
Yet most men diagnosed with prostate cancer receive little dietary guidance from their oncology teams. Online information is contradictory and overwhelming, leaving patients uncertain about which foods truly matter. This guide cuts through the noise, presenting the foods most strongly linked to protection and risk, how nutritional needs shift through treatment phases, and the dietary patterns backed by the strongest evidence.
TLDR: Key Nutrition Takeaways
- A predominantly plant-based, anti-inflammatory diet is associated with lower prostate cancer risk and slower progression
- Prioritize lycopene from cooked tomatoes, cruciferous vegetables, omega-3-rich fish, soy products, and green tea
- Avoid red and processed meats, high-fat dairy (especially whole milk), refined carbohydrates, and omega-6-heavy oils
- Nutritional needs shift across treatment phases — ADT, radiation, surgery, and chemotherapy each call for targeted dietary adjustments
- Long-term dietary consistency and maintaining a healthy body weight drive better outcomes than chasing any single nutrient
How Diet Shapes Prostate Cancer Risk and Progression
Geographic Evidence Points to Diet as a Key Factor
Prostate cancer rates look dramatically different depending on where you live. According to GLOBOCAN 2022 data, incidence in Western nations far exceeds rates in regions where traditional plant-based diets are the norm:
| Region | Incidence Rate (per 100,000 men) |
|---|---|
| United States | 95.9 |
| Australia | 77.2 |
| United Kingdom | 74.0 |
| Japan | 50.1 |
| South Korea | 38.6 |
This near two-fold difference between Western and East Asian countries suggests diet is a key modifiable risk factor, not simply genetics or screening practices.
Biological Pathways Linking Diet to Disease
Dietary choices influence prostate cancer through several interconnected mechanisms:
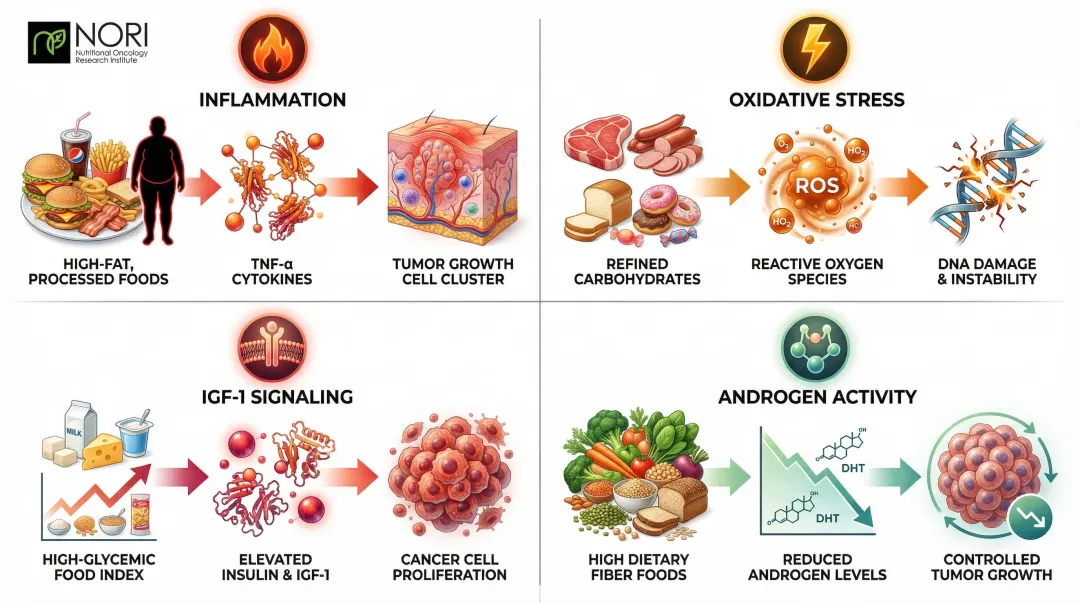
- High-fat diets and obesity increase tumor necrosis factor-alpha (TNF-α) secretion, triggering chronic inflammation that creates an environment favorable to tumor growth.
