
Introduction
Liver cancer is one of the hardest diagnoses to face. The five-year survival rate in the United States sits at just 22.0%, fewer than 30% of patients qualify for curative surgery at diagnosis, and for those who do undergo resection, recurrence reaches 50–70% within five years.
That leaves most patients looking for every available tool — and peer-reviewed research increasingly shows that diet, herbal compounds, and nutritional strategies belong in that conversation.
Evidence points to specific compounds that suppress tumor growth, protect liver function, and strengthen the effects of conventional therapies — with far fewer toxic side effects than drugs alone.
This article covers food-based compounds, evidence-backed supplements, dietary strategies, and lifestyle factors showing real promise for liver cancer prevention and support, along with how to safely integrate them into a care plan.
Why Conventional Treatments Fall Short for Many Liver Cancer Patients
Standard-of-care options for liver cancer include surgical resection, liver transplantation, targeted therapy (sorafenib), transarterial chemoembolization (TACE), and radiation. Yet many patients either cannot tolerate or do not respond adequately to these treatments, largely because of:
- Late-stage diagnosis, which rules out curative surgery in most cases
- Pre-existing liver dysfunction that limits tolerable treatment doses
- High recurrence rates even after successful initial intervention
The chemotherapy challenge is especially acute here: because the liver metabolizes toxins, systemic treatment hits the organ hardest. Sorafenib, the most prescribed drug for advanced hepatocellular carcinoma, extended median overall survival to 10.7 months versus 7.9 months for placebo in the SHARP trial.
The objective response rate, however, was only 2%—just 7 out of 299 patients achieved a partial response, and zero achieved complete response. Resistance develops quickly, leaving most patients with limited next steps.
These gaps are precisely where integrative and nutritional oncology has drawn serious scientific attention. Targeting cancer cell vulnerabilities through diet and natural agents is not a fringe idea—multiple peer-reviewed studies support the agents discussed throughout this article.
Food-Based Natural Compounds That Show Promise Against Liver Cancer
Epidemiological research consistently links high vegetable and plant-based food consumption with reduced liver cancer risk. A 2019 meta-analysis of nine prospective cohort studies covering 1,326,176 participants found that higher vegetable intake correlates with a 39% reduction in liver cancer risk — roughly 4% per additional 100g/day. Notably, high fruit intake alone was not significantly associated with reduced HCC risk.
Fruits and Polyphenol-Rich Foods
Grapes, pomegranate, and black currant have demonstrated wellness-supporting effects in laboratory and animal models of hepatocellular carcinoma:
- Grapes (procyanidins): Grape seed proanthocyanidins have been investigated for their effects on cellular stress pathways in HepG2 cells, including effects on tumor growth through survivin modulation
- Pomegranate (polyphenols): Punicalagin suppresses NF-κB-p65 and downregulates miR-21 in rat hepatocarcinogenesis models
- Black currant (anthocyanins): Have been investigated for their effects on cellular stress pathways while sparing healthy cells

Each of these fruits affects cellular health pathways in liver cancer models through distinct but complementary mechanisms — reducing oxidative stress, blocking inflammatory signaling, and affecting cellular processes being investigated in research selectively in tumor tissue.
Cruciferous and Anti-Carcinogenic Vegetables
Cruciferous vegetables show the ability to upregulate Phase II detoxification enzymes in the liver:
- Broccoli (sulforaphane): Inhibits TGF-β-induced epithelial-mesenchymal transition, suppresses STAT3/HIF-1α/VEGF angiogenesis, and blocks cancer cell invasion
- Radish (glucoraphasatin/isothiocyanates): Induces quinone reductase and Phase II detoxification enzymes in HepG2 cells
- Asparagus (asparanin A): Has been investigated for its effects on cellular stress pathways including G2/M cell cycle arrest in hepatocellular carcinoma
These vegetables are relevant for both prevention (detoxifying chemical carcinogens like aflatoxin B1) and therapeutic support.
