
This article explores evidence-backed natural strategies as a complement, not a replacement, to conventional care. We'll examine anti-inflammatory dietary strategies, specific natural compounds studied in breast cancer research, the role of metabolic nutrition in targeting cancer cell vulnerabilities, and lifestyle practices that support recovery and quality of life.
TLDR
- IBC requires conventional tri-modality treatment; natural approaches complement, never substitute
- Anti-inflammatory diets and targeted phytochemicals have research support for reducing cancer-driving inflammation
- Methionine restriction targets a metabolic weakness unique to cancer cells
- Mind-body practices like meditation reduce stress hormones, supporting immune function during treatment
- Always consult your oncologist before introducing supplements or dietary changes
What Makes Inflammatory Breast Cancer Different—and Why Natural Support Matters
IBC's Unique Biology
Unlike most breast cancers, IBC does not typically present as a lump. Instead, cancer cells invade dermal lymphatics, causing the breast to appear red, swollen, and inflamed—often with a characteristic "peau d'orange" (orange peel) skin texture. According to the National Cancer Institute, IBC accounts for 1% to 5% of all breast cancer diagnoses in the United States.
Because of its rapid progression, IBC is always diagnosed at an advanced stage (Stage III or IV), with approximately 30% of patients presenting with metastatic disease at diagnosis.
Why IBC's Inflammatory Nature Makes Supportive Nutrition Relevant
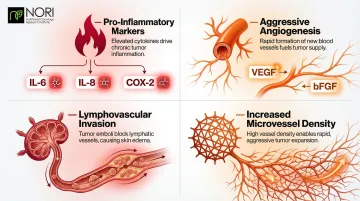
IBC tumors are characterized by:
- High expression of pro-inflammatory markers including IL-6, IL-8, and COX-2
- Aggressive angiogenesis driven by elevated VEGF, bFGF, and other growth factors
- Lymphovascular invasion with tumor emboli blocking dermal lymph vessels
- Increased microvessel density supporting rapid tumor growth
These biological characteristics give dietary and natural interventions a clear rationale: targeting tumor-promoting inflammation may help reduce the conditions IBC depends on to progress. Natural approaches do not replace neoadjuvant chemotherapy (pre-surgery chemo given to shrink tumors), but they can work alongside it by addressing the inflammatory processes driving IBC's aggressive behavior.
The Critical Importance of Conventional Treatment
That distinction matters, because the stakes of forgoing conventional treatment are serious. A 2018 study in the Journal of the National Cancer Institute found that breast cancer patients who refused conventional treatment in favor of alternative medicine alone faced a 5.68-fold increased risk of death compared to those receiving standard care.
The responsible path is integrative: use conventional treatment as the foundation, and layer in natural interventions that support it—not substitute for it.
Anti-Inflammatory Dietary Foundations for IBC Patients
IBC's defining feature is runaway inflammation—which makes an anti-inflammatory diet one of the most direct nutritional tools available. The goal is reducing oxidative stress and disrupting the pro-inflammatory signals that fuel cancer cell growth.
Dietary Patterns That Support Immune Function
The evidence for plant-rich eating is substantial. Long-term adherence to a low-fat, plant-rich diet significantly reduces breast cancer-specific mortality (HR 0.79, 95% CI 0.64–0.97) in the Women's Health Initiative Dietary Modification trial across a 19.6-year follow-up. Eating more than 5.5 servings of fruits and vegetables daily is associated with an 11% lower breast cancer incidence (HR 0.89, 95% CI 0.83–0.96).
Cruciferous vegetables—broccoli, cauliflower, Brussels sprouts, and cabbage—deserve particular attention. Their glucosinolates convert to active health-supporting compounds (sulforaphane, indole-3-carbinol) that laboratory models show can:
- Downregulate estrogen receptor activity
- Inhibit tumor cell migration
- Has been investigated for its effects on cellular stress pathways in breast cancer cell lines
- Suppress metastatic pathways
Consumption of cruciferous vegetables >5 servings/week is associated with an 8% reduction in breast cancer incidence.
Foods to Prioritize and Avoid
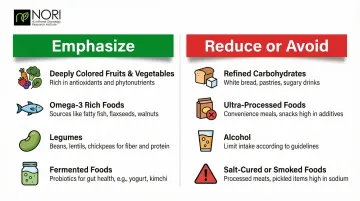
Foods to Emphasize:
- Deeply colored fruits and vegetables (berries, pomegranates, citrus) provide polyphenolic compounds with anti-inflammatory and antioxidant properties
- Omega-3 rich foods (fatty fish, walnuts, flaxseed) reduce inflammatory cytokines and support immune function
- Legumes offer fiber, plant protein, and compounds that modulate estrogen metabolism
- Fermented foods (kefir, sauerkraut, kimchi) support gut microbiome diversity, which influences immune response
Foods to Reduce or Avoid:
- High-glycemic refined carbohydrates activate mTOR and IGF-1 signaling pathways that promote cancer cell proliferation. High glycemic index diets are associated with a 5% increased breast cancer risk.
