
Introduction
A kidney cancer diagnosis forces fast decisions — and many patients don't want to limit those decisions to what their oncologist recommends. More than half of metastatic renal cell carcinoma (RCC) patients start using supplements or natural therapies after diagnosis, according to published survey data. The desire for options beyond surgery, targeted therapy, and immunotherapy is real, and the research has begun to catch up.
This guide covers the natural compounds, dietary strategies, and mind-body approaches being studied and used by kidney cancer patients today.
One distinction is worth drawing early: complementary therapies used alongside standard care show meaningful promise in lab studies and quality-of-life outcomes. Alternative approaches used instead of conventional treatment lack the same clinical backing and can delay proven care. Both categories appear here — with that context clearly noted.
What follows is a practical look at what the evidence actually shows — and what it doesn't — so you can make informed decisions about your care.
TLDR
- Alternative therapies used instead of conventional care lack clinical proof and may delay effective treatment
- Complementary approaches such as dietary changes, natural compounds, and mind-body practices can provide meaningful support alongside standard care
- Lab studies demonstrate health-supporting effects for curcumin, EGCG, resveratrol, and quercetin, but human trials for kidney cancer are limited
- A shift toward plant-based whole foods and away from red meat and processed foods may support treatment outcomes
- Always discuss any supplements or dietary changes with your oncologist, as some can interfere with targeted therapies or immunotherapy
Alternative vs. Complementary: Understanding the Key Difference
The National Cancer Institute defines alternative medicine as treatments used instead of standard medical care, while complementary medicine refers to approaches used alongside conventional treatments. This distinction carries significant consequences for kidney cancer patients.
Alternative therapies—when chosen as sole treatments—typically lack strong scientific evidence of efficacy against RCC and carry serious risks if they delay proven interventions like surgery, targeted therapy, or immunotherapy. Time spent without effective treatment allows aggressive forms of kidney cancer to progress, potentially moving from curable to advanced stages.
Integrative oncology represents a third category — care that combines conventional treatment with complementary practices shown to be safe and supportive. Major cancer centers now operate formal integrative medicine programs that typically include:
- Acupuncture for pain and nausea management
- Nutrition counseling to support treatment tolerance
- Mind-body therapies such as meditation and guided imagery
- Supplement and herb guidance to avoid drug interactions
Kidney cancer patients seek non-traditional options for understandable reasons: desire for greater control over treatment decisions, concerns about side effects from targeted therapies or immunotherapy, and hope for approaches addressing overall wellbeing rather than just tumor burden. These motivations are valid — and the best outcomes tend to come from exploring the full range of evidence-based options, both conventional and nutritional, with a clear understanding of what each approach offers.
Natural Compounds and Supplements Studied for Kidney Cancer
Growing preclinical research has identified natural compounds showing health-supporting activity against renal cell carcinoma in laboratory and animal models. A 2022 review in Nutrients examined over 30 natural products with reported anti-RCC effects, though human clinical trials remain absent for most.
Cellular Stress Pathway Compounds
Several natural substances demonstrate the ability to affect cellular health pathways, as investigated in nutritional oncology research, in kidney cancer models:
- Curcumin (from turmeric): Has been investigated for its effects on cellular stress pathways in RCC cells by suppressing the Akt/mTOR pathway, a signaling network kidney cancer cells rely on for growth and survival
- EGCG (epigallocatechin-3-gallate from green tea): Has been investigated for its effects on cellular health in RCC cells, including downregulation of MMP-2 and MMP-9, proteins involved in cancer cell migration
- Quercetin (found in apples, onions, and grapes): Targets Akt/mTOR/ERK pathways in kidney cancer cell lines, particularly when combined with other interventions
- Resveratrol (from grapes and berries): Shows synergistic effects with sorafenib (a targeted therapy for advanced RCC) by inhibiting Akt/mTOR and c-Raf/MEK/ERK signaling in both lab studies and mouse models

Additional compounds studied for anti-metastatic effects include:
- Honokiol (magnolia bark extract): Blocks epithelial-mesenchymal transition (EMT) and cancer stem cell properties
- Sulforaphane (from broccoli and cruciferous vegetables): Disrupts cancer cell energy pathways and reduces proliferation
- Thymoquinone (black cumin seed): Suppresses metastasis-related proteins and affects cellular health processes being investigated in nutritional oncology research via AMPK/mTOR signaling
While these compounds are available as dietary supplements, quality and dosing standards vary widely across manufacturers, and recommended doses from lab studies don't translate directly to human supplementation.
