Introduction
If you've been diagnosed with kidney cancer, you've likely encountered conflicting dietary advice. Some patients fear all protein, believing it harms the kidneys. Others eliminate entire food groups unnecessarily, unsure what truly helps or hurts their recovery. The confusion is understandable, but here's what matters: while there's no single "kidney cancer diet," research consistently shows that what you eat significantly influences both cancer risk and treatment outcomes.
Diet for kidney cancer patients serves two distinct goals: supporting kidney function that may be compromised by cancer or treatment, and creating an internal environment less hospitable to cancer cell growth. Both goals are achievable — but only when dietary choices are grounded in evidence, not anxiety.
What follows are evidence-backed strategies for what to eat, what to limit, and how nutritional support can work alongside your treatment plan.
TLDR
- Plant-rich diets emphasizing cruciferous vegetables, berries, and whole grains reduce kidney cancer risk by 27-29% and improve treatment outcomes
- Limit or avoid red/processed meats, high-sodium processed foods, alcohol, and sugary beverages
- Potassium and phosphorus restrictions should be based on individual lab values, not assumed for all patients
- During active treatment, managing appetite, muscle mass, and immune function takes priority over general dietary rules
- Working with a nutritional oncology specialist produces better results than following any one-size-fits-all food list
How Diet Influences Kidney Cancer Risk and Recovery
The connection between diet and renal cell carcinoma (RCC) runs deeper than most patients realize. Chronic inflammation, oxidative stress, obesity, and insulin resistance all drive kidney cancer development—and all respond directly to dietary changes.
Research from the UK Biobank cohort shows that high adherence to healthy dietary patterns (DASH and Mediterranean diets) reduces RCC risk by 29–33%, while pro-inflammatory dietary patterns increase risk by 45%. Your daily food choices create systemic conditions that either support or suppress tumor growth.
The CKD Diet vs. Cancer Nutrition Confusion
Acting on that evidence requires clarity about which dietary framework applies — and many patients, along with some providers, conflate chronic kidney disease (CKD) renal diets with kidney cancer nutrition. They serve different goals:
| CKD Diet | Cancer Nutrition | |
|---|---|---|
| Primary goal | Protect failing kidney function | Reduce inflammation, support treatment |
| Protein target | 0.8 g/kg/day | 1.0–1.5 g/kg/day |
| Key concern | Mineral restriction | Muscle wasting and cachexia |
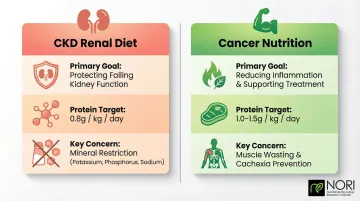
Care teams should pivot to oncology protein targets during active treatment, adjusting only if dialysis becomes necessary.
Why Malnutrition Affects Up to 80% of Patients During Treatment
An estimated 50–80% of kidney cancer patients undergoing treatment aren't getting adequate nutrition due to poor appetite, nausea, or malabsorption. This isn't a minor concern—malnutrition directly impacts treatment tolerance, recovery speed, and survival outcomes. Proactive nutritional planning from diagnosis onward reduces treatment complications and supports better outcomes — reactive management after problems emerge is far less effective.
Best Foods to Eat with Kidney Cancer
Cruciferous and Leafy Green Vegetables
Cruciferous vegetables—broccoli, cauliflower, Brussels sprouts, kale, cabbage—deliver bioactive compounds including isothiocyanates (ITC), sulforaphane (SFN), and indole-3-carbinol (I3C). These compounds have documented antiproliferative and carcinogen-detoxifying activity in laboratory studies.
Meta-analysis demonstrates that high cruciferous vegetable intake reduces RCC risk by 27%. The mechanisms involve cell cycle arrest, inhibition of tubulin polymerization in RCC cells, and delayed resistance to targeted therapies like sunitinib.
General leafy greens like spinach and bok choy provide anti-inflammatory antioxidants but contain higher potassium. If lab values indicate elevated potassium, choose lower-potassium options:
- Raw cabbage: moderate potassium, excellent ITC content
- Kale: 348 mg potassium per 100g, nutrient-dense
- Lettuce varieties: low potassium, mild flavor
- Arugula: 369 mg potassium, peppery flavor, rich in ITCs
Practical guidance: Steam vegetables rather than boiling to preserve phytonutrients. Rotate between different cruciferous vegetables weekly—variety delivers a broader phytonutrient profile than eating only broccoli or only kale.