Spices with Anti-Hepatoma Properties
Three culinary spices are backed by preclinical research:
- Turmeric/curcumin: Shows wellness-supporting activity against chemically induced liver cancer development, has been investigated for its effects on cellular stress pathways, and offers potential protection against HBV-related HCC. A 2024 clinical pilot study found curcumin enhanced the efficacy of TACE therapy in intermediate-stage HCC patients
- Garlic: Organo-sulphur compounds inhibit DNA damage from aflatoxin and other carcinogens, suppress cancer cell invasion and migration, and enhance NK cell activity
- Ginger: 6-shogaol and 6-gingerol suppress liver cancer metastasis through MMP-2/-9 downregulation and reduce serum cancer markers
Most evidence is preclinical and should not be overstated.
Edible Mushrooms and Immune-Modulating Polysaccharides
Edible fungi contain beta-glucans and polysaccharides that have demonstrated measurable effects:
- Agaricus blazei, shiitake, and Pleurotus species contain compounds that have been investigated for their effects on cellular stress pathways in hepatoma cells via the EGR1/PTEN/AKT axis
- Decrease abnormal collagen fiber formation (relevant to liver cirrhosis)
- Enhance immune function including NK cell activity
- Show synergistic potential when combined with chemotherapy by sensitizing cancer cells and reducing drug resistance
Across all four food categories above, the pattern is consistent: whole food compounds and their active constituents affect liver cancer biology through multiple simultaneous pathways. That multi-target activity is what makes them worth considering alongside — not instead of — a structured nutritional protocol.
Herbal Supplements and Their Evidence for Liver Cancer Support
Beyond dietary food sources, several botanical compounds are widely used in supplement form for liver cancer support. Supplement quality varies widely, doses differ significantly from dietary intake, and interactions with cancer medications are possible — always consult a healthcare provider before starting any supplement.
Milk Thistle (Silymarin/Silibinin)
Silymarin has generated more peer-reviewed liver research than most botanical compounds. It has demonstrated hepatoprotective effects, anti-invasion and anti-metastasis properties in MHCC97 hepatoma cells, and suppression of VEGF/MMP-9 expression (proteins that promote tumor growth and spread). Some trials have also examined silymarin's ability to reduce liver toxicity caused by chemotherapy.
Important limitation: A Phase I dose-finding study of silybin phosphatidylcholine in advanced HCC patients failed to establish a maximum tolerated dose because all participants died within 23 to 69 days, likely from hepatic failure related to their advanced disease. More large-scale clinical trials are needed.
Green Tea Extract (EGCG)
Epigallocatechin gallate (EGCG) from green tea shows promise:
- Synergistic wellness-supporting effects when combined with doxorubicin by inhibiting protective autophagy
- Suppresses angiogenesis through MAPK/ERK and PI3K/AKT/HIF-1α/VEGF pathways
- Reverses drug resistance in chemoresistant liver cancer cells by suppressing P-glycoprotein efflux pumps
Critical warning: High-dose green tea extract supplements can paradoxically cause liver injury. EFSA and LiverTox warn that EGCG doses exceeding 800 mg/day can cause idiosyncratic, clinically apparent acute liver injury. Moderation and clinical guidance are essential.
Resveratrol
Resveratrol (found naturally in grapes and berries) is a polyphenolic compound that:
- Inhibits liver cancer cell invasion and migration through the miR-186-5p/EMT pathway
- Has been investigated for its effects on cellular stress pathways
- Shows synergistic cytotoxicity with paclitaxel
Dietary sources like moderate red wine and fresh grapes differ substantially from high-dose supplements. In practice, oral resveratrol supplements are rapidly metabolized, meaning tissue exposure may be far lower than the administered dose — a key reason clinical results have been inconsistent and why dosing should be guided by a clinician.
Berberine
Berberine—derived from plants like Coptis and widely used in Traditional Chinese Medicine—demonstrates multiple anti-liver cancer mechanisms:
- Being investigated for their effects on cellular stress pathways in HepG2 cells
- Inhibiting epithelial-mesenchymal transition via TGF-β/Smad pathway suppression
- Downregulating CD147
- Showing synergistic effects when combined with vincristine
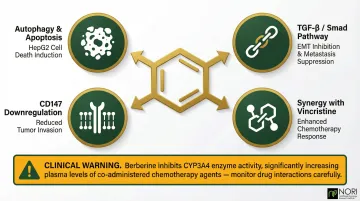
Berberine is a potent CYP3A4 inhibitor, meaning it can raise blood levels of drugs metabolized by that enzyme — including several chemotherapy agents and immunosuppressants. Clinical supervision is essential before combining berberine with any prescription medication.