- Animal proteins, refined carbohydrates, and excess fats generate reactive oxygen species (ROS) that promote genetic instability and cell proliferation — antioxidant-rich diets counteract this directly.
- Dairy-heavy and high-glycemic diets elevate insulin and insulin-like growth factor 1 (IGF-1), which drive cancer cell proliferation and suppress apoptosis (programmed cell death).
- Certain dietary fibers reduce circulating androgens and raise sex hormone-binding globulin, potentially slowing hormone-driven tumor growth.
The Obesity Connection
These biological mechanisms don't operate in isolation — body weight amplifies each of them. A dose-response meta-analysis of 280,199 patients found that obesity (BMI ≥ 30) is associated with a 19% increased risk of prostate cancer-specific mortality, with death risk rising 9% for every additional 5 kg/m² in BMI.
For men managing or trying to prevent prostate cancer, this means dietary choices carry a two-level impact: they shape the molecular environment inside cells and determine the metabolic conditions that govern long-term outcomes.
Best Foods for Prostate Cancer: What the Research Supports
Lycopene-Rich Foods
Lycopene is a potent carotenoid antioxidant found in tomatoes, watermelon, and pink grapefruit. It neutralizes free radicals, helps regulate the cell cycle, and influences IGF-1 activity.
A comprehensive meta-analysis of 42 studies involving 692,012 participants found that both dietary intake and circulating lycopene levels are associated with reduced prostate cancer risk. The findings showed a 1% risk reduction per 2 mg/day increase in dietary lycopene, and a 3.5–3.6% risk reduction per 10 μg/dL increase in circulating levels.
The preparation method matters significantly. A clinical study demonstrated that consuming tomatoes cooked with extra virgin olive oil resulted in an 82% increase in plasma lycopene compared to tomatoes cooked without oil. Heat breaks down plant cell walls, and fat enhances absorption of this fat-soluble compound.
Practical application: Cook diced tomatoes with olive oil for pasta sauces, soups, and stews rather than eating raw tomatoes.
Cruciferous Vegetables
Broccoli, cauliflower, kale, Brussels sprouts, and cabbage contain glucosinolates that break down into sulforaphane and indole-3-carbinol—compounds that activate liver detoxification enzymes, protect against DNA damage, and induce cancer cell apoptosis.
The evidence for disease management is particularly strong. In a prospective study of 1,560 men with non-metastatic prostate cancer, those in the highest quartile of post-diagnostic cruciferous vegetable intake had a 59% decreased risk of disease progression compared to men in the lowest quartile.

Mechanism: Sulforaphane suppresses prostate cancer cell proliferation by causing cell cycle arrest and triggering protein degradation pathways that lead to apoptosis. Indole-3-carbinol acts as a dietary histone deacetylase (HDAC) inhibitor, reducing HDAC activity by up to 66% in prostate cancer cells.
Practical guidance: Aim for 3–5 servings of cruciferous vegetables weekly. Lightly steam or sauté rather than boiling, which can leach beneficial compounds into cooking water.
Omega-3 Fatty Acids and Oily Fish
Marine omega-3 fatty acids (EPA and DHA from fish; ALA from flaxseed and walnuts) block the arachidonic acid cascade at cyclooxygenase (COX) and lipoxygenase (LOX) pathways, reducing pro-inflammatory prostaglandins that fuel tumor growth.
Omega-3s also modulate IGF-1 signaling and may delay the transition from androgen-sensitive to androgen-resistant disease — a critical progression point in advanced prostate cancer.
How you cook fish changes its risk profile. A population-based case-control study found that high intake of deep-fried fish was associated with a 41% increased risk of aggressive prostate cancer. High temperatures and frying oils introduce carcinogenic compounds and destroy beneficial fatty acids.