- Ultra-processed foods contain inflammatory compounds and lack protective nutrients
- Alcohol exhibits a linear dose-response relationship with breast cancer risk—every 10g/day increases risk by 10.5%
- Salt-cured, smoked, or pickled foods may contain carcinogenic compounds
Key Natural Compounds Studied for Breast Cancer Management
The following compounds have demonstrated wellness-supporting activity in laboratory studies for breast cancer. No compound has been proven to treat IBC independently, but the underlying mechanisms have measurable biological support and these agents are regularly incorporated into integrative oncology programs.
Curcumin
The active compound in turmeric, curcumin has demonstrated anti-inflammatory activity by inhibiting NF-κB signaling—a pathway particularly active in IBC tumors.
In breast cancer xenograft models, curcumin suppressed paclitaxel-induced NF-κB activation, downregulated metastatic proteins (VEGF, MMP-9), and significantly decreased the incidence of lung metastasis.
One practical limitation is bioavailability. Standard curcumin absorbs poorly on its own — co-administration with piperine (black pepper extract) increases bioavailability by 2000%, and phospholipid formulations demonstrate 29-fold higher absorption compared to standard preparations.
Sulforaphane and Indole-3-Carbinol
Johns Hopkins researchers identified broccoli sprouts as an exceptionally rich source of sulforaphane, and subsequent studies demonstrated measurable sulforaphane metabolites in human breast tissue following oral consumption.
Relevant mechanisms include:
- Downregulates estrogen receptor-alpha expression
- Has been investigated for its effects on cellular stress pathways through multiple mechanisms
- Inhibits metastatic activity via NF-κB suppression
- I3C significantly inhibits experimental breast cancer bone metastasis by downregulating the CXCR4/NF-κB pathway
Polyphenols: Resveratrol, Pomegranate Ellagitannins, and Quercetin
These three plant-derived polyphenols have been studied for complementary wellness-supporting mechanisms:
- Resveratrol (red grapes): Combined with quercetin and catechin, significantly reduced primary tumor growth in breast cancer xenografts
- Pomegranate ellagitannins: Urolithin B, a gut metabolite, effectively inhibits aromatase activity and suppresses testosterone-induced proliferation in breast cancer cells
- Quercetin: Inhibits the PI3K/AKT/mTOR signaling cascade, inducing approximately 70% inhibition of Akt phosphorylation in metastatic breast cancer cells at therapeutic concentrations
Medicinal Mushrooms
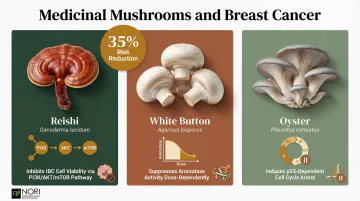
A meta-analysis found that higher mushroom consumption is associated with a 35% lower risk of breast cancer (pooled RR 0.65; 95% CI: 0.52, 0.81). Several specific species have been studied for mechanisms directly relevant to breast cancer, including IBC:
- Reishi (Ganoderma lucidum): Selectively inhibits IBC cell viability and invasion and reduced tumor growth in IBC animal models by modulating the PI3K/AKT/mTOR pathway
- White Button (Agaricus bisporus): Suppresses aromatase activity dose-dependently and inhibits proliferation of aromatase-transfected breast cancer cells
- Oyster (Pleurotus ostreatus): Suppresses breast cancer cell proliferation by inducing p53-dependent cell cycle arrest
Methionine Restriction: Targeting a Metabolic Vulnerability in Cancer Cells
The Hoffman Effect
Cancer cells exhibit an absolute dependence on exogenous methionine—a phenomenon known as methionine addiction or the "Hoffman Effect." Unlike normal cells, which can synthesize methionine from homocysteine, malignant cells lack this capacity and undergo cell cycle arrest and apoptosis when methionine is restricted.
The Dietary Mechanism
Methionine restriction involves reducing intake of high-methionine animal proteins while focusing on plant-based proteins naturally lower in methionine. Reducing animal protein in this way, without causing malnutrition, can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research. This creates a nutritional environment hostile to cancer cell replication, while normal cells tolerate the restriction well. The approach isn't something to improvise: it requires careful structuring by a knowledgeable nutritional practitioner to maintain adequate nutrition while achieving therapeutic methionine depletion.
Clinical Evidence and Application
Clinical research validates what the dietary approach is designed to achieve. A Phase I clinical trial demonstrated that methioninase safely depleted serum methionine (from 23.1 μM to 0.1 μM) without acute toxicity in advanced breast cancer patients. Additionally, methionine deprivation enhances TRAIL Receptor-2 expression in triple-negative breast cancer cells, sensitizing tumors to proapoptotic therapies.
Key findings from the research include:
- A Phase I trial showed methioninase safely reduced serum methionine from 23.1 μM to 0.1 μM in advanced breast cancer patients with no acute toxicity
- Methionine deprivation increases TRAIL Receptor-2 expression in triple-negative breast cancer cells, sensitizing tumors to proapoptotic therapies
NORI's Methionine Restriction Protocol
The Nutritional Oncology Research Institute has built its protocol on over 20 years of focused research into this approach, combining cycled methionine restriction with targeted nutraceutical formulations designed to exploit universal vulnerabilities in cancer cells.