Berries and Vitamin C-Rich Fruits
Berries combat oxidative stress, a key driver of RCC tumorigenesis. Blueberries, strawberries, raspberries, and cranberries provide concentrated antioxidants in low-potassium packages—ideal for kidney cancer patients managing mineral levels.
Meta-analysis shows the highest vitamin C intake reduces RCC risk by 22%. Beyond antioxidant activity, vitamin C serves as a cofactor for TET enzymes involved in DNA methylation—a process frequently disrupted in kidney cancer. Preclinical studies reveal vitamin C restores 5hmC DNA methylation and significantly enhances anti-PD-L1 immunotherapy efficacy in RCC models.
Potassium content (per 100g):
- Cranberries: 80 mg
- Blueberries: 77 mg
- Raspberries: 151 mg
- Strawberries: 153 mg
Citrus fruits provide vitamin C but require individual consideration if potassium or acid reflux concerns exist. Check your labs first, since potassium tolerance varies widely between patients.
High-Fiber Whole Grains
Dietary fiber protects against RCC by improving insulin sensitivity and reducing systemic inflammation. In the NIH-AARP cohort, highest total fiber intake reduced RCC risk by 15-20%, while whole grain intake specifically lowered risk by 16%.
Whole grains—oats, brown rice, quinoa, whole wheat—provide sustained energy, support gut health, and manage blood sugar. The risk is significant: high glycemic load diets increase RCC risk by 2.5-fold, and high glycemic index diets raise risk by 38%.
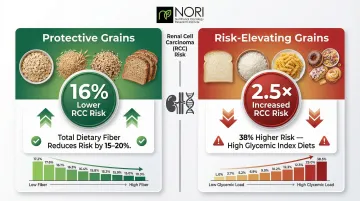
The same research links refined grain intake to increased kidney cancer risk. Practical swaps: whole wheat bread over white, brown rice over white rice, steel-cut oats over instant oatmeal.
Phosphorus caution: Bran cereals and certain whole-grain products contain high phosphorus. If labs show elevated phosphate levels, check with your care team before loading up on bran-based products.
Lean and Plant-Based Proteins
Protein source matters. High animal protein intake associates with increased RCC risk in pooled analyses, while plant protein shows neutral or marginally protective associations.
Plant-based proteins—lentils, beans, tofu, tempeh—are gentler on kidneys than large amounts of animal protein. For most kidney cancer patients, they're the safer default.
For patients post-nephrectomy, requirements can shift considerably. Dialysis patients may need 1.0-1.2 g/kg/day to compensate for protein losses—the opposite of standard CKD restriction. Let your care team guide the target.
Safer lean animal protein options:
- Chicken and turkey (skinless)
- Fish, particularly oily fish like salmon for omega-3s
- Eggs (moderate portions)
Avoid large portions of red meat or any processed/cured meats. Cooking method matters: grilling meat at high temperatures produces heterocyclic amines linked to 2-fold increased risk of papillary RCC.
Hydration and Kidney-Friendly Beverages
Adequate hydration supports waste filtration and reduces concentration of potential carcinogens in the urinary tract. Water should be your primary beverage. Herbal teas (with physician clearance to avoid drug interactions) and low-sugar fruit juices contribute to hydration goals.
Caution: Over-hydration can be problematic for patients with compromised kidney function post-surgery. Hydration needs should be guided by lab values and physician advice, not generic "8 glasses daily" rules.
Foods to Avoid or Limit with Kidney Cancer
Red and Processed Meats
Meta-analysis demonstrates highest red meat intake increases RCC risk by 36%, while processed meat raises risk by 13%. The mechanisms likely include high-temperature cooking byproducts like heterocyclic amines and polycyclic aromatic hydrocarbons (cancer-linked compounds formed during high-heat cooking), plus heme iron and nitrate content in processed meats.
Practical substitutions:
- Replace deli meat sandwiches with grilled chicken breast or hummus wraps
- Swap red meat mains for legume-based dishes, fish, or tofu stir-fries
- Use acidic marinades (lemon juice, vinegar) before cooking animal proteins to reduce carcinogen formation
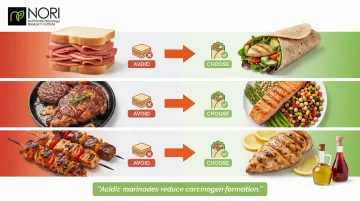
High-Sodium and Ultra-Processed Foods
Excess sodium raises blood pressure, straining already-compromised kidneys and worsening existing kidney impairment. Ultra-processed foods hide sodium and contain phosphate additives, nitrates, and artificial sweeteners that create additional kidney burden.
