats
Multiple large cohort studies link higher animal fat intake to elevated ovarian cancer risk. The NIH-AARP Diet and Health Study found that women in the highest quintile of animal fat consumption had a 30% increased risk of ovarian cancer compared to the lowest quintile.
Processed meats present additional concerns. Research from the same NIH-AARP cohort showed that women with the highest intake of animal-sourced nitrites had a 34% increased risk of epithelial ovarian cancer. Plant-sourced nitrites showed no such association—the concern is specific to cured meats like bacon, sausage, ham, hot dogs, and pepperoni.
Practical steps:
- Minimize red meat consumption
- Eliminate or drastically reduce processed meats
- Replace animal proteins with plant proteins, fish, or poultry
- When eating meat, use it as a condiment rather than a centerpiece
Dairy and Lactose
The dairy-ovarian cancer relationship is complex but worth taking seriously. A pooled analysis of 12 cohort studies involving 553,217 women found a 19% higher risk of ovarian cancer for lactose intakes ≥30 g/day (equivalent to ≥3 servings of milk) versus <10 g/day.
Additional studies strengthen this association:
- Swedish Mammography Cohort: Women consuming ≥4 servings of dairy daily had twice the risk of serous ovarian cancer
- Nurses' Health Study: Women consuming ≥1 serving of skim or low-fat milk daily had 32% higher overall risk and 69% higher risk of serous ovarian cancer
Researchers point to several possible mechanisms: galactose (lactose's breakdown product) may be toxic to ovarian cells, and milk proteins can elevate IGF-1 levels and disrupt hormonal pathways. Some conflicting findings exist, but the overall evidence supports limiting dairy intake.
Added Sugars, Refined Carbohydrates, and Alcohol
High added sugar intake contributes to obesity and elevated insulin levels, both independently linked to poorer ovarian cancer outcomes. An Australian cohort study of 811 women with invasive ovarian cancer found that higher pre-diagnosis dietary glycemic index was associated with 28% worse overall survival.
Alcohol is a separate consideration. Large pooled analyses haven't consistently linked it to ovarian cancer incidence, but it weakens immune function, disrupts hormonal balance, and adds empty calories with no nutritional benefit. Limiting or avoiding it during treatment and recovery is a reasonable, low-risk step.
Limit or eliminate:
- Sugary beverages (soda, sweetened tea, fruit juice)
- Refined carbohydrates (white bread, pastries, cookies)
- Added sugars (candy, desserts, processed foods)
- Alcohol (or limit to occasional small amounts)
Managing Treatment Side Effects Through Diet
Nausea, Appetite Loss, and Taste Changes
Nausea responds well to small, frequent meals eaten every 2-3 hours. Other practical strategies:
- Choose cold or room-temperature foods, which produce less aroma than hot meals
- Try ginger tea or ginger-containing foods — meta-analyses confirm ginger significantly reduces chemotherapy-induced nausea
- Favor bland, starchy foods (plain crackers, rice, toast)
- Avoid lying down immediately after eating
Appetite loss is worth taking seriously — undereating during treatment can impair recovery and reduce treatment tolerance. Calorie-dense, nutrient-rich options that work well in small portions:
- Greek yogurt or plant-based yogurt
- Nut butters (almond, peanut, cashew)
- Eggs and avocado
- Smoothies with protein powder
Taste changes, including metallic taste, are common with chemotherapy. These adjustments often help:
- Use plastic utensils instead of metal to reduce metallic perception
- Add tart or sour flavors (lemon, lime, vinegar)
- Incorporate fresh herbs and spices
- Marinate proteins to enhance flavor
- Experiment with different food temperatures
Constipation, Diarrhea, and Digestive Issues
Digestive symptoms are among the most common — and manageable — challenges during ovarian cancer care.
Constipation often develops with pain medications and certain chemotherapy agents. To address it:
- Gradually increase fiber from whole grains (oats, quinoa, bran)
- Include vegetables (broccoli, carrots, artichokes)
- Eat fiber-rich fruits (pears, berries, avocado, prunes)
- Stay well-hydrated throughout the day
- Gentle movement helps stimulate bowel function
Diarrhea requires a different approach:
- Temporarily reduce raw vegetables and fruit juice
- Favor soluble fiber foods (oatmeal, bananas, cooked vegetables, applesauce)
- Restore electrolytes with broth or electrolyte drinks
- Avoid fatty or greasy foods
- Seek medical guidance if diarrhea persists more than 48 hours
Regardless of which digestive symptoms arise, aim for at least 2 liters of fluid daily through water, herbal teas, diluted juices, and broth. Consistent hydration supports digestion, treatment efficacy, and energy levels.