Nutritional Strategies: Diet Patterns and Metabolic Approaches for Liver Cancer
What you eat shapes your liver cancer risk more than most people realize. A diet high in refined carbohydrates, processed foods, and alcohol drives non-alcoholic fatty liver disease (NAFLD) and cirrhosis—both primary risk factors for hepatocellular carcinoma. A meta-analysis of 13,371 subjects revealed that 37% of NAFLD-associated HCC cases presented without cirrhosis at diagnosis.
Targeting Cancer Cell Metabolism Through Diet
Liver cancer cells have a unique dependency on the amino acid methionine to proliferate—distinct from healthy liver cells. This metabolic vulnerability creates an opportunity for nutritional intervention.
Cycled methionine restriction—deliberately limiting methionine-rich foods such as red meat, processed meats, and full-fat dairy for strategic periods—may selectively stress cancer cells while normal cells adapt. Preclinical research shows acute methionine deprivation induces irreversible cell cycle arrest and profound DNA damage in human liver cancer cells.
This principle is central to the NORI Protocol, which pairs cycled methionine restriction with targeted nutraceuticals designed to exploit cancer cells' metabolic vulnerabilities. For patients interested in applying this approach alongside their current treatment plan, NORI offers free initial consultations at 800-634-3804.
Mediterranean and Plant-Forward Dietary Patterns
The Mediterranean diet offers a practical, evidence-aligned framework for liver cancer risk reduction:
- High in polyphenol-rich fruits and vegetables, olive oil, legumes, whole grains, and fish
- Low in ultra-processed foods, red meat, and alcohol
- Reduces HCC risk significantly (pooled HR 0.65; 95% CI: 0.56–0.75)
This pattern reduces chronic inflammation, oxidative stress, and insulin resistance—three interlocking drivers of hepatocarcinogenesis.
Gut Microbiome Health and the Gut-Liver Axis
A diverse, healthy microbiome reduces endotoxin (lipopolysaccharide) exposure to the liver, decreases liver inflammation, and may lower hepatocarcinogenesis risk. Dysbiosis promotes HCC by disrupting the intestinal barrier and facilitating LPS translocation, which binds to TLR4 receptors and activates pro-cancer signaling.
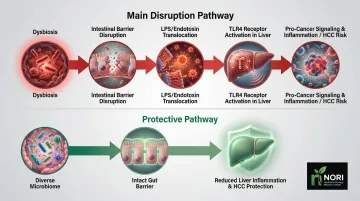
Microbiome-supporting foods to prioritize:
- Prebiotic vegetables (artichokes, asparagus, onions, garlic)
- Fermented foods (kimchi, sauerkraut, yogurt)
- Minimizing unnecessary antibiotic use, which can significantly disrupt gut flora and liver-protective microbiome diversity
Lifestyle Factors for Liver Cancer Prevention
Several modifiable lifestyle factors have meaningful, evidence-backed effects on liver cancer risk. Each of the areas below targets a distinct biological pathway — from viral immunity to toxin clearance.
Alcohol Reduction
Alcohol is a direct hepatotoxin and carcinogen. In 2020, an estimated 154,700 liver cancer cases globally were attributable to alcohol consumption. Alcohol contributes to approximately 26% of HCC cases worldwide.
Hepatitis B/C Vaccination and Screening
HBV and HCV infection are the leading global risk factors for HCC. Globally, 56% of liver cancer cases are attributable to HBV and 20% to HCV. Nutritional immune support can reinforce the body's antiviral defenses alongside vaccination and screening. Key factors include:
- Consistent quality sleep (7–9 hours)
- Stress reduction practices
- Adequate zinc and vitamin D intake
Maintaining Healthy Body Weight
Obesity and NAFLD are rising causes of liver cancer. Exercise, caloric balance, and avoiding sugar-sweetened beverages each reduce NAFLD-related liver cancer risk. A meta-analysis of 14 prospective studies found high versus low physical activity reduces liver cancer risk by 25%.