According to a 2018 BMJ cohort study, a 10% increase in ultra-processed food consumption drives a 12% increase in overall cancer risk. This dose-response pattern strengthens the case for reducing ultra-processed foods across all stages of kidney cancer.
Common high-sodium foods to limit:
- Fast food and restaurant meals
- Canned soups and broths
- Packaged snacks (chips, crackers, pretzels)
- Frozen ready meals
- Processed deli meats
Flavor alternatives: Fresh herbs (basil, cilantro, parsley), lemon juice, garlic, black pepper, cumin, paprika, and other spices add flavor without sodium.
High-Phosphorus Foods
Kidneys regulate phosphorus balance. When function is impaired, excess phosphorus accumulates, weakening bones and contributing to cardiovascular complications. Not all patients need phosphorus restriction—base decisions on blood phosphate levels, not assumptions.
Natural high-phosphorus foods:
- Dark-colored sodas (phosphoric acid)
- Dairy products (milk, cheese, yogurt)
- Processed bran cereals
- Oysters and organ meats
- Beans, lentils, nuts, seeds
Hidden phosphorus sources: Check labels for phosphoric acid, sodium phosphate, calcium phosphate, pyrophosphate, and polyphosphates. Inorganic phosphate additives have absorption rates exceeding 90% and must be avoided if kidney function is reduced.
High-Potassium Foods (When Labs Indicate Concern)
Potassium restriction is not universally necessary for kidney cancer patients. It becomes important when labs show impaired potassium filtration (hyperkalemia risk). Blanket potassium restriction for all kidney cancer patients is a common misconception.
When restriction is indicated, moderate these foods:
- Bananas, oranges, melons
- Tomatoes and tomato products
- Potatoes and sweet potatoes
- Avocados
- Raisins and dried fruits
- Artichokes, spinach (cooked)
Unnecessary restriction can compromise nutrient intake without clinical benefit. Always confirm hyperkalemia through bloodwork before limiting potassium-rich foods.
Alcohol and Sugary Beverages
While moderate alcohol intake (<30g/day) historically associates with 28% decreased RCC risk, recent data reveals alcohol disrupts wellness-supporting immunity and reduces survival efficacy of anti-PD1 immunotherapies. Alcohol also increases TKI toxicity for patients taking sunitinib or similar drugs.
Even moderate consumption should be discussed with your oncologist given drug interactions and treatment interference.
Sugary beverages present a separate concern. They drive obesity and insulin resistance, both established kidney cancer risk factors, while placing additional filtration burden on the kidneys.
Better beverage choices:
- Water (still or sparkling)
- Herbal teas (unsweetened)
- Diluted, low-sugar vegetable juices
- Infused water (cucumber, lemon, mint)
Nutrition During Kidney Cancer Care
Active cancer care—surgery, targeted therapy, immunotherapy—creates unique nutritional challenges. Loss of appetite, nausea, taste changes, mouth sores, and fatigue all affect eating ability. Research suggests 50-80% of kidney cancer care patients are nutritionally deficient, so working with a dietitian before cancer care starts can prevent significant declines.
When Appetite Drops
- Eat small, frequent meals (5-6 per day instead of 3 large)
- Prioritize nutrient-dense, easy-to-eat foods: smoothies, yogurt, nut butters, eggs, soft-cooked grains, soups
- Eat your largest meal at peak hunger, regardless of time of day
- Keep ready-to-eat snacks visible and accessible
Treatment also suppresses the immune system, which means food safety becomes more critical than usual. Simple precautions significantly reduce the risk of foodborne illness.
Food Safety During Treatment
- Wash all produce thoroughly under running water
- Avoid raw shellfish, sushi, raw sprouts
- Use separate cutting boards for meats and vegetables
- Cook whole meats to 145°F, ground meats to 160°F, poultry to 165°F
- Discard produce showing mold or decay
Memorial Sloan Kettering and American Cancer Society recommend strict food safety protocols rather than overly restrictive neutropenic diets (low-bacteria diets that restrict fresh produce) that eliminate beneficial foods unnecessarily.