Practical recommendations:
- Consume oily fish (salmon, sardines, mackerel, herring) 2–3 times weekly
- Bake, grill, or poach fish — avoid frying
- Plant-based alternatives: ground flaxseed (1–2 tablespoons daily) or walnuts for those preferring non-animal sources
The omega-6 contrast: Excess omega-6 fatty acids from corn, safflower, sunflower, and soybean oils generate pro-inflammatory arachidonic acid metabolites that alter the tumor microenvironment and raise androgen levels. Maintaining a low omega-6 to omega-3 ratio may delay progression to castration-resistant disease.
Soy and Plant-Based Proteins
Soy isoflavones — genistein and daidzein — accumulate in prostate tissue and work through several pathways: inhibiting 5-alpha-reductase (which converts testosterone to the more potent DHT), inducing apoptosis, and suppressing both androgen-dependent and androgen-independent cancer cell growth.
An updated meta-analysis demonstrated significant protective associations:
- Genistein: 10% reduced risk (RR: 0.90)
- Daidzein: 16% reduced risk (RR: 0.84)
The protective effect was strongest for dietary intake in Asian populations, suggesting whole food sources are superior to isolated supplements.
Practical sources:
- Tofu (firm or silken for different recipes)
- Tempeh (fermented, higher protein)
- Edamame (whole soybeans)
- Unsweetened soy milk (fortified with calcium and vitamin D)
Aim for 1–2 servings daily. One serving equals ½ cup tofu, 1 cup soy milk, or ½ cup edamame.
Protective Phytonutrients: Green Tea, Garlic, and Turmeric
Three additional plant compounds have meaningful research support for prostate cancer risk reduction and management.
- Green tea: Catechins (especially EGCG) inhibit cancer cell proliferation and reduce COX-2-mediated inflammation. The Japan Public Health Center-based Prospective Study followed 49,920 men and found those drinking 5+ cups daily had a 48% reduced risk of advanced prostate cancer (RR: 0.52) versus those drinking less than 1 cup daily.
- Garlic and allium vegetables: Organosulfur compounds like diallyl disulfide (DADS) cause caspase-dependent apoptosis through a mitochondrial pathway. This reduces survival of androgen-independent prostate cancer cells by inhibiting Akt phosphorylation and NF-κB expression.
- Turmeric (curcumin): Demonstrates anti-proliferative and anti-androgen effects. In animal models, oral curcumin inhibited androgen receptor expression at both mRNA and protein levels and reduced PSA expression.
Practical integration: Brew 3–5 cups of green tea daily, add crushed garlic to cooked dishes (let it sit 10 minutes after crushing to activate compounds), and incorporate turmeric into curries, soups, or golden milk beverages with black pepper to enhance absorption.
What to Avoid: Foods That May Fuel Prostate Cancer
Red and Processed Meats
Cooking red meat at high temperatures generates heterocyclic amines (HCAs) and polycyclic aromatic hydrocarbons (PAHs) like benzo[a]pyrene—compounds the prostate metabolizes into activated carcinogens.
In the NIH-AARP Diet and Health Study, grilled or barbecued meat intake was associated with an 11% increased risk of total prostate cancer and a 36% increased risk of advanced disease. Estimated benzo[a]pyrene intake was linked to a 28% increased risk of advanced cancer.
Processed meats preserved with nitrites and nitrates (bacon, sausages, deli meats) contribute to N-nitroso compound formation—potential human carcinogens. Nitrite and nitrate from meat were associated with advanced prostate cancer risk increases of 24% and 31% respectively.