The program is structured to work alongside conventional treatment and is available worldwide as a home-based system with professional guidance. Patients interested in exploring this approach can reach NORI for a free initial consultation at 800-634-3804.
Lifestyle Practices That Complement Natural Treatment for IBC
Physical Activity and Immune Support
Each 10 MET-hour/week increase in post-diagnosis physical activity is associated with 14% lower breast cancer-specific mortality (95% CI: 4%–23%) and 15% lower all-cause mortality. Moderate, regular exercise positively influences immune function and reduces inflammatory cytokines. Intensity should be adjusted to the patient's current treatment phase and functional capacity.
Stress Reduction and Mind-Body Practices
Chronic stress elevates cortisol, which suppresses immune function and promotes pro-inflammatory pathways. In a disease driven by dysregulated inflammation, managing stress is not optional — it's a core part of the protocol.
Evidence-Based Benefits:
- A 12-week Iyengar yoga intervention significantly reduced NF-κB activity and stabilized soluble TNF receptor levels in fatigued breast cancer survivors
- Mindfulness-Based Stress Reduction (MBSR) produced significant reductions in salivary cortisol and IL-6 in breast cancer survivors
- Thrice-weekly massage for 5 weeks reduced anxiety and increased Natural Killer cell and lymphocyte counts in breast cancer patients

Cortisol dysregulation from chronic stress also directly impairs sleep — which brings its own immune consequences.
Sleep Quality and Circadian Rhythm
Adequate sleep (7–9 hours) is essential for immune surveillance and hormonal balance. The International Agency for Research on Cancer classifies night shift work causing circadian disruption as a probable human carcinogen.
Practical Strategies:
- Maintain consistent sleep and wake times
- Limit light exposure (especially blue light) in the evening
- Reduce caffeine and stimulants after 2 PM
- Create a cool, dark sleep environment
Integrating Natural Approaches Safely: What IBC Patients Need to Know
Critical Safety Considerations
Some natural agents can interact with conventional IBC treatments. Strong antioxidants may interfere with certain chemotherapy mechanisms that rely on oxidative stress to kill cancer cells. Herbal supplements should never be taken during chemotherapy without oncologist guidance, as they may affect drug metabolism or efficacy.
Always disclose all supplement use to your oncology team. High-dose supplements can contain contaminants or create unexpected interactions with conventional medications.
Finding Qualified Integrative Support
IBC patients benefit most from working with practitioners who understand both oncology and nutritional medicine. IBC patients benefit most from working with practitioners who understand both oncology and nutritional medicine.
One example is NORI (Nutritional Oncology Research Institute), a non-profit research organization offering a home-based nutritional support program that combines methionine restriction with proprietary nutraceuticals formulated at their own facility. Free initial consultations are available to patients worldwide.
Whichever path you pursue, look for professionals who can customize approaches to your specific cancer subtype, staging, and treatment regimen. Integrative oncology consultations should address:
- Timing of supplements relative to chemotherapy
- Contraindications with current medications
- Monitoring protocols and biomarkers
- Adjustments based on treatment response
Frequently Asked Questions
How do you treat inflammatory breast cancer?
IBC is primarily treated with a multimodal conventional approach: neoadjuvant chemotherapy first, followed by surgery (usually mastectomy) and radiation therapy. Integrative strategies such as anti-inflammatory diet and evidence-based nutraceuticals may be used as supportive complements, always in coordination with an oncology team.
How rare is inflammatory breast cancer?
IBC accounts for 1% to 5% of all breast cancer diagnoses in the United States and is considered rare but disproportionately deadly due to its aggressive, locally advanced presentation at diagnosis. Because of this, patients benefit from seeking oncologists or NCI-designated centers with specific IBC experience.
Can natural remedies replace conventional treatment for IBC?
No. Natural remedies alone are not a reliable substitute for conventional IBC treatment — patients who forgo standard therapy face significantly elevated mortality risk. Natural approaches are best used as complements to oncology care, not replacements for it.
What dietary changes can help inflammatory breast cancer patients?
An anti-inflammatory, plant-rich diet is the pattern most supported by research for IBC patients. Key priorities include:
- Cruciferous vegetables and polyphenol-rich fruits
- Omega-3 sources (fatty fish, flaxseed, walnuts)
- Reduced refined carbohydrates and added sugars
A nutritional professional experienced in oncology can help personalize this approach.
Is curcumin effective for inflammatory breast cancer?
Curcumin has shown promising anti-inflammatory and wellness-supporting activity in cell and animal studies, but clinical evidence in IBC specifically is limited. It is generally considered safe as a complementary supplement but should be discussed with an oncologist, particularly regarding timing with chemotherapy.
What makes inflammatory breast cancer different from other breast cancers?
Unlike most breast cancers, IBC typically presents without a palpable lump and instead causes rapid breast swelling, redness, and skin changes (peau d'orange) due to cancer cells blocking lymphatic vessels. It is nearly always locally advanced at diagnosis and requires immediate aggressive treatment.