A Deeper Nutritional Approach: Targeting Cancer Cell Metabolism
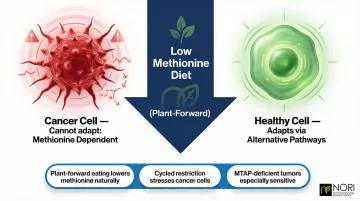
Cancer cells have fundamentally different metabolic needs than healthy cells. They rely heavily on glucose and specific amino acids—particularly methionine—to sustain rapid division. Methionine is an essential amino acid found predominantly in animal proteins. Research shows that restricting methionine availability selectively stresses cancer cells because healthy cells can adapt using alternative metabolic pathways, while cancer cells cannot.
This metabolic vulnerability is sometimes called the "Hoffman Effect," named after pioneering research in this field. Studies demonstrate that dietary methionine restriction alters cancer cell metabolism in ways that enhance the effectiveness of conventional therapies. Reducing protein intake — especially animal protein — without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. A plant-based dietary pattern naturally reduces methionine intake because plant foods contain significantly lower methionine levels than animal proteins — reinforcing why a plant-forward approach has both epidemiological and mechanistic support.
Research specific to ovarian cancer shows that low expression of MTAP (an enzyme involved in methionine recycling) is associated with platinum resistance and poor survival, suggesting methionine restriction may offer particular benefit for this cancer type.
Key findings from the methionine restriction research converge on several actionable principles:
- Plant-forward eating lowers methionine intake naturally, without extreme restriction
- Cycled restriction — alternating periods of low and normal methionine — may stress cancer cells while preserving healthy tissue function
- MTAP-deficient tumors, common in ovarian cancer, appear especially sensitive to methionine-targeted approaches
NORI has applied these principles through its home-based nutritional support program since 2011, combining cycled methionine restriction with nutraceutical support designed to target cancer cell metabolic vulnerabilities. For patients interested in this approach, free initial consultations are available at 800-634-3804.
Frequently Asked Questions
What is the best food to eat if you have ovarian cancer?
No single food cures cancer, but the strongest evidence supports a plant-forward diet rich in cruciferous vegetables (broccoli, kale), legumes, soy foods, flavonoid-rich berries and green tea, and whole grains. This dietary pattern is most consistently associated with better ovarian cancer outcomes.
What foods should I avoid with ovarian cancer?
The most evidence-supported categories to minimize are animal fat from processed meats and dairy (especially whole milk), added sugars and refined carbohydrates, and alcohol. These foods promote inflammation and elevate IGF-1, which can compromise both immune response and hormonal balance.
Can diet affect ovarian cancer recurrence or survival?
Yes. The Women's Health Initiative and other cohort studies link diet quality directly to ovarian cancer mortality — women eating the most healthful diets had 27% lower mortality risk, with fiber intake and lower glycemic index diets also associated with survival advantages.
Should I take supplements during ovarian cancer care?
Most supplements lack sufficient evidence for ovarian cancer specifically. Some (like St. John's Wort) interfere with chemotherapy, and high-dose antioxidant supplements may actually protect cancer cells during cancer care. Always consult your oncology team before adding any supplement.
Does sugar "feed" ovarian cancer?
While cancer cells preferentially consume glucose, cutting all sugar isn't necessary or effective. The real concern is excess added sugar and high-glycemic foods that drive insulin and IGF-1 elevation — whole food sources like fruit and whole grains remain appropriate.
How can I manage appetite loss during ovarian cancer care?
Practical strategies include:
- Eat small, frequent meals rather than three large ones
- Choose calorie-dense options like nut butters, eggs, avocado, and yogurt
- Try protein-rich smoothies when solid food is difficult
- Light movement before meals can help stimulate appetite
Work with a registered dietitian or oncology nutrition team for guidance tailored to your treatment phase.