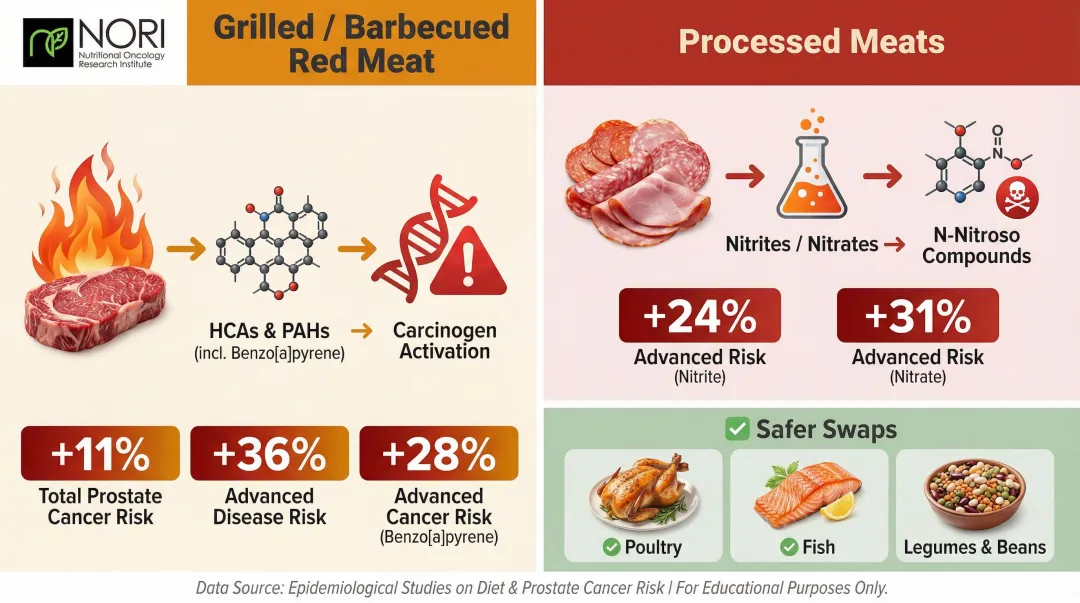
Practical substitutes: Skinless poultry prepared at lower temperatures, fish, legumes (lentils, chickpeas, black beans), and tofu as protein sources.
High-Fat Dairy Products
Multiple mechanisms link dairy to prostate cancer progression:
IGF-1 Elevation: Dairy protein increases circulating IGF-1 by an estimated 0.10 standard deviation per standard deviation increase in milk intake. Elevated IGF-1 is positively associated with prostate cancer risk.
Whole Milk and Mortality: Post-diagnostic consumption of whole milk is particularly concerning. In the Physicians' Health Study survival analysis, whole milk intake (≥237 mL/day or 1 serving daily) was associated with a 117% increased risk of progression to fatal prostate cancer compared to non-drinkers.
Excessive Calcium: Intakes exceeding 1,500–2,000 mg/day may promote prostate cell proliferation. Non-dairy calcium sources, however, don't appear to carry the same elevated risk.
Practical alternatives: Unsweetened almond, oat, or soy milk fortified with calcium and vitamin D; nutritional yeast for cheese-like flavor; cashew-based cream sauces.
Refined Carbohydrates and Added Sugars
High-glycemic foods drive elevated insulin and IGF-1 levels, which serve as growth signals for prostate cancer cells. Hyperinsulinemia affects cancer directly through mitogenic effects (cell-growth-promoting signals) and indirectly by increasing bioactive IGF-1.
Research linking refined carbs to risk:
- Malmö Diet and Cancer cohort: High sugar-sweetened beverage intake associated with 38% increased risk of symptomatic prostate cancer
- PLCO Cancer Screening Trial: Highest quartile of sugar consumption from beverages linked to 21% increased risk
Foods to limit: Sugar-sweetened beverages, white bread, pastries, cookies, sweetened cereals, candy, and desserts.
Better choices: Steel-cut oats, quinoa, brown rice, whole grain bread, fresh fruit (which contains fiber that slows sugar absorption).
Omega-6-Heavy and Trans Fats
Like refined carbs, certain dietary fats feed the inflammatory pathways that prostate cancer exploits. Excess omega-6 fatty acids from corn, safflower, sunflower, and soybean oils generate pro-inflammatory arachidonic acid metabolites—compounds that ramp up enzymes producing prostaglandin E2, which drives prostate cancer cell proliferation.