Anti-Angiogenic Natural Products
Clear cell RCC—the most common kidney cancer subtype—depends heavily on blood vessel formation (angiogenesis) due to VHL gene mutations that activate VEGF signaling. Several natural compounds target this vulnerability:
- Genistein (from soy): Inhibits VEGF and bFGF expression in human RCC cell lines
- Ganoderma lucidum (reishi mushroom): Suppresses VEGF overexpression and tumor angiogenesis in animal models
- Cinnamon polyphenols: Block VEGFR2 kinase activity and suppress HIF-1α gene expression
Drug Sensitization: Natural Compounds as Adjuncts
Emerging research explores using natural products to enhance conventional treatment effectiveness:
- Kahweol acetate (from coffee beans): Enhanced sorafenib sensitivity in kidney cancer cells by down-regulating anti-apoptotic proteins Mcl-1 and c-FLIP
- Korean red ginseng extract: Improved sorafenib's health-supporting effects in RCC by blocking CREB and c-Jun activation in both lab and animal studies
- Lycium barbarum polysaccharides (wolfberry/goji berry): Synergized with interferon-α2b in mouse RCC models by reducing myeloid-derived suppressor cells
For patients and oncologists alike, the key takeaway is that natural products show the most promise as complements to targeted therapy or immunotherapy, not substitutes for them.
Safety Note
High-dose supplements can interact with targeted therapies or immunotherapy. Some antioxidants may reduce treatment effectiveness by protecting cancer cells from oxidative damage that certain therapies deliberately induce. Share all supplement use with your oncologist before starting.
Dietary Approaches That May Support Kidney Cancer Treatment
While no specific diet has been proven to cure RCC, dietary choices influence inflammation, immune function, metabolic environment, and treatment tolerability. For kidney cancer patients, diet is one of the most practical and accessible areas where evidence-backed changes can make a real difference.
Plant-Based and Anti-Inflammatory Diet
The NIH-AARP Diet and Health Study—following 492,186 participants—found that red meat intake showed a tendency toward increased RCC risk and a 2-fold increased risk of papillary RCC. Particularly concerning: benzo(a)pyrene (BaP) from high-temperature cooking methods like grilling and barbecuing increased RCC risk by 50%, with a doubling of papillary RCC risk.
On the protective side, high dietary fiber intake was associated with a 15-20% lower RCC risk in the highest consumption groups. Legumes, whole grains, and cruciferous vegetables correlated with 16-18% reduced risk. A pooled analysis of nine prospective studies found vegetarian and pescatarian diets associated with 28% and 27% lower kidney cancer risk, respectively, compared to meat eaters.
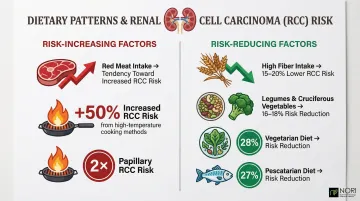
Practical application: Emphasize whole plant foods—fruits, vegetables, legumes, whole grains—while limiting or avoiding charred meats, processed meats, and high-temperature cooked animal proteins.
Methionine Restriction: A Targeted Nutritional Strategy
Cancer cells exhibit dependence on the amino acid methionine for growth and proliferation—a phenomenon called the Hoffman effect. When methionine is replaced with homocysteine, cancer cells cannot proliferate, while normal cells continue functioning normally.
Dietary methionine restriction may selectively starve cancer cells while remaining tolerable for healthy tissues. Methionine is concentrated in animal proteins, making plant-based diets naturally lower in this amino acid.
Reducing animal protein intake without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research — the core rationale underpinning methionine restriction protocols. NORI (Nutritional Oncology Research Institute) has developed a structured protocol around this principle, combining cycled methionine restriction with pro-oxidant nutraceutical combinations being studied in nutritional oncology research. Key parameters include:
- Cycle schedule: 7 days restriction, 7 days off
- Protein targets: Below 0.3 g/kg of body weight during restriction phases, emphasizing plant-based sources low in methionine
- Methionine/cysteine limit: No more than 10 mg/kg daily during active restriction
- Delivery: Entirely home-based, with support via phone and Zoom—no clinic visits required
Patients interested in a structured nutritional intervention beyond general dietary advice can reach NORI at 800-634-3804 or info@nutritionaloncology.net for a free initial consultation.
