
Introduction
Food is more than fuel—for millions of people managing chronic or serious illness, what they eat is part of their treatment. An estimated 40% of incident cancers and 44% of cancer deaths in the United States are attributable to modifiable risk factors, including diet, excess body weight, and physical inactivity. Yet once diagnosed, up to 41% of active cancer patients suffer from malnutrition, which nearly doubles mortality risk and increases postoperative complications.
That gap is exactly where the therapeutic diet meal plan comes in. A therapeutic diet is a physician- or dietitian-prescribed modification of regular eating, tailored to control specific nutrients, textures, or food groups based on a person's medical condition. It is not a wellness cleanse or a trend—it is a clinical intervention with measurable outcomes.
TLDR:
- Therapeutic diets are medically prescribed interventions, not wellness trends
- Up to 41% of cancer patients suffer from malnutrition, doubling mortality risk
- Dietary counseling reduces weight loss and improves quality of life during treatment
- Methionine restriction targets cancer cell metabolism at a biochemical level
- The NORI Protocol combines cycled dietary restriction with nutraceuticals for cancer support
What Is a Therapeutic Diet Meal Plan?
A therapeutic diet is a medically prescribed nutrition intervention — not simply a "healthy eating plan." The Academy of Nutrition and Dietetics defines it as a regimen that modifies, eliminates, decreases, or increases specific micro- and macronutrients based on a patient's medical condition.
This differs from a general "healthy diet" because it's prescribed for a specific medical purpose and tailored to the individual.
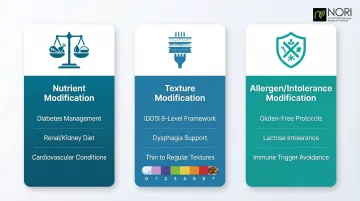
The therapeutic diet framework encompasses three primary modification categories:
Nutrient Modification — Manages conditions like diabetes, kidney disease, or cardiovascular disease by adjusting macronutrients (protein, fat, carbohydrates) or micronutrients (sodium, potassium, vitamins).
Texture Modification — Adapts food consistency for patients with swallowing or chewing difficulties. The International Dysphagia Diet Standardisation Initiative (IDDSI) 8-level framework became the sole recognized standard in 2021, replacing the older National Dysphagia Diet.
Allergen/Intolerance Modification — Removes foods that trigger immune reactions or digestive intolerance, such as gluten in celiac disease or lactose in dairy sensitivity.
Who Prescribes Therapeutic Diets?
Therapeutic diets are ordered by physicians or registered dietitians. A 2014 CMS final rule empowered qualified dietitians to independently order therapeutic diets in certain Medicare- and Medicaid-participating facilities, without requiring a separate physician co-signature.
In practice, the prescribing professional depends on the clinical setting. Hospitals typically involve a multidisciplinary team — physician, dietitian, and sometimes a speech-language pathologist — while outpatient or home-based programs may be guided primarily by a registered dietitian nutritionist (RDN).