Trans fats found in hydrogenated oils (margarine, commercial baked goods, fried foods) add a separate layer of risk. They disrupt hormone metabolism and increase oxidative stress. Circulating trans fatty acids are associated with higher prostate cancer odds, with a more than two-fold increased risk comparing highest to lowest levels.
Practical swaps: Replace vegetable oils high in omega-6 with extra virgin olive oil, avocado oil, or small amounts of coconut oil. Avoid products listing "partially hydrogenated" oils in ingredients.
Alcohol and Caloric Excess
Heavy alcohol consumption, particularly liquor, is associated with increased risk of aggressive prostate cancer. Ethanol metabolism produces acetaldehyde and promotes oxidative stress, damaging DNA and contributing to carcinogenesis.
Total caloric intake is an independent risk factor as well. A population-based case-control study found men consuming ≥2,439 kcal/day had a 115% increased risk of local cancer and 96% increased risk of regional or distant disease, compared to those consuming under 1,322 kcal/day.
Practical guidance: Limit alcohol to special occasions; practice portion control using smaller plates; eat mindfully without distractions; stop eating when 80% full.
Eating Through Treatment: Nutrition Phase by Phase
Pre-Treatment
Achieving or maintaining a healthy weight before treatment significantly improves outcomes and treatment tolerance. Build nutritional reserves through:
- Aim for 0.8–1.0g of protein per kg body weight daily — fish, poultry, legumes, and tofu are solid sources
- Prioritize vitamin D, selenium, zinc, and B vitamins through whole foods rather than isolated supplements
- Target 25–35g of fiber daily from vegetables, fruits, whole grains, and legumes
- Drink 8–10 glasses of water daily to support kidney and liver function
During Active Treatment
Surgery/Prostatectomy
Recovery demands higher protein and targeted micronutrients to support wound healing:
- Increase protein to 1.2–1.5g per kg body weight
- Emphasize vitamin C (citrus, bell peppers, strawberries) and zinc (pumpkin seeds, cashews) for tissue repair
- Stay hydrated to prevent constipation from pain medications
Radiation Therapy
GI symptoms — diarrhea, rectal urgency — are common. Dietary adjustments help manage them:
- Temporarily reduce insoluble fiber during acute symptoms
- Avoid spicy foods, caffeine, and high-fat meals that worsen GI distress
- Discuss probiotic use with your care team before starting
Androgen Deprivation Therapy (ADT)
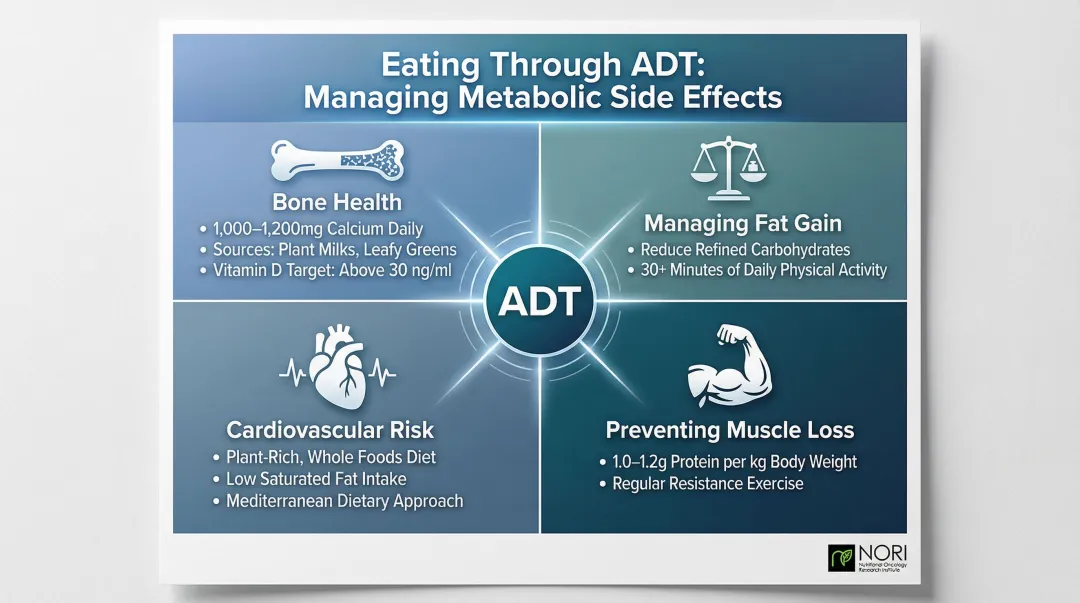