Fasting and Caloric Restriction
Short-term fasting may create metabolic conditions—lower IGF-1, reduced glucose availability—that make cancer cells more vulnerable to treatment while protecting normal cells. A 2018 review discussed molecular mechanisms and clinical applications of fasting in cancer care, while a 2021 systematic review noted that while the concept shows promise, high-quality human trials remain limited.
RCC-specific clinical data for fasting-mimicking diets is lacking, making this an experimental approach best discussed with your care team.
Foods and Substances to Avoid
Kidney cancer patients should minimize or avoid:
- Processed meats and high red meat intake (especially grilled or barbecued)
- High-salt and high-phosphorus foods (stress compromised kidney function)
- Excess supplemental antioxidants during active chemotherapy or radiation (may interfere with treatment)
- Unpasteurized foods during immunosuppression
- Alcohol and tobacco
Work with a registered dietitian familiar with oncology nutrition to personalize these recommendations based on your kidney function, treatment protocol, and individual circumstances.
Mind-Body and Lifestyle Therapies
Mind-body practices rank among the most well-supported complementary approaches in integrative oncology. They don't target tumors directly, but reliably reduce treatment-related stress, anxiety, fatigue, and pain—major quality-of-life concerns for kidney cancer patients.
Three approaches have the strongest evidence backing:
- Mindfulness-based interventions — strongly recommended by the 2023 Society for Integrative Oncology-ASCO guidelines for anxiety during and after treatment
- Yoga — earns similar SIO-ASCO recommendations for anxiety and cancer-related fatigue
- Acupuncture — recognized by NCCN guidelines for fatigue, nausea, and pain management
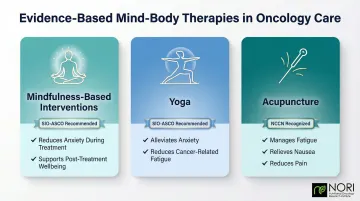
All three are generally safe when performed by qualified practitioners, can be practiced at home, and don't interfere with conventional treatments. That combination makes them practical additions to most care plans.
Critical safety note: If you have bone metastases or suspect spinal involvement, avoid high-force spinal or chiropractic manipulation. Approximately 40% of cancer patients develop spinal metastases, creating real fracture risk. Discuss any physical therapy with your oncologist before starting.
Exercise and Physical Activity
Moderate exercise during active treatment improves fatigue, mood, and immune function — and may lower recurrence risk. ASCO guidelines strongly recommend both aerobic and resistance exercise during treatment to reduce side effects and preserve physical function.
A 2026 case series of 19 metastatic RCC patients on immunotherapy (with or without TKIs) found a 12-week remote exercise program significantly improved health-related quality of life and reduced fatigue. Ask your oncologist or a certified oncology exercise specialist to help you build a plan matched to your current treatment and fitness level.
Risks and Precautions When Exploring Alternative Options
The most significant risk of alternative treatments is delaying or forgoing proven conventional therapy. Integrative approaches can meaningfully support wellbeing, but none have been shown to shrink kidney tumors or cure RCC. In aggressive forms, time without effective treatment directly allows cancer to advance.
Specific Safety Risks
Herb-drug interactions pose serious concerns:
- St. John's Wort induces CYP3A4 enzymes, reducing plasma levels of targeted therapies like imatinib by approximately 30%, potentially leading to treatment failure
- Grapefruit juice inhibits CYP3A4, increasing plasma concentrations of RCC TKIs like sunitinib and pazopanib, raising toxicity risk
Supplement quality issues include contamination, inaccurate dosing, and adulteration with unapproved pharmaceutical ingredients in unregulated markets.
Antioxidant interference: High-dose antioxidant supplements may reduce effectiveness of radiation therapy or certain targeted agents that work by creating oxidative stress in cancer cells.
Given these risks, disclose every supplement and herb to your full oncology team — not just your primary oncologist. Pharmacists can run comprehensive interaction reviews that may prevent life-threatening complications.
Natural ≠ Safe or Effective
Many substances marketed as cancer treatments have not been proven effective and may cause direct harm. Laetrile (amygdalin/Vitamin B-17) has shown no health-supporting activity in human trials and releases toxic hydrogen cyanide — causing liver damage, coma, and potentially death. The FDA actively issues warnings against it and other fraudulent cancer cure claims.
Before pursuing any unproven remedy, check NCI's guidance on unproven treatments or Quackwatch. Both resources give patients a concrete way to evaluate claims before acting on them.