Reducing Aflatoxin Exposure
Aflatoxin—a fungal toxin found in improperly stored grains and nuts—is a recognized driver of HCC. The population attributable risk is 17% overall and 23% in high-risk areas. Cruciferous vegetables, garlic, and rosemary actively upregulate Phase II liver detoxification enzymes that neutralize these carcinogens.
Stress Reduction, Sleep, and Physical Activity
Chronic stress and sleep disruption elevate cortisol and suppress NK cell activity—a key natural wellness-supporting defense. Even modest movement matters: brisk walking for over 1 hour/week was associated with 50% lower HCC risk.
How to Use Natural Approaches Safely Alongside Medical Treatment
Natural approaches work best within a medically supervised, integrative plan. They should complement conventional care, not replace it. Some natural compounds—antioxidants in particular—can interfere with chemotherapy and radiation at high doses during active treatment. Always disclose all supplements to your oncologist before starting anything new.
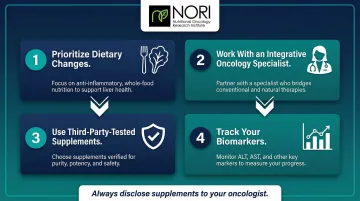
Practical framework for getting started:
- Prioritize dietary changes first (low risk, high reward)
- Work with an integrative oncology practitioner or nutritional oncology specialist to identify appropriate supplements based on individual health status, medications, and cancer stage
- Use reputable, third-party-tested supplements to avoid contamination
- Track changes in biomarkers (liver enzymes, alpha-fetoprotein, imaging) to assess response
Finding qualified guidance is often the hardest step. NORI (Nutritional Oncology Research Institute) offers a home-based nutritional support program built around structured, evidence-informed protocols with continuous one-on-one guidance—no clinic visits required. Patients worldwide use the program to access personalized nutritional oncology support alongside their existing care. Call 800-634-3804 for a free consultation to explore how a nutritional approach may fit your current treatment plan.
Frequently Asked Questions
What natural treatments or supplements can help with liver cancer?
The most evidence-backed options include curcumin, silymarin (milk thistle), garlic compounds, EGCG (green tea), berberine, and mushroom polysaccharides. These are supportive agents used alongside—not instead of—medical treatment. Consult your doctor before starting any supplement.
Can liver cancer be treated without chemotherapy?
Some liver cancers are managed without systemic chemotherapy through surgery, ablation, or targeted therapy. For patients who cannot tolerate or no longer respond to conventional drugs, integrative nutritional strategies are being studied as adjuncts. Treatment decisions should always involve an oncologist familiar with your case.
Can stage 4 liver cancer go into remission?
Stage 4 liver cancer remission is rare but has been documented in case reports, particularly with aggressive multimodal integrative approaches. Response rates vary widely depending on tumor burden, liver function, and treatment combination. Nutritional and integrative support may improve quality of life and, in some cases, complement medical therapy.
What are the chances of liver cancer returning?
Recurrence rates after liver cancer care are high—50–70% of patients experience recurrence within five years post-surgery. Ongoing dietary strategies, antiviral management (for HBV/HCV patients), and integrative support are important for reducing recurrence risk.
Can liver damage from chemo be reversed?
Chemotherapy-induced liver damage can sometimes partially improve after treatment ends. Hepatoprotective agents like silymarin have been studied to reduce chemo-related liver toxicity, though results vary and study sizes remain small. Check with your oncologist before adding any supplement during active treatment.
Can you survive liver cancer?
Survival depends heavily on stage at diagnosis and liver function. Early-stage liver cancer carries relatively good outcomes with surgery or ablation (37.6% five-year survival for localized disease), while advanced-stage survival remains challenging (3.5% for distant disease). Nutritional and integrative approaches may support quality of life and, for some patients, complement conventional treatment.