ADT triggers significant metabolic shifts — increased fat mass, muscle loss, and elevated cardiovascular risk — each requiring a specific dietary response:
- Get 1,000–1,200mg of calcium daily from fortified plant milks, leafy greens, and almonds; keep vitamin D levels above 30ng/ml
- Cut refined carbohydrates and stay active (30+ minutes daily) to offset fat gain
- Follow a heart-healthy, plant-rich diet low in saturated fats to reduce cardiovascular risk
- Combine adequate protein (1.0–1.2g per kg) with resistance exercise to counter muscle loss
Chemotherapy
Appetite disruption and nausea are the primary nutritional challenges during chemo:
- Eat small, frequent meals every 2–3 hours to manage nausea
- Use ginger or mint when taste changes make food unappealing
- Rely on smoothies to maintain calories and protein when appetite is poor
- Stay hydrated with herbal tea, diluted juice, or broth
- Avoid raw foods if white blood cell count is low
Post-Treatment and Survivorship
The same foods and patterns supporting prevention also lower recurrence risk. A study of men with non-metastatic prostate cancer found those with the highest plant-based diet scores had significantly lower risk of disease progression.
Continuing a low-saturated-fat, plant-rich diet in survivorship:
- Supports long-term quality of life
- Reduces cardiovascular risk (especially important given ADT-related metabolic effects)
- May help prevent biochemical recurrence
- Maintains healthy body weight
Beyond Single Foods: Dietary Patterns and Integrative Approaches
The most meaningful dietary impact comes from sustained overall eating patterns, not individual "superfoods." Multiple systematic reviews support two primary patterns:
- Mediterranean Diet: Rich in olive oil, fish, vegetables, legumes, and whole grains. A study in the Health Professionals Follow-up Study found greater adherence after diagnosis was associated with a 22% reduction in overall mortality.
- Whole-Food Plant-Based Diets: Emphasize vegetables, fruits, whole grains, legumes, nuts, and seeds while minimizing animal products. These patterns naturally reduce saturated fat, provide abundant fiber and phytonutrients, and help maintain a healthy body weight.
Methionine Restriction: An Advanced Nutritional Strategy
Methionine is an essential amino acid found primarily in animal proteins. Research shows cancer cells depend on methionine far more heavily than normal cells — a pattern called the "Hoffman effect." When methionine is restricted, cancer cells lose the ability to maintain stable gene regulation, which can trigger growth arrest and cell death.