Building an Integrative Kidney Cancer Support Plan
A personalized integrative oncology plan pairs conventional treatment — targeted therapy, immunotherapy, or surgery — with evidence-informed complementary approaches. The right mix depends on your cancer stage, treatment protocol, existing health conditions, and personal goals. For kidney cancer patients especially, where systemic therapies like TKIs and checkpoint inhibitors carry significant side effects, integrative support can meaningfully improve day-to-day quality of life.
Practical Framework
Step 1: Inform your full care team about any supplements, herbs, or dietary changes you're considering. This includes oncologists, surgeons, pharmacists, and any integrative practitioners.
Step 2: Prioritize interventions with the strongest safety and evidence profile. Start with diet modifications, mind-body practices, and exercise—approaches with documented benefits and minimal interference risk.
Step 3: Approach higher-risk interventions like herbs and high-dose supplements only with explicit clearance from your oncologist. Provide brand names, dosages, and ingredient lists for review.
Step 4: Track how you feel and report changes to your care team regularly. Keep a simple log of symptoms, energy levels, and quality of life markers.

Structured Nutritional Support Programs
For patients seeking science-based nutritional support beyond standard care—particularly those with limited conventional options—organizations like NORI (Nutritional Oncology Research Institute) offer home-based programs built on over 20 years of research.
NORI's approach targets cancer cell vulnerabilities through cycled methionine restriction and proprietary nutraceutical combinations designed to target metabolic dependencies unique to cancer cells. The program is:
- Entirely home-based with no clinic visits required
- Delivered via phone and Zoom consultations with unlimited support
- Affordable with flat-fee pricing (monthly, yearly, or lifetime options)
- Accessible worldwide
NORI formulates and manufactures all nutraceuticals at their facility with guaranteed potency and purity. Initial consultations are free (800-634-3804 or info@nutritionaloncology.net).
While NORI's published case reports document significant outcomes for thyroid, breast, prostate, and blood cancers, kidney cancer-specific outcomes are not detailed in public documentation. Contact NORI directly to discuss whether their protocol has been applied to RCC patients and what results have been observed.
Integration, Not Replacement
Most patients use conventional and integrative approaches together — not as competing options. Targeted therapies and immunotherapy address tumor burden directly, while nutritional and lifestyle support works alongside them. The combined approach can help:
- Maintain immune function during active treatment
- Reduce treatment-related fatigue and side effects
- Support metabolic health and reduce systemic inflammation
- Lower long-term recurrence risk through sustained lifestyle changes
Neither approach has to come at the expense of the other.
Frequently Asked Questions
What is the most effective treatment for kidney cancer?
Standard treatment depends on stage and type. Localized kidney cancer is typically treated with surgery (partial or radical nephrectomy) or thermal ablation. Advanced or metastatic RCC is managed with targeted therapies (TKIs like sunitinib or cabozantinib), immunotherapy (checkpoint inhibitors), or combination regimens. Complementary approaches support but cannot replace these treatments.
Can advanced kidney cancer be cured?
Advanced (stage 3-4) or metastatic kidney cancer is generally not curable with current treatments but can often be managed long-term with systemic therapies. Some patients achieve prolonged stable disease or partial remission, and integrative nutritional support can help maintain treatment tolerance and quality of life throughout that process.
What helps fight kidney cancer?
Conventional approaches include targeted therapy and immunotherapy. Supportive approaches include a plant-rich anti-inflammatory diet, natural compounds studied for RCC (curcumin, EGCG, quercetin), mind-body practices supporting immune function, and structured nutritional protocols that target how cancer cells process nutrients.
How to keep kidney cancer from coming back?
Regular surveillance imaging as recommended by your care team is essential. Maintain a healthy weight, adopt an anti-inflammatory plant-based diet, avoid tobacco and excessive alcohol, stay physically active, and discuss nutritional support protocols with an integrative oncologist or qualified nutritional oncology specialist.
Is kidney cancer slow growing?
Growth rate varies widely by type and stage. Many early-stage tumors discovered incidentally grow slowly, which is why active surveillance is sometimes appropriate. However, some subtypes — including sarcomatoid RCC and collecting duct carcinoma — can be highly aggressive, so never assume a slow trajectory without imaging-confirmed data from your care team.
What to avoid if you have kidney cancer?
Key things to limit or avoid:
- High red meat and processed meat intake
- Excess salt and phosphorus, which stress compromised kidneys
- Tobacco and alcohol
- High-dose supplements without oncologist clearance (drug interaction risk)
- Unproven alternative therapies that could delay effective treatment
Disclaimer: This guide provides educational information and should not replace professional medical advice. Always consult with your oncology team before starting any complementary therapy, supplement, or dietary change.