Mouth sores and swallowing difficulties are another common side effect that directly disrupts eating. Adjusting food texture and temperature can make a real difference.
Managing Mouth Sores and Swallowing Difficulties
- Avoid spicy, acidic, and crunchy foods
- Focus on soft, cool, or room-temperature foods
- Consider honey for its soothing effects on inflamed tissue
- Discuss pain management medications with your oncologist if sores interfere with eating
Anti-Cancer Dietary Patterns and Nutritional Oncology
Oncology is shifting toward recognizing diet not just as supportive care but as a potentially therapeutic intervention. Anti-inflammatory dietary patterns—high vegetable intake, fiber, healthy fats, and limited processed foods and red meat—create systemic conditions less favorable to tumor growth.
Scientific evidence confirms healthy dietary patterns associate with lower RCC risk, while Western/inflammatory patterns link to higher risk. The mechanisms behind this include:
- Moderating insulin and IGF signaling (which drives cell proliferation)
- Activating AMPK, a metabolic regulator being studied for its role in metabolic wellness in nutritional oncology research
- Attenuating PI3K/Akt/mTOR pathways that cancer cells rely on to survive
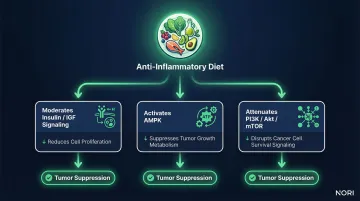
Nutritional oncology is the targeted use of diet and specific nutrients to exploit metabolic vulnerabilities in cancer cells. These mechanisms explain why what you eat can influence the environment in which kidney cancer cells either thrive or struggle. One approach studied in kidney and other cancers is methionine restriction, which limits this amino acid (found primarily in animal proteins) to disrupt cancer cell metabolism while preserving overall nutrition. Reducing animal protein intake without causing malnutrition can support metabolic wellness, reduce IGF-1 levels, and is being explored alongside conventional care in ongoing research.
NORI has spent over 20 years researching this approach, combining cycled methionine restriction with proprietary nutraceuticals into an integrative support program for cancer patients. Patients interested in individualized nutritional support can schedule a free initial consultation or call 800-634-3804.
Critical reminder: Nutritional interventions work best as complements to conventional treatment, not replacements. Always disclose dietary changes and supplements to your oncology team to avoid drug-nutrient interactions.
Frequently Asked Questions
What is the best diet for someone with kidney cancer?
There's no single "best" diet, but a plant-forward approach rich in cruciferous vegetables, berries, whole grains, and lean/plant proteins—while limiting processed foods, red meat, sodium, and alcohol—is consistently supported by research. Individualization based on lab values and treatment status is essential.
What foods should be avoided with kidney cancer?
Limit red and processed meats, ultra-processed high-sodium foods, high-phosphorus packaged products, alcohol, and sugary beverages. High-potassium foods only need restriction if blood labs indicate elevated potassium levels—not as a blanket rule.
How to cope with kidney cancer?
Focus on what you can control: maintaining adequate intake, eating anti-inflammatory foods, and staying hydrated. Working with a registered dietitian or an integrative program like NORI can help reduce overwhelm and build a clear, personalized plan.
Can kidney damage from chemo be reversed?
Some chemo-related kidney damage (nephrotoxicity) can partially recover with time, hydration, and removal of the offending agent. VEGF-targeted TKIs cause proteinuria in 6–34% of patients, while immune checkpoint inhibitors can cause acute kidney injury. Damage severity determines reversibility, and adequate hydration during treatment plays a meaningful role in minimizing harm.
Can you eat eggs if you have kidney cancer?
Yes. Eggs are generally acceptable, nutrient-dense protein sources for kidney cancer patients. They're lower in methionine than many red meats, easy to digest, and provide high-quality protein for muscle maintenance. Patients with specific potassium or phosphorus restrictions should discuss portion guidance with their dietitian.
Is tomato good for creatinine?
Tomatoes don't directly lower creatinine levels (creatinine is a byproduct of muscle metabolism filtered by the kidneys). However, at 287 mg potassium per 100g, patients with elevated creatinine may need to moderate intake based on potassium levels and physician guidance. Lycopene in tomatoes has antioxidant properties, though research hasn't confirmed specific kidney cancer protection.