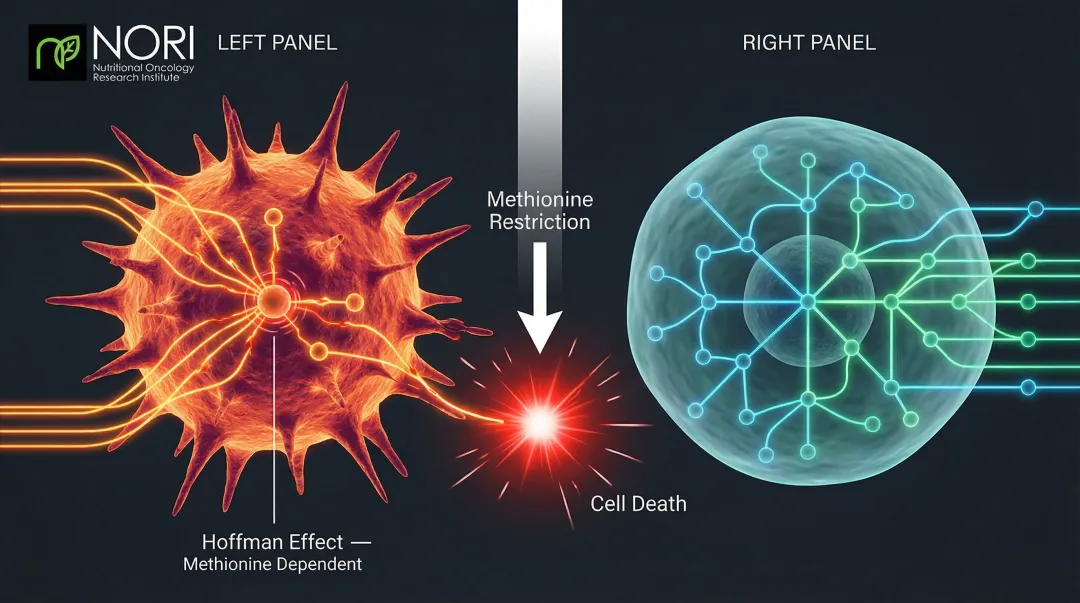
Methionine and cysteine are also required to produce glutathione, the cell's primary antioxidant shield. Restricting these amino acids leaves cancer cells exposed to oxidative stress in ways that healthy cells can tolerate.
NORI's protocol is built on this science. Men looking for a structured nutritional support program beyond general dietary guidelines can explore NORI's home-based program for prostate cancer, which combines cycled methionine restriction with targeted nutraceuticals designed to exploit these cancer cell vulnerabilities.
Working with Professionals
Consult a registered dietitian experienced in oncology nutrition to develop a personalized plan tailored to your specific cancer stage, treatment regimen, and nutritional status. Coordinate dietary changes with your oncology care team, particularly during active treatment, to avoid interactions and ensure nutritional adequacy.
Frequently Asked Questions
What is the best diet for someone with prostate cancer?
A plant-based diet rich in vegetables, fruits, whole grains, legumes, and omega-3 fatty acids—while low in saturated fats and processed foods—is the most evidence-supported approach. Consistency matters more than any single food; sustainable daily choices make the real difference.
What foods should you avoid if you have prostate cancer?
Limit or avoid:
- Red and processed meats, especially grilled or fried
- High-fat dairy products, particularly whole milk
- Refined carbohydrates and sugar-sweetened beverages
- Foods high in trans fats or omega-6 oils
These foods promote inflammation, elevate IGF-1, and may accelerate disease progression.
What supplements should be avoided with prostate cancer?
High-dose vitamin E supplementation alone has been shown in the SELECT trial to increase prostate cancer risk by 17%. Excessive calcium supplementation above 1,500mg/day may promote cell proliferation. All supplement decisions should be made in consultation with your oncology team to avoid interactions.
How can you prevent prostate cancer from returning?
Continue a low-fat, plant-rich diet post-treatment. Maintain a healthy weight (BMI under 25), stay physically active with aerobic and resistance exercise, and avoid processed and red meats. These factors are most consistently linked to lower biochemical recurrence risk.
How to protect prostate after 60?
Prioritize plant proteins (legumes, tofu, tempeh) over animal products and follow an anti-inflammatory diet rich in vegetables and omega-3s. Maintain a healthy body weight, stay active with 150+ minutes of moderate exercise weekly, and get regular PSA screening as your physician recommends.
How to help husband with prostate cancer?
Cook plant-based, low-fat meals together and learn which adjustments support his specific treatment phase. Focus on making changes positive rather than restrictive—attending a nutrition consultation as a couple helps both partners understand the approach and stay consistent.